Pelvic inflammatory disease (PID) is a broad term that encompasses a spectrum of infection and inflammation of the upper female genital tract, resulting in a range of abnormalities.
On this page:
Epidemiology
The highest incidence is seen among sexually-active women in their teens, with 75% of cases being under 25 years of age. In the United States, approximately 1 million females are thought to be afflicted with pelvic inflammatory disease per year, and nearly 275,000 of them are believed to be hospitalized 7.
Clinical presentation
More common presentations include acute pelvic pain (of variable intensity), cervical motion tenderness, vaginal discharge, fever, dyspareunia, and leukocytosis. Right upper quadrant pain from perihepatitis in Fitz-Hugh-Curtis syndrome is possible.
Pathology
PID is defined as an acute clinical syndrome associated with ascending spread of micro-organisms, unrelated to pregnancy or surgery. The infection generally ascends from the vagina or cervix (cervicitis) to the endometrium (endometritis), then to the fallopian tubes (salpingitis, hydrosalpinx, pyosalpinx), and then to and/or contiguous structures (oophoritis, tubo-ovarian abscess, peritonitis).
PID can result from a number of causative organisms:
-
common
Chlamydia trachomatis: pelvic chlamydial infection
Neisseria gonorrhoeae: pelvic gonococcal infection
polymicrobial infection: can account for ~35% of cases 3
-
less common
Mycobacterium tuberculosis: pelvic tuberculous infection
Actinomyces spp.: pelvic actinomyces infection
PID is usually bilateral, except when it is caused by the direct extension of an adjacent inflammatory process such as appendiceal, diverticular, or post-surgical abscesses.
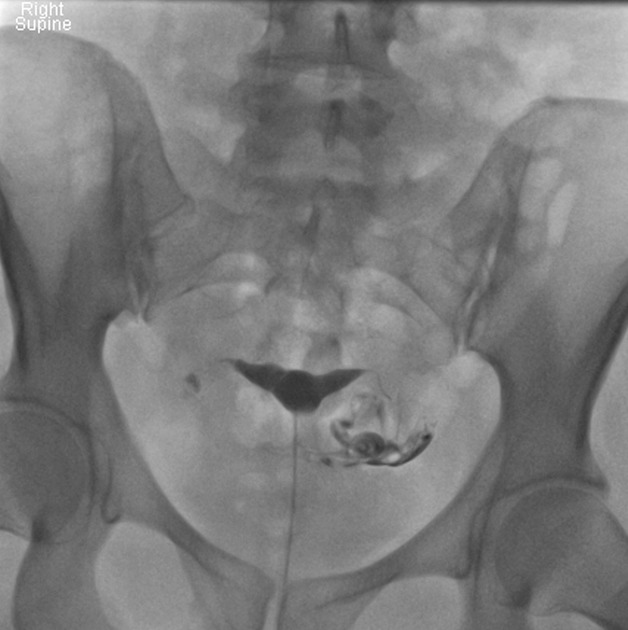
Radiographic features
Imaging features are often non-specific but are disproportionate to what may be apparent from symptoms. If imaged early (e.g. during the cervicitis stage), there may be no finding. If imaged very late, there may be an adnexal mass-like region with surrounding inflammatory change, and the fallopian tube and ovary may not be distinguished.
Other associated findings include 7:
soft-tissue stranding and infiltration of pelvic floor fascial planes
thickening of uterosacral ligaments
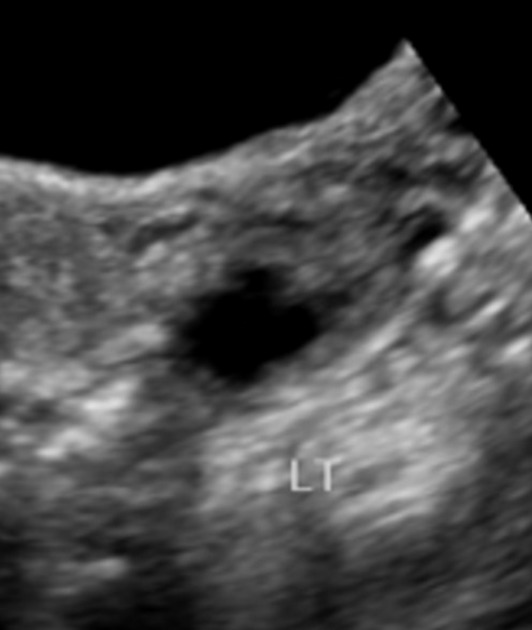
Ultrasound
Ultrasound is usually the first imaging requested in a case of lower abdominal pain.
