Nitrous oxide (N2O) toxicity has serious medical sequelae affecting both the CNS and the bone marrow. Neurological effects include encephalopathy, myelopathy, and neuropathy. This results from demyelination and gliosis due to a functional deficiency of vitamin B12 1. Bone marrow toxicity may lead to myelosuppression, including neutropenia and megaloblastic anemia.
N2O is an established and widely used anesthetic gas though also misused quite commonly for recreational purposes as a legal 'high'. Canisters of nitrous oxide, colloquially known as “whippets”, "nangs", or "bulbs" 5, are used commercially as a propellant for whipped cream, and are commonly abused 6.
On this page:
Epidemiology
Nitrous oxide is one of the most frequently utilized inhalational anesthetics worldwide. Its use may represent an occupational hazard to chronically exposed medical and dental providers and, given its propensity to induce euphoria, a common substance of abuse in the same population. Other uses of nitrous oxide include as a propellant for the preparation of whipped cream, as well as a component of some automobile fuels 9.
Recreational use is most common among adolescents and teenagers with a male predominance. Estimated prevalence of lifetime use from varies from 11% in Germany to 29.4% in the United States and 38.6% in the United Kingdom 10.
Pre-existing vitamin B12 deficiency increases the risk of nitrous oxide-induced toxicity 8.
Clinical presentation
The clinical presentation is that of a myeloneuropathy, with features varying in severity based upon the relative degree of involvement of the corticospinal tracts, the dorsal columns, and peripheral nerves. Paresthesias and numbness involving the digits of the upper and/or lower extremities represent the most common complaints.
Physical examination may reveal decreased sensation to light touch and pain/temperature, hyperreflexia, spasticity, increased tone, disorders of gait, and the emergence of an extensor plantar response. Urinary and/or fecal incontinence or retention may also be seen 11.
Pathology
Nitrous oxide exerts much of its toxicity by oxidizing the cobalt moeity central to cobalamin, or vitamin B12, which renders it functionally inert, inducing a physiologic state that resembles a true quantitative deficiency. Cobalamin is an essential cofactor for a number of enzymes including:
methionine synthase, which catalyzes the conversion of homocysteine to methionine coupled with the regeneration of tetrahydrofolate 9
methylmalonyl CoA mutase, which converts methylmalonyl CoA to succinyl CoA
Synthesis of methionine is required for eventual methylation reactions crucial to the stability of phospholipids in myelin sheaths, which invest axons. Regeneration of tetrahydrofolate is important for a methylation reaction required for nucleotide biosynthesis and deoxyribonucleic acid synthesis, which affects cell proliferation in processes including erythropoesis 12. Methylmalonyl CoA mutase activity prevents the accumulation of methylmalonate as well as propionate 11.
Cobalamin deficiency impairs the abovementioned reactions resulting in the production of structurally abnormal myelin sheaths and a megaloblastic anemia. The end result of toxicity is demyelination and eventual gliosis, both within the central nervous system and to a lesser extent the peripheral nervous system.
Radiographic features
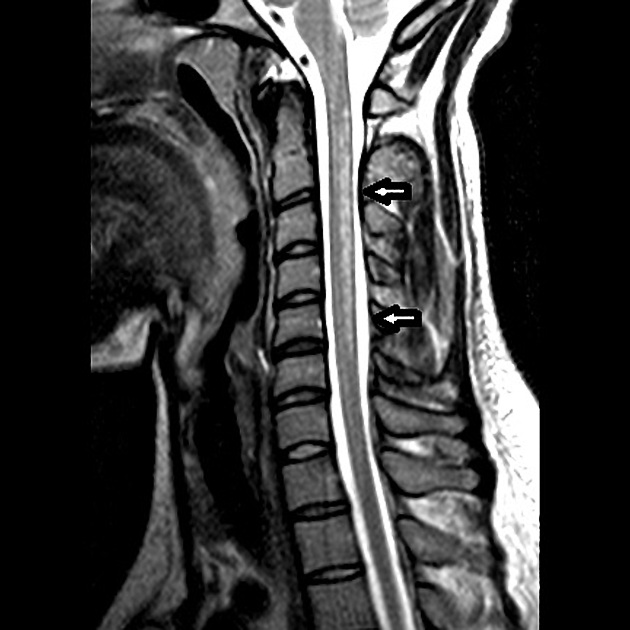
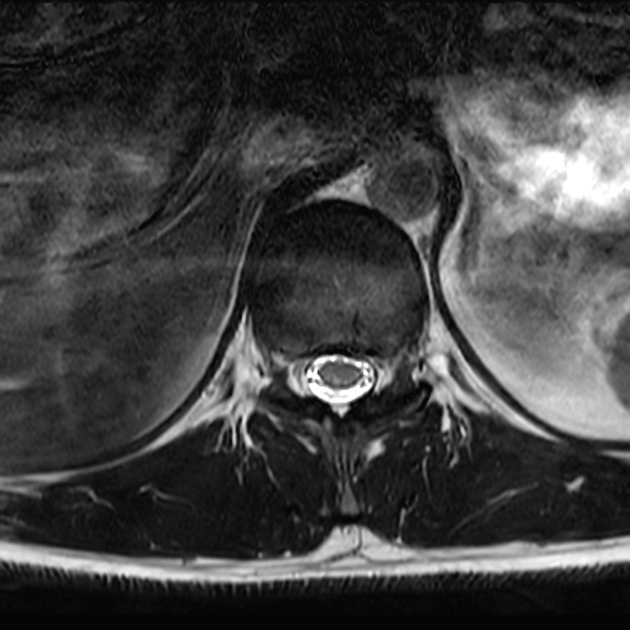
Radiographic features are identical to those of subacute combined degeneration of the cord.
MRI
T2: thoracic hyperintense signal involving the dorsal columns (inverted "V" sign), although less commonly lateral tracts of the spinal cord may also be affected; very rarely is there involvement of the anterior spinal cord
Treatment and prognosis
Treatment options include:
cessation of exposure to nitrous oxide
high dose of intramuscular vitamin B12, followed by oral supplementation
methionine supplementation has also been used 2
intravenous folinic acid is often administered if a megaloblastic anemia is present 11
Prognosis
Despite optimal treatment, some patients are left with a permanent deficit, including lifelong paraparesis.
Although there is no risk of physical addiction, the risk of a psychological N2O habit is a clear and present danger 8.
History and etymology
Nitrous oxide gas was first synthesized in 1772 by an English theologian and chemist, Joseph Priestley, chiefly remembered for his discovery of oxygen. Within only a few years it was already being abused as a recreational 'high', aware of this Humphry Davy coined the term "laughing gas" 7,8. By 1844, Horace Wells, an American dentist, had reported its usefulness as an anesthetic gas.
Differential diagnosis
See the differential diagnosis for subacute combined degeneration of the cord.






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.