Subchondral insufficiency fracture of the knee (SIF/SIFK) are stress fractures in the femoral condyles or tibial plateau that occur in the absence of acute trauma, typically affecting older adults.
On this page:
Terminology
The entity subsumes that previously known as spontaneous osteonecrosis of the knee (SONK/SPONK) or Ahlbäck disease. Recognizing that spontaneous osteonecrosis of the knee was a misnomer and actually represents a subchondral insufficiency fracture that progressed to subchondral collapse with secondary osteonecrosis, the Society of Skeletal Radiology Subchondral Bone Nomenclature Committee recommended that "subchondral insufficiency fracture" be the preferred term 17.
Epidemiology
Subchondral insufficiency fracture of the knee is seen more frequently in women (M:F 1:3) and affects older patients, typically over the age of 55.
Clinical presentation
Patients often recall an acute onset of severe pain without significant trauma.
Pathology
By definition, secondary osteonecrosis of the knee occurs secondary to an insult. Subchondral insufficiency fracture of the knee is not thought to be caused by bone death but instead by osteoporosis and insufficiency fractures, with histopathologically proven origins in weakened trabeculae and applied microtraumatic forces 6,13.
Classification
Radiographic features
It is almost always unilateral, usually affects the medial femoral condyle (but can occasionally involve the tibial plateau 9) and is often associated with a meniscal tear.
Plain radiograph
In the later stages features seen include:
