Caroticocavernous fistulas represent abnormal communication between the carotid circulation and the cavernous sinus. They can be classified as direct or indirect which are separate conditions with different etiologies.
On this page:
Epidemiology
Direct caroticocavernous fistulas are often secondary to trauma, and as such the demographics reflect the distribution of head trauma, most commonly seen in young male patients. The presentation is acute and symptoms develop rapidly.
In contrast, indirect caroticocavernous fistulas have a predilection for the postmenopausal female patient and the onset of symptoms is often insidious.
Other conditions that predispose to increased risk include:
Clinical presentation
pulsatile exophthalmos: ~75% 3
chemosis and subconjunctival hemorrhage
progressive visual loss: 25-32% 3
pulsatile tinnitus (usually objective)
subarachnoid hemorrhage, intracerebral hemorrhage, otorrhagia, epistaxis: ~5% 3
Pathology
Caroticocavernous fistulas can be classified according to various features:
flow: high flow vs low flow
etiology: spontaneous vs traumatic
vascular anatomy
Of these, vascular anatomy is most frequently used and most broadly divides caroticocavernous fistulas into two main types:
direct: direct communication between intracavernous ICA and cavernous sinus
indirect: communication exists via branches of the carotid circulation (internal carotid artery or external carotid artery)
The Barrow classification of caroticocavernous fistulas further characterizes fistulas according to angiographic features:
type A: direct connection between the intracavernous internal carotid artery and cavernous sinus
type B: dural shunt between intracavernous branches of the internal carotid and cavernous sinus
type C: dural shunts between meningeal branches of the external carotid artery and cavernous sinus
type D: type B and type C combined
Direct (Barrow type A)
A direct fistula is due to direct communication between the intracavernous internal carotid artery and the surrounding cavernous sinus. There are a number of causes, however, aneurysm rupture and trauma are by far the most common:
ruptured intracavernous carotid artery aneurysm
trauma (including surgery/angiography)
-
other causes include
Indirect (Barrow types B, C, D)
Indirect fistulas are due to communication by multiple branches between the internal and/or external carotid arteries and the cavernous sinus. The most frequent are type C, with meningeal branches of the external carotid forming the fistula 3.