Early findings in PID include 12 :
indistinct uterine margins
echogenic pelvic fat
fallopian tube thickening
Few non-specific findings include 8:
fluid in cul-de-sac
fluid in endometrial cavity
increased ovarian volumes
increased thickness and vascularity of the endometrium
In the most severe cases, ultrasound may show adnexal masses with a heterogeneous echo-pattern.
Some sonographic signs associated with tubal inflammation include:
-
thickened/dilated fallopian tubes
incomplete septa in the tube
fluid collection within the tubes (hydrosalpinx)
increased vascularity around the tube on color Doppler
the fat around the tube may be echogenic and there may be a small amount of reactive free fluid in the pelvis
-
echogenic fluid in the tube (pyosalpinx)
results from adhesions causing tubal obstruction
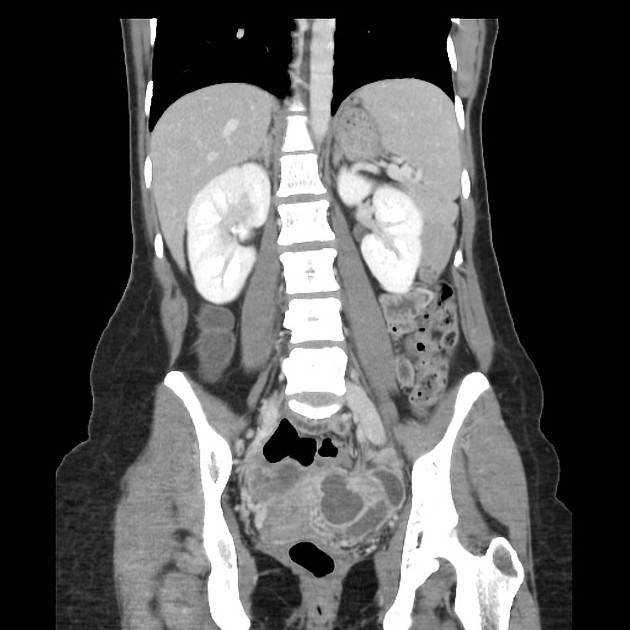
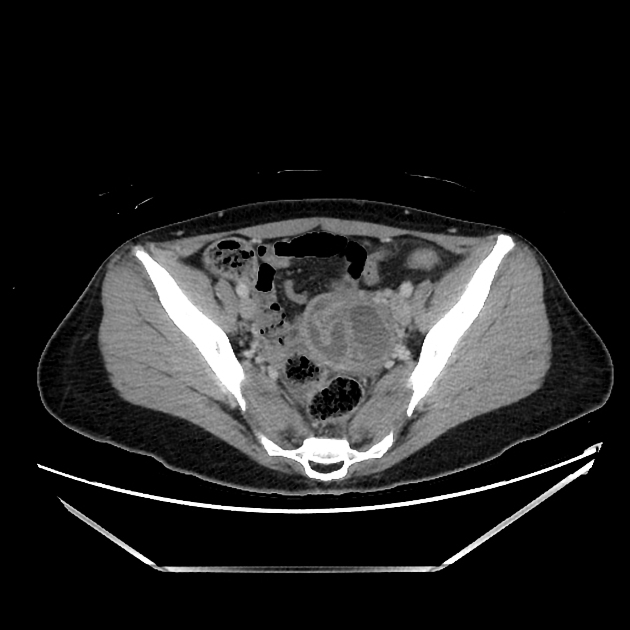
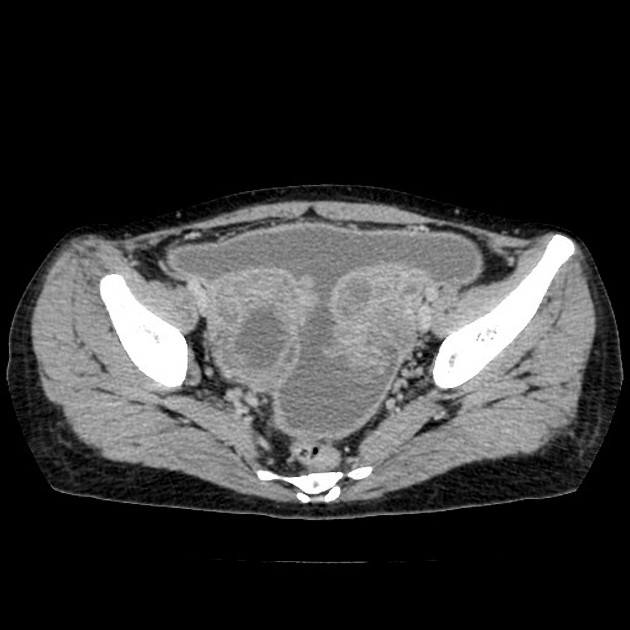
CT
tubular adnexal "mass"
fallopian tube thickening of >5 mm with enhancing wall: has high specificity of 95%
indistinct uterine border
thickening of the uterosacral ligaments
complex free fluid in the pouch of Douglas (cul-de-sac)
