Foreign bodies are objects lying partially or wholly within the body that originated in the external environment. Foreign body placement is voluntary or involuntary. Although implanted medical devices represent foreign bodies in the broad sense of the term, these have their own set of articles (see below).
On this page:
Images:
Pathology
Etiology
There are many ways in which a foreign body can be introduced into various parts of the human body.
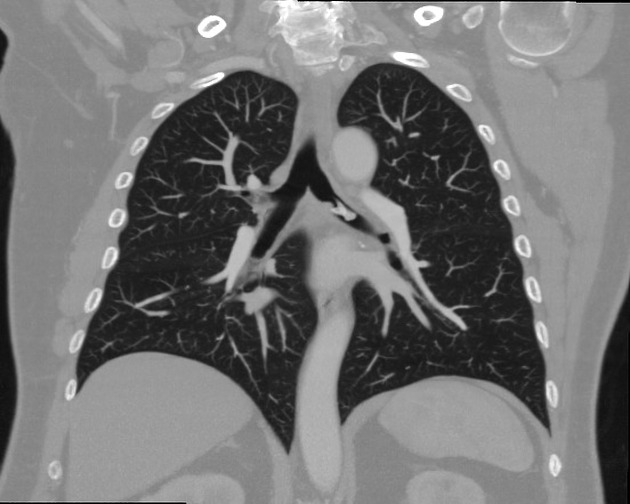
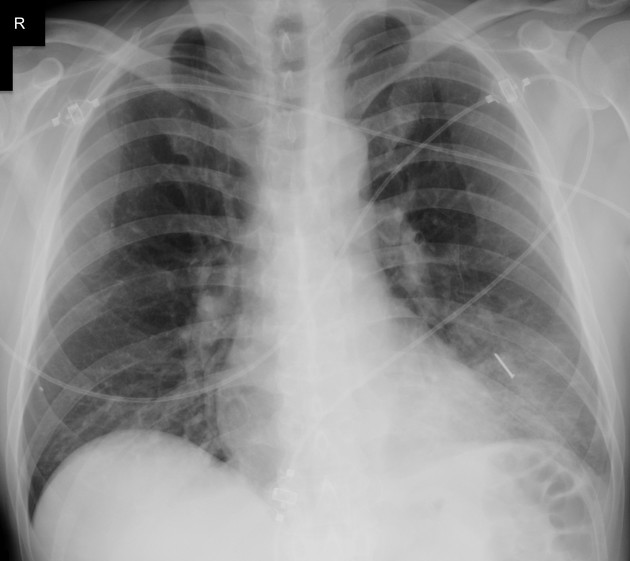
Aspirated
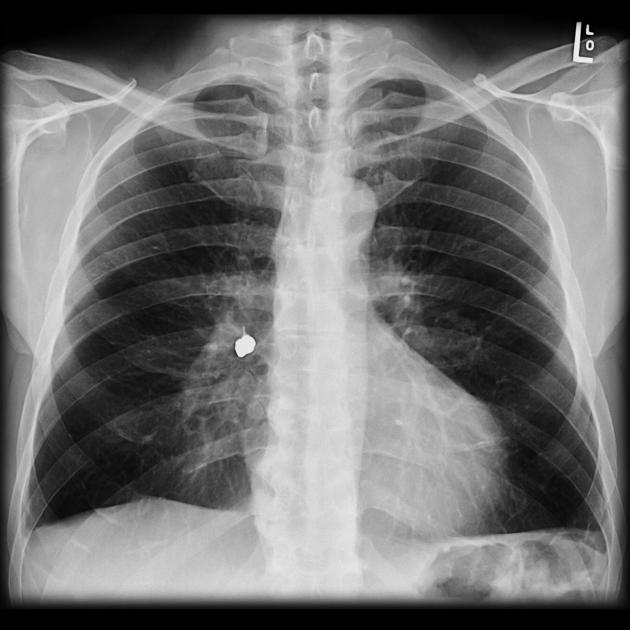
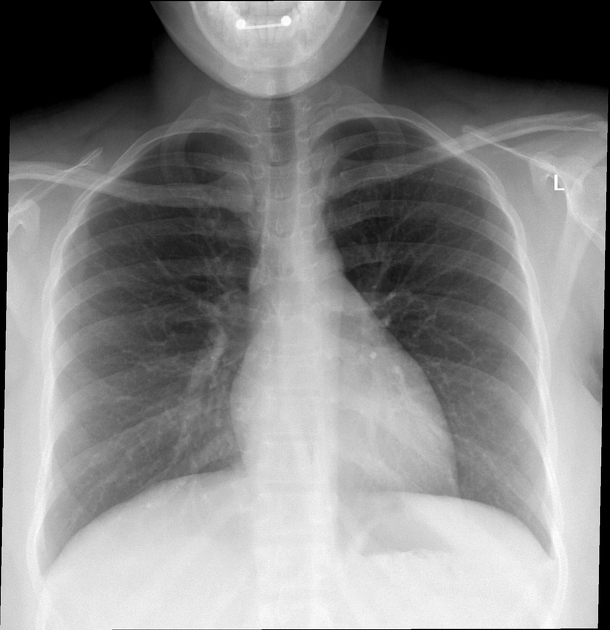
Aspirated foreign bodies will have a clear clinical correspondence: choking, coughing, neck pain or struggling to breathe. Risk factors for foreign body aspiration include intubation, neurological deficit, facial trauma, and dental instrumentation. The right main bronchus is the most common site of obstruction due to the anatomy of the bronchial tree favoring the right side (larger diameter, more vertical orientation). Often two orthogonal plain radiographs are the primary investigation of choice 12.
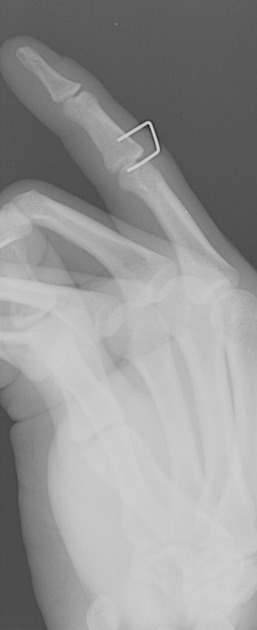
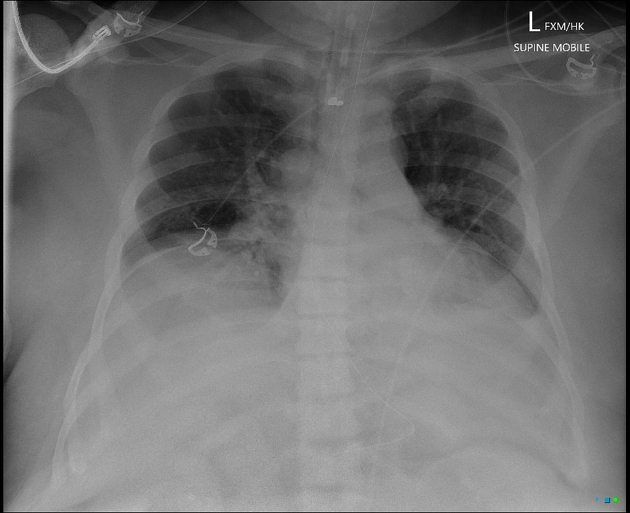
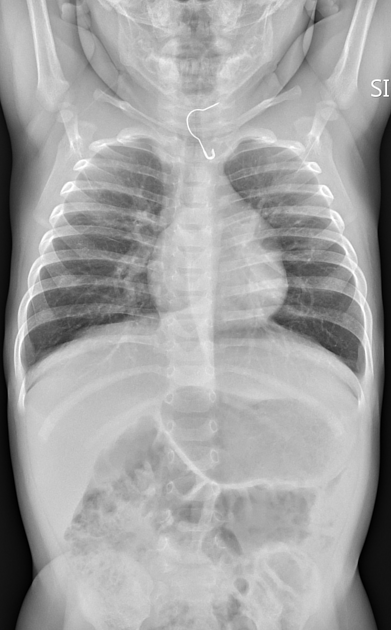
Iatrogenic
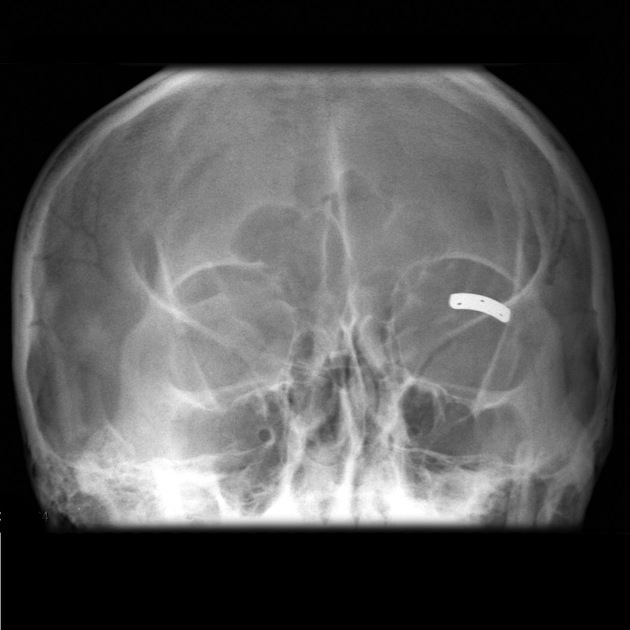
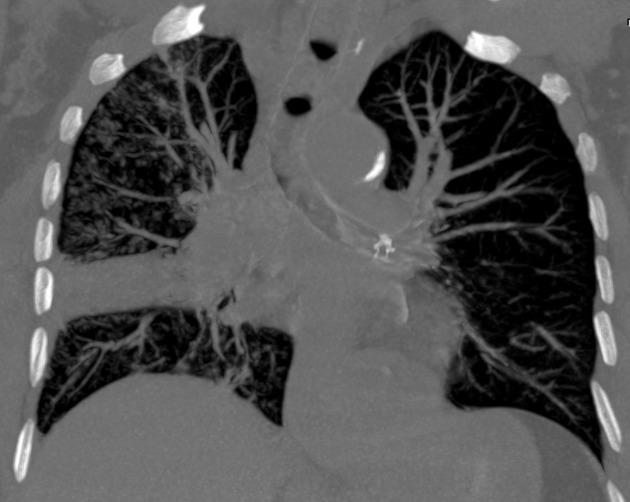
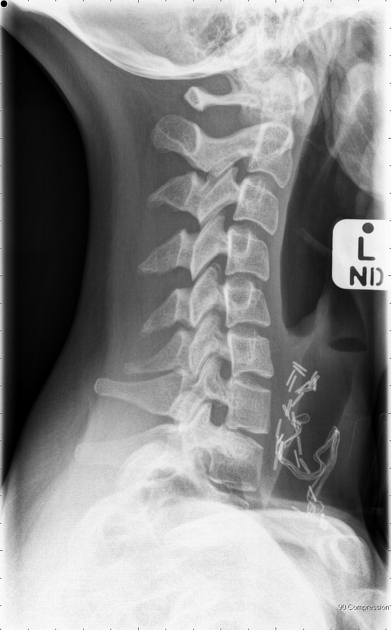
Many surgical procedures deliberately introduce foreign bodies either in the form of hemostatic clips (most common), stents, valve replacements, pacing boxes, catheters, etc. or accidentally when a surgical instrument or surgical pack is inadvertently left in situ.
