Splenic hemangiomas, also known as splenic venous malformations, splenic cavernous malformations, or splenic slow flow venous malformations, while being rare lesions, are considered the second most common focal lesion involving the spleen after simple splenic cysts 5,12 and the most common primary benign neoplasm of the spleen 6. They are usually found incidentally and have imaging appearances similar to hepatic hemangiomas.
Please refer to the main article for a general discussion on cavernous venous malformation.
On this page:
Terminology
It is important to note that according to newer nomenclature (ISSVA classification of vascular anomalies) these lesions are merely known as slow flow venous malformations. Nevertheless, it is probably helpful in reports to include the word "hemangioma" as this term is ubiquitous in the literature and most familiar to many clinicians. The remainder of this article uses the term "splenic hemangioma" for consistency with the majority of the existing literature.
Epidemiology
Their autopsy prevalence rate is thought to range around 0.1-14% 7,8,13. Most hemangiomas tend to be discovered in adults from the mid-30s to the mid-50s years of age 8.
Associations
- splenic haemangiomatosis: the presence of multiple splenic hemangiomas
- splenic manifestations of a systemic angiomatosis syndrome such as
Clinical presentation
The vast majority are asymptomatic and are incidentally discovered. Occasionally they may be associated with splenomegaly, abdominal pain, dyspnea, diarrhea, or constipation ref.
Pathology
Splenic hemangiomas are comprised of non-encapsulated non-neoplastic vascular channels of varying sizes ranging from capillary to cavernous, containing slow flowing blood. These vessels are lined with a single layer endothelium 2,8.
Radiographic features
Most lesions tend to be small in size (<2 cm) 12. Calcification (either central punctate or peripheral curvilinear), if present, can be detected on radiographs or CT scans.
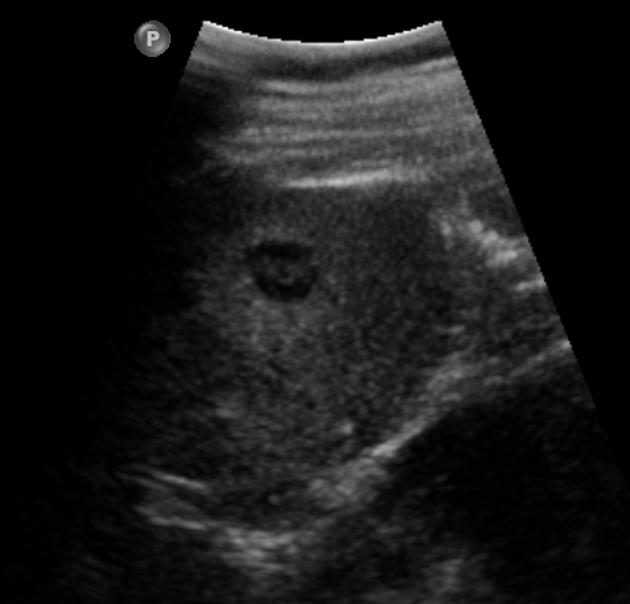
Ultrasound
Hemangiomas can have a variety of sonographic appearances depending on their exact histological composition (i.e. hypo, iso or hyperechoic). The dominant pattern, however, is considered to be a homogeneous echotexture that is predominantly hyperechoic 11.
- usually does not demonstrate any intrinsic color flow (~80% of cases) 11,13
- contrast-enhanced ultrasound: isoechogenicity to splenic parenchyma in all phases is the most frequent typical enhancement pattern of splenic hemangiomas observed on contrast-enhanced sonography 11
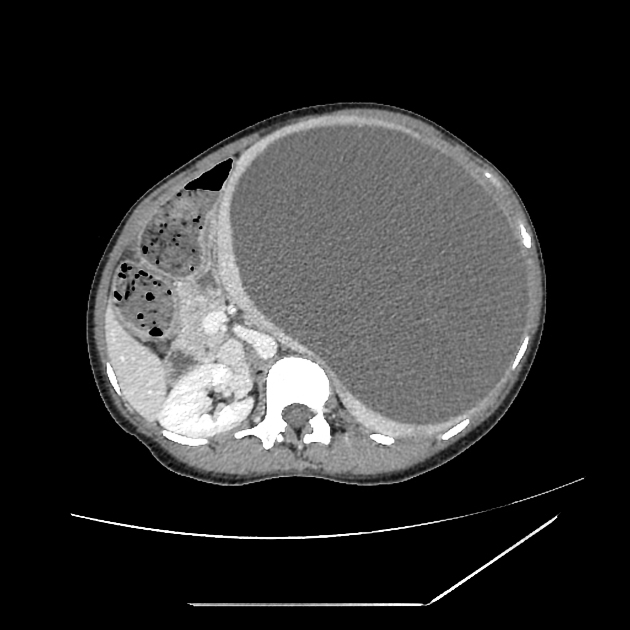
CT
Unenhanced CT scans can show a low-attenuation mass. Following intravenous contrast, the vascular channels show centripetal fill-in (from the periphery inward). Larger lesions can fill more slowly and may do so incompletely and inhomogeneously 2.
MRI
Reported signal characteristics of most hemangiomas are similar to hepatic hemangiomas and are 6,10:
- T1: iso to hypo-intense to normal splenic parenchyma
- T2: hyperintense to splenic parenchyma
-
T1 C+ (Gd)
- most demonstrate early nodular centripetal enhancement and uniform enhancement at delayed imaging
- smaller lesions may, however, show homogeneous enhancement on immediate post-contrast acquisitions remaining enhanced on delayed images 12
Nuclear medicine
Nuclear imaging with 99mTc labeled red cells shows slow accumulation of activity in the lesion followed by slow washout. Nuclear scans with 99mTc labeled sulfur colloid usually show a photopenic defect due to the radionuclide accumulation being restricted to functional splenic tissue.
Treatment and prognosis
They are benign lesions and carry no malignant potential. Their natural course is very slow growth over time 8. Hemangiomas are generally not treated unless they are symptomatic or very large, with an increased risk of hemorrhage; treatment then is usually a splenectomy.
Complications
- hypersplenism 13
- spontaneous rupture with hemorrhage is a risk with larger lesions
- may cause Kasabach-Merritt syndrome 8
- malignant degeneration (rare) 13













 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.