Brucellosis is a global zoonotic infection secondary to any of the four Brucella spp. that infect humans. It can be focal or systemic but has a particular affinity for the musculoskeletal system.
On this page:
Epidemiology
Brucellosis occurs worldwide but is particularly prevalent in Mediterranean regions, the Middle East, South Asia, and Central and South America 2. Risk in these countries is partly attributed to ineffective public and domestic animal health services.
Clinical presentation
Patients present typically with fever, which can be undulating and lasts for 2-3 weeks. Arthralgia, myalgia, and back pain are also common 5. Brucellosis may affect any system, so signs and symptoms are heterogeneous. Please see neurobrucellosis for manifestations of central nervous system infection.
Diagnosis
Due to the insidious onset of the disease, brucellosis presents in both acute and chronic forms.
Various methods to detect IgM and/or IgG antibodies have been proposed, with some conflict in the literature regarding which is optimal for diagnosis. The Rose Bengal test, serum agglutination test, Coombs test, lateral flow immunochromatography assay, a fluorescence polarization assay, indirect ELISA assays, and the immunocapture BrucellaCapt test may be used independently or in combination to confirm Brucella infection 6.
Pathology
Brucella spp. are gram-negative coccobacilli, which are mostly spread animal-to-human via unpasteurised dairy products. A number of species can act as primary hosts to infect humans as secondary hosts. Four main species infect humans 1-4:
Brucella melitensis (camel, sheep)
Brucella suis (pigs)
Brucella abortus (cattle)
Brucella canis (dogs)
Rarely, the more recently discovered fifth and sixth species B. ceti and B. pinnipediae - found in marine mammals - have been isolated in the context of neurobrucellosis. The CDC has classified the Brucella abortus, canis, and suis species as "select agents" due to their potential to be aerosolized for bioterrorism purposes.
Radiographic features
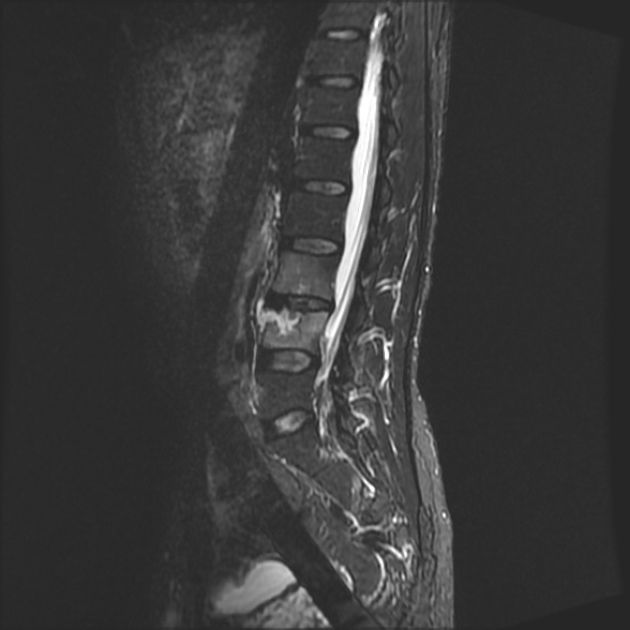
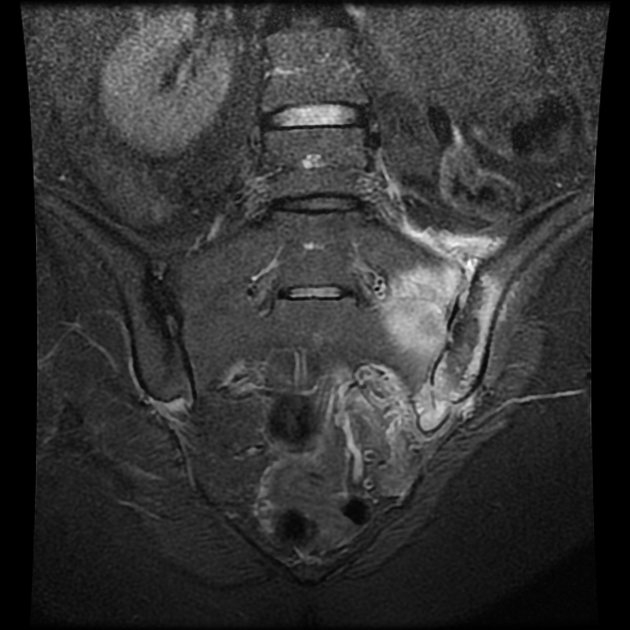
Brucellosis may affect any body part and may be focal or systemic, but it has an affinity for infecting the spine:
-
musculoskeletal manifestations 1,2
spondylodiscitis (in particular of the lumbar spine)
-
CNS manifestations (neurobrucellosis) 3
sensorineural hearing loss (most common)
-
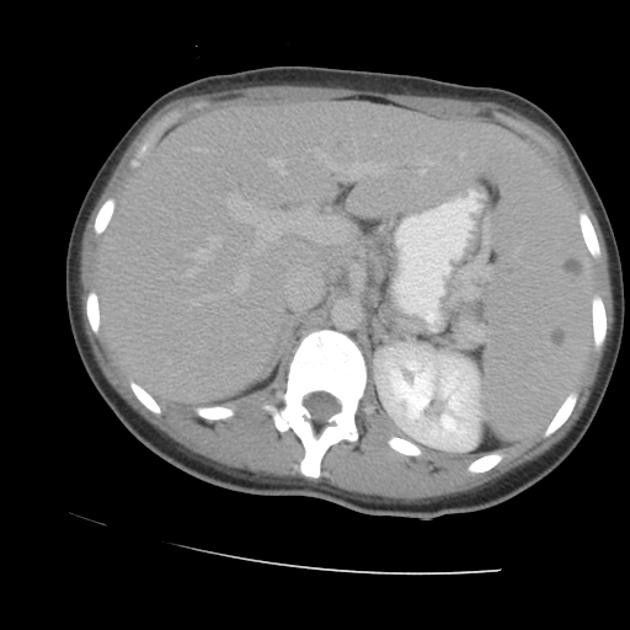
abdominal manifestations 4,5
hepatitis (4%)
splenic brucellosis: splenic abscess or calcified splenic lesion
-
thoracic manifestations
-
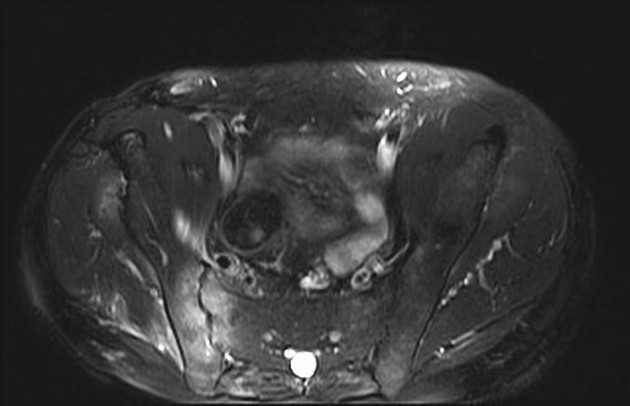
urogenital manifestations 5
-
epididymo-orchitis (10%)
one of the rare causes of an isolated orchitis 8
-
History and etymology
Brucella is eponymously named in honor of the early investigatory work into disease pathogenesis performed by Scottish microbiologist Sir David Bruce (1855-1931), who was born in Melbourne, Australia 9.
Of note, B. abortus is so named as it causes spontaneous abortion in the third trimester in cattle 7.
Historically, brucellosis was also known as undulant fever, but this is rarely used contemporaneously.



 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.