They are postulated to occur secondary to cavernous sinus thrombosis with revascularization and thus are similar to dural arteriovenous fistulas elsewhere. Other predisposing factors appear to be pregnancy, surgical procedures in the region, and sinusitis 3.
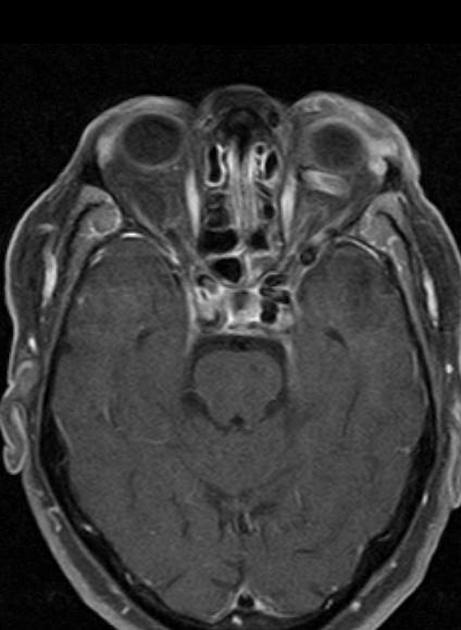
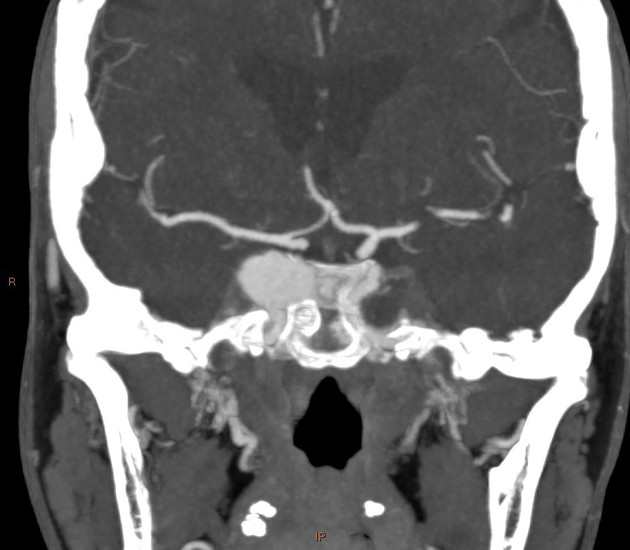
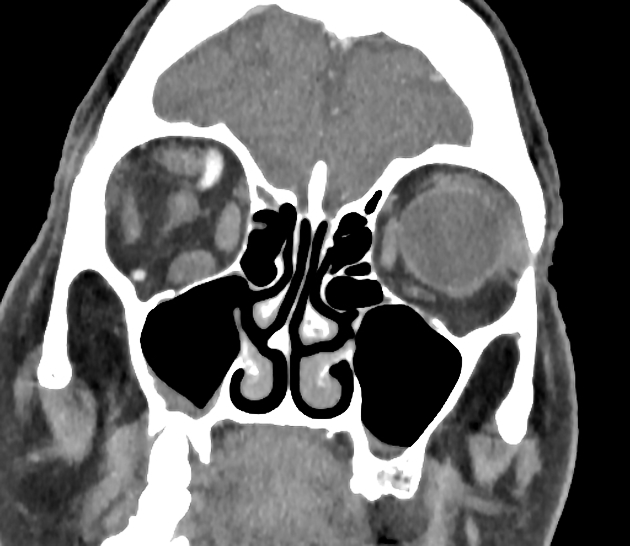
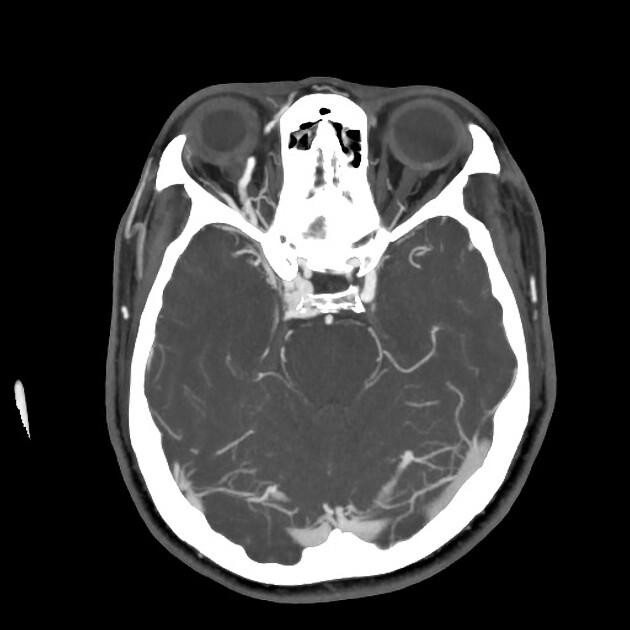
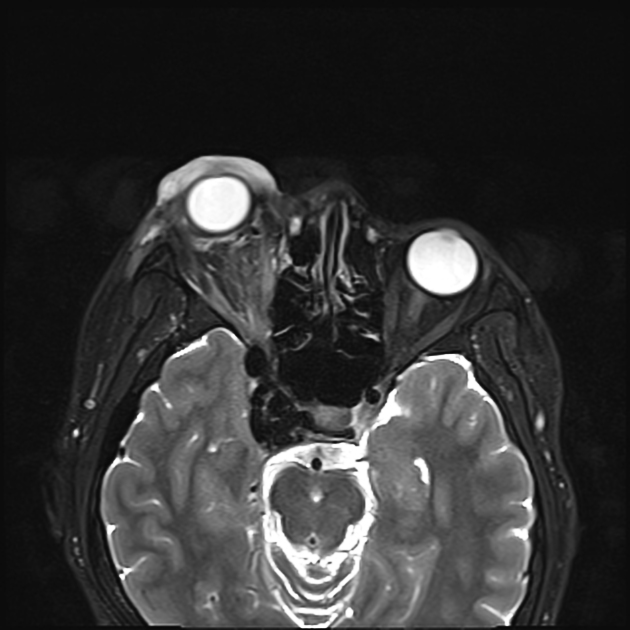
Radiographic features
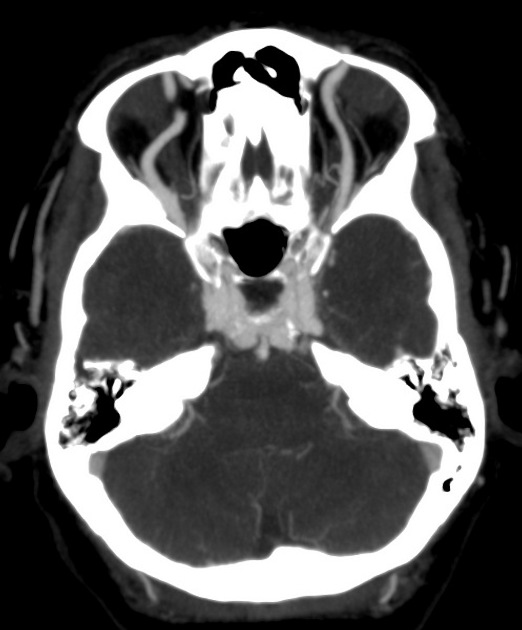
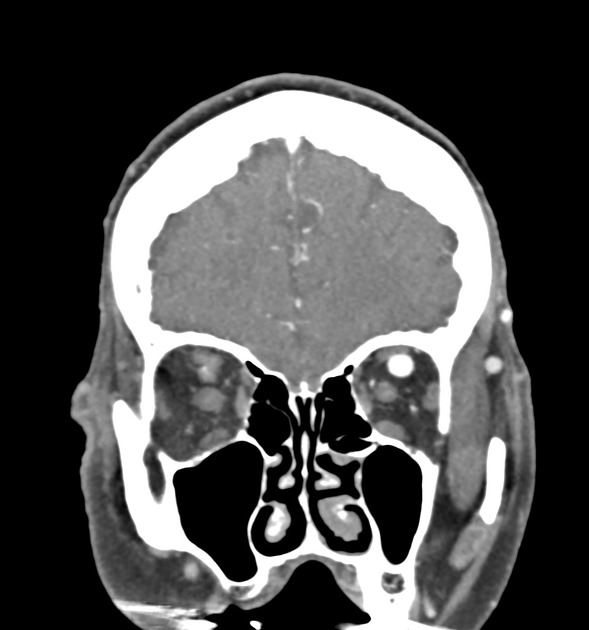
CT
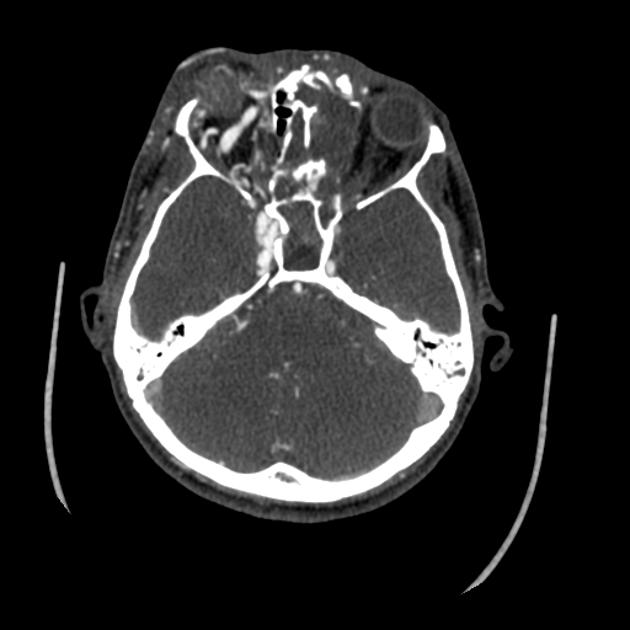
CT angiography is the noninvasive imaging modality of choice for evaluation of suspected caroticocavernous fistula 9. Features include
-
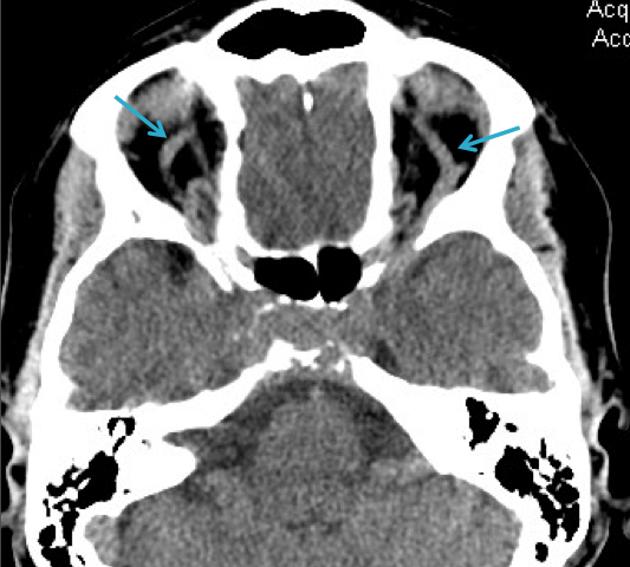
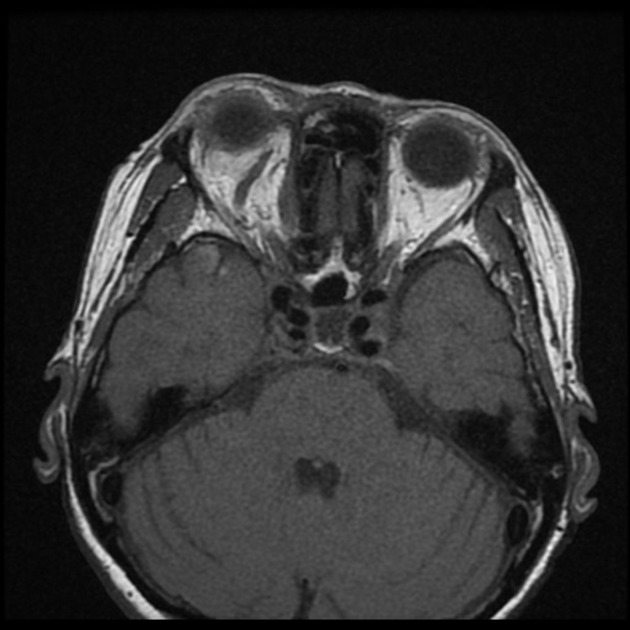
orbital congestion
retrobulbar fat stranding/edema
enlargement of extraocular muscles
-
venous engorgement and enhancement 10
bulging cavernous sinus
asymmetric enhancement of cavernous sinus with attenuation similar to that of internal carotid artery and higher than that of transverse sinus
dehiscent internal carotid artery (for direct type fistulas): snowman appearance of fistula tract involving the feeding carotid artery and draining venous pouch 10
intracranial hemorrhage from a ruptured cortical vein
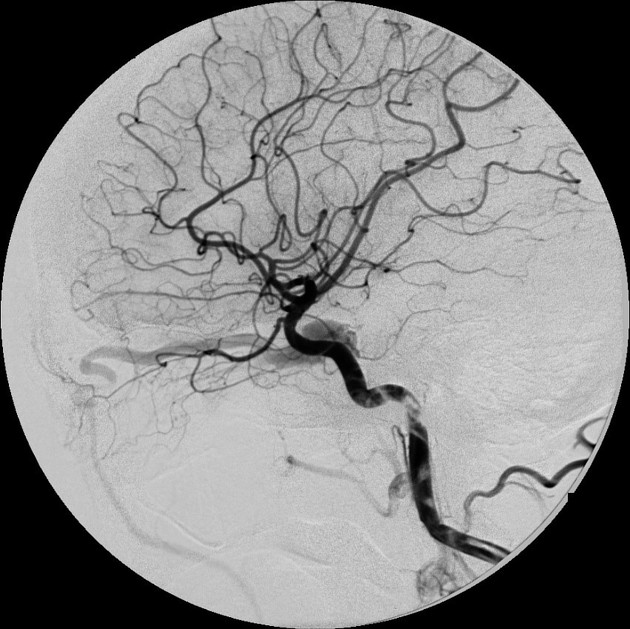
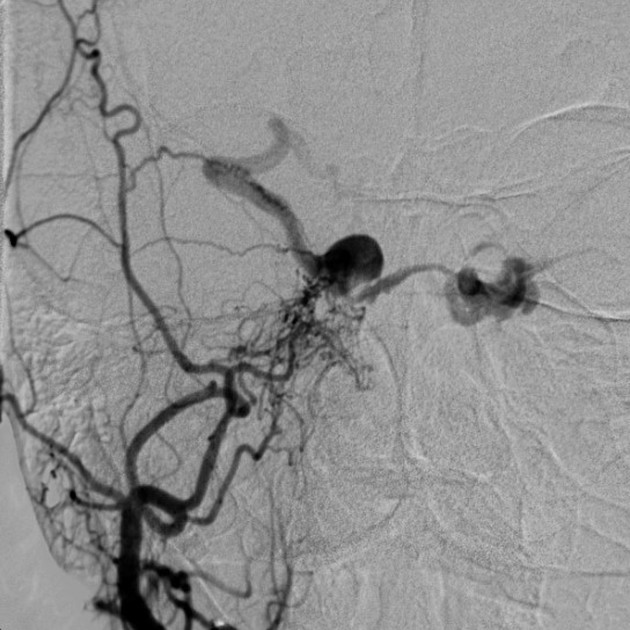
