A pilomatricoma is an uncommon, benign neoplasm thought to arise from hair cortex cells.
On this page:
Terminology
It was formerly referred to as pilomatrixoma or calcifying epithelioma of Malherbe.
Epidemiology
the reported incidence of pilomatricoma ranges between 1 in 500-2000
they make up 0.12% of cutaneous neoplasms and 20% of all hair follicle related tumors
more common in females; F:M ratio = 3:2
more common in the Caucasian population
more common in children, but occurrence in adults is increasingly being recognized
bimodal peak during the first and sixth decades of life
usually develops within the first two decades of life with 40% of cases occurring before the age of 10 years and 60% before the age of 20 years
usually solitary but up to 3% are multiple
Associations
Recognized associations include:
myotonic muscular dystrophy (associated with multiple and recurring lesions)
Familial forms may be present.
Clinical presentation
The main clinical features of pilomatricoma are:
painless
slow-growing
superficial
mobile
hard mass
ranges in size from 0.5 to 5 cm in diameter
overlying skin has a bluish-red discolouration
Pathology
Location
Approximately 50% of pilomatricoma cases occur in the head and neck region. This is followed by the upper extremities, trunk and the lower extremities. Less commonly seen in the frontal, temporal, cheek, periorbital and preauricular areas.
Macroscopic appearance
A pilomatricoma is usually a well-circumscribed nodulocystic tan-colored mass containing irregularly shaped, lobulated islands of cells separated by fine, fibrovascular connective tissue stroma.
Microscopic appearance
Microscopically pilomatricoma demonstrates:
peripheral basaloid cells, which are darkly stained, round or elongated, with indistinct cell borders and minimal cytoplasm; they contain round to ovoid deeply basophilic nuclei with most showing prominent nucleoli
central ghost cells with abundant, pale, eosinophilic cytoplasm and well-defined cell borders and a central clear area
Variants
Pilomatrix carcinoma = malignant pilomatricoma (rare)
Radiographic features
Plain radiograph
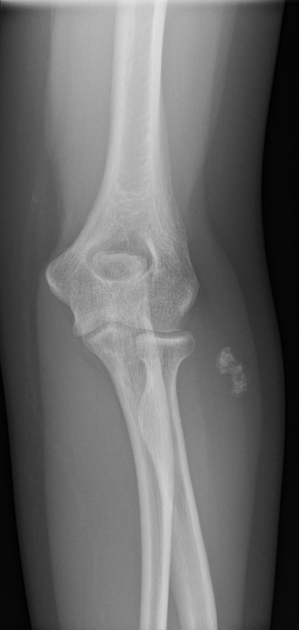
pilomatricomas may show non-specific soft tissue calcification
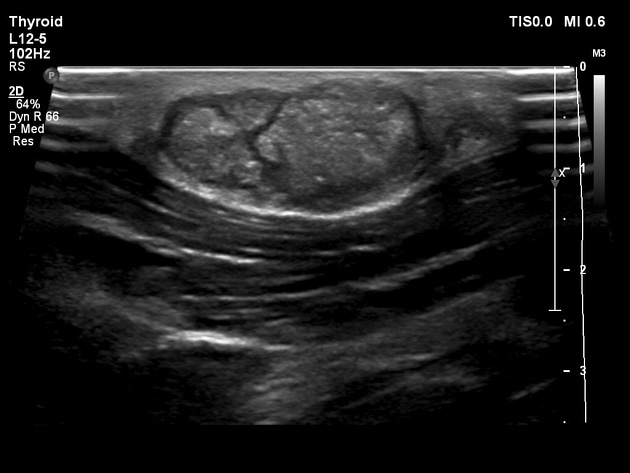
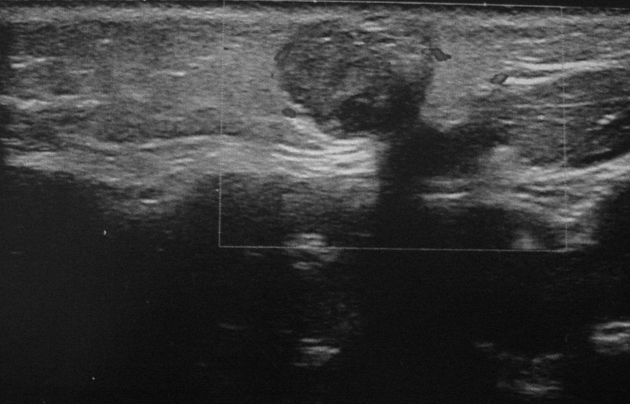
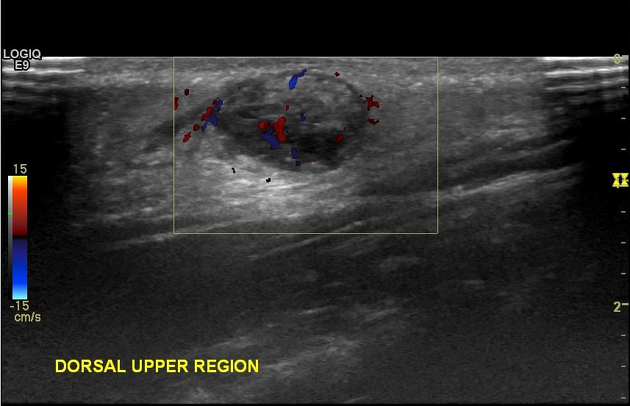
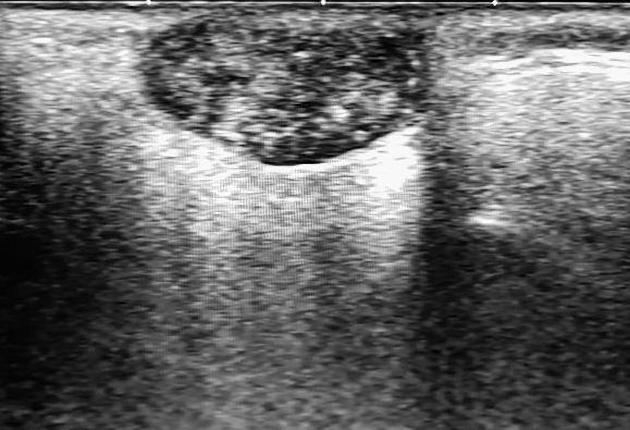
Ultrasound
Pilomatricomas may be seen as
ovoid complex mass, often with calcification, at the junction of the dermis and subcutaneous fat with focal thinning of the overlying dermis
appear as target lesions with a hypoechoic connective tissue capsule and central hyperechoic epithelial cells
CT
pilomatricomas tend to be well-defined, subcutaneous tumors with microcalcifications
MRI
T1: uniform, homogeneously low to intermediate to high signal
T2: variable appearance either inhomogeneous with multiple areas of intermediate signal or homogeneous with either intermediate signal intensity or high signal radiating from the center
T1 C+ (Gd): variable post-contrast T1 appearance, where some only enhance peripherally
Treatment and prognosis
Surgical resection is often curative for pilomatricomas.
History and etymology
A pilomatricoma was first described by Malherbe and Chenantias in 1880, as a subcutaneous tumor, and was shown to be a derivative from hair cortex cells in 1942 by Turhan and Krainer.
The root of the term pilomatricoma is derived from the Latin word 'pilus' meaning hair.
Differential diagnosis
General imaging differential considerations of a pilomatricoma include:
dermoid cyst
foreign body reaction
degenerating fibroxanthoma
metastatic bone formation









 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.