Hepatic mesenchymal hamartomas are uncommon benign hepatic lesions that are mostly seen in children under the age of 2. Some authors consider them to be developmental anomalies rather than cystic neoplasia 9,12.
On this page:
Epidemiology
Hepatic mesenchymal hamartomas typically occur in children and neonates 3 with most cases presenting within the first two years of life 3. They rarely present in adults 10. There is a reported male predominance of 2:1 13.
Clinical presentation
Hepatic mesenchymal hamartoma can be rather large at presentation, therefore abdominal distension and respiratory distress are thought to be the most common presenting features in children.
Classically presents with normal serum alpha-fetoprotein (AFP) level, although unusual cases presenting with elevated AFP have been reported 2.
Pathology
The lesions are characterized by an admixture of ductal structures (blood vessels, small groups of hepatocytes, and bile ducts) within a copious loose/edematous connective tissue stroma 7,8. They rarely calcify 15.
On a cut surface, there are typically multiple cysts in an edematous stroma; the cysts can vary in size ranging from a few millimeters to 16 cm, and in number and distribution, being discrete or connected 13.
Microscopic appearance
Mesenchymal hamartomas in adults may show a series of histologic modifications: progressive loss of hepatocytes, degeneration of bile duct epithelium, and cystic changes of the mesenchymal component 12,13.
Genetics
Mesenchymal hamartomas of the liver are attributed to abnormal expression of the chromosome 19 microRNA cluster, such as due to chromosome rearrangement, or DICER1 gene mutation, which in turn causes microRNA dysregulation 14.
Radiographic features
As with other hamartomas, hepatic mesenchymal hamartomas are disorganized lesions that are usually cystic with a variable amount of associated soft tissue. A wide spectrum of imaging features has been described, from cystic and often multiseptated, to mixed solid/cystic, to even completely solid 1.
The dominant radiographic pattern, however, is a large (often around 12-15 cm 8), predominantly cystic mass with internal septations 3. There can be considerable variation in the size of septae and cystic spaces 9.
Plain radiograph
Although nonspecific, radiographs may show a large, non-calcified mass in the right upper quadrant 9.
Ultrasound
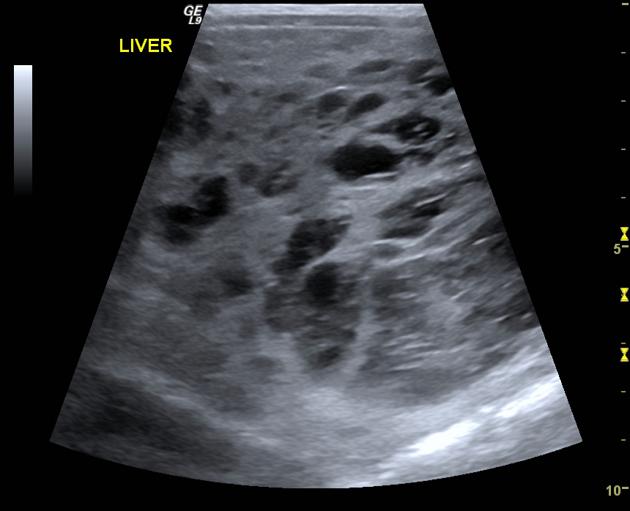
It usually appears as a multiseptated cystic lesion interspersed with solid components. Detection is difficult for pedunculated lesions. In some lesions may be the predominance of solid structures 13.