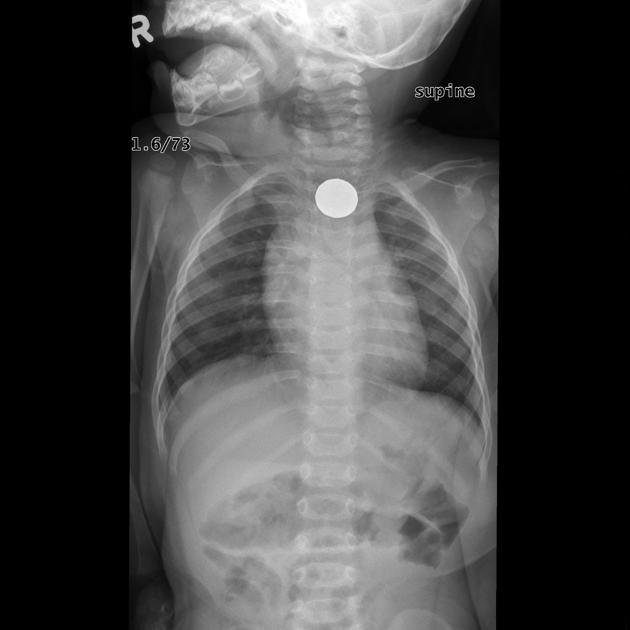
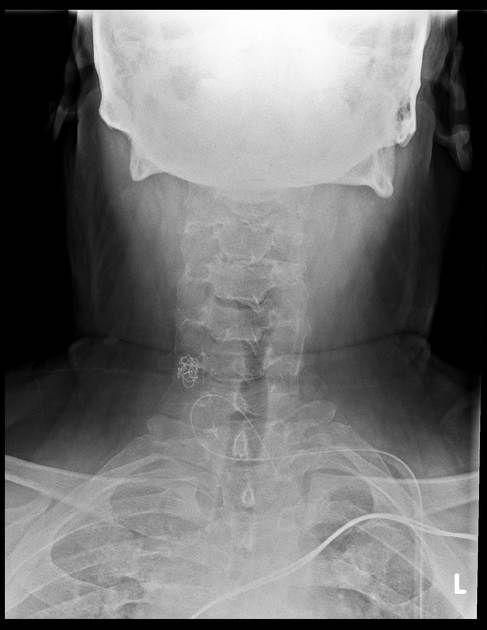
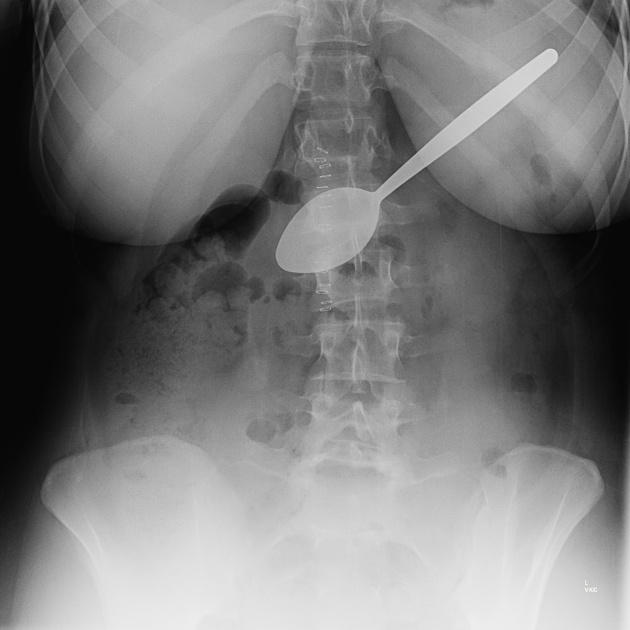
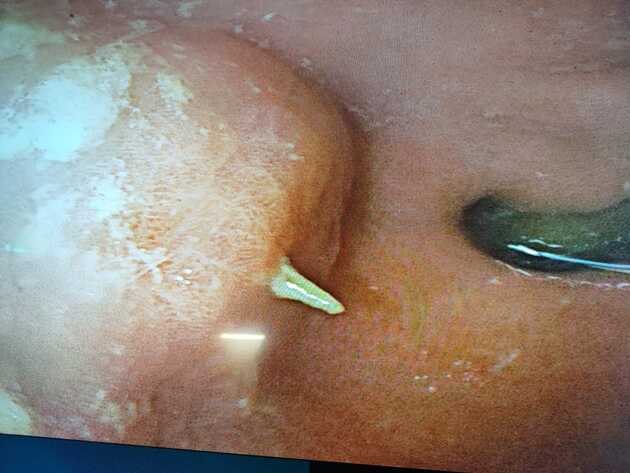
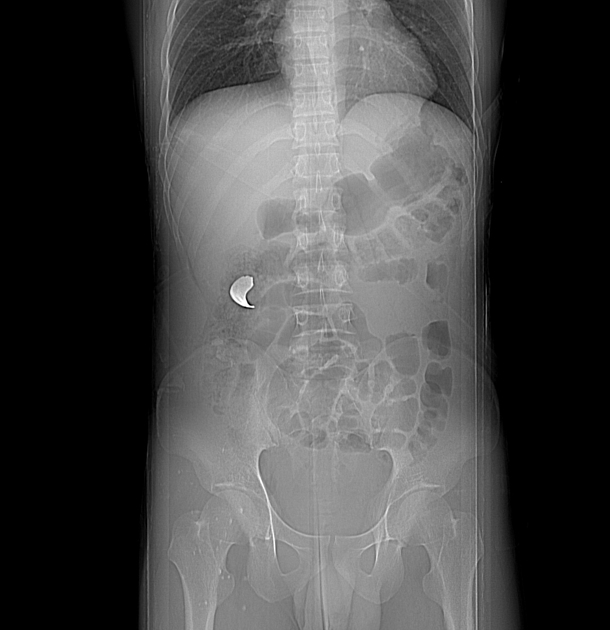
Ingested
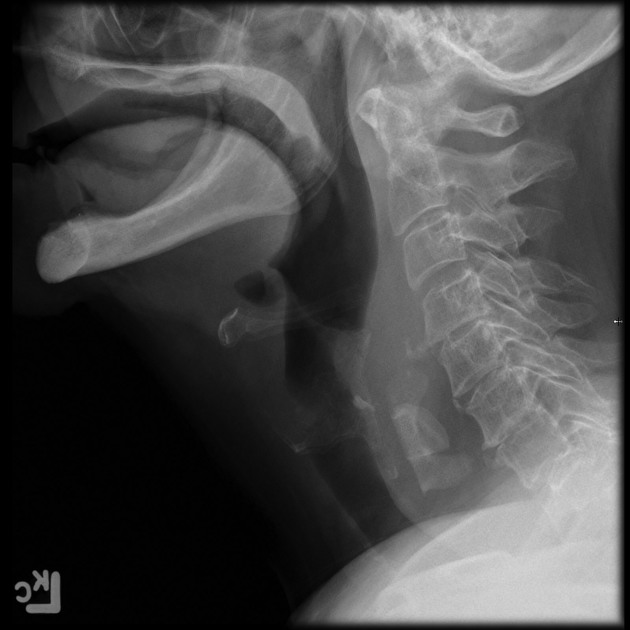
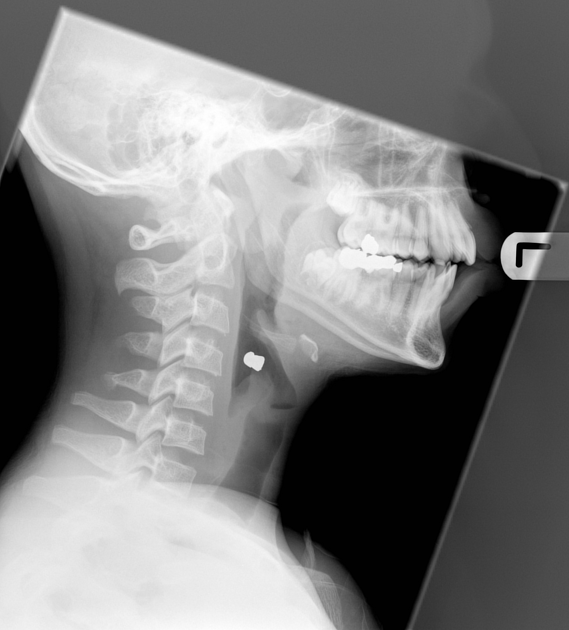
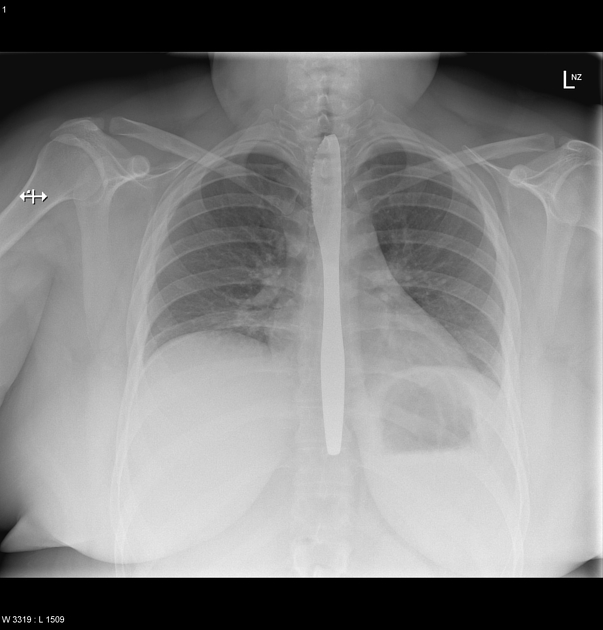
Ingested foreign bodies range from pediatric patients placing objects in their mouths, to mental-health-related self-harm, to bones stuck in the pharynx or gastrointestinal tract. Coins account for 70% of pediatric ingested foreign bodies and will typically become ‘stuck’ at the level of the cricopharyngeus muscle 8,14.
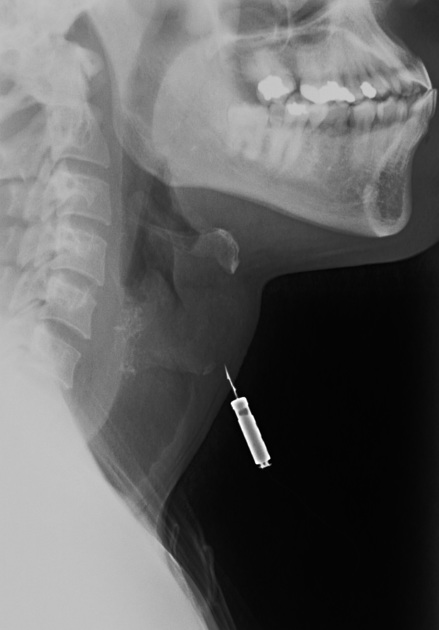
