Pneumonectomy is a radical lung surgery involving complete surgical removal of the lung. It is most commonly performed for primary lung malignancy. The lung is removed in its entirety providing the patient has adequate pulmonary reserve from the contralateral lung.
On this page:
Radiographic features
The typical course of possible appearances on imaging following pneumonectomy are:
acutely, there is partial filling of the hemithorax with a combination of fluid, air/gas and contralateral lung and mediastinum
mediastinal shift occurs gradually accompanied by hyperinflation of the contralateral lung and herniation
-
sequential chest radiographs should demonstrate increasing fluid and decreasing gas within the pneumonectomy space, which is evident by a gas-fluid level which gradually rises
if the gas-fluid level starts to lower, a bronchopleural fistula is suspected
-
sequential chest radiographs should demonstrate gradual volume loss on the pneumonectomy side
if there are signs of increasing volume on the side of the pneumonectomy, then bronchopleural fistula, empyema or hemorrhage is suspected
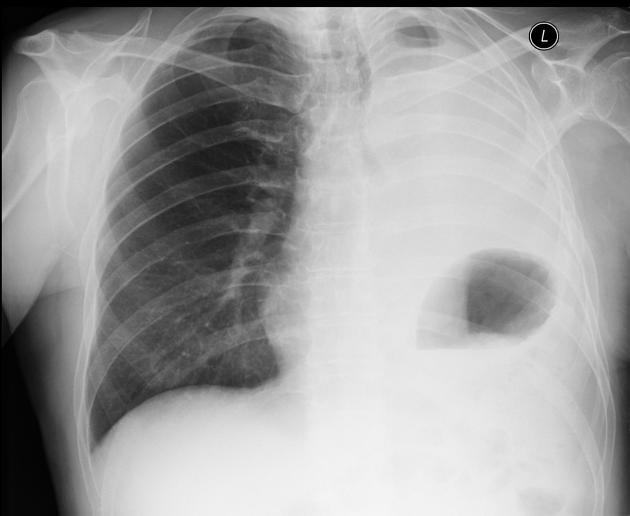
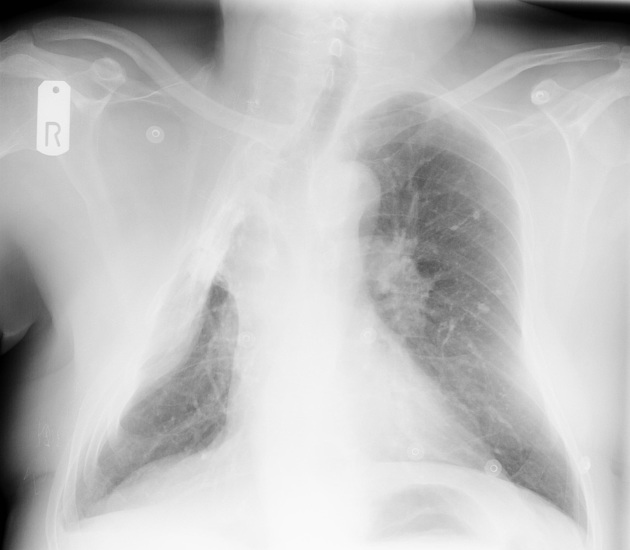
Plain radiograph
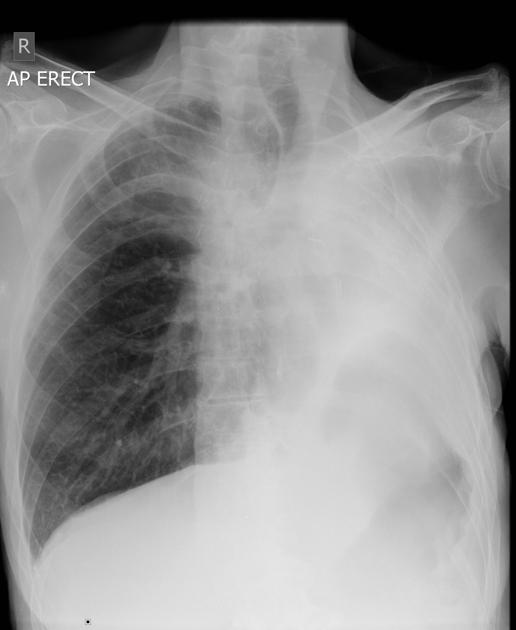
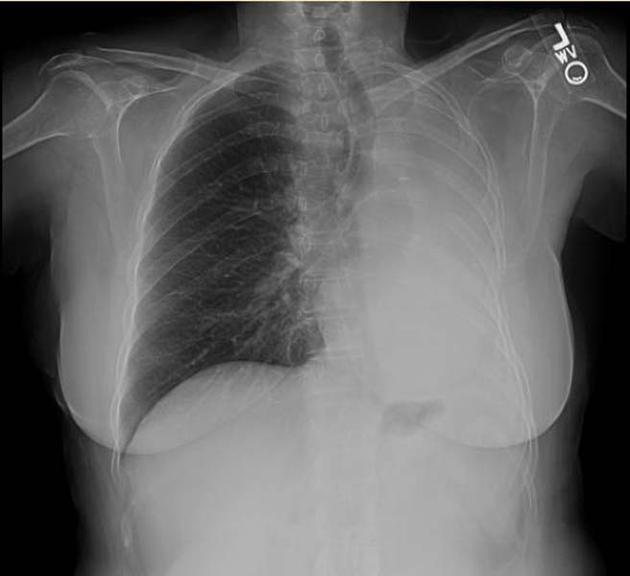
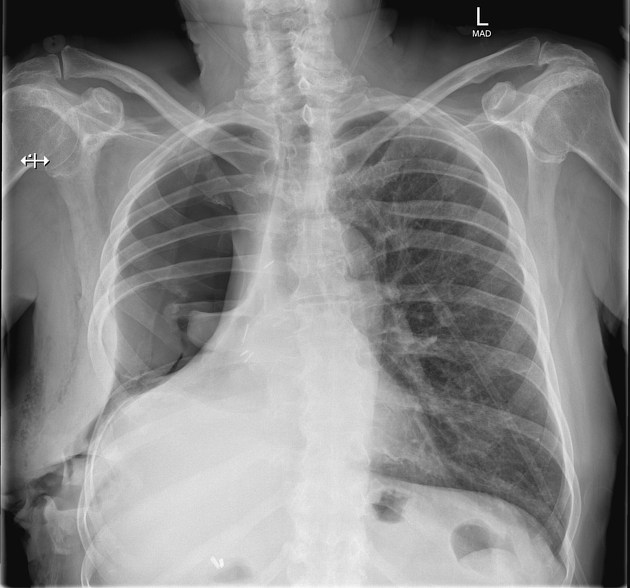
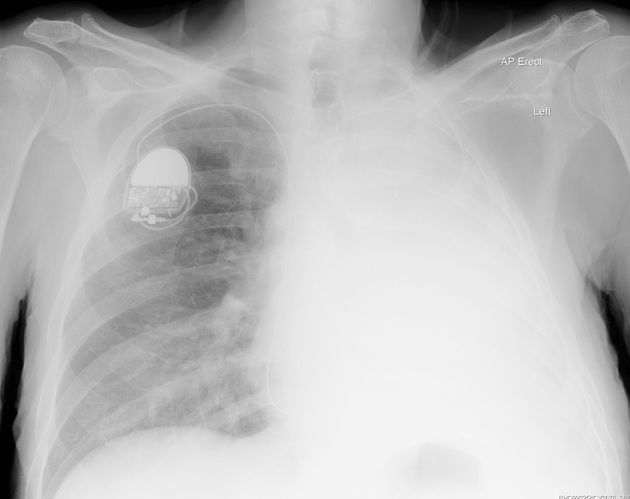
Pneumonectomy is one of the causes of a white out of the hemithorax. The hemithorax is completely opacified with the trachea pulled towards the side of the abnormality. Surgical clips may be identified at the lung hilum.
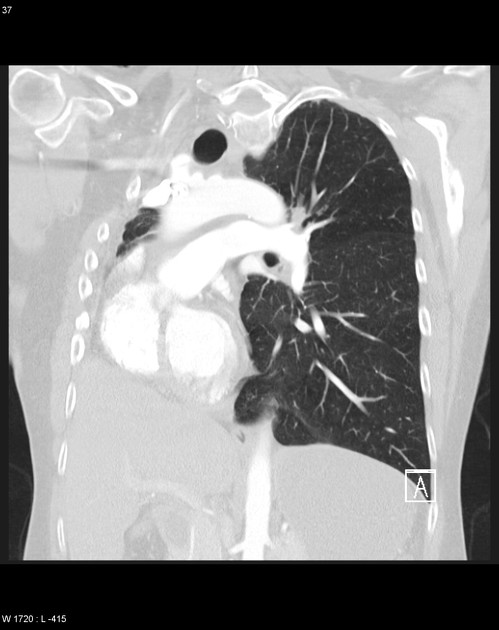
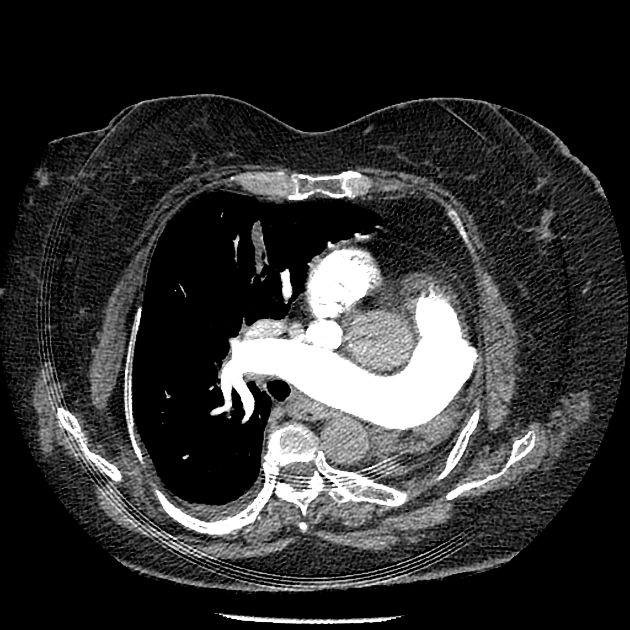
CT
The lung is absent on the side of surgery, with resultant mediastinal shift and compensatory hyperinflation of the contralateral lung.
Complications
Recognized post-pneumonectomy complications include:
bronchopleural fistula formation
recurrent pneumothorax






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.