flattening of the femoral condyle (most commonly medial)
subchondral radiolucent focus
complicating subchondral fracture with periosteal reaction
Classification
On radiographs, the Koshino classificiation is often used (c. 2022) to determine treatment 18:
stage I: normal radiograph
stage II: radiolucency in subchondral weight-bearing area
stage III: expanded lucent area surrounded by sclerosis, subchondral bone collapse
stage IV: osteophytes and osteosclerosis on affected condyle
Fractures stage III or or IV may be considered for arthroplasty, while non-operative management can be considered for stages I or II 18.
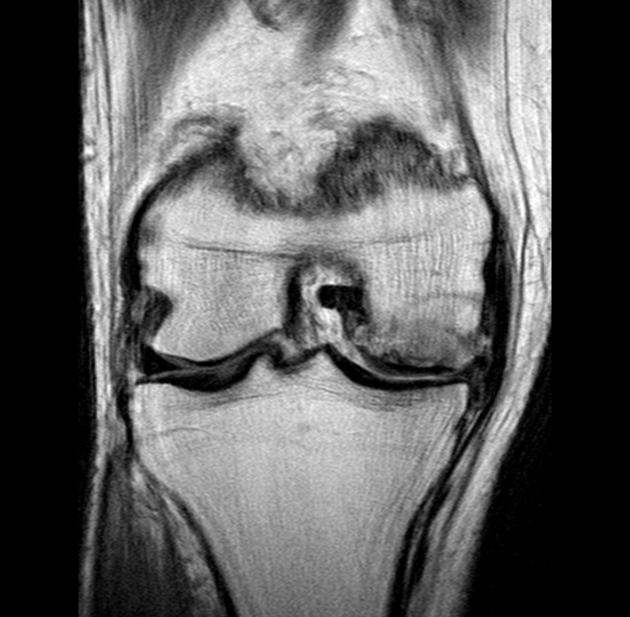
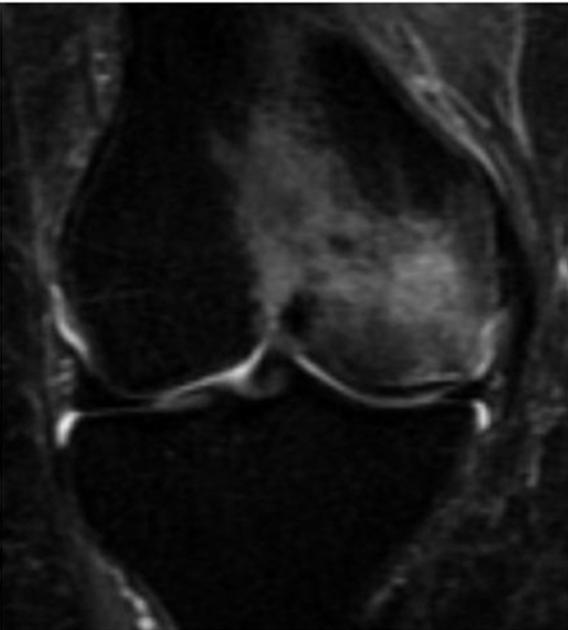
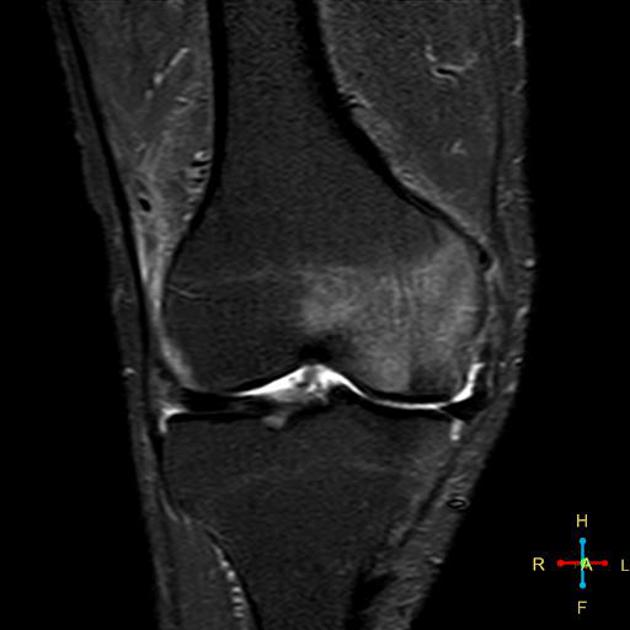
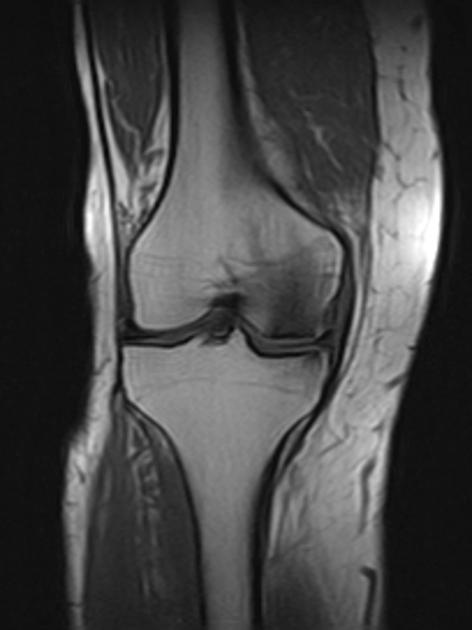
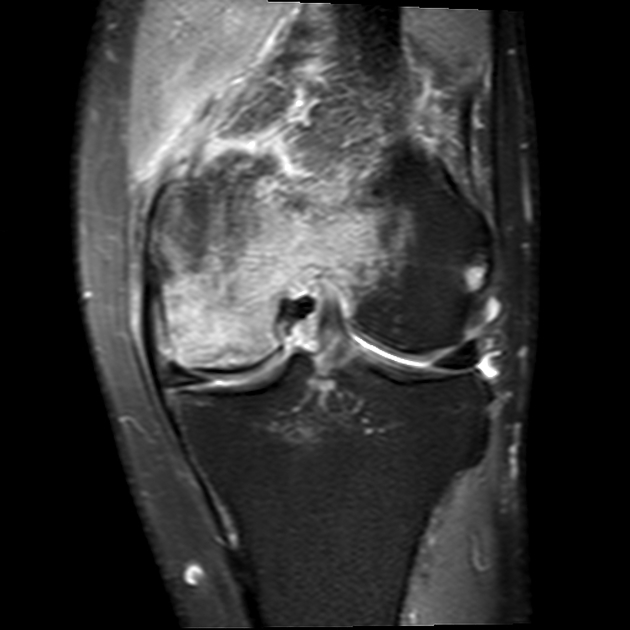
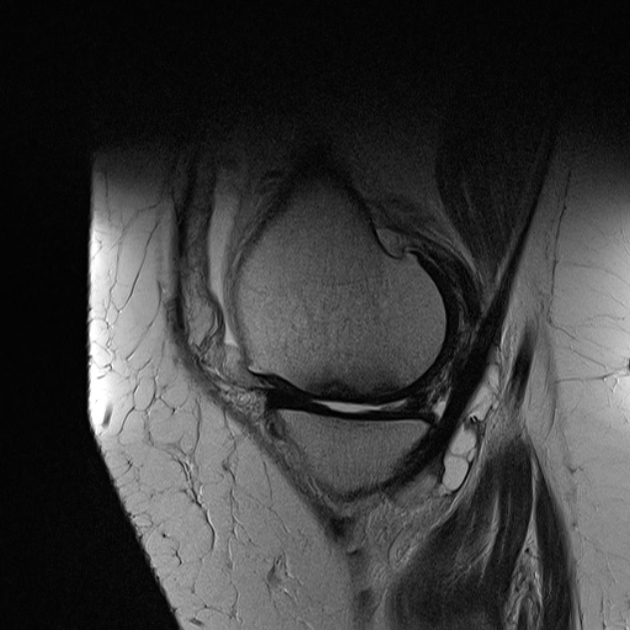
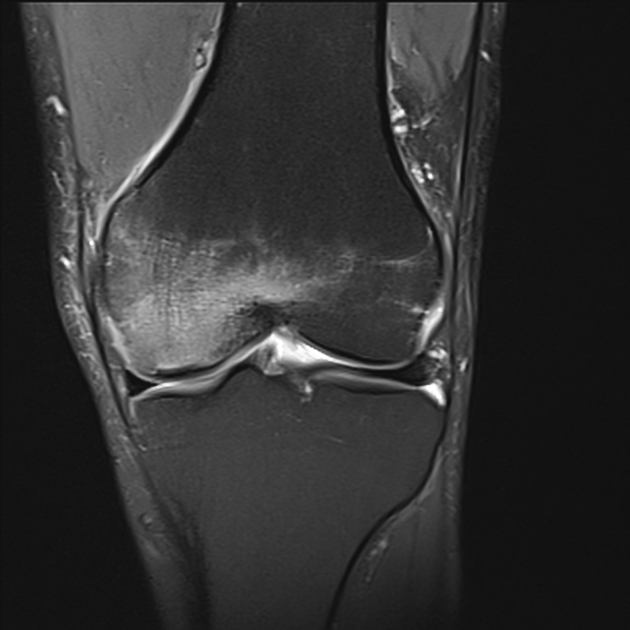
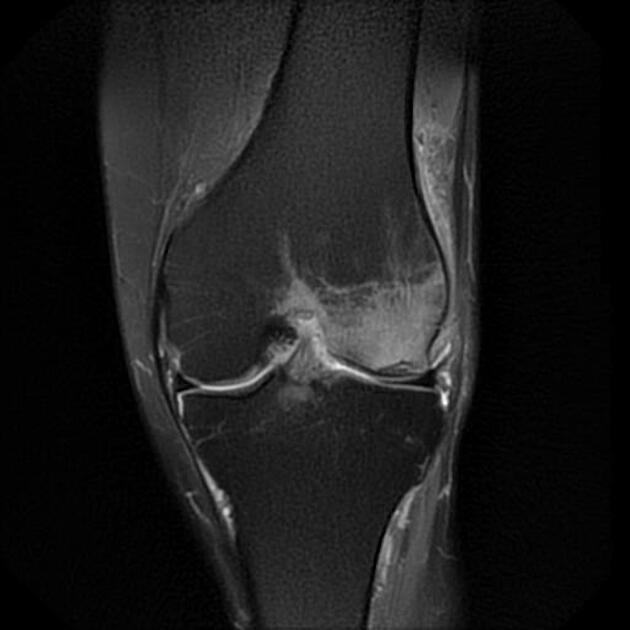
MRI
Features can vary depending on the stage and are best characterized on T2-weighted and proton density-weighted sequences. The following criteria apply to lesions without overlying cartilage abnormalities:
-
subchondral bone plate fracture 13
in the weight-bearing area of the involved condyle
subtle flattening or a focal depressive deformity
an irregular, discontinuous hypointense line in the subarticular marrow, representing callus and granulation tissue
there may be a fluid-filled cleft within the subchondral bone plate (poor prognostic factor) 13
excavated defect of the articular surface (advanced cases)
-
focal subchondral area of low signal intensity subjacent to the subchondral bone plate representing local ischemia (considered most important in early lesions and a specific MRI finding 12)
this area shows no enhancement on post-contrast; if it is thicker than 4 mm or longer than 14 mm, the lesion may be irreversible and may evolve into irreparable epiphyseal collapse and articular destruction
appears as a thickened subchondral bone plate, which represents a fracture with callus and granulation tissue and secondary osteonecrosis in the subarticular region 13
ill-defined bone marrow edema and a lack of peripheral low signal intensity rim as seen in osteonecrosis and bone infarcts
Associated features that may predict prognosis include:
associated meniscal tear and degree of extrusion
chondrosis severity
Treatment and prognosis
Prognosis varies from complete recovery to total joint collapse 2. Treatment can either be operative or non-operative, with initial treatment often conservative and consisting of analgesia and protected weight bearing. Subchondral hypointense fracture lines tend to resolve with conservative therapy. In more advanced cases, subchondroplasty (where a bone substitute is injected) may be considered.
Differential diagnosis
Possible considerations include:
subchondral stress/fatigue fracture: overuse injuries in patients without associated risk factors 17
History and etymology
It was first systematically described by Ahlbäck in 1968 2.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.