Malignant peripheral nerve sheath tumors (MPNSTs) are forms of peripheral nerve sheath tumors occurring either de novo or arising from pre-existing tumors (e.g. neurofibromas, schwannomas etc.). Approximately half of such tumors are seen in individuals with neurofibromatosis type I (NF1), in such cases arising from pre-existing neurofibromas.
On this page:
Epidemiology
Malignant peripheral nerve sheath tumors are estimated to account for 3-5% of all soft-tissue sarcomas 9. They typically present in young and middle-aged adults (20-50 years) 8,9. There is no recognized gender predilection.
Risk factors
NF1
radiation therapy 8,9
Diagnosis
Diagnostic criteria according to the WHO classification of soft tissue and bone tumors (5th edition) 9:
essential: sarcoma arising from a nerve or pre-existing nerve sheath tumor or in an NF1 patient
Clinical presentation
These tumors are often fairly rapidly enlarging and clinical presentation varies depending on location with mass effect and pain often present 11.
Pathology
Malignant peripheral nerve sheath tumors can arise in a number of different situations 8-10:
de novo
-
de-differentiation
more often in plexiform neurofibromas than in cutaneous neurofibromas in NF1
rarely other neurogenic tumors (e.g schwannoma, ganglioneuroblastoma, ganglioneuroma, pheochromocytoma, perineurioma) 8
radiation therapy-associated
Although by definition, these are malignant lesions, the mitotic rate and presence of necrosis vary significantly between tumors and also within individual tumors 1. These features are important in distinguishing MPNSTs from atypical neurofibromatous neoplasms of uncertain biologic potential (ANNUBP) 8.
Location
MPNSTs usually arise from a large nerve, and thus usually occur close to a plexus (e.g. brachial plexus/sacral plexus), with the sciatic nerve the most commonly affected peripheral nerve 9. Cranial nerves are rarely involved, and, on rare occasions they are, then the MPNST has usually arisen from an underlying schwannoma rather than a neurofibroma 8.
Genetics
Most MPNSTs demonstrate inactivation of a number of genes: NF1, CDKN2A, and PRC2 8.
Macroscopic appearance
The macroscopic appearance depends both on location and on whether or not the MPNST has arisen from an underlying pre-existing tumor. They are often large (>5 cm) at diagnosis, and may demonstrate local infiltration into surrounding tissues 8,9. It is common to identify areas of necrosis and hemorrhage 8.
Microscopic appearance
The microscopic appearance of MPNSTs is heterogeneous, varying in cellularity and growth pattern, generally including tightly packed spindle cells arranged in either a herringbone or interwoven fasciculated pattern 8.
Immunophenotype
Immunohistochemistry reflects their neurogenic origin, with the following immunoreactivity 8:
S100: positive in 50-70% - low in high-grade MPNSTs
p53 protein: positive in 75%
EGFR: positive in ~35%
Variants
A number of histological variants are recognized 8:
epithelioid MPNST
MPNST with divergent differentiation (a.k.a. malignant triton tumor)
MPNST with perineural differentiation (a.k.a. malignant perineurioma)
Grading
MPNST are designated as low-grade or high-grade according to the WHO classification of soft tissue and bone tumors on the basis of histological and genetic features (e.g. loss of H3K27me3 expression) 9.
It is worth noting that this grading is in contrast many benign neurogenic tumors (e.g. neurofibromas, schwannomas and perineuiomas) that sometimes can give rise to MPNST are given a grade of 1 in the WHO classification of CNS tumors 8.
