Thyroid lymphoma is rare, accounting for a minority of both thyroid malignancies and lymphoma in general.
The thyroid may be affected primarily or secondary to lymphoma elsewhere. This article is concerned with primary thyroid lymphoma.
On this page:
Epidemiology
Thyroid lymphoma accounts for <5% of thyroid malignancies and ~2.5% of extranodal lymphoma.
Thyroid lymphoma is rare with an incidence of 1-2 per 1,000,000. It typically presents between 50-70 years of age with a strong female predominance (M: F = 1:3).
Clinical presentation
Typically, it presents as a rapidly enlarging goiter with compressive symptoms and cervical lymphadenopathy common. B-type symptoms are uncommon (20%) and approximately half of patients are euthyroid.
Pathology
The etiology of thyroid lymphoma is unclear. Hashimoto thyroiditis is a major risk factor (~60 times increased risk) but the development of thyroid lymphoma is still rare in this group.
The histological subtype of thyroid lymphoma is heterogeneous with diffuse large B cell lymphoma being the most common in one series. Hodgkin lymphoma affects the thyroid very rarely, non-Hodgkin lymphoma accounts for the vast majority of thyroid lymphoma cases 2 .
Radiographic features
The radiographic features of thyroid lymphoma are nonspecific and similar to other primary thyroid malignancies and Hashimoto thyroiditis.