Sharp ingested foreign bodies can be potentially problematic when lodged in the esophagus; patients will often require emergency endoscopy; more often than not, if the sharp object is within reach of endoscopy, it will be removed before it progresses further 12.
Plastic bread clips are diagnostically challenging. The limited literature on this foreign body suggests they are invisible on both plain radiography and CT. The rigid shape can cause bowel perforations or gastrointestinal hemorrhage 15,16.
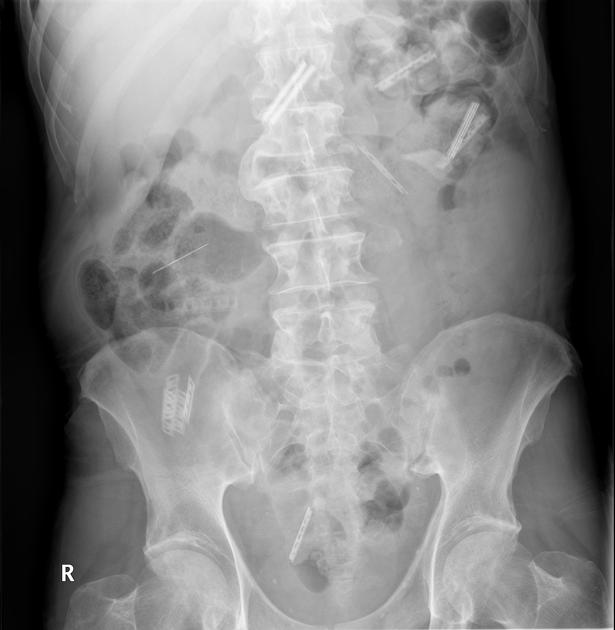
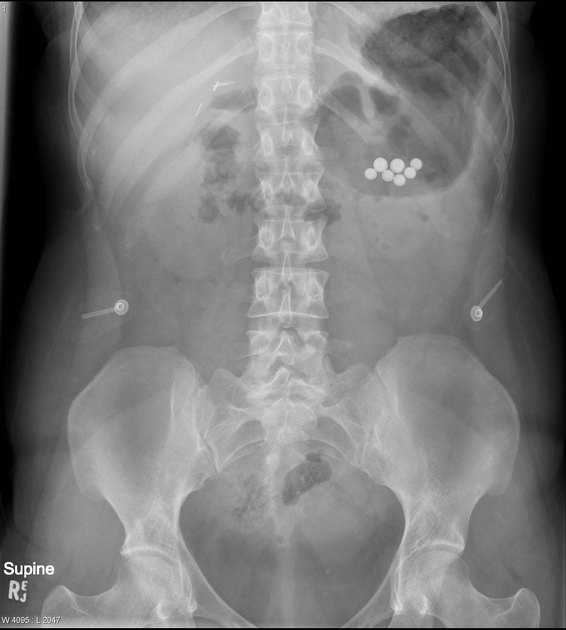
Drug packing
Drug packing is a well-documented form of foreign body. Often drugs are placed within condoms, or wrapped in foil, latex or cellophane, then swallowed or inserted anally or vaginally. These should be considered hazardous to the patient until evacuated due to the possibility of the containment method rupturing.
