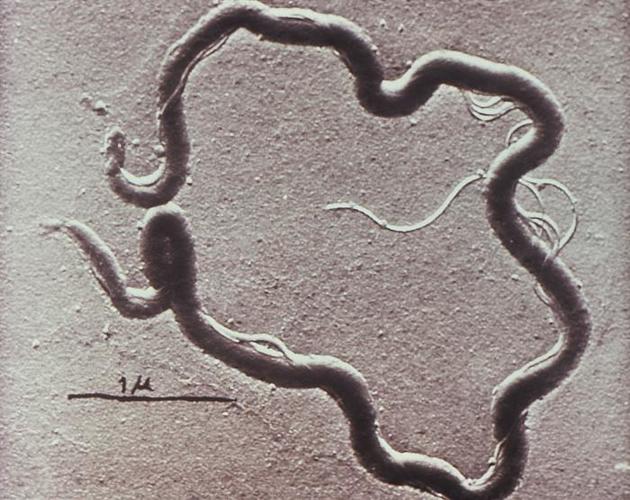
Syphilis is the result of infection with the gram-negative spirochete Treponema pallidum, subspecies pallidum. It results in a heterogeneous spectrum of disease with many systems that can potentially be involved, which are discussed separately.
On this page:
Epidemiology
Despite the discovery of penicillin, syphilis remains common worldwide and has become especially prevalent since the late 1990s 1-3. Most cases are diagnosed in low-to-middle income countries where the infection is endemic, however, syphilis is also present in high-income countries where it predominantly affects those with poor access to healthcare or those in sexuality minority populations 1-3. In these countries, the incidence of syphilis is closely related to that of HIV 2,3.
Clinical presentation
Clinical manifestations are classified into three distinct temporal stages of the disease 1,2. In addition to these well-described stages, patients may also have latent syphilis 1,2.
Primary syphilis
Primary syphilis is characterized by a lesion at the site of T. pallidum inoculation, most commonly the genitals, usually within three weeks of inoculation 1,2. The lesion is typically a single red-brown chancroid 1,2. The lesion begins as a macule before developing into a papule and finally the chancroid - a firm, painless, non-pruritic clean-based ulceration 1,2. There is often painless unilateral regional lymphadenopathy associated with the chancroid. If left untreated, the chancroid usually heals spontaneously after 4-5 weeks 1,2.
Secondary syphilis
Secondary syphilis occurs up to eight weeks after inoculation and reflects T. pallidum bacteremia 1,2. This stage may self-resolve after approximately six weeks and become latent or may relapse during the first two years before latency manifests 1,2. Due to being mediated by bacteremia, these patients not only have non-specific constitutional symptoms such as low-grade fever, malaise, headache, and generalized lymphadenopathy, but there may also be multi-organ involvement 1,2:
-
dermatological syphilis
the most characteristic finding is a symmetrical red-copper maculopapular rash on the palms and soles, however, there is a highly variable appearance 1,2
wart-like lesions known as condylomata lata may be seen in the genital regions 1,2
-
gastrointestinal syphilis
the most common gastrointestinal manifestation is syphilitic hepatitis 1,4
-
musculoskeletal syphilis
musculoskeletal symptoms are generally mild and include synovitis and periostitis 1,5
however, more serious complications such as osteomyelitis and pathological fractures can also develop 6
-
renal syphilis
a variety of renal pathologies may be seen, including either nephritic or nephrotic syndromes 1,7
these may precipitate acute kidney injury and a hypertensive crisis 7
-
early neurosyphilis
initially asymptomatic neurosyphilis, before development of acute syphilitic meningitis and later, meningovascular syphilis which may present with cerebral vasculitis and ischemic stroke 1,2,8
there may be associated ocular syphilis and otosyphillis, most commonly during acute syphilitic meningitis 1,2,8
Tertiary syphilis
Approximately one-third of patients with latent secondary syphilis will develop features of tertiary syphilis 1,2. Three potential manifestations of tertiary syphilis have been described:
-
late neurosyphilis
characterized initially by meningovascular syphilis, which may not have presented in the secondary syphilitic time-frame 1,2,8
many decades later, neurosyphilis may present with general paresis, dementia with marked personality changes, and tabes dorsalis, characterized by ataxia and sensory pains due to dorsal column involvement of the disease 1,2,8
-
usually occurs decades after initial inoculation and may involve any large vessel 1,2
typically, the proximal ascending aorta is involved (syphilitic aortitis), resulting in aortic root dilation, thoracic aortic aneurysm (luetic aneurysm), aortic valve regurgitation, and eventual congestive heart failure 1,2
-
this is an uncommon manifestation of tertiary syphilis characterized by the formation of gummas (or gummata) 1,2
these gummas can form anywhere in the body but are most commonly seen affecting the skin or bones, and exhibit symptoms related to local mass-effect or local inflammation 1,2
Congenital syphilis
Pregnant women with untreated syphilis may transmit the infection transplacentally to their fetus 1,9. Congenital syphilis is contracted in one-third of cases, while another one-third do not get syphilis, and the final one-third of pregnancies result in miscarriage or stillbirth 1,9. Due to the nature of transmission, the spirochete is disseminated to almost all organs in the fetus and thus has a very varied clinical presentation 1,9. The vast majority of these signs are not present antenatally or at birth 9.