CT
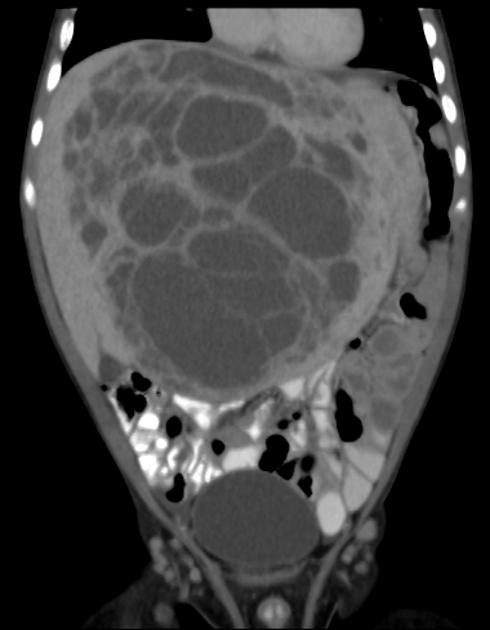
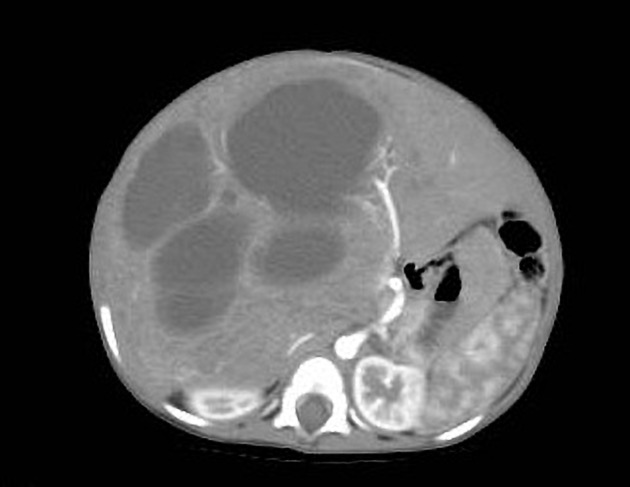
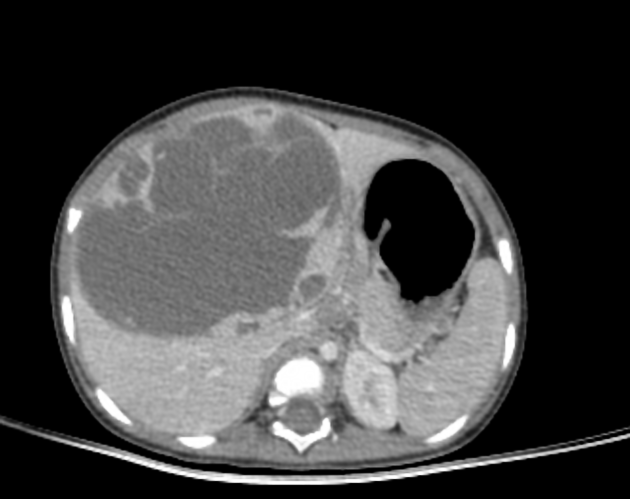
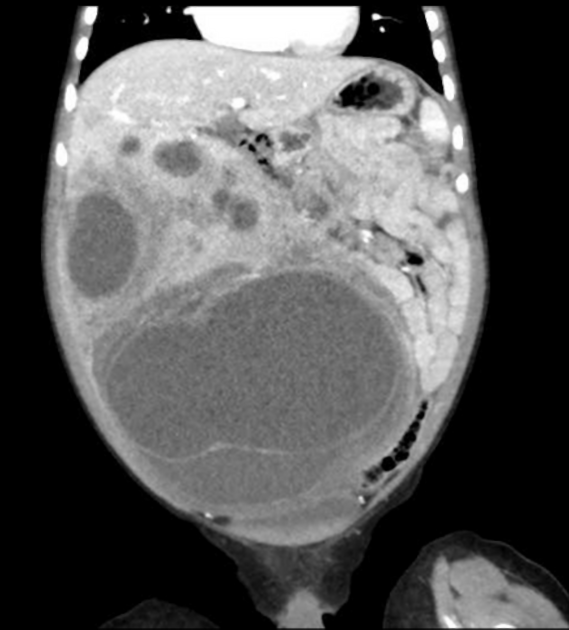
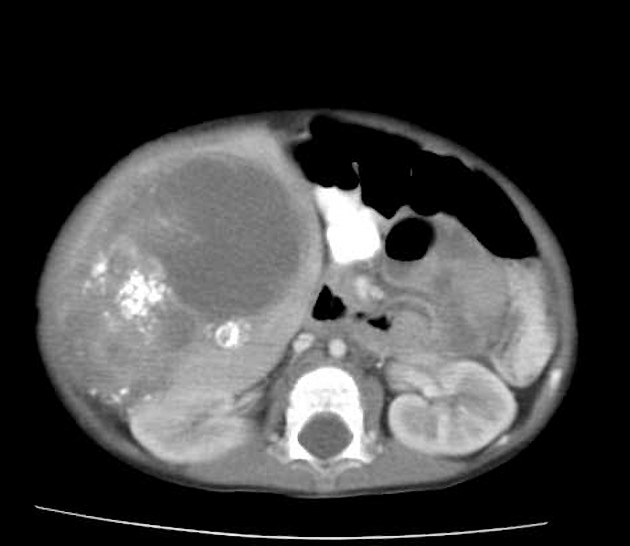
On unenhanced CT, it usually has a heterogeneous appearance. The stromal elements often appear hypoattenuating, whereas the cystic components have water attenuation 8,9. The appearance of cystic and solid portions has been likened to Swiss cheese.