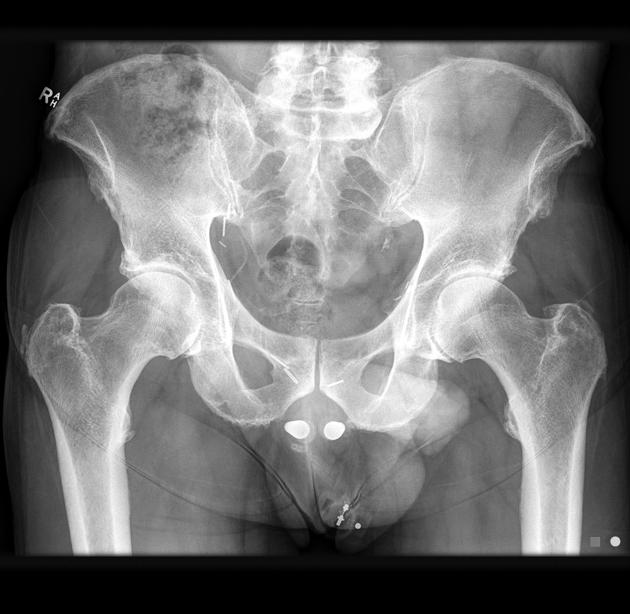
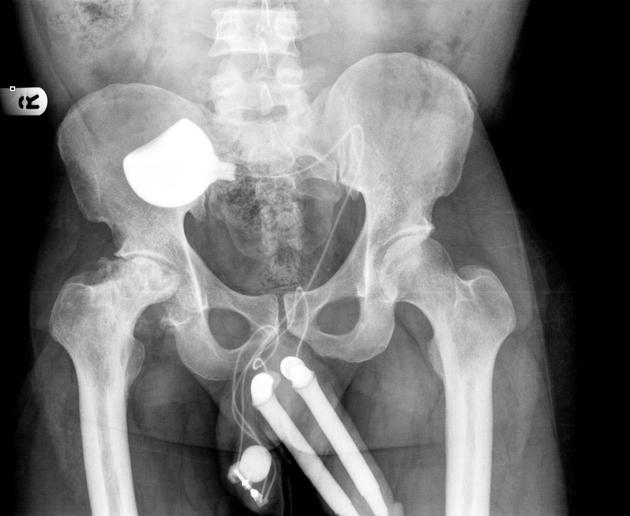
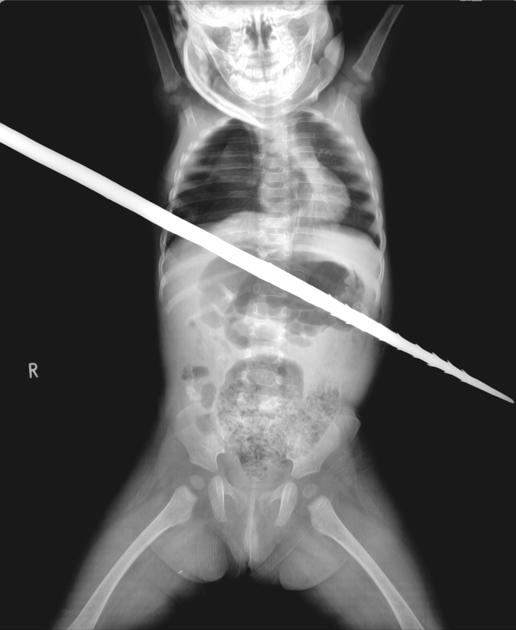
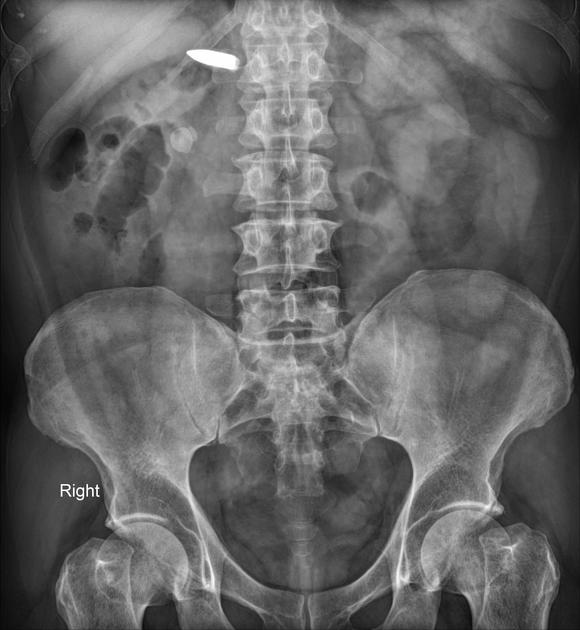
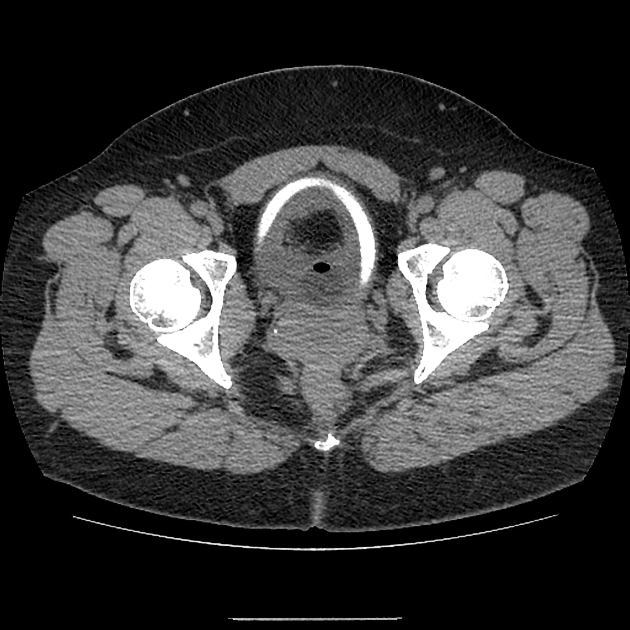
Rectal
Most rectal foreign bodies are inserted via the anus, although occasionally the foreign body has been ingested and has passed through to lie in the rectum. Commonly, rectal foreign bodies are used for sexual purposes 1-3. Rectal foreign will vary from case to case. The main problem with this is the often delayed presentation due to the reluctance of patients to present to emergency departments. Patients may suffer from extraperitoneal mucosal injuries or suffer from a more severe complication such as perforation 1-5.
Two plain radiographs are recommended to accurately demonstrate the rectal foreign body's size, shape, and location. This should be performed before a digital examination to prevent staff-related injuries from sharper foreign bodies.
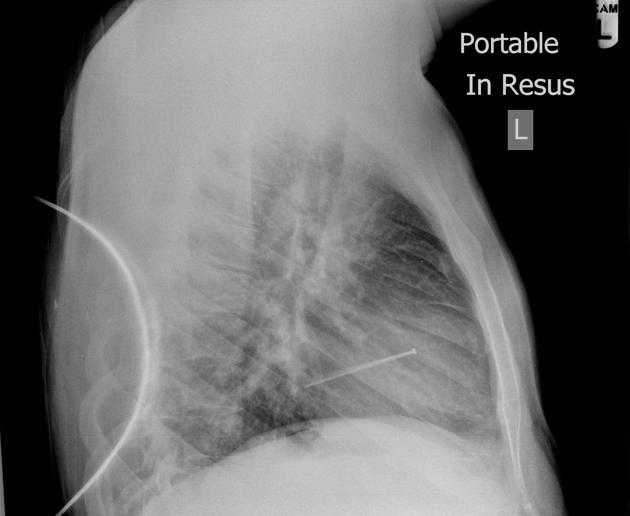
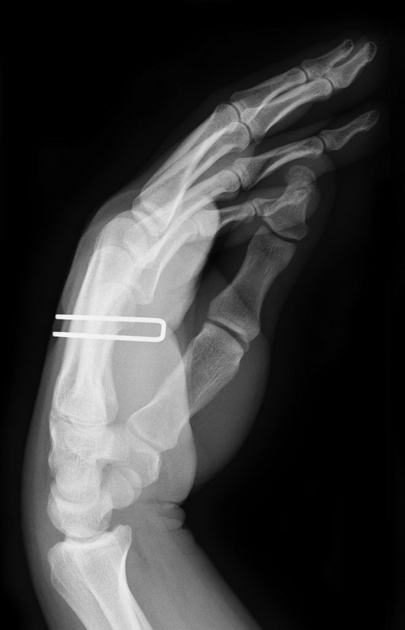
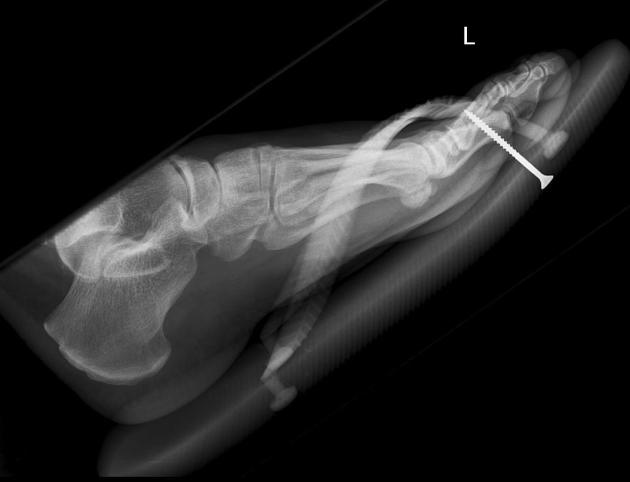
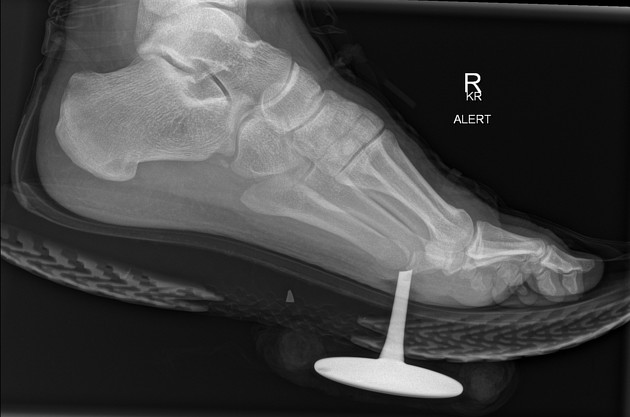
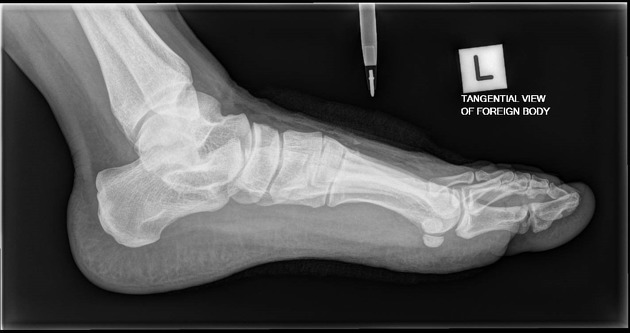
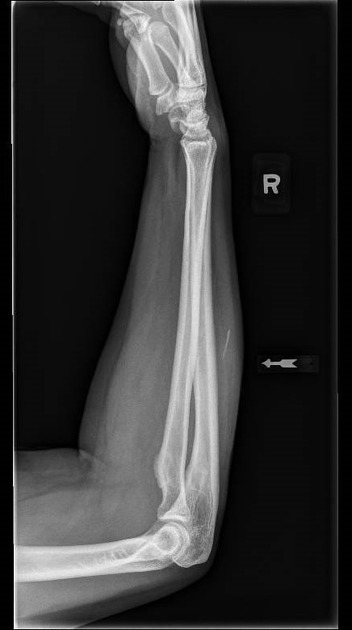
Soft tissue
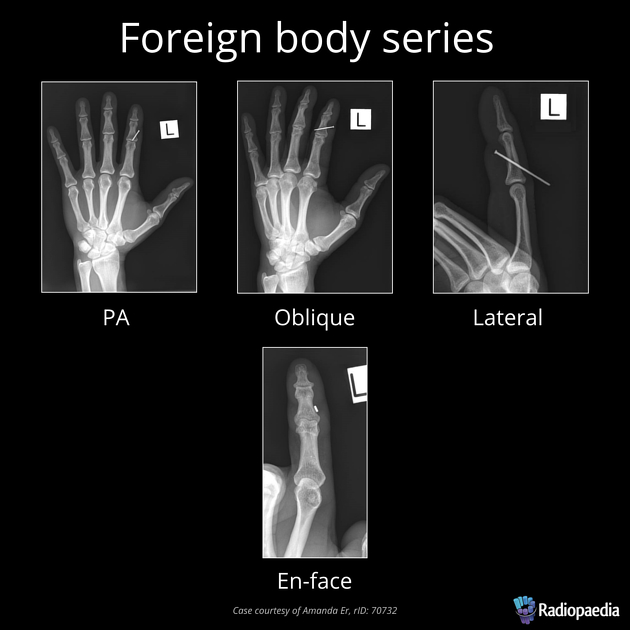
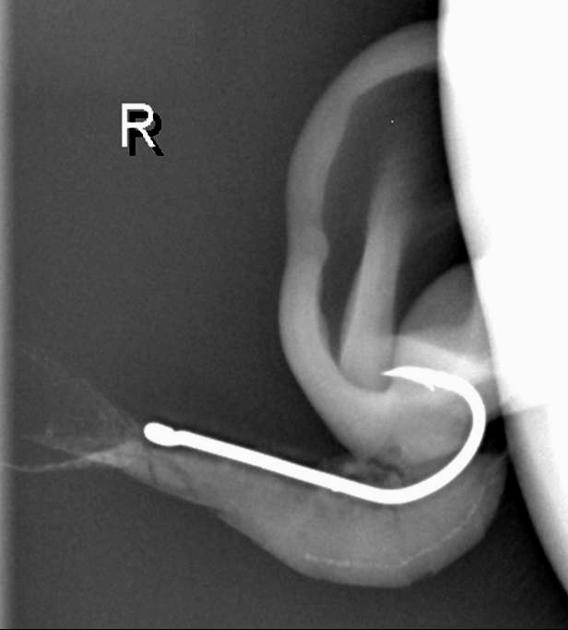