-
early congenital syphilis - before two years of age, more unpredictable presentation
prematurity
necrotizing funisitis (inflammation of the umbilical cord)
hepatosplenomegaly and jaundice
nasal chondritis and 'runny' nose
neurosyphilis, predominantly acute leptomeningitis and chronic hydrocephalus
generalized lymphadenopathy
generalized maculopapular rash
musculoskeletal anomalies
-
late congenital syphilis - after two years of age, more predictable presentation
craniofacial anomalies such as frontal bossing, saddle nose, and prognathism
dental anomalies (part of Hutchinson triad), such as Hutchinson teeth and perforation of the hard palate
interstitial keratitis (part of Hutchinson triad)
neurosyphilis including sensorineural deafness (part of Hutchinson triad)
musculoskeletal anomalies
Pathology
This heterogenous disease results from infection by Treponema pallidum, subspecies pallidum 1-3. The bacteria is usually transmitted through direct lesion contact, although transplacental transmission also occurs 1,2.
This spirochete is closely related to other members of the Treponema pallidum subspecies, including 2:
Treponema pallidum, subspecies endemicum, which causes bejel
Treponema pallidum, subspecies carateum, which causes pinta
Treponema pallidum, subspecies pertenue, which causes yaws
Diagnosis
Diagnosing syphilis relies on either direct testing or utilizing a variety of serological tests to assess reactivity 1:
direct testing: identification of the spirochete by dark microscopy - very sensitive but requires specialist services so is rarely performed
-
serology:
-
treponemal:
T. pallidum enzyme immunoassay (TP-IgM EIA) - favored method
T. pallidum particle agglutination assay (TP-PA)
T. pallidum hemagglutination assay (TPHA)
fluorescent treponemal antibody absorption (FTA-ABS)
microhaemagglutination test for antibodies to T. pallidum (MHA-TP)
-
non-treponemal:
venereal disease research laboratory (VDRL)
rapid plasma reagin (RPR)
toluidine red unheated serum test (TRUST)
-
Radiographic features
Primary syphilis and many manifestations of secondary syphilis do not exhibit any radiographic features. Of those that do, below is a summary of the main findings with links to individual articles where applicable.
Musculoskeletal syphilis
Musculoskeletal manifestations of syphilis are discussed separately. The radiographic features are in keeping with the clinical presentation, including synovitis, osteitis, periostitis, osteomyelitis, and pathological fractures 6,10. Despite these associations with the clinical presentation, it has been further reported that syphilitic bone lesions can resemble any sort of bony lesion, and thus atypical radiographic features are common 6,10.
These must be differentiated from non-musculoskeletal manifestations of congenital syphilis, below, which are far more commonly reported in the literature.
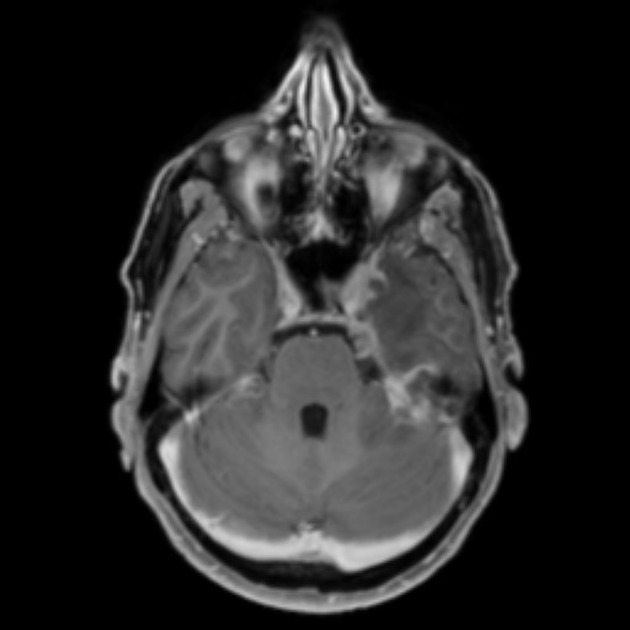
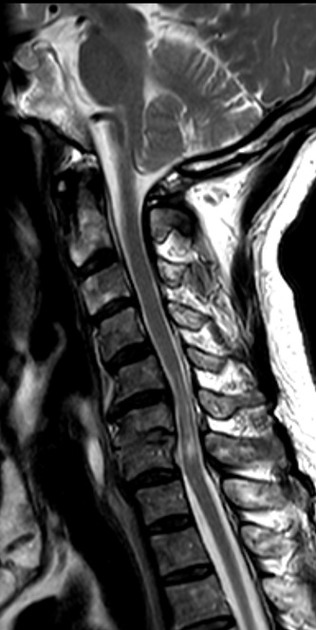
Neurosyphilis
Neurosyphilis, both early and late manifestations, is discussed separately. It is the result of CSF invasion by the infection, and subsequent sequential invasion into the meninges, leptomeningeal vessels, and finally the brain parenchyma and spinal cord tracts 8,11,12. Thus, radiographic features are highly variable depending on the temporal stage of the disease, but can potentially include those of leptomeningitis (e.g. leptomeningeal enhancement), cerebral vasculitis, ischemic stroke, cerebral atrophy, and spinal cord atrophy 11,12.
