Diastematomyelia, also known as a split cord malformation, refers to a type of spinal dysraphism (spina bifida occulta) characterized by a longitudinal split in the spinal cord.
On this page:
Terminology
Although traditionally, it has been distinguished from diplomyelia (in which the cord is duplicated rather than split), the term split cord malformation is advocated to encompass both conditions 6. For the purposes of this article, the terms diastematomyelia and split cord malformation are used interchangeably.
Epidemiology
Split cord malformations are a congenital abnormality and account for ~5% of all congenital spinal defects 6.
Clinical presentation
The majority of patients with diastematomyelia are symptomatic, presenting with signs and symptoms of tethered cord, although patients with mild type II (see below) may be minimally affected or entirely asymptomatic 6. Presenting symptoms include:
leg weakness
incontinence
Patients with diastematomyelia also frequently have other associated anomalies including:
hemangioma overlying spine
Pathology
The condition is believed to occur during the gastrulation stage of development due to abnormal movement and separation of precursor cells 7. Specifically, it has been thought that a persistent or abnormal adhesion between the ectoderm and endoderm creates an additional neuroenteric canal which in turn leads to the notocord developing into two hemicords 8.
Classification
Split cord malformations are divided into two types according to the division of the dural sac 9:
type I: duplicated dural sac, with midline rigid osseous or cartilaginous spur; usually symptomatic
type II: single dural sac, with midline nonrigid fibrous or fibrovascular septum; impairment less marked
Type I
Type I is the classic diastematomyelia, characterized by 1-6:
duplicated dural sac separated by midline spur (osseous or osteocartilaginous)
hydromyelia: common
vertebral abnormalities: hemivertebrae, butterfly vertebrae, spina bifida, fusion of laminae of adjacent levels
skin pigmentation, hemangioma, and hypertrichosis (hair patch) are common
patients are usually symptomatic presenting with scoliosis and tethered cord syndrome
Type II
Type II is milder than type I, and lack many of the features of the latter:
single dural sac and no rigid spur but rather only a nonrigid fibrous or fibrovascular septum
hydromyelia may be present
spina bifida may be present, but other vertebral anomalies are far less common
patients are less symptomatic or may even be asymptomatic
Radiographic features
Split cord malformations are more common in the lower cord but can sometimes occur at multiple levels.
50% occur between L1 and L3
25% occur between T7 and T12
An associated bony, cartilaginous, or fibrous spur projecting through the dura mater forwards from the vertebral arch is visible in 33% of cases 1.
Vertebral anomalies (spina bifida, butterfly, or hemivertebrae) are common. Laminar fusion associated with a vertebral arch defect is a good predictor of diastematomyelia and occurs at the level of the defect, or at an adjacent level.
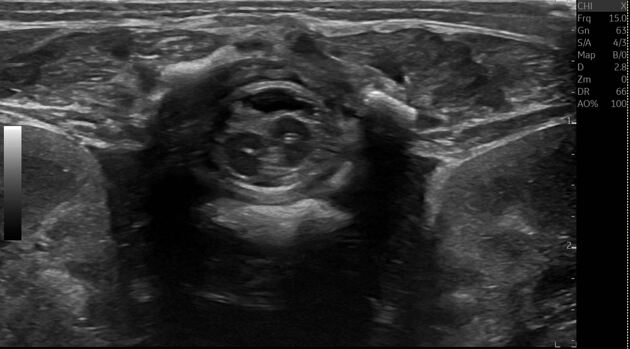
Ultrasound
On antenatal ultrasound, the presence of an extra echogenic focus in the midline between the fetal spinal posterior elements has been described as a reliable sign 2.
Plain radiograph
multilevel spina bifida
widening of interpedicular distance: but this may be remote from the site of the spur
associated scoliosis
anteroposterior vertebral body narrowing
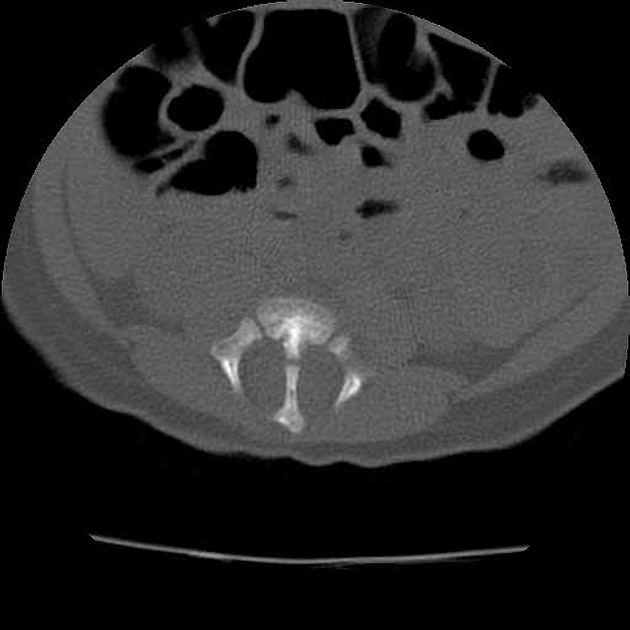
CT
CT is able to better image many of the features seen on plain films and in addition may demonstrate the bony septum.