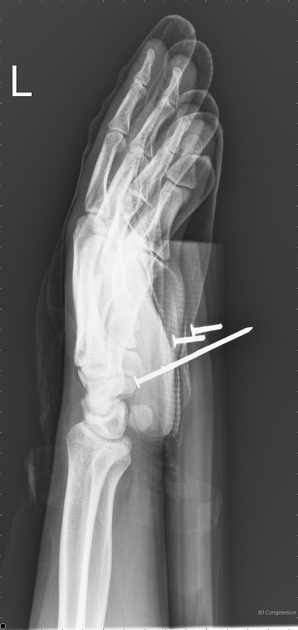
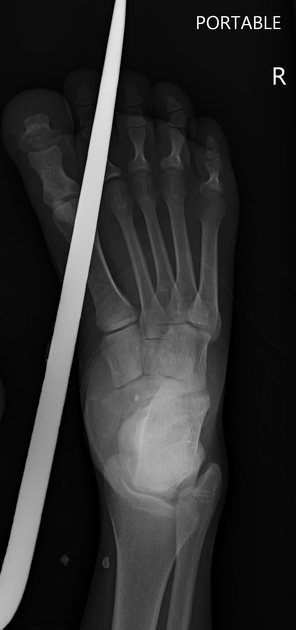
Most soft tissue foreign bodies are involuntary, resulting from accidental injury 18. The most commonly reported soft-tissue foreign bodies are glass, metal, and splinters from wood 5 and the most common location is the wrist/hand/finger 18.
It is imperative to locate foreign bodies before they become infected or worse, such as damage close-by organs, ideally within 24 hours of injury 18. ~40% are missed on clinical examination 18. Patients may have a delayed presentation with a foreign body granuloma.
Radiographic features
The investigation of foreign bodies relies heavily on radiology and every foreign body will have an optimal modality for investigation 17. Metal, glass, and stone can be visualized very well using conventional plain film radiography, whereas more organic structures, such as wood, may require further imaging such as ultrasonography 5-7.
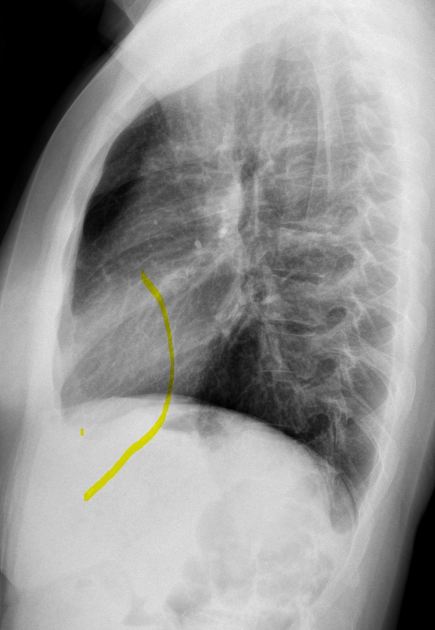
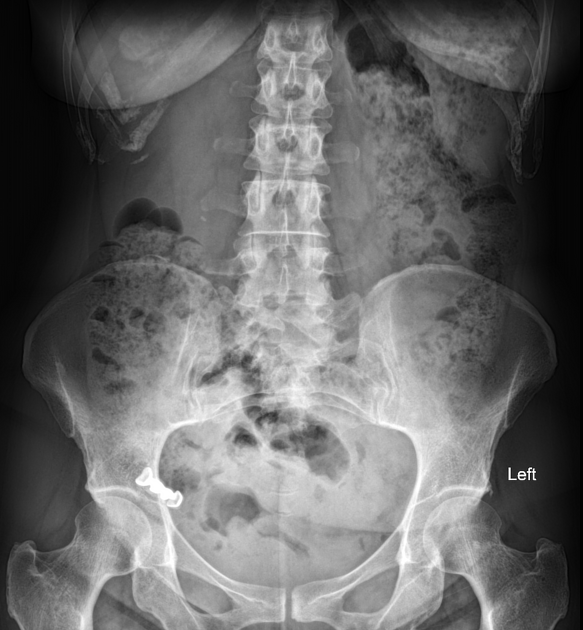
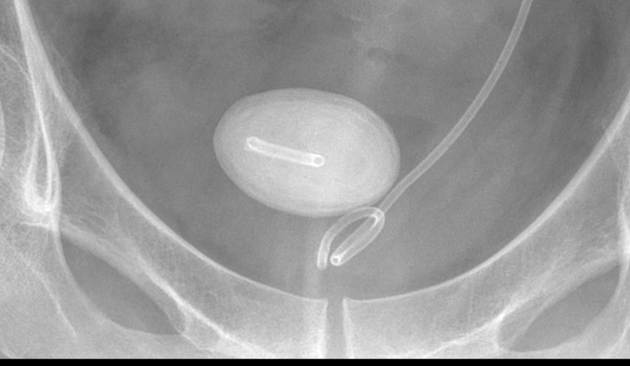
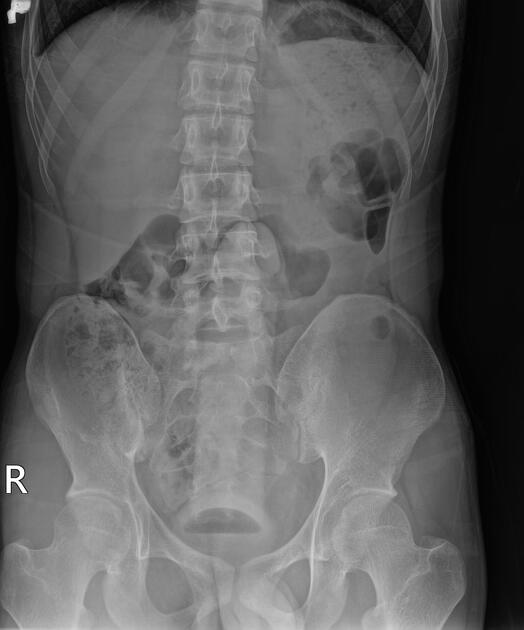
Plain radiograph
The radiological appearance in plain radiography of foreign bodies depends on three factors: the x-ray attenuation of the foreign body, the surrounding structures and any overlying structures that may veil the object.
