CT perfusion of the brain is a dynamic, contrast-enhanced study utilized in patients with suspected stroke to differentiate salvageable ischemic brain tissue (i.e. penumbra) from damaged infarcted brain 1.
NB: This article is intended to outline some general principles of protocol design. The specifics will vary depending on CT hardware and software, radiologists' and referrers' preference, institutional protocols, patient factors (e.g. allergy) and time constraints.
On this page:
Indications
CT perfusion studies are performed in the context of patients presenting with acute neurological symptoms that may represent cerebral infarction or cerebral hemorrhage. It is often the last study in the code stroke CT pathway.
Purpose
The purpose of this scan is to measure/observe contrast enhancement as it makes its way through the arterial and venous system, making this a 'functional scan'. The scan will calculate the enhancement (if any) over time.
Contraindications
Previous severe reactions to iodinated contrast.
Technique
-
patient position
supine with their arms by their side
the head is placed in a 'chin tuck position' with the neck flexed (helped with a sponge behind the head) to reduce dose to the ocular lens
sponges can be placed on both sides to ensure that the head is straight
-
scout
-
base of the skull to the top of the vertex
if this is part of the code stroke pathway the scout may be from the carina to the tip of the skull as a CT angiogram of the neck and head will be performed before or after
-
-
scan extent
most perfusion scans begin at the base of the pituitary fossa focussing on the basal ganglia and supra-ganglionic level with a shuttle range of around 10 cm.
Coverage of less than 8 cm will underestimate the ischemic volume, while coverage of less than 4 cm will underestimate the core volume 1.
-
scan direction
this is a functional scan, the scan will 'shuttle' up and down as contrast is injected
-
scan duration
scan duration is often 45-60 seconds, but to be more precise, it takes as long as is required for the contrast to fully dissipate
-
contrast injection considerations
-
cannula size
this exam requires an injection of contrast at a considerable rate (ranging from 6-8 mL/s); therefore, a large bore (at least 18 gauge) cannula is required
-
injection rate
6-8 mL/s 1
-
injection volumes
35-40 mL of highly concentrated iodinated contrast 1 (300-350 mg/cc) followed by 30-40 mL of saline chaser
-
-
scan delay
minimal scan delay
Practical points
perfusion maps need to delineate the venous component from the arterial, the enhancement curves should be separate in the automated results, if this is not clearly defined in the preliminary results manual adjustment may be necessary
perfusion scans focus on the pituitary fossa at the basal ganglia and supra-ganglionic level; however, patients with symptoms of cerebellar infarction will require an adjustment of the scan extent
thick slices are often used to minimize noise
two of the most important factors of this exam are patient positioning and a quality IV access
poor cardiac output can lead to inaccurate perfusion maps; performing the carotid angiogram before the perfusion is a good way to get an idea of cardiac output and decide whether or not the scan duration needs to be adjusted
Post-processing
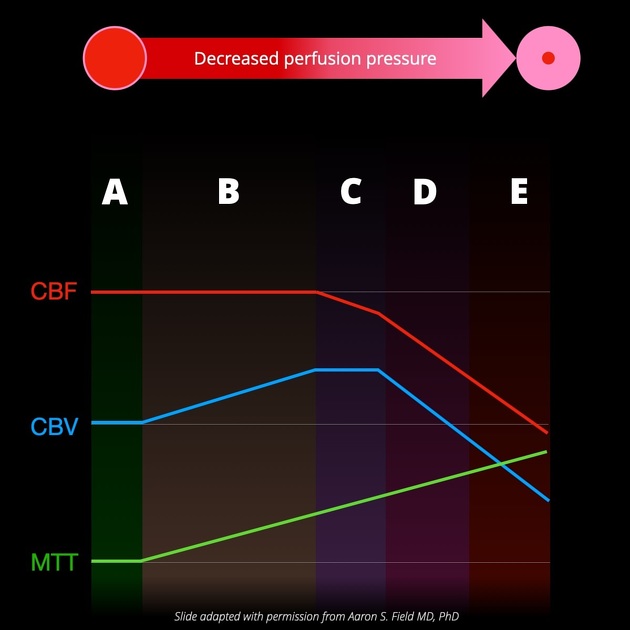
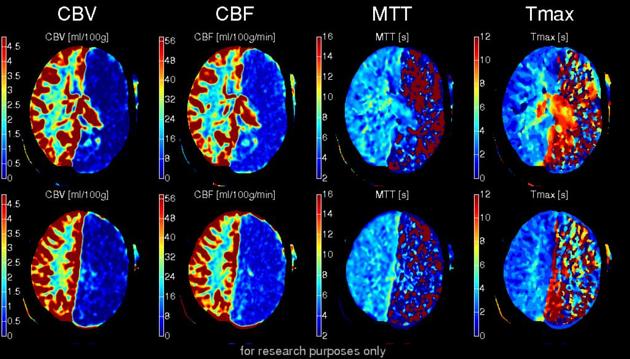
Post-processing methods differ, depending on the vendor of the machine; however, the primary focus of the post-processing will be the measure of:
mean transit time (MTT) or time to peak (TTP) of the deconvolved tissue residue function (Tmax)






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.