Inferior vena cava filter, or just IVC filter, is an endovascular device that is typically placed in the infrarenal inferior vena cava (IVC) to prevent pulmonary embolism in selected patients. This procedure is most often performed by interventional radiologists under fluoroscopic guidance.
On this page:
Indications
contraindication to anticoagulation, eg active gastrointestinal bleed or recent neurosurgery
pulmonary embolism despite anticoagulation
poor patient compliance with anticoagulation treatment
large iliocaval or floating IVC thrombus “widow-maker” thrombus
A temporary (i.e. retrievable) vena cava filter is typically placed for a short duration, usually weeks to a few months. The design of the temporary filter permits subsequent endovascular retrieval. In certain patients vena cava filters are left in situ indefinitely, these devices may be called permanent filters.
Contraindications
It is uncommon to be unable to place an inferior vena cava filter. Contraindications include:
complete vena cava thrombosis
vena cava is too small or too large to safely admit a filter
septic thromboembolism
Procedure
Preprocedural evaluation
review all available imaging to establish the indication for the procedure; previous studies can help assess IVC patency, size and presence of anomalies such as duplicated IVC and circumaortic renal vein
whilst departmental practices vary, interventionists often place IVC filters without stopping anticoagulation therapy
obtain informed consent for the procedure
arrange analgesia and sedation according to patient's comfort
Positioning/room set up
The procedure is usually performed in the angiography suite with the patient in a supine position. Regular monitoring of the vital signs by a suitably trained staff member is recommended during the procedure. Clean skin with an antiseptic solution and drape to maintain sterility for the procedure.
Equipment
ultrasound machine
18 gauge needle. Alternatively 22 or 21 gauge needle and a micro-puncture access set
0.035" vascular guide wire
multi-sidehole straight or pigtail catheter
commercially available vena cava filter set
Technique
Specific technical steps may vary according to personal preference and the type of filter being used. Generally, the internal jugular or femoral vein is punctured under ultrasound guidance and a guide wire is placed in the IVC. A venogram is obtained by injecting contrast through a multisidehole catheter positioned in the lower IVC or distal common iliac vein. The venogram is used to reassess the IVC for patency, size and anomalies. The location of the renal veins is often indicated by the presence of contrast reflux or flow voids. The venous access is dilated using a dilator. The vena cava filter is subsequently deployed in a suitable location through a delivery sheath, typically the infra-renal IVC. Another venogram is obtained to ensure satisfactory deployment of the filter. The delivery sheath is removed. Hemostasis is secured using manual compression.
Technical considerations in rare cases of a double IVC include bilateral infrarenal IVC filter placement 4. This is the most common approach, however, there is no consensus yet on the most optimal filter placement method ref. Other approaches include placement of the IVC filter in the common suprarenal IVC or embolizing the smaller, non-dominant IVC and then placing the filter in the dominant IVC 5.
Suprarenal placement 6 is reserved for special indications as the suprarenal IVC is wider and shorter and its caliber is more variable (under more influence of the heart). There is no increase in renal dysfunction 7 nor other complications 8 when compared to infrarenal filters. The major indications for suprarenal filter placement are:
pregnant women where an infrarenal filter may be compressed by the gravid uterus, and
pre-existing infrarenal caval thrombus, in which case a suprarenal filter would need to be placed via a jugular approach.
Post-procedure care
Regular monitoring of vital signs is performed for the first few hours after the procedure.