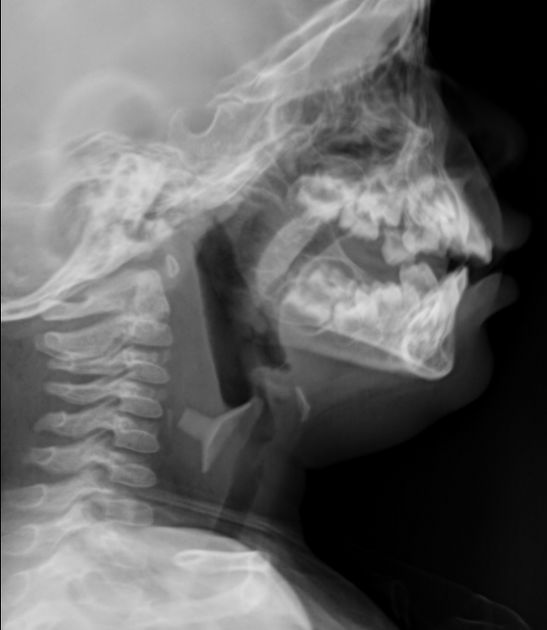
The anatomical location will affect the radiopacity of the suspected foreign body and the magnification rate as the object is placed further or closer to the detector; lateral cervical radiographs can have a magnification rate of up to 21.6% 9-11.
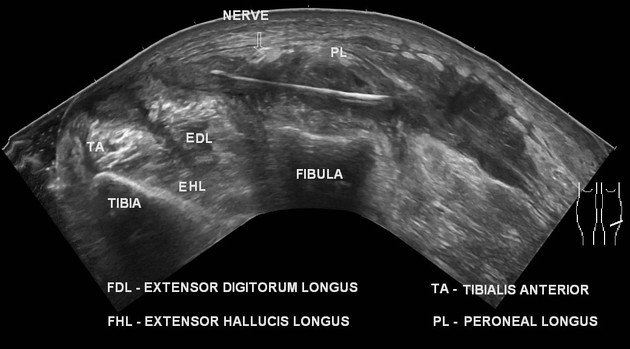
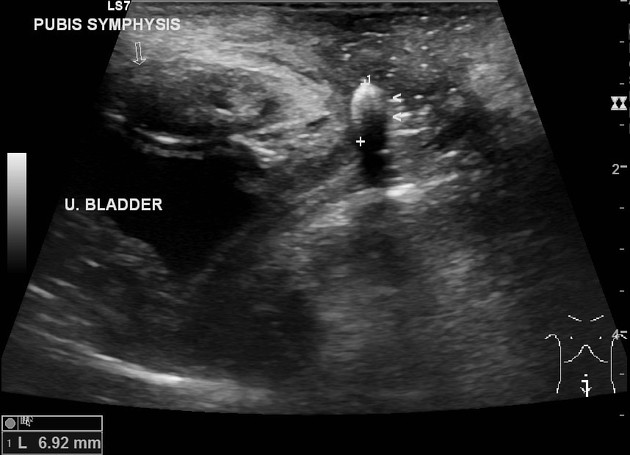
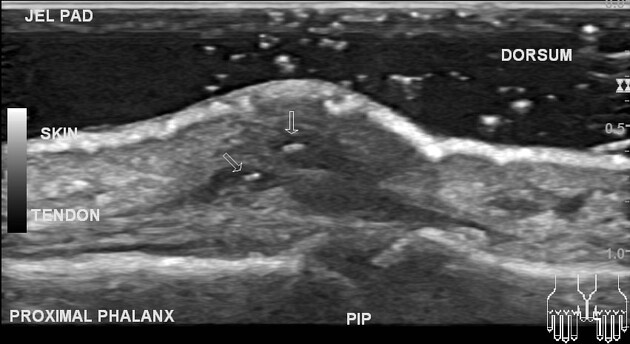
Ultrasound
Most foreign bodies are hyperechoic ref. Ultrasound scan is often helpful in identifying the dimensions and depth of the foreign body. It can be used to mark the site of the foreign body as part of pre-operative surgical planning ref.