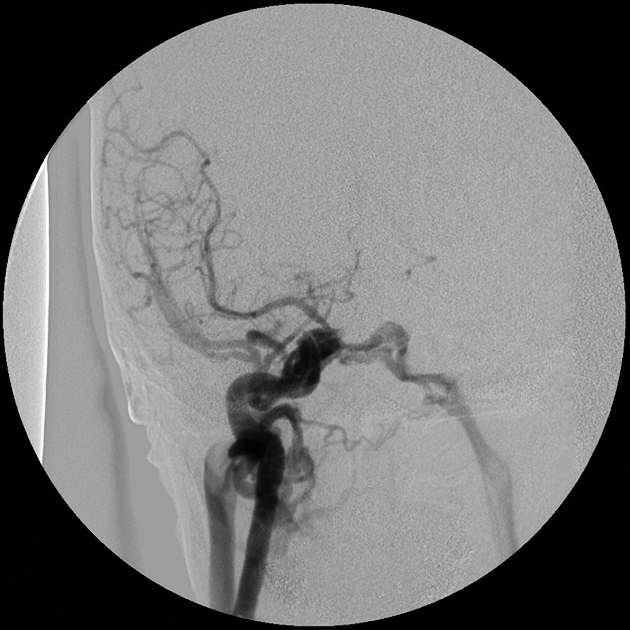
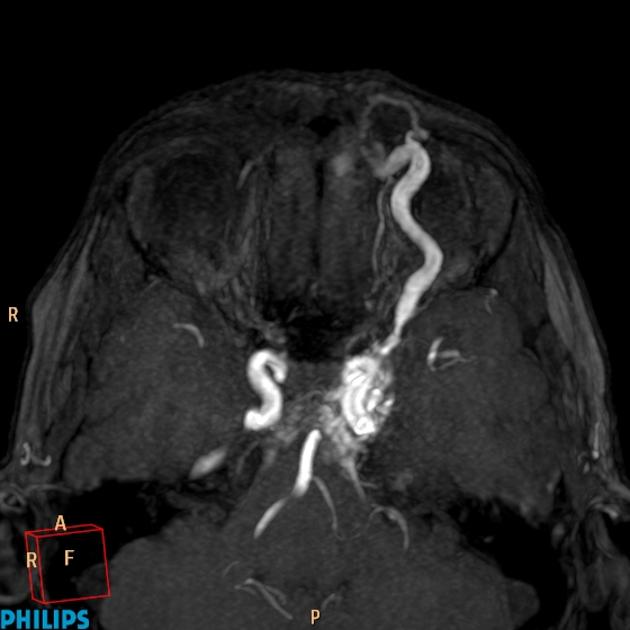
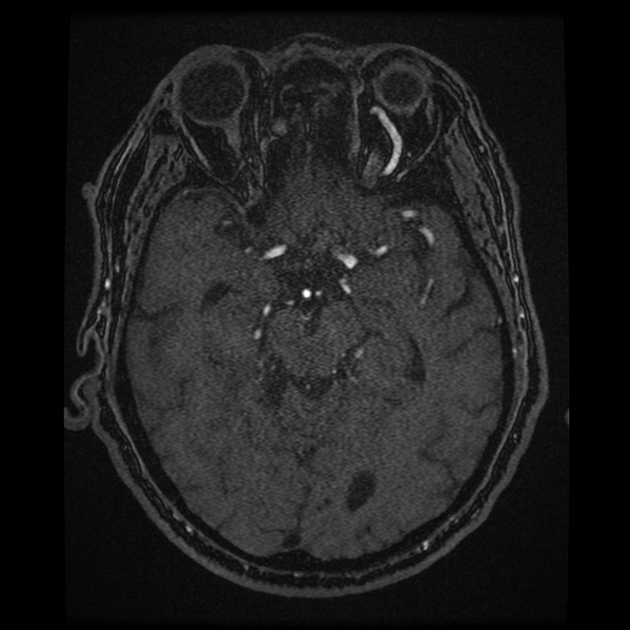
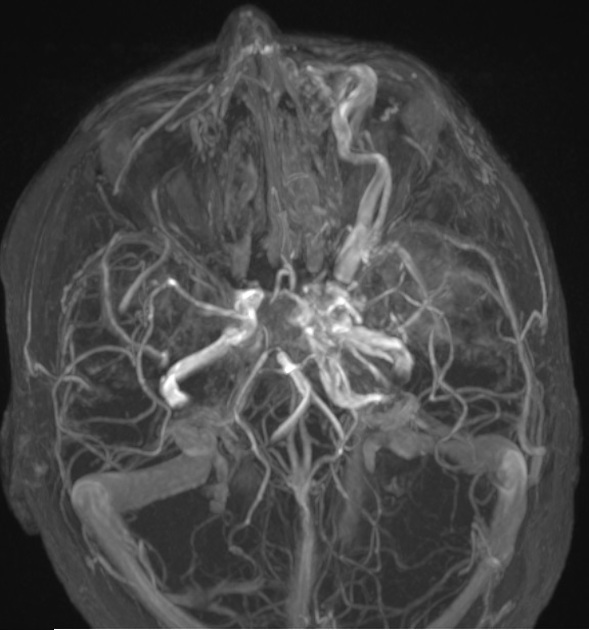
Angiography (DSA)
Catheter-based digital subtraction angiography is the gold standard imaging technique due to its superior spatial and temporal resolution.
rapid shunting from internal carotid artery to cavernous sinus
enlarged draining veins
retrograde flow from cavernous sinus, most commonly into the ophthalmic veins
Ultrasound
Doppler assessment may show arterialized enlarged ophthalmic veins.
Treatment and prognosis
The natural history of caroticocavernous fistulas is highly varied, ranging from spontaneous closure to rapidly progressive symptoms. As such therapy is similarly variable ranging from conservative expectant management to emergent endovascular or surgical intervention.
Conservative management
As a proportion of low flow caroticocavernous fistulas spontaneously close initial conservative management of ocular symptoms is often first employed provided no high-risk features (e.g. aneurysms of feeding vessels) or severe ocular or intracranial complications are present 6.
Carotid compression therapy
