Limy bile stands for the presence of a viscous substance in the dependent parts of the gallbladder and/or bile ducts, probably as a result of stasis, almost entirely composed of calcium carbonate and, therefore, highly radiopaque.
On this page:
Terminology
The terms limy bile and milk of calcium gallbladder can be used interchangeably for incidentally discovered cases of milk of calcium in the gallbladder and/or bile ducts.
The term limy bile syndrome is reserved for cases with biliary symptoms 2, usually resulting from associated biliary tract disease, and not from the limy bile in the gallbladder itself 3.
Epidemiology
Limy bile is a rare finding, with a prevalence of ~1% (range 0.1-1.7%) in patients who underwent surgery for biliary calculi 4. Women are more frequently affected than men 3.
The disorder can occur in any age group, although patients over 40 years of age are most commonly affected 5.
There is a high association with biliary lithiasis 6,8 and chronic cholecystitis 7. Limy bile rarely passes into the cystic and common bile ducts 6.
Clinical presentation
Limy bile may be an incidental finding 2 on x-ray or unenhanced abdominal scans performed for other reasons.
Relevant symptoms are those of cholestasis, e.g. right upper quadrant tenderness or jaundice, especially in those patients with an already known history of biliary disease 6.
Pathology
Although the typical constitution of calcium milk is well known to be an inadequate concentration of calcium carbonate mixed with calcium phosphate and/or calcium bilirubinate 7, the exact pathophysiological mechanism as to its formation is not well understood.
It is hypothesized, though, that limy bile develops from the stasis of sludge and debris in the gallbladder 8, such as in a phrygian cap or a porcelain gallbladder, or due to bile duct obstruction or pancreatic tumors 7.
Eventually, the gallbladder becomes chronically inflamed 3 and nonfunctional, sometimes presenting as a hydrops. However, the thick, paste-like substance itself seldom migrates towards the distal biliary ducts 6.
Radiographic features
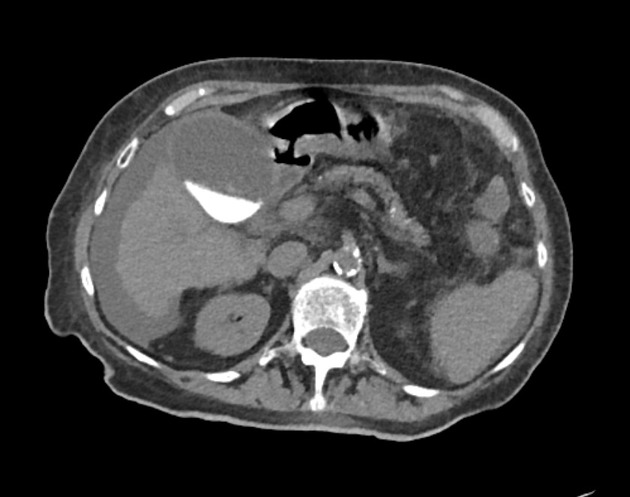
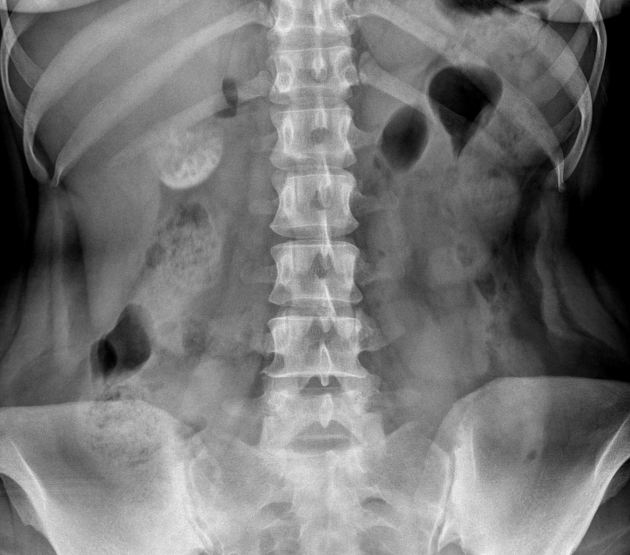
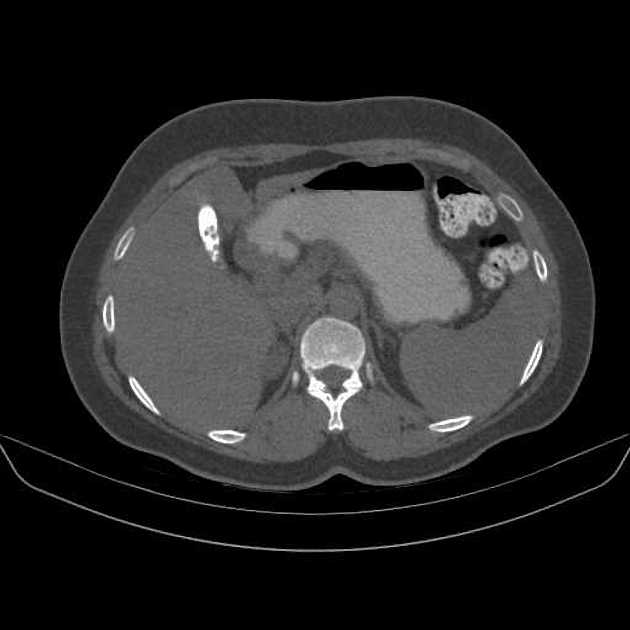
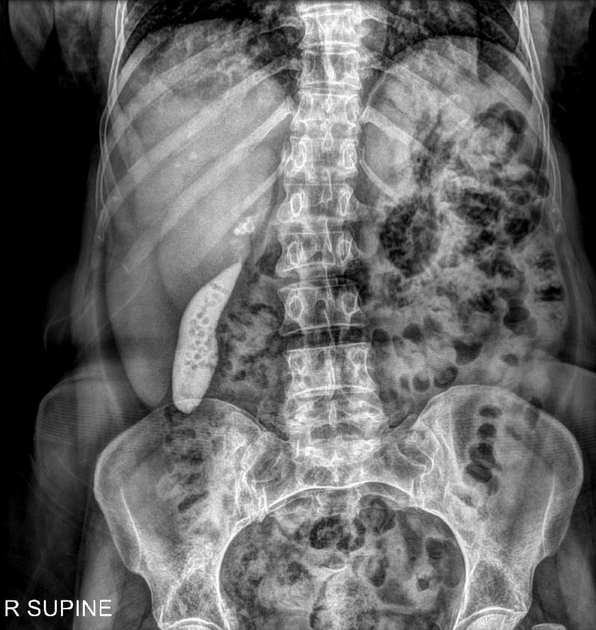
Milk of calcium gallbladder is highly radiodense on standard x-rays and CT 6. The density of calcium milk on radiographic studies and CT depends on the proportional presence of calcium carbonate 7.