Sonographic appearances of specific materials are:
wood: typically hyperechoic with posterior acoustic shadowing 19,20
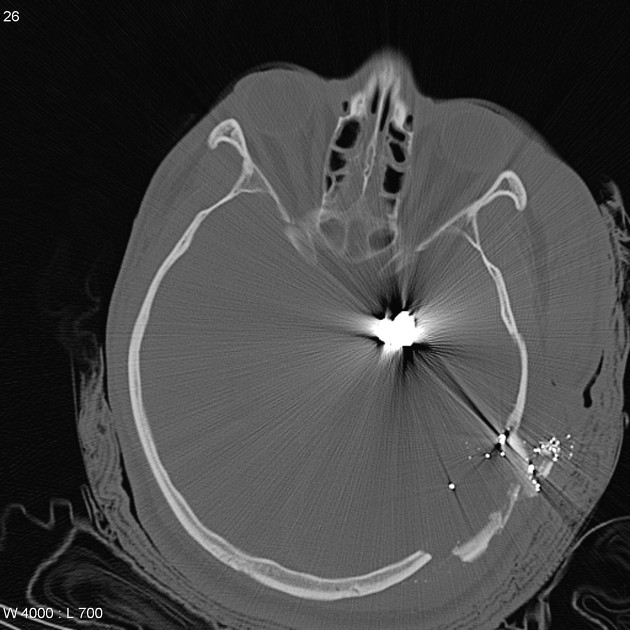
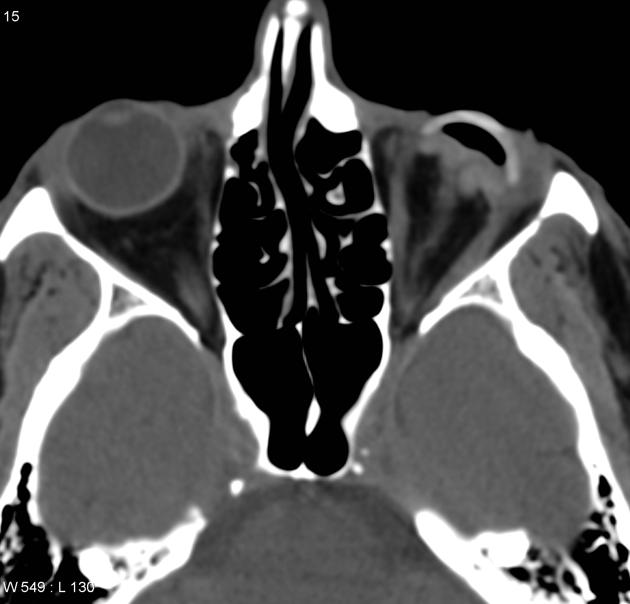
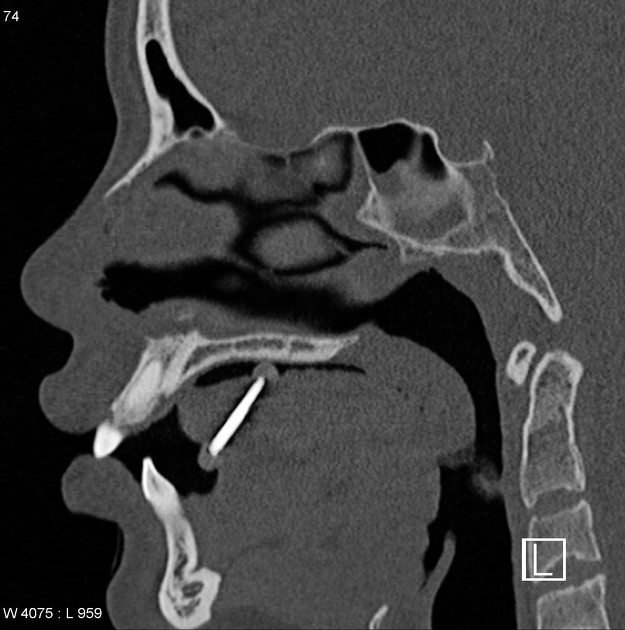
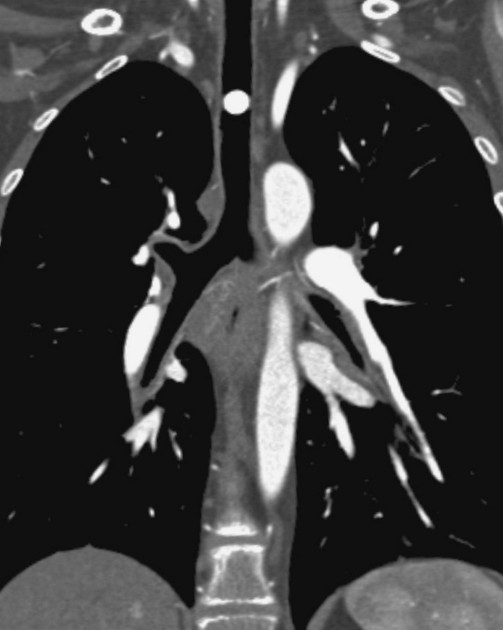
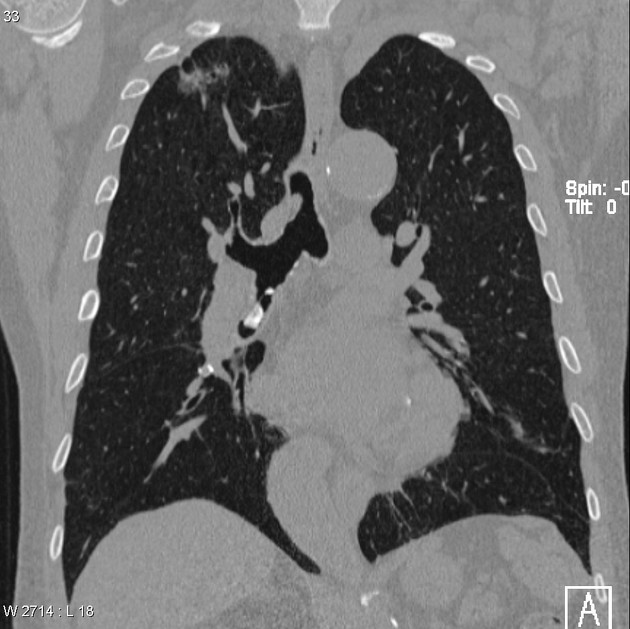
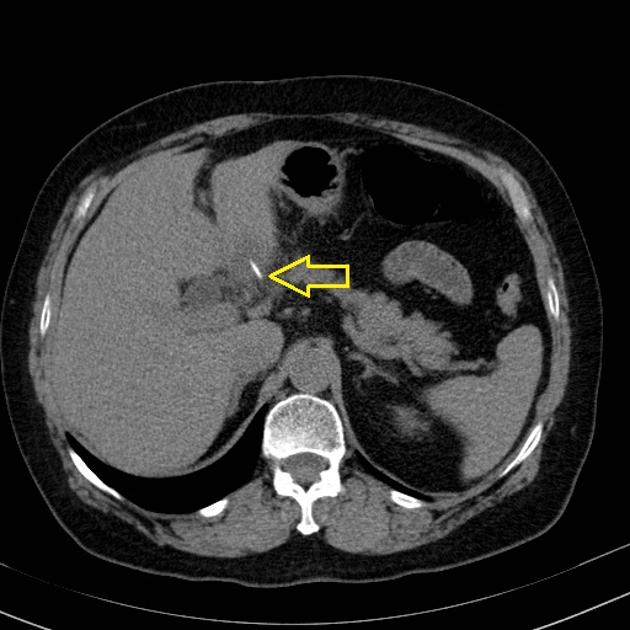
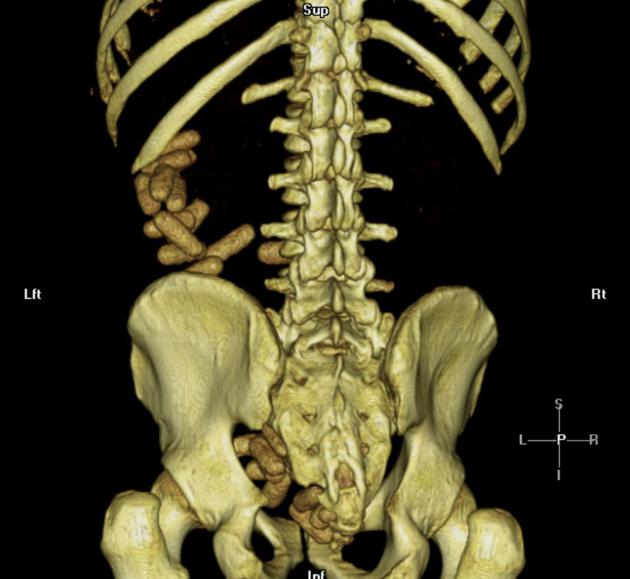
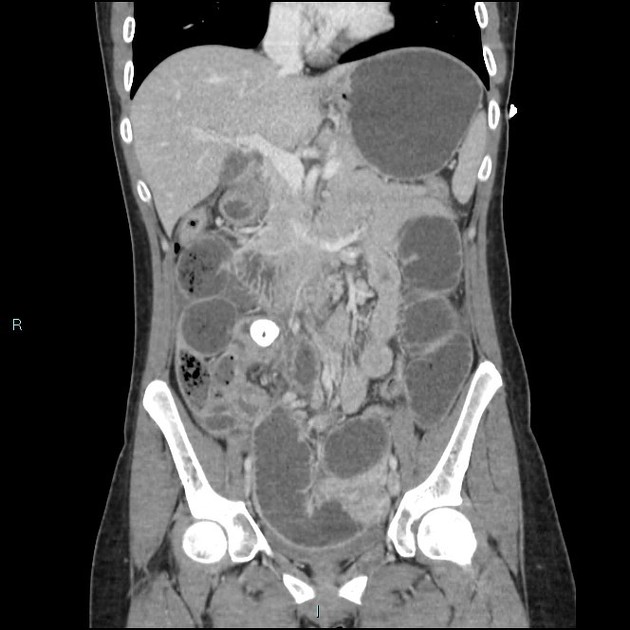
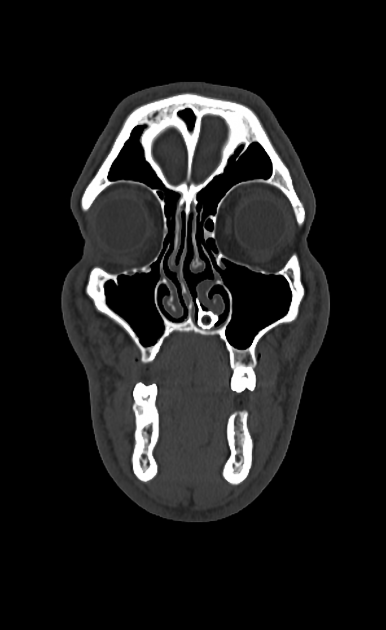
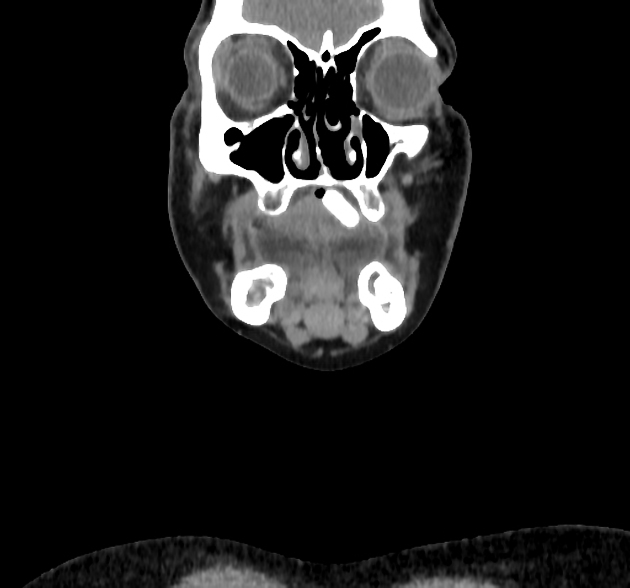
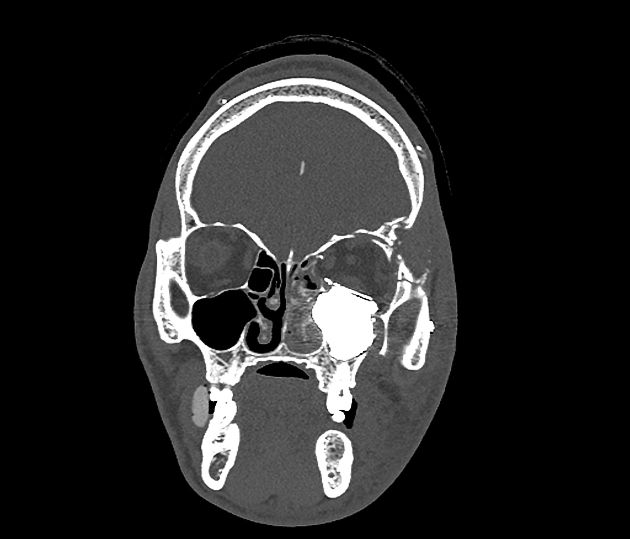
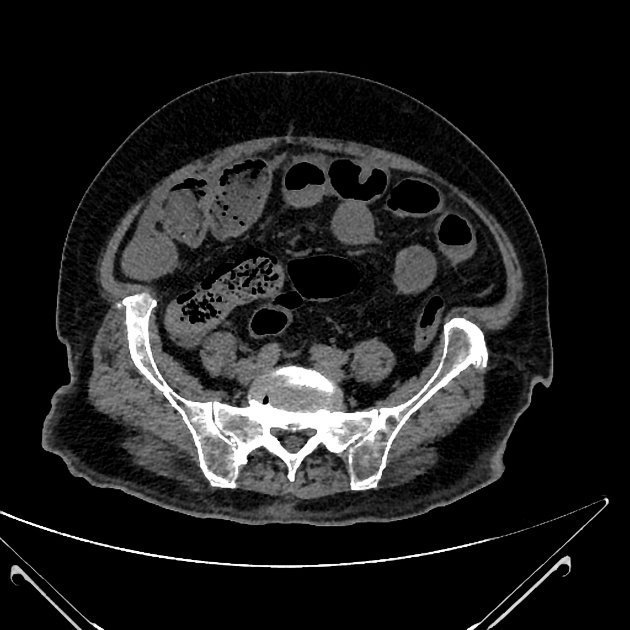
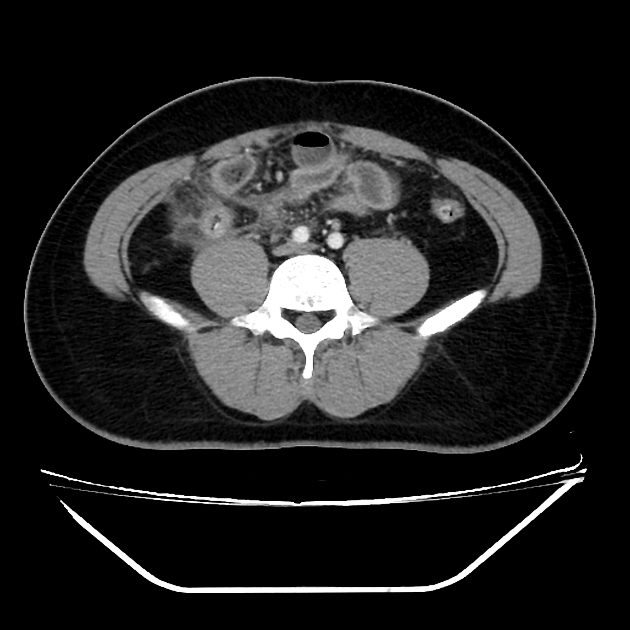
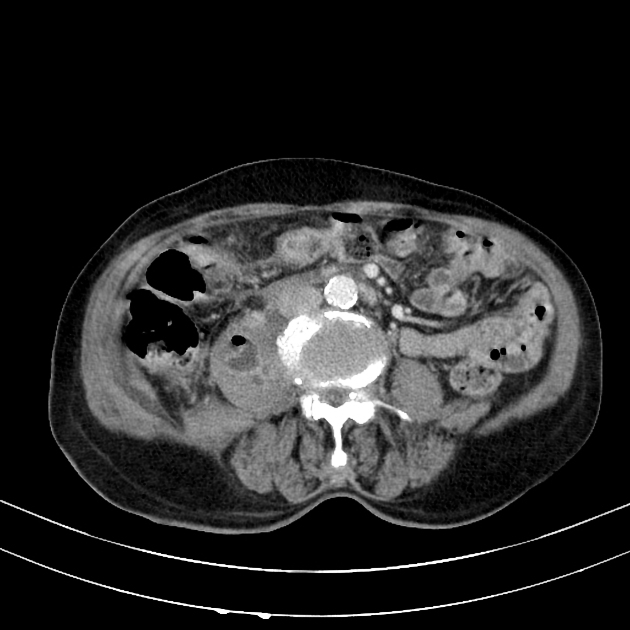
