Assessment of thyroid lesions is commonly encountered in radiological practice.
Thyroid mass
hyperplastic/colloid nodule/nodular hyperplasia: 85%
-
adenoma
follicular: 5%
others: rare
-
primary thyroid cancer (carcinoma)
papillary: 60-80% of carcinomas
follicular: 10-20%
medullary: 5%
anaplastic: 1-2%
-
other malignancies
thyroid lymphoma: 1%
SCC: rare
-
others
Risk factors for malignancy
young
male
solitary
cold on thyroid scan
past history of radiotherapy
The first three risk factors are really a reflection that elderly women with multiple benign thyroid nodules are very common.
On this page:
Clinical presentation
Thyroid enlargement: The patients complain of a visible swelling in the neck, a heavy feeling and discomfort when swallowing, or difficulty with respiration. They sometimes awake with a start for shortness of breath just after having fallen asleep. Occasionally they may complain about vague, irritating pain.
The enlarged thyroid may present as a midline neck swelling that moves on swallowing. Asymmetry may suggest nodularity. Tracheal deviation may also be noted.
The mass may be diffusely enlarged with hyperthyroidism (Graves / thyroiditis) or normal function (colloid, goiter or iodine deficiency). The mass may show multinodularity with hyperfunction of secondary hyperthyroidism or mutinodularity with normal function of multinodular hyperplasia.
There maybe a single autonomically hyperfunctioning adenoma or a single nodule with 'relatively normal function' of an adenoma, cyst or carcinoma.
A painful thyroid may represent thyroiditis, anaplastic carcinoma or colloidal hemorrhage.
Hypothyroidism: patients may have changes in weight and thinning of body hair.
Hyperthyroidism: patients may have bulging eyes and disturbances in vision, raised metabolic rate, tachycardia, or anxiety and tremor.
Radiographic features
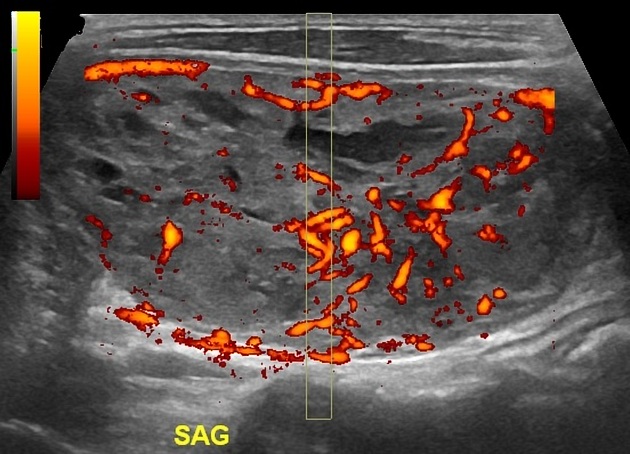
Ultrasound
taller-than-wide in axial/transverse dimension, microcalcifications, local invasion, microlobulated contour, and hypoechogenicity are suspicious features
size criteria are controversial and continuously evolving
cervical lymphadenopathy is a feature
for detailed assessment, see: assessment of thyroid lesions (ultrasound)
Nuclear medicine
A single 'cold' nodule has a 10% chance of being malignant. A single 'hot' nodule has <1% chance of being malignant.
Treatment and prognosis
Indications for FNA
Each grading system provides recommendations for when FNA is indicated (see snippet for individual systems).
Both appearance and size are factors to consider.
The criteria developed by the American Thyroid Association (2015) 6 are often used in clinical practice. See ATA guidelines for assessment of thyroid nodules.
The ACR TI-RADS system recommends FNA for TR3 lesions >25 mm, TR4 lesions >15 mm and TR5 lesions >10 mm 11.
The BTA U classification recommends FNA for any non-benign lesion (i.e. U3, U4 or U5) 12.
Additional recommendations for FNA by the American Association of Clinical Endocrinologists 4:
FNA recommended for nodules <10 mm whenever clinical information or ultrasound features raises suspicion about the presence of a malignancy
Management of FNA results
benign: clinical and imaging follow-up
-
follicular neoplasm
-
require excisional biopsy because of overlap between
hyperplastic nodule
follicular variant of papillary carcinoma
-
-
atypia of uncertain significance / follicular lesion of uncertain significance (AUS/FLUS)
3-6% of all FNA
-
repeat FNA
two samples obtained at second biopsy
if AUS/FLUS again (~20%) on the first sample, then the risk of malignancy is 5-15% 10
-
the second sample may be sent for gene sequencing, if available (gene expression classifier)
if benign, then normal clinical and imaging follow-up
if suspicious, 50% risk of malignancy
malignant: partial or total thyroidectomy with lymph node exploration






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.