In addition to conservative measures, carotid-jugular compression (at the level of the carotid bulb) can be useful in the treatment of indirect fistulas resulting in closure in up to 30% of cases, presumably due to progressive thrombosis due to intermittent stagnation of blood adjacent to existing clot. In contrast, it is only successful in 17% of direct fistulas, presumably due to the higher flow through larger defect 3. It is important that atherosclerotic disease of the carotid bifurcation is excluded prior to the commencement of compression 6. Patients are instructed to compress the carotid bulb for 10 seconds four to six times an hour 6. Compression should be performed with the contralateral hand so that if symptomatic hemispheric ischemia occurs the transient paralysis results in cessation of compression.
Endovascular treatment
Endovascular management is the mainstay of treatment for patients that fail or are not suitable for conservative management and compression therapy 6.
Two main approaches are available, depending on the anatomy of the fistula: transarterial embolization or transvenous embolization.
Direct fistulas
Treatment of direct fistulas requires the occlusion of the tear in the internal carotid artery. This can be achieved in a variety of ways 6:
transarterial covered stent or flow-diverting stent placement in the internal carotid artery 7
transarterial placement of a detachable balloon through the defect into the cavernous sinus
transarterial or transvenous coil or other embolic material placed through the defect obliterating the cavernous sinus
transarterial occlusion of the internal carotid artery
Indirect fistulas
Indirect fistulas require either transarterial occlusion of feeding arterial branches and/or transvenous occlusion of the cavernous sinus 6. Transvenous access can be challenging and may require access via the superior ophthalmic vein (sometimes with the aid of surgical exposure), inferior ophthalmic vein, lateral pterygoid plexus, superior petrosal sinus 6. Occasionally flow-diverting stents can be used to treat indirect fistulas if no other transarterial or transvenous approaches are available 8.
Surgical treatment
Surgery is relegated in most institutions for cases where endovascular management is unsuccessful or impossible. Treatment may involve ligation or trapping of involved arterial segments 3
Complications
Spontaneous hemorrhage can be subarachnoid hemorrhage, intracerebral hemorrhage or extracranial hemorrhage (e.g. epistaxis or otorrhagia).
Ocular complications are also common and often one of the driving factors in embarking upon treatment.
History and etymology
From the Latin, fistula means tube or pipe 11.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.