Mastocytosis is characterized by excessive accumulation of mast cells in one or more organs. According to the World Health Organizatiοn classification, three clinical entities fall under the mastocytosis umbrella: cutaneous mastocytosis, systemic mastocytosis (with or without cutaneous manifestations), and mast cell sarcoma. This article deals primarily with systemic mastocytosis.
On this page:
Clinical presentation
There is considerable heterogeneity in the presentation of mastocytosis, and in the rate of disease progression. Clinical features include:
cutaneous manifestations
flushing
hypotension and syncope
urticaria pigmentosa
abdominal pain
nausea, vomiting and diarrhea
malabsorption
bone pain and pathological fractures
associated hematological disorders 7
Pathology
Mast cells are bone marrow-derived cells that are widely distributed in tissues. They store various biologically active mediators, such as heparin and histamine. Mediator release from mast cells has a central role in the development of type 1 hypersensitivity 1.
In systemic mastocytosis, abnormal proliferation and microscopic infiltration of mast cells involve the skin, bone marrow, gastrointestinal tract, liver and spleen. It is thought that the effects of mastocytosis relate at least in part to mediator release 7.
Classification
Under the 2016 revision of the WHO classification of tumors of hematopoietic and lymphoid tissues, mastocytosis is no longer considered a type of myeloproliferative neoplasm due to unique clinical and pathologic features.
There are multiple subtypes of systemic mastocytosis with varying clinical courses:
indolent systemic mastocytosis (most common)
smoldering systemic mastocytosis
systemic mastocytosis with an associated hematological neoplasm
aggressive systemic mastocytosis
mast cell leukemia
Radiographic features
Imaging findings are best categorized by the system rather than by modality. Most features are relatively non-specific but may suggest the diagnosis in the correct clinical setting.
Skeletal
Bone involvement in mastocytosis can be either lytic, sclerotic or mixed 4,5. Diffuse involvement tends to be more common 11. Usually, the radiographic appearance is that of sclerosis involving primarily the axial skeleton and the ends of the long bones. In some patients, there is generalized osteoporosis with the risk of pathological fractures.
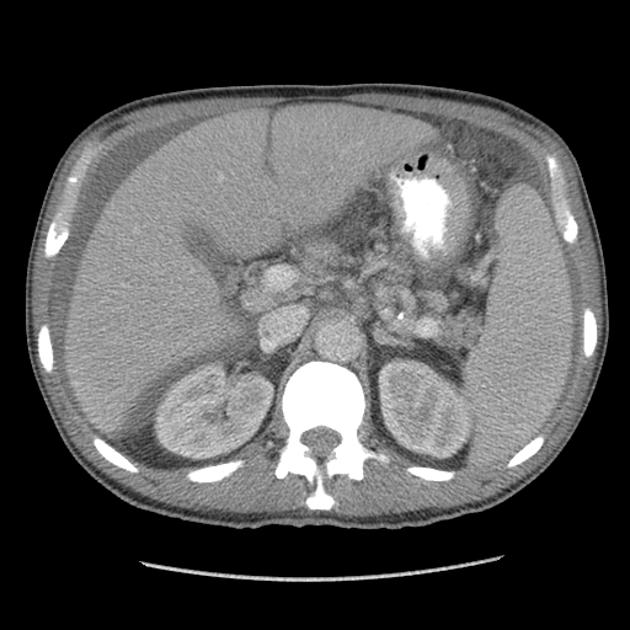
Abdominal
diffuse small bowel thickening
omental and mesenteric thickening 9
Pulmonary
pulmonary nodules (rare) 2,8






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.