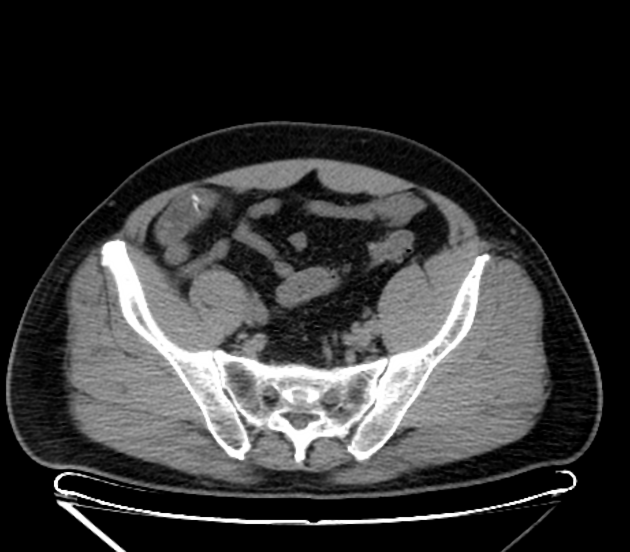
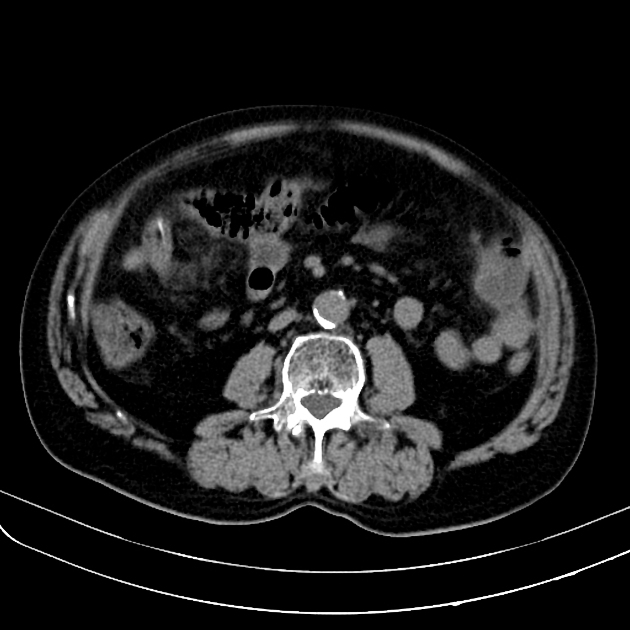
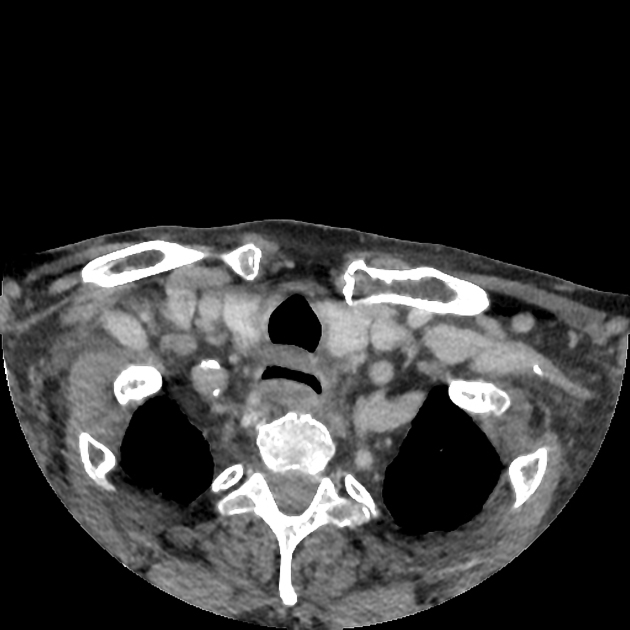
CT
The density of the foreign material in the body can range markedly, so using multiple window settings is crucial in identifying the presence of the objects. Routinely soft tissue, lung, and bone windows should be assessed. Certain plastics may be occult on CT.
MRI
The signal intensity of the foreign material in the body can range markedly, but most objects cause artifacts of some sort. Particular objects may be occult on MRI, such as those made of wood or plastic.















 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.