On a postcontrast CT scan, solid portions or thick septa of the tumors can show heterogeneous enhancement 1-8,13.
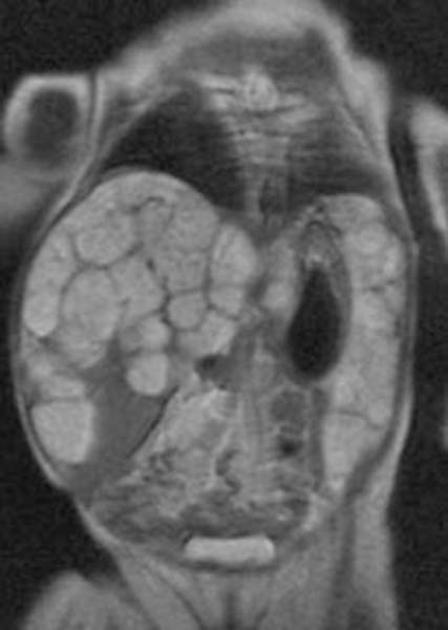
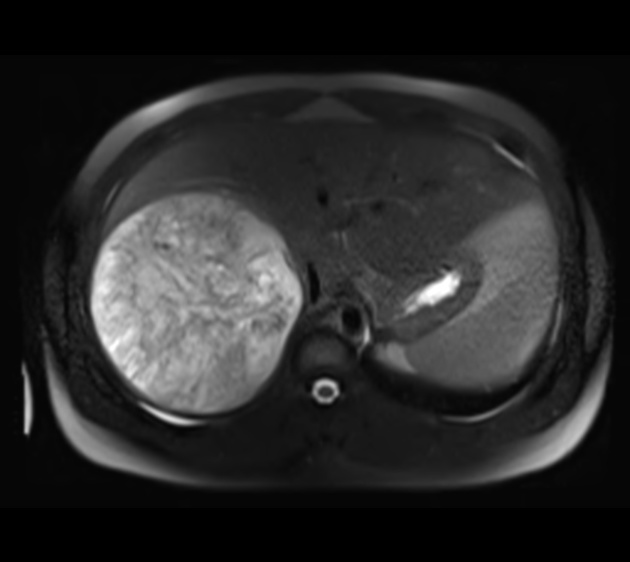
MRI
prominent cystic components
multifocality is uncommon
MR imaging appearance of mesenchymal hamartoma can also vary depending on the presence of stromal elements as well as the protein content of the fluid 8.
Angiography (DSA)
While not being a standard diagnostic imaging modality of choice, angiography may show peripheral hypervascularity to the lesion with a septated avascular center 3-9.
Treatment and prognosis
Mesenchymal hamartomas are benign lesions and are best treated by surgical resection, which usually results in cure 2. There are occasional reports of ultrasound-guided intraoperative aspiration of fluid from the cystic components of the tumor to reduce its volume, facilitating surgical resection 5.
Complications
There are fatal complications associated with hepatic mesenchymal hamartomas (particularly in the prenatal group) that generally result from the size of lesion 2:
respiratory distress: neonatal respiratory distress
circulatory complications/compromise owing to a large space-occupying abdominal lesion
Differential diagnosis
On imaging consider:
hepatoblastoma: often predominance of the solid component and persistently elevated or rising AFP
undifferentiated (embryonal) sarcoma of the liver: older age at presentation (6-10 years)
infantile hemangioendothelioma of the liver: associated with midaortic syndrome
simple hepatic cyst (or cluster): no solid component




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.