Caroli disease
Updates to Article Attributes
Caroli disease and Caroli syndrome are congenital disorders comprising of multifocal cystic dilatation of segmental intrahepatic bile ducts. However, some series show that extrahepatic duct involvement may exist. They are also classified as a type V choledochal cyst, according to the Todani classification.
Terminology
Caroli disease is limited to the dilatation of larger intrahepatic bile ducts, whereas Caroli syndrome describes the combination of small bile ductsduct dilatation and congenital hepatic fibrosis.
Epidemiology
Caroli disease and Caroli syndrome are rare autosomal recessive disorders with a slight female predilection.
Associations
simple Caroli disease is uncommon; it occurs more frequently with congenital hepatic fibrosis, constituting the Caroli syndrome
Clinical presentation
Presentation is in childhood or young adulthood. Caroli disease presents with right upper quadrant pain, recurrent cholelithiasis, and cholangitis with fever and jaundice. Caroli syndrome presents with the previous symptoms along with signs of portal hypertension, including haematemesis and melaena secondary to bleeding varices.
Pathology
Pathologically, Caroli disease and Caroli syndrome belong to the spectrum of fibropolycystic liver disease which results from in utero malformation of the ductal plate 4. There is a high association with fibrocystic anomalies of the kidneys which share the same genetic defect (PKHD1 gene, chromosome region 6p21) 5.
The ductal plate is a layer of hepatic precursor cells that surround the portal venous branches and is the anlage of the intrahepatic bile ducts. The manifestation of ductal plate malformation depends on the level of the biliary tree that is affected 3-5.
Thus, Caroli disease (the simple type) results from the abnormal development of the large bile ducts.
In contrast, in Caroli syndrome (the periportal type of Caroli disease), both the central intrahepatic bile ducts and the ductal plates of the smaller peripheral bile ducts are affected, with the latter leading to the development of fibrosis.
At the other end of the fibropolycystic disease spectrum are von Meyenburg complexes, also known as biliary hamartomas, which result from discrete foci of ductal plate malformation affecting the smallest bile ducts 5.
Associations
simple Caroli disease is uncommon; it occurs more frequently withcongenital hepatic fibrosis, constituting the Caroli syndrome
Radiographic features
The disease may be diffuse, lobar or segmental. Dilatation is most frequently saccular rather than fusiform, a feature that might help in the differential diagnosis.
Ultrasound
may show dilated intrahepatic bile ducts
(IHBD)intraductal bridging: echogenic septa traversing the dilated bile duct lumen
-
small portal venous branches partially or completely surrounded by dilated bile ducts 1,3
theintraluminal portal vein sign: dilated ducts surrounding the portal vein
intraductal calculi
CT
multiple hypodense rounded areas which are inseparable from the dilated intrahepatic bile ducts
“central dot” sign: enhancing dots within the dilated intrahepatic bile ducts, representing portal radicles 1
MRI
T1: hypointense dilatation of IHBD
T2: hyperintense
T1 C+ (Gd): enhancement of the central portal radicles within the dilated IHBD 1
MRCP: demonstrates continuity with the biliary tree
Nuclear medicine
Intrahepatic bile ducts can have a beaded appearance on HIDA scans 8.
Treatment and prognosis
PrognosisThe prognosis is generally poor. If the disease is localised, segmentectomy or lobectomy may be offered. In diffuse disease management is generally with conservative measures; liver transplantation may be an option 1.
Complications
-
simple type
intrahepatic stone formation
recurrent cholangitis that may lead to bacteraemia and sepsis
-
periportal fibrosis type
there is an increased risk of cholangiocarcinoma, which develops in 7% of patients 1
History and etymology
It is named after Jacques Caroli (1902-1979), a French gastroenterologist, who described it in 1958 7.
Differential diagnosis
-
no associated biliary duct dilatation
rarely communicate with the biliary ducts
-
may be cystic
generally do not communicate with the
bililarybiliary tree
-
primary sclerosing cholangitis
dilatation typically more fusiform and isolated, with a
'beaded'"beaded" appearanceassociated inflammatory bowel disease in 70% of
CaucasianWhite patients
-
recurrent pyogenic cholangitis
both present with sepsis and biliary dilatation
saccular (vs fusiform) dilatation favours Caroli disease 2
For a further CT differential, consider also focal hypodense hepatic lesions on a non-contrast CT scan.
