Ovarian Sertoli-Leydig cell tumors (SLCT), also known as ovarian androblastomas, are a subtype of ovarian sex cord-stromal tumor.
On this page:
Epidemiology
They are rare and only account for ~0.5% of all ovarian tumors. While they can present at any age, they typically present <30 years old, with a mean age of 14 years.
Clinical presentation
In ~30-50% of patients, the presenting symptoms are related to clinical signs of androgenic activity 6. Many patients have symptoms of virilization depending on the quantity of androgen production. A small subset is hyperoestrogenic.
Hormonally inactive tumors often have a nonspecific presentation such as an abdominal mass and/or pain. The majority of patients present with stage I disease.
Pathology
Most tumors are unilateral (>90% of cases) and confined to the ovaries. These tumors are characterized by the presence of testicular structures that produce androgens. However, only 30% are hormonally active.
Ovarian SLCTs can be divided into four subtypes:
- well-differentiated
- intermediately-differentiated
- poorly-differentiated
- retiform
The tumors may contain heterologous elements in approximately 20% of cases. These can, in turn, be further separated into two basic types: endodermal and mesenchymal. Heterologous hepatic differentiation is responsible for elevated AFP levels 11.
Variants
Radiographic features
SLCTs are usually unilateral.
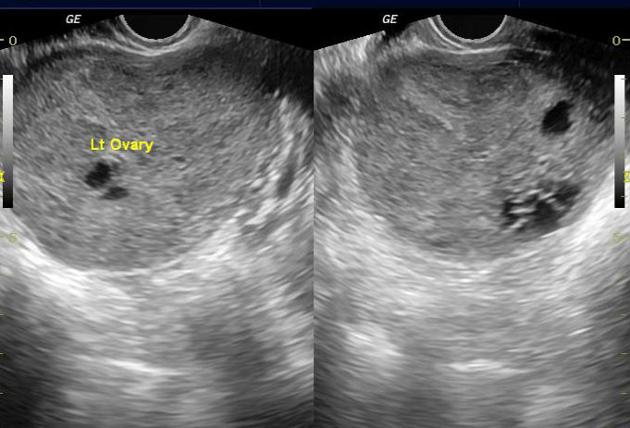
Ultrasound
Imaging features are nonspecific and variable. SLCT may manifest as a well-defined, enhancing solid mass 3 or as a cystic lesion 6. It typically presents as a solid mass with intratumoral cysts.
MRI
The signal intensity on T2-weighted MR images depends on their fibrous content. Most tumors demonstrate predominantly low T2 signal intensity with scattered areas of high signal intensity 5.
Treatment and prognosis
Most tumors are benign although ~10-20% can be malignant.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.