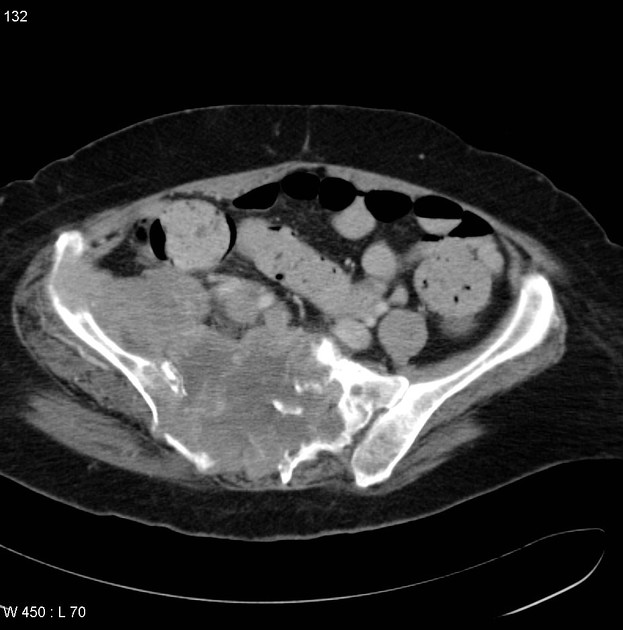
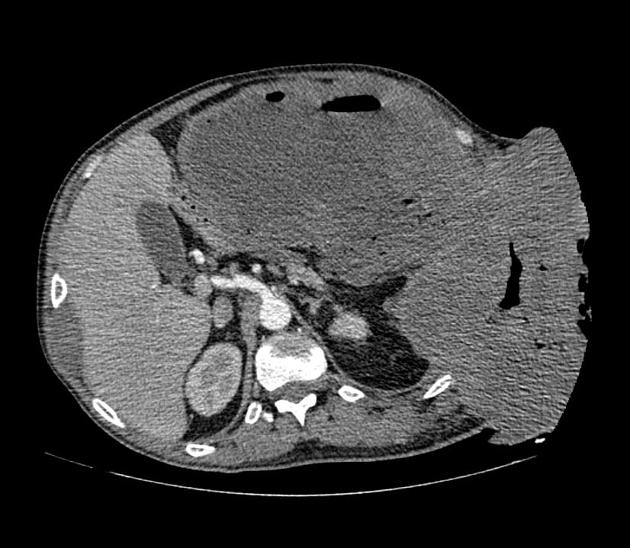
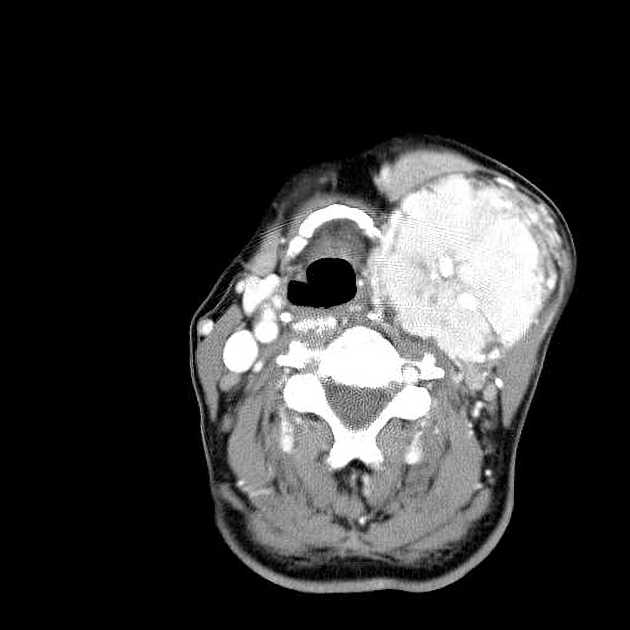
Radiographic features
Imaging criteria are generally considered unreliable in differentiating from a more benign neurofibroma or schwannoma 4 and there are no features to differentiate MPNST from other sarcomas 9. However, general rules favoring an MPNST include ref:
the larger the lesion, the more likely for it to be malignant
irregular borders (although most MPNSTs can have well-defined margins)
rapid growth in interval imaging
Ultrasound
Fusiform mass continuous with a nerve that is heterogeneous and hypoechoic. An irregular hyperechoic pseudocapsule may be present 11.