-<p><strong>Caroli disease </strong>and<strong> Caroli syndrome</strong> are congenital disorders comprising of multifocal cystic dilatation of segmental intrahepatic bile ducts. However, some series show that extrahepatic duct involvement may exist. They are also classified as a type V <a href="/articles/choledochal-cyst">choledochal cyst</a>, according to the <a href="/articles/todani-classification-of-bile-duct-cysts">Todani classification</a>.</p><h4>Terminology</h4><p><strong>Caroli disease</strong> is limited to the dilatation of larger intrahepatic bile ducts, whereas <strong>Caroli syndrome</strong> describes the combination of small bile ducts dilatation and <a href="/articles/congenital-hepatic-fibrosis">congenital hepatic fibrosis</a>. </p><h4>Epidemiology</h4><p>Caroli disease and Caroli syndrome are rare autosomal recessive disorders with a slight female predilection. </p><h4>Clinical presentation</h4><p>Presentation is in childhood or young adulthood. Caroli disease presents with right upper quadrant pain, recurrent cholelithiasis, and <a href="/articles/cholangitis">cholangitis</a> with <a href="/articles/pyrexia">fever</a> and <a href="/articles/jaundice">jaundice</a>. Caroli syndrome presents with the previous symptoms along with signs of <a href="/articles/portal-hypertension">portal hypertension</a>, including haematemesis and melaena secondary to bleeding varices.</p><h4>Pathology</h4><p>Pathologically, Caroli disease and Caroli syndrome belong to the spectrum of <a href="/articles/fibropolycystic-liver-disease">fibropolycystic liver disease</a> which results from <em>in utero</em> malformation of the <a href="/articles/ductal-plate">ductal plate</a> <sup>4</sup>. There is a high association with fibrocystic anomalies of the kidneys which share the same genetic defect (<em>PKHD1</em> gene, chromosome region 6p21) <sup>5</sup>.</p><p>The ductal plate is a layer of hepatic precursor cells that surround the portal venous branches and is the anlage of the intrahepatic bile ducts. The manifestation of ductal plate malformation depends on the level of the biliary tree that is affected <sup>3-5</sup>.</p><p>Thus, <strong>Caroli disease</strong> (the <strong>simple type)</strong> results from the abnormal development of the large bile ducts.</p><p>In contrast, in <strong>Caroli syndrome</strong> (the <strong>periportal type</strong> of Caroli disease), both the central intrahepatic bile ducts and the ductal plates of the smaller peripheral bile ducts are affected, with the latter leading to the development of fibrosis.</p><p>At the other end of the fibropolycystic disease spectrum are von Meyenburg complexes, also known as <a href="/articles/multiple-biliary-hamartomas-1">biliary hamartomas</a> which result from discrete foci of ductal plate malformation affecting the smallest bile ducts <sup>5</sup>.</p><h5>Associations</h5><ul>- +<p><strong>Caroli disease </strong>and<strong> Caroli syndrome</strong> are congenital disorders comprising of multifocal cystic dilatation of segmental intrahepatic bile ducts. However, some series show that extrahepatic duct involvement may exist. They are also classified as a type V <a href="/articles/choledochal-cyst">choledochal cyst</a>, according to the <a href="/articles/todani-classification-of-bile-duct-cysts">Todani classification</a>.</p><h4>Terminology</h4><p>Caroli disease is limited to the dilatation of larger intrahepatic bile ducts, whereas Caroli syndrome describes the combination of small bile duct dilatation and <a href="/articles/congenital-hepatic-fibrosis">congenital hepatic fibrosis</a>. </p><h4>Epidemiology</h4><p>Caroli disease and Caroli syndrome are rare autosomal recessive disorders with a slight female predilection.</p><h5>Associations</h5><ul>