pelvic fat stranding or haziness
-
reactive lymphadenopathy
lymph nodes in the para-aortic and paracaval regions often become prominent due to infection draining into lymphatics along the course of the gonadal veins
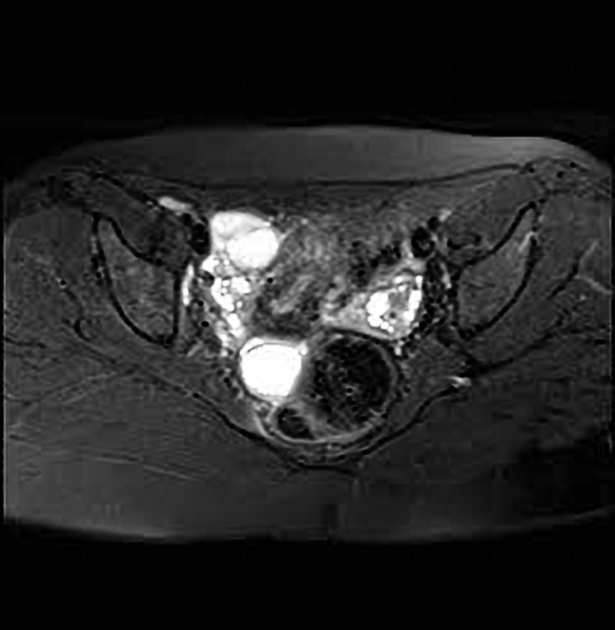
MRI
May show an ill-defined adnexal mass containing fluid with various signal intensities:
T1: if there is proteinaceous debris in a dilated tube, then it may have increased T1 signal
T1+C (Gd): wall and surrounding tissues may enhance
Treatment and prognosis
In the absence of complications, PID is often treated conservatively with education, antibiotics, and partner tracing.
Complications
infertility due to tubal adhesions
peritoneal adhesion formation causing bowel obstruction
Differential diagnosis
-
rare
consider in a patient without risk factors for PID and/or a patient in whom a course of antibiotics did not resolve the PID
-
endometriosis/endometrioma: different to PID on MRI criteria:
more likely to have high T1 signal
less likely to show restricted diffusion
-
malignant cystic ovarian tumors:
usually have solid components.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.