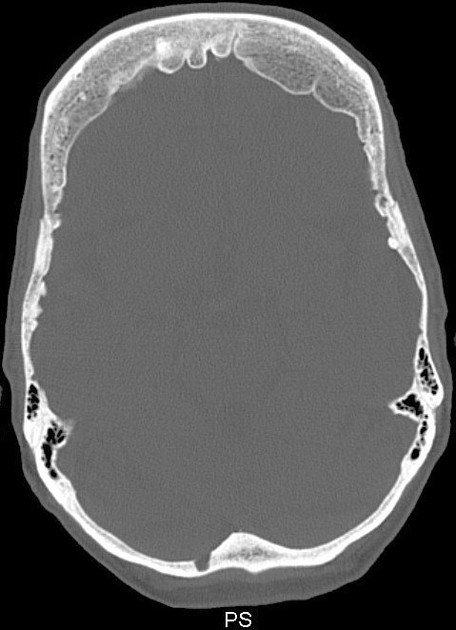
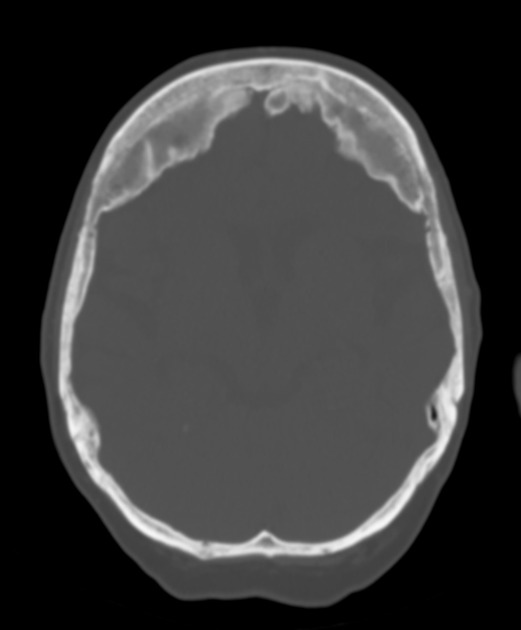
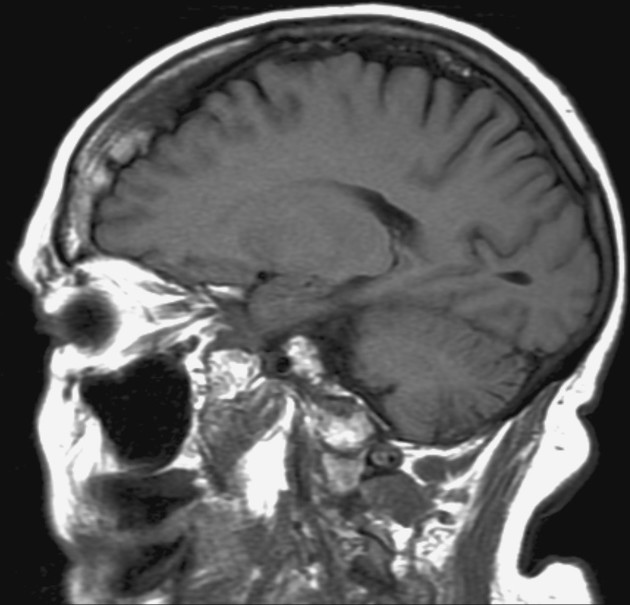
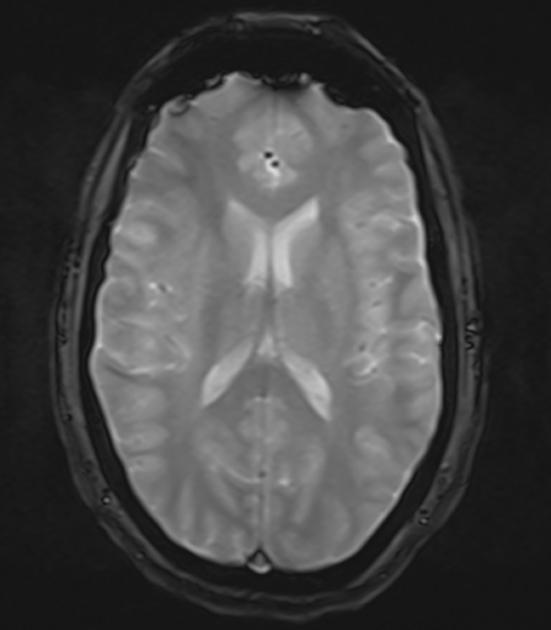
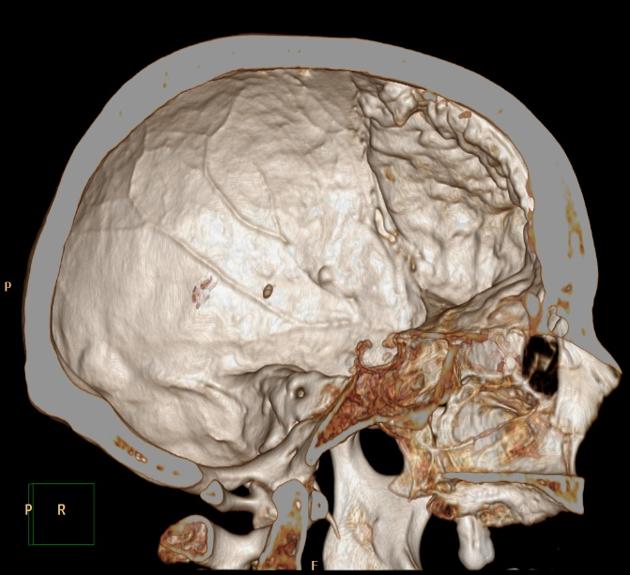
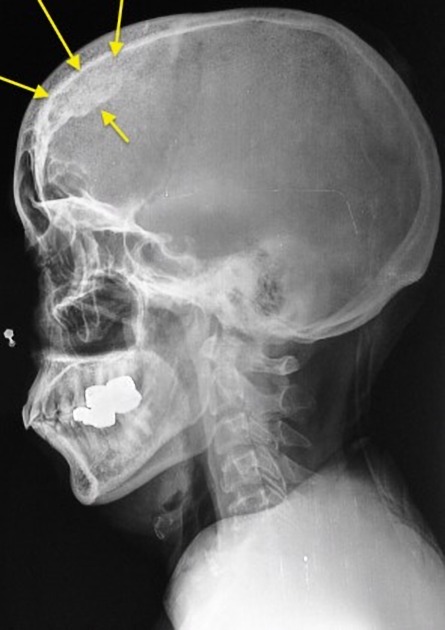
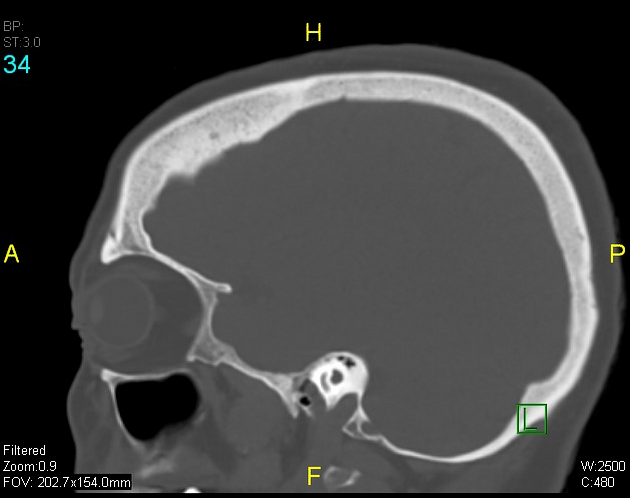
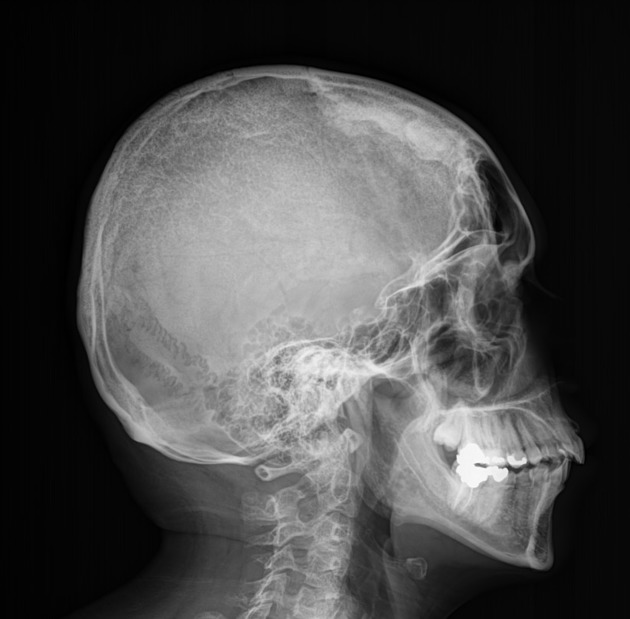
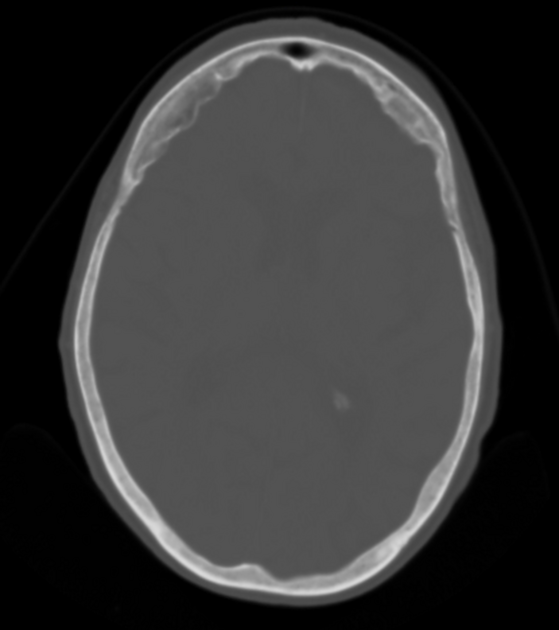
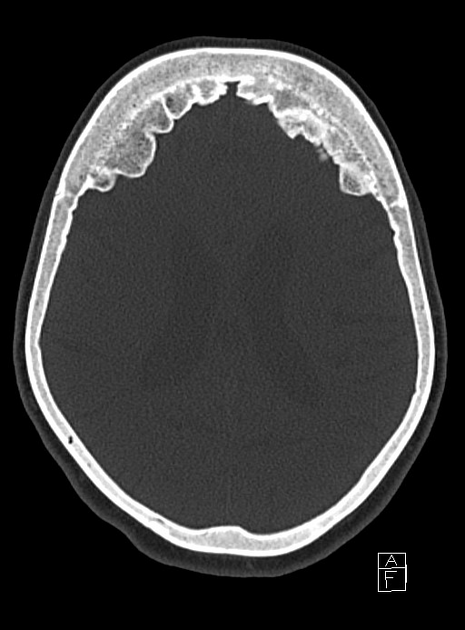
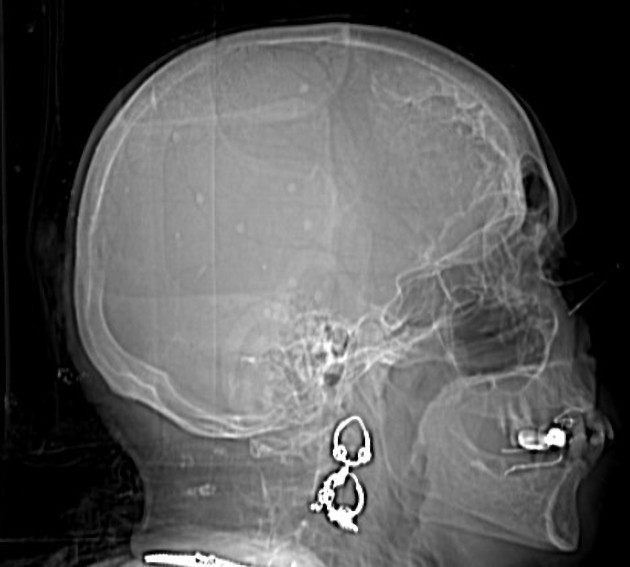
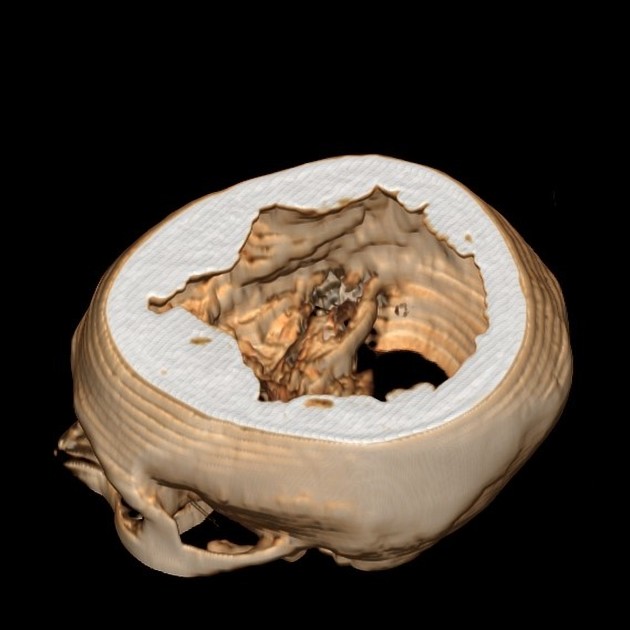
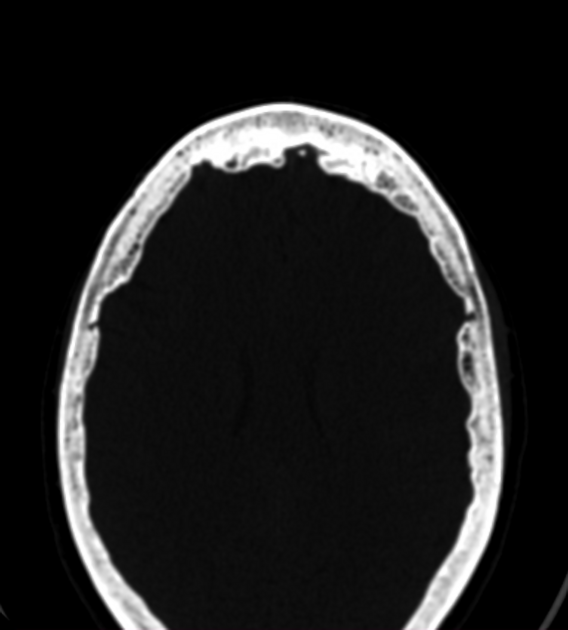
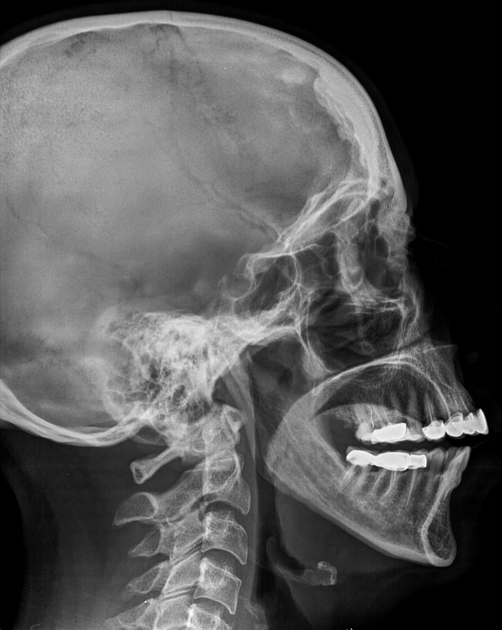
Hyperostosis frontalis interna is characterized by benign overgrowth of the inner table of the frontal bone. The etiology is unknown. The condition is generally an incidental finding of no clinical significance. It is typically