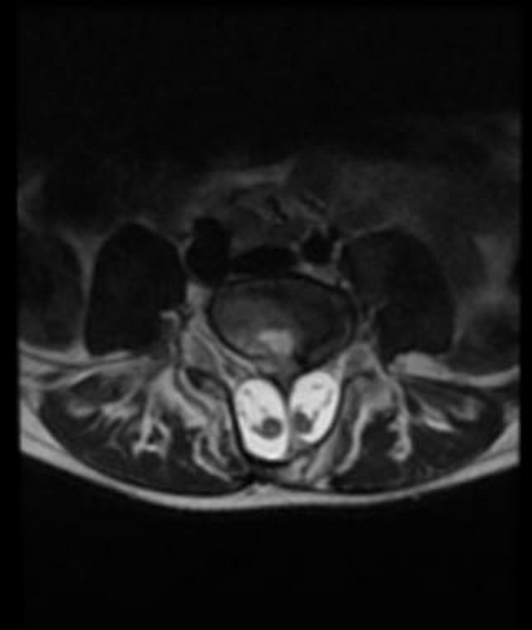
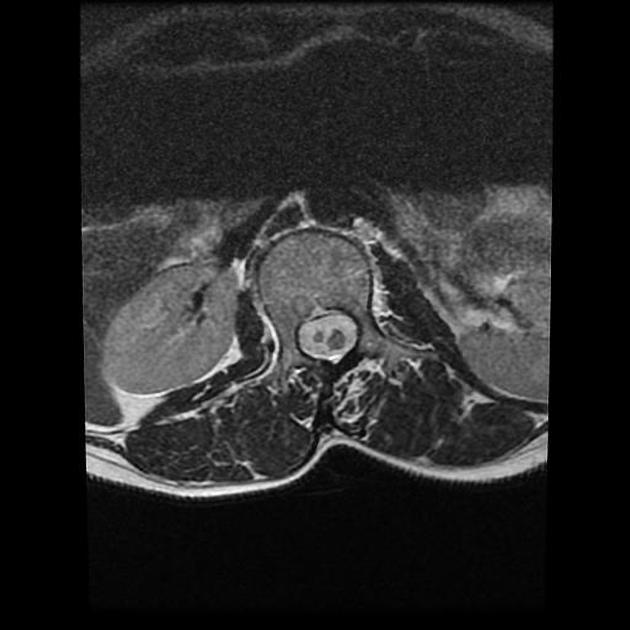
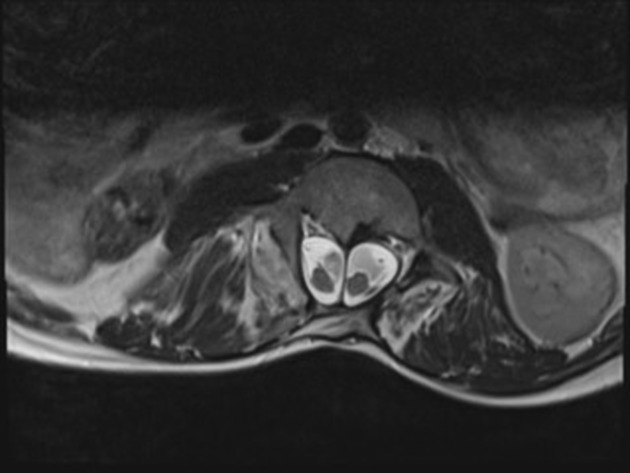
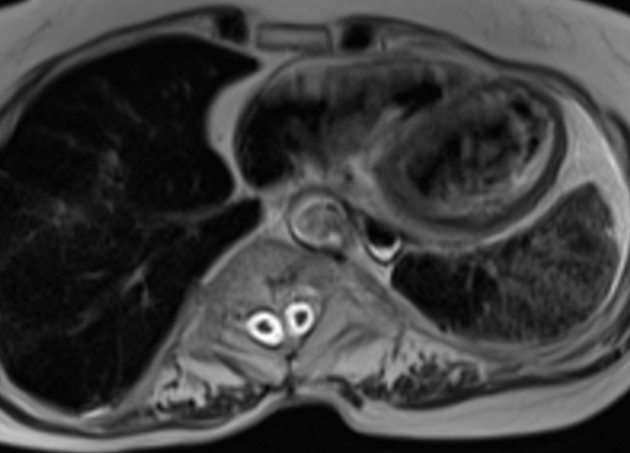
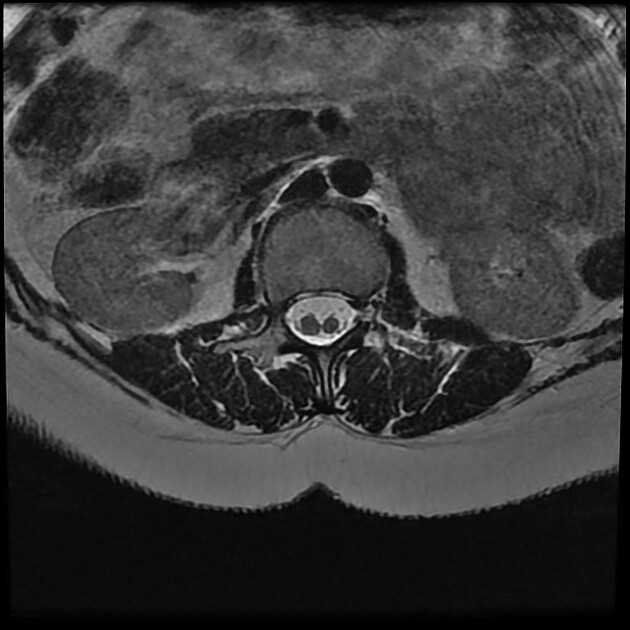
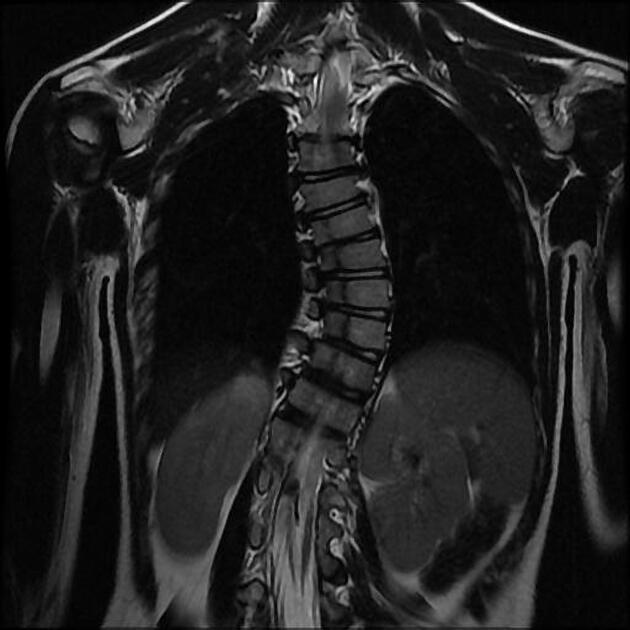
MRI
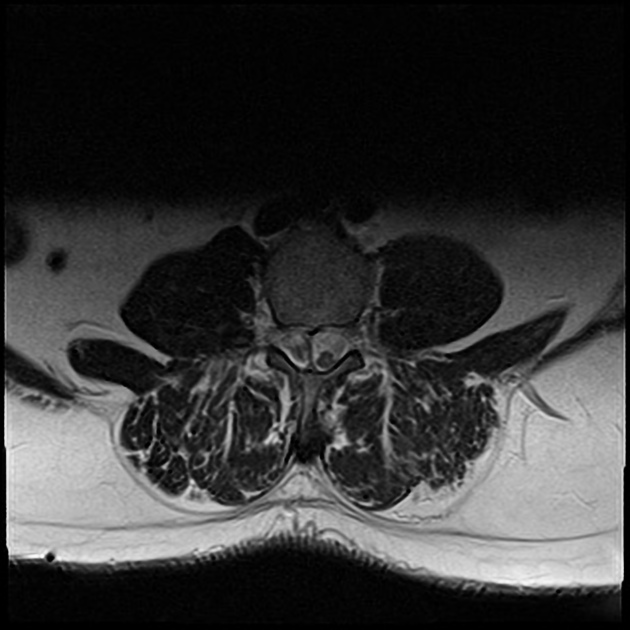
MRI is the modality of choice for assessing children with split cord malformations. As well as being able to elegantly demonstrate the cord and presence of hydromyelia (if present), it can also assess for the presence of the numerous associated anomalies (see above).
History and etymology
The term derives from the ancient Greek word διαστεμα (diastema) meaning cleft 7.
Differential diagnosis
Usually, there is little in the way of a differential diagnosis when the cord has been adequately imaged and features are typical (especially now that diplomyelia is considered part of the same spectrum by many authors 6).





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.