A calcium-fluid level is usually seen on standing x-rays and CT due to its high relative weight, comparable to that of gallbladder sludge, calcium milk is found in the dependent portion of the gallbladder.
Plain radiograph
The so-called exclamation mark sign on standard radiography is pathognomonic for the concurrent presence of calcium milk and a calculus in the common bile duct 9.
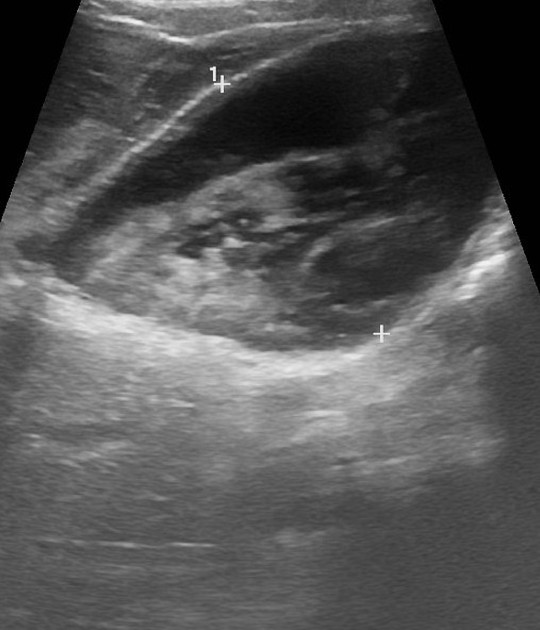
Ultrasound
Ultrasound is non-specific for differentiating gallbladder sludge from limy bile 4 - in both cases, it will reveal the presence of a hyperechoic and heterogeneous substance dependently in the gallbladder.
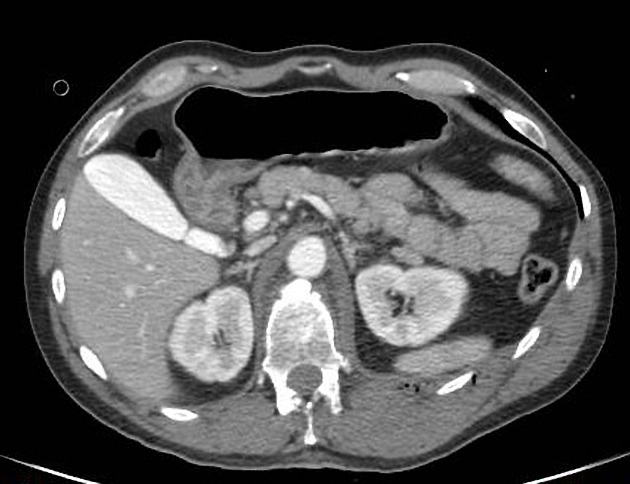
CT
Unenhanced CT much better appreciates the presence of any associated gallstones and may or may not confirm the presence of calcium milk or stones in the distal bile ducts 7. Moreover, CT allows assessment of chronic cholecystitis and gallbladder hydrops.
MRI
MRI probably has no added value in the diagnosis of limy bile; MRCP, however, has a high sensitivity and specificity in detecting associated obstructive biliary tract pathology.
Treatment and prognosis
Spontaneous dissolution of limy bile has been reported 5, but usually, limy bile is a chronic condition that needs to be treated surgically, especially when associated with (chronic) cholecystitis and (obstructive) bile duct stones, as it may lead to more severe conditions, such as emphysematous cholecystitis or pancreatitis 2.
As opposed to porcelain gallbladder, there are no reports of limy bile predisposing to malignancy.
History and etymology
The entity appears to have been discovered by JW Churchman in 1911 10, while the term limy bile itself was coined by F Knutsson in 1933 11.
The Germans initially used the word kalkmilchgalle 6, and the French term is lait calcique biliaire or syndrome de la bile calcique 2.
Differential diagnosis
-
intrabiliary contrast medium
recent ERCP 6
-
vicarious contrast material excretion (VCME)
renal and/or hepatobiliary insufficiency may be present but is not a sine qua non
-
gastrobiliary, duodenobiliary, or colobiliary fistula
perforated ulcer or tumor 7
iatrogenic gastric or bowel wall defect
-
same appearance on ultrasound 4
intermediate to high density on x-ray and CT
gallstones: often concomitant
-
extensive or scattered calcification of the gallbladder wall
slightly increases risk of gallbladder cancer (about 6%)





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.