Complications
bleeding
-
filter migration
locations include the heart, intrahepatic IVC, hepatic veins, renal veins and iliac veins 4
filter tilting (which makes removal more difficult)
vena cava injury
vena cava thrombosis 3 and obstruction
pulmonary embolism may occur despite the filter
-
filter fracture
'natural/attritional'' or iatrogenic
fragments may embed in the IVC wall or migrate
insertion and guidewire-related complications







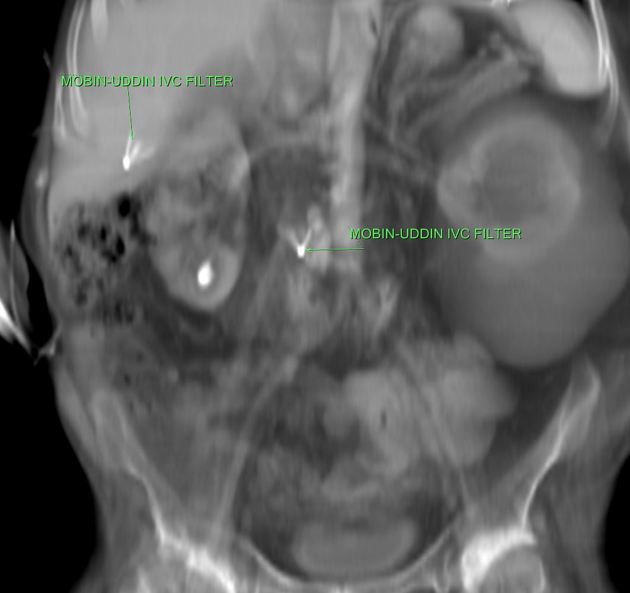
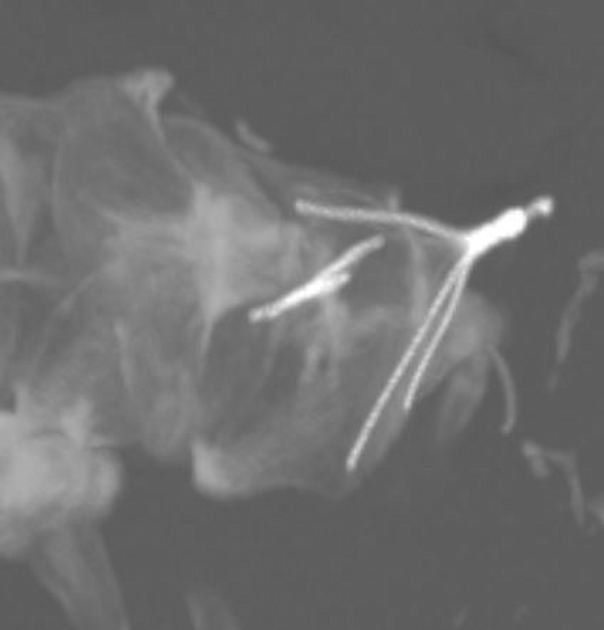
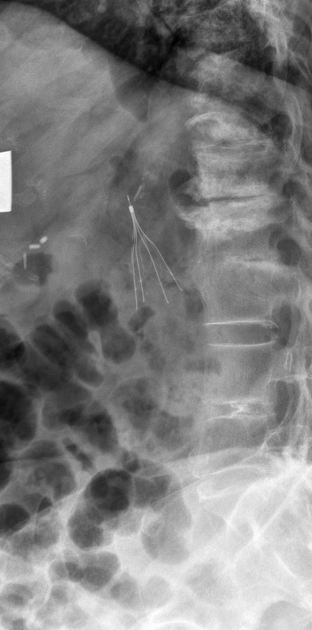

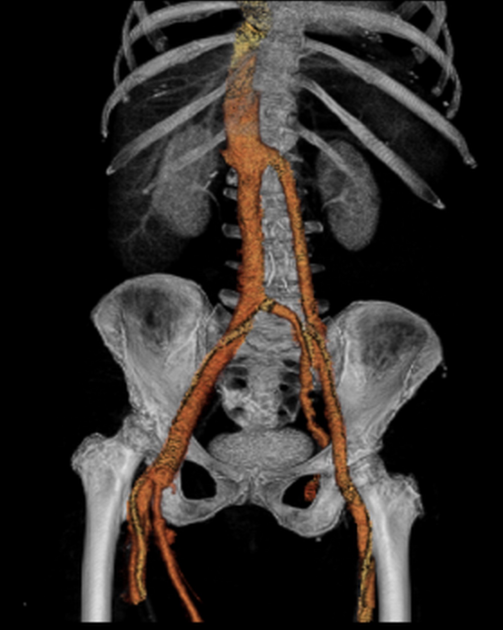
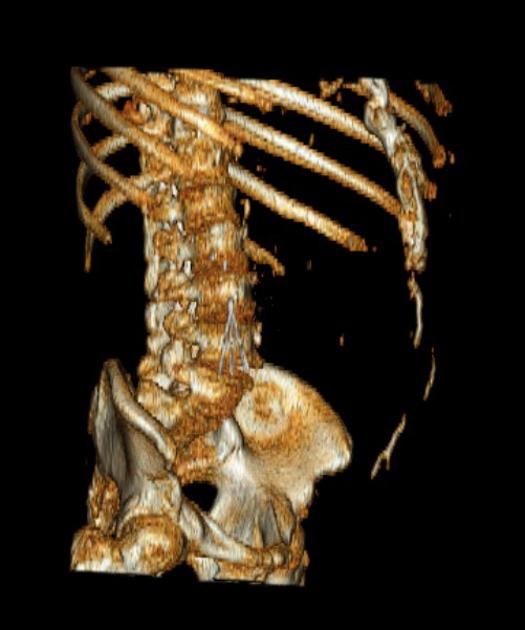
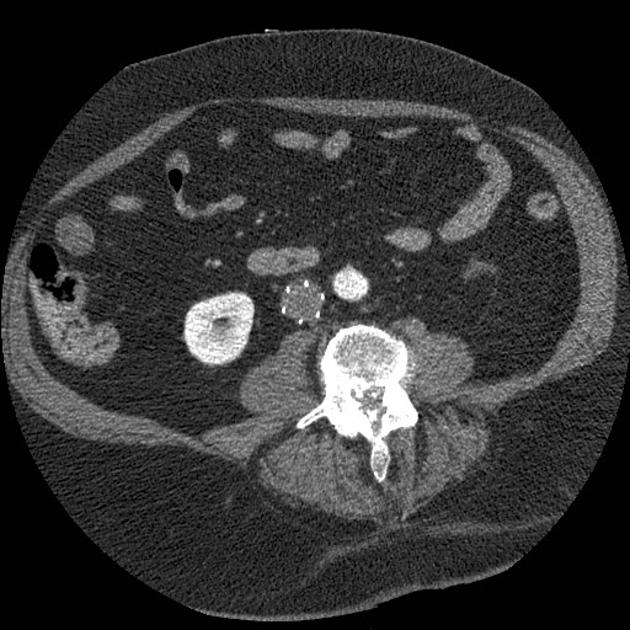
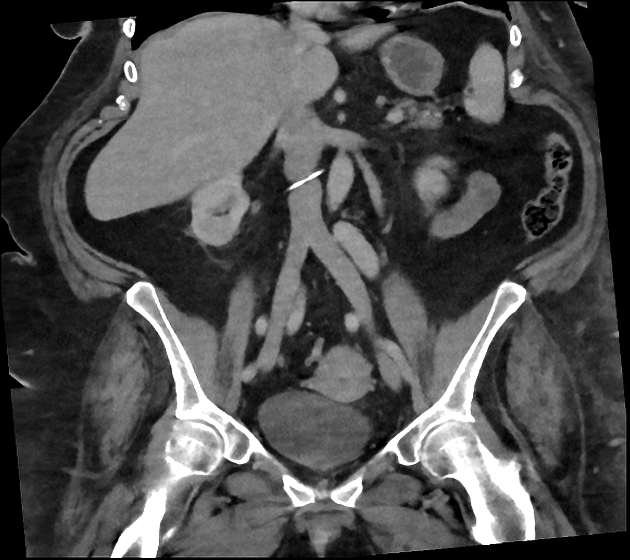


 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.