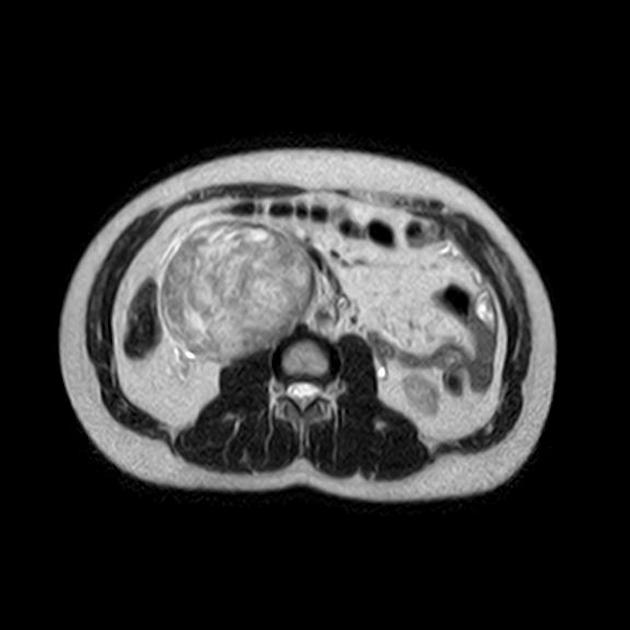
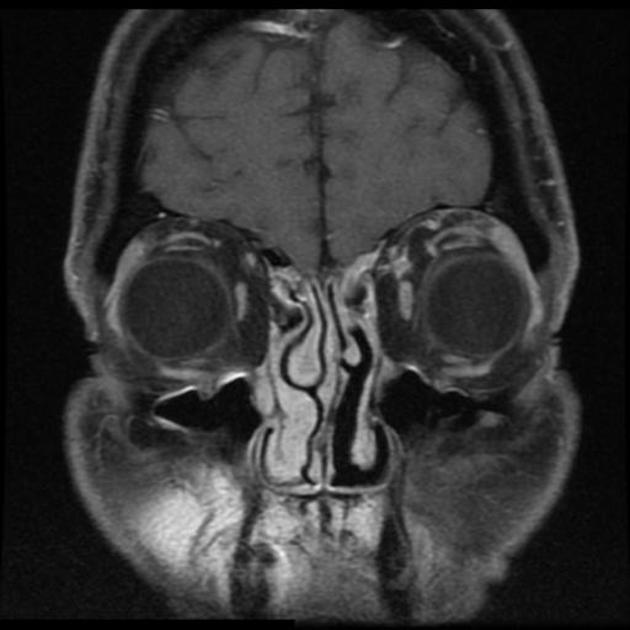
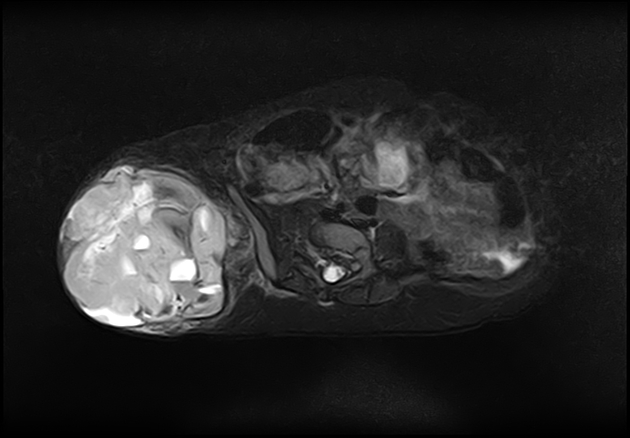
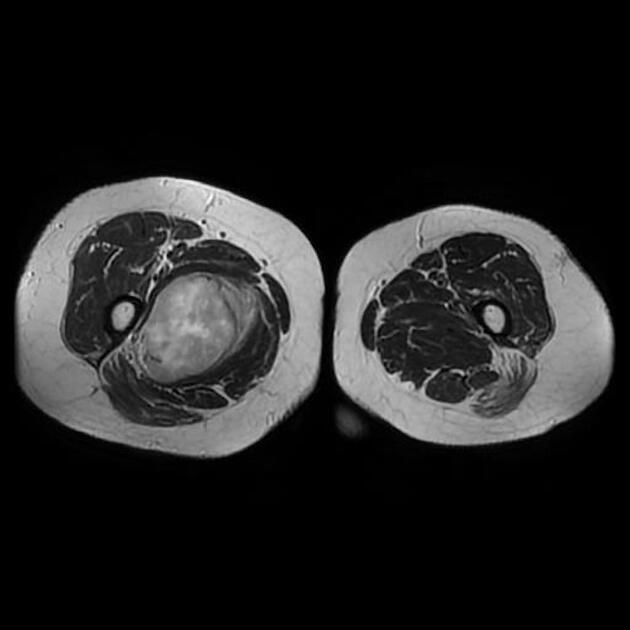
MRI
-
T1
usually isointense to muscle 4
heterogeneous T1 signal (if present) may useful in differentiating from a neurofibroma 3
T2: can have low signal due to high collagen content 4
Nuclear medicine
Gallium67 scintigraphy may show higher uptake than that of a neurofibroma 6,7.
Treatment and prognosis
MPNST are aggressive tumors that carry a poor prognosis, with 20-25% of patients developing metastases 8. Overall 5-year survival for sporadic tumors is 65% 8. Poor prognostic factors include 8,9:
NF1
large size
location on the trunk
high-grade histological features




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.