Papillary tumors of the pineal region are one of five pineal parenchymal tumors under the current (2021) WHO classification of CNS tumors with intermediate natural history and a grade of 2 or 3.
On this page:
Epidemiology
Papillary tumors of the pineal region are seen in a wide range of ages, reported from 5 to 66 years, while the mean age is in the fourth decade (30-40 years of age) 3,5. They show no significant sex predilection, perhaps marginally more commonly encountered in females 3,5.
Clinical presentation
As with all other pineal region masses, the clinical presentation is mainly from obstructive hydrocephalus secondary to compression of the tectum of the midbrain and obstruction of the aqueduct, being headache of short duration is the most common presentation 5. Compression of the superior colliculi can also lead to a characteristic gaze palsy, known as Parinaud syndrome.
Pathology
Papillary tumors of the pineal region are thought to arise from specialized ependymocytes of the subcommissural organ located in the lining of the posterior commissure rather than from the pineal gland itself 1-3. It is also hypothesized that some, or perhaps many, previously published descriptions of unusual pineal region tumors (e.g. choroid plexus papillomas and papillary ependymomas) actually represent papillary tumors of the pineal region, as histologically they are difficult to distinguish, requiring immunohistochemistry 1.
These tumors are considered WHO grade 2 or 3 tumors, although precise grading criteria are not yet available 3.
Macroscopic appearance
Papillary tumors are well-circumscribed lesions and their size may range from 2.5 to 4 cm. They may also have a cystic component 5.
Microscopic appearance
Papillary tumors of the pineal region demonstrate variable morphology ranging from solid to predominantly papillary, reminiscent of ependymomas, including the presence of ependymal rosettes 3. Areas of necrosis are sometimes identified 3,4.
Immunophenotype
Papillary tumors of the pineal region have a fairly characteristic immunohistochemical profile that allows them to be distinguished from other pineal parenchymal tumors.
- cytokeratins (AE1/3, CAM5.2, KL1, CK18): positive
- S100: positive
- vimentin: positive
- tansthyretin: positive
- neuron-specific enolase: positive
- MAP2: positive
- GFAP: variable
Radiographic features
MRI
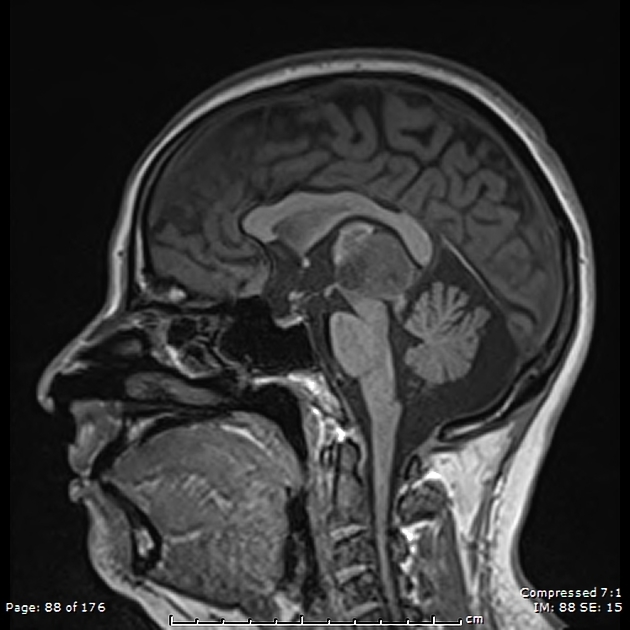
Papillary tumors of the pineal region are typically well-defined masses with variable T1 signal, high T2 signal, and heterogeneous postcontrast enhancement and are without pathognomic features 6-8. Cystic areas within the mass are commonly seen 6. T1 high signal has been described and is considered to be related to secretory inclusions containing glycoprotein or protein 1 but is considered a non-specific finding 7.
Treatment and prognosis
Screening of the entire neural axis is required as CSF dissemination has been reported in up to 7% of cases 4,6,7. These masses are typically treated with surgical resection and postoperative radiotherapy 7. 5-year survival rates are 73% 3,6.
History and etymology
In 2003, Jouvet et al reported six cases and named this entity as papillary tumor of pineal region 5. This tumor was first described in the WHO 2007 classification of brain tumors and was named as “A rare neuroepithelial tumor of the pineal region in adults, characterized by papillary architecture and epithelial cytology, immunopositivity for cytokeratin and ultrastructural features suggesting ependymal differentiation" 5.
Differential diagnosis
All pineal region lesions which are known to have papillary architecture are included in the differential diagnosis of PTPR. These include pineal parenchymal tumors, papillary ependymoma, choroid plexus ependymoma/carcinoma, papillary meningioma, and metastases 5.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.