-</ul><h4>Radiographic features</h4><p>The disease may be diffuse, lobar or segmental. Dilatation is most frequently saccular rather than fusiform, a feature that might help in the differential diagnosis.</p><h5>Ultrasound</h5><ul>-<li><p>may show dilated intrahepatic bile ducts (IHBD)</p></li>- +</ul><h4>Clinical presentation</h4><p>Presentation is in childhood or young adulthood. Caroli disease presents with right upper quadrant pain, recurrent cholelithiasis, and <a href="/articles/cholangitis">cholangitis</a> with <a href="/articles/pyrexia">fever</a> and <a href="/articles/jaundice">jaundice</a>. Caroli syndrome presents with the previous symptoms along with signs of <a href="/articles/portal-hypertension">portal hypertension</a>, including haematemesis and melaena secondary to bleeding <a href="/articles/portosystemic-collateral-pathways-1" title="Varices (portosystemic shunts)">varices</a>.</p><h4>Pathology</h4><p>Pathologically, Caroli disease and Caroli syndrome belong to the spectrum of <a href="/articles/fibropolycystic-liver-disease">fibropolycystic liver disease</a> which results from in utero malformation of the <a href="/articles/ductal-plate">ductal plate</a> <sup>4</sup>. There is a high association with fibrocystic anomalies of the kidneys which share the same genetic defect (<em>PKHD1</em> gene, chromosome region 6p21) <sup>5</sup>.</p><p>The ductal plate is a layer of hepatic precursor cells that surround the portal venous branches and is the anlage of the intrahepatic bile ducts. The manifestation of ductal plate malformation depends on the level of the biliary tree that is affected <sup>3-5</sup>.</p><p>Caroli disease (the simple type) results from the abnormal development of the large bile ducts.</p><p>In contrast, in Caroli syndrome (the periportal type of Caroli disease), both the central intrahepatic bile ducts and the ductal plates of the smaller peripheral bile ducts are affected, with the latter leading to the development of fibrosis.</p><p>At the other end of the fibropolycystic disease spectrum are von Meyenburg complexes, also known as <a href="/articles/multiple-biliary-hamartomas-1">biliary hamartomas</a>, which result from discrete foci of ductal plate malformation affecting the smallest bile ducts <sup>5</sup>.</p><h4>Radiographic features</h4><p>The disease may be diffuse, lobar or segmental. Dilatation is most frequently saccular rather than fusiform, a feature that might help in the differential diagnosis.</p><h5>Ultrasound</h5><ul>
- +<li><p>may show dilated intrahepatic bile ducts</p></li>
-<ul><li><p><sup></sup>the intraluminal portal vein sign: dilated ducts surrounding the portal vein</p></li></ul>- +<ul><li><p><sup></sup>intraluminal portal vein sign: dilated ducts surrounding the portal vein</p></li></ul>
-</ul><h5>Nuclear medicine</h5><p>Intrahepatic bile ducts can have a beaded appearance on <a href="/articles/hida-scan">HIDA scans</a> <sup>8</sup>.</p><h4>Treatment and prognosis</h4><p>Prognosis is generally poor. If the disease is localised, segmentectomy or lobectomy may be offered. In diffuse disease management is generally with conservative measures; liver transplantation may be an option <sup>1</sup>.</p><h5>Complications</h5><ul>- +</ul><h5>Nuclear medicine</h5><p>Intrahepatic bile ducts can have a beaded appearance on <a href="/articles/hida-scan">HIDA scans</a> <sup>8</sup>.</p><h4>Treatment and prognosis</h4><p>The prognosis is generally poor. If the disease is localised, segmentectomy or lobectomy may be offered. In diffuse disease management is generally with conservative measures; liver transplantation may be an option <sup>1</sup>.</p><h5>Complications</h5><ul>
-<li><p>hepatomegaly</p></li>-<li><p>ascites</p></li>-<li><p>varices</p></li>- +<li><p><a href="/articles/hepatomegaly" title="Hepatomegaly">hepatomegaly</a></p></li>
- +<li><p><a href="/articles/ascites" title="Ascites">ascites</a></p></li>
- +<li><p><a href="/articles/portosystemic-collateral-pathways-1" title="Varices (portosystemic shunts)">varices</a></p></li>
-<li><p>generally do not communicate with the bililary tree </p></li>- +<li><p>generally do not communicate with the biliary tree</p></li>
-<li><p>dilatation typically more fusiform and isolated, with a 'beaded' appearance</p></li>-<li><p>associated <a href="/articles/inflammatory-bowel-disease">inflammatory bowel disease</a> in 70% of Caucasian patients</p></li>- +<li><p>dilatation typically more fusiform and isolated, with a "beaded" appearance</p></li>
- +<li><p>associated <a href="/articles/inflammatory-bowel-disease">inflammatory bowel disease</a> in 70% of White patients</p></li>
Image 1 CT (C+ portal venous phase) ( update )
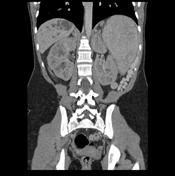
Image 4 MRI (T2) ( update )

Image 9 CT (non-contrast) ( update )

Image 12 CT (C+ portal venous phase) ( update )








 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.