Cardiovascular syphilis
The most common manifestation of cardiovascular syphilis is syphilitic aortitis, which is discussed separately. The most common radiographic observations made are those of syphilitic aortitis and its complications such as luetic aneurysm, aortic valvulitis with aortic valve regurgitation, and coronary ostial stenosis 13,14.
Gummatous syphilis
Gummatous syphilis is discussed separately. Due to this manifestation of tertiary syphilis being able to affect virtually any organ with gummas, radiographic features are highly varied and mainly reported in case reports rather than larger studies 15. In the vast majority of cases, gummas have a very varied appearance across CT and MRI modalities and are often mistaken for malignancy 15.
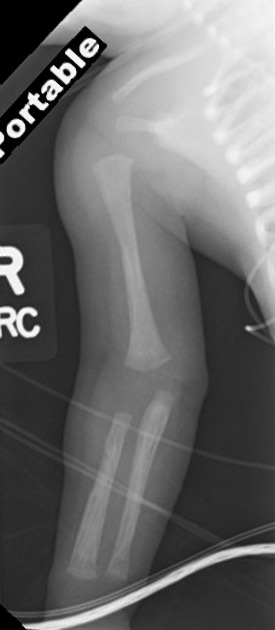
Congenital syphilis
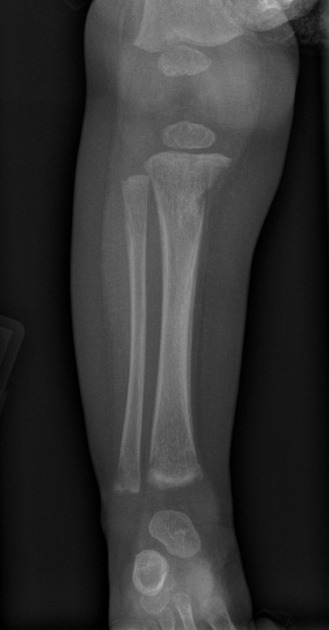
Congenital syphilis is discussed separately. Due to congenital syphilis having very different early and late presentations, there is a wide array of radiographic features 16,17. The best-described features are the musculoskeletal anomalies, which include periostitis (including the Higoumenakis sign), metaphysitis (including Wimberger sign and saw-tooth metaphysis in Wegner sign), diaphyseal osteomyelitis, pathological fractures, joint effusions, sabre shin, dactylitis, and a variety of craniofacial anomalies (including Hutchinson teeth and the Hennebert sign) 16,17. Some of these features, in addition to other signs of congenital syphilis such as fetal intrahepatic calcification, can be detected antenatally, but most will only manifest after birth 16,17.
Treatment and prognosis
Treatment of acquired syphilis is with intravenous penicillin-based antibiotics such as benzathine penicillin G (benzylpenicillin) 1,2. For patients allergic to penicillin, doxycycline (not recommended if there is neurosyphilis) or ceftriaxone may be used 1,2,20. A potential complication of therapy is the Jarisch-Herxheimer reaction, which is due to release of endotoxin-like substances from dying bacterial cells, and resembles sepsis and lasts for up to 24 hours 18. Management should also be initiated for HIV if concomitantly present 1,2. Prognosis is generally good unless there are established non-reversible changes associated with tertiary syphilis 1,2.
Treatment of congenital syphilis is also with benzathine penicillin G (benzylpenicillin) 19. Prompt treatment of early congenital syphilis prevents some, but not all, of the late manifestations of congenital syphilis 19.






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.