bilateral and symmetrical and may extend to involve the parietal bones. The skull thickening may be sessile or nodular, and may affect the bone in a focal or diffuse manner.
The importance of this condition stems mainly from the necessity of not mistaking it for pathology (see below).
Hyperostosis calvariae diffusa and hyperostosis frontoparietalis are related entities.
On this page:
Epidemiology
Post-mortem studies report a prevalence of 12% 3. It is most common in women over the age of 65, with 87% of severe hyperostosis frontalis interna occurring in this cohort of patients 3.
Associations
It is part of the triad of Morgagni-Stewart-Morel syndrome and may be encountered in a number of other syndromes 3:
Clinical presentation
As hyperostosis frontalis interna is usually an incidental finding of no clinical significance, patients are generally asymptomatic. Compression by calvarial thickening may lead to cerebral atrophy and may present with cognitive impairment, neuropsychiatric symptoms, headache, and epilepsy 1,3.
Pathology
The etiology and pathogenesis are not well understood, although many theories have been proposed. These include a genetic predisposition, angiosomes of numerous vascular anastomoses on the frontal bone of the calvaria, and the estrogen theory 3. Nodular endocranial remodeling may result in compression of the cerebrum.
Classification
Hyperostosis frontalis interna is classified into four grades of severity based on Hershkovitz's morphological and histopathological findings 1. The Hershkovitz classification was modified to include a fifth grade of severity after a cadaveric study in 2011 described hyperostotic findings at the falx cerebri 1,3.
type A: endocranial frontal bone elevations less than 10 mm in diameter
type B: nodular bony formations occupying less than 25% of the frontal bone
type C: nodular bony formations occupying up to 50% of the frontal bone
type D: continuous nodular bony formations involving more than 50% of the frontal endocranium
type E: severe hyperostosis frontalis interna with soft tissue expansion
History and etymology
It was first described in 1719 by Italian anatomist Giovanni Battista Morgagni as a pathology accompanying virilism and obesity 3.
Differential Diagnosis
The differential is that of hyperostosis of the skull and includes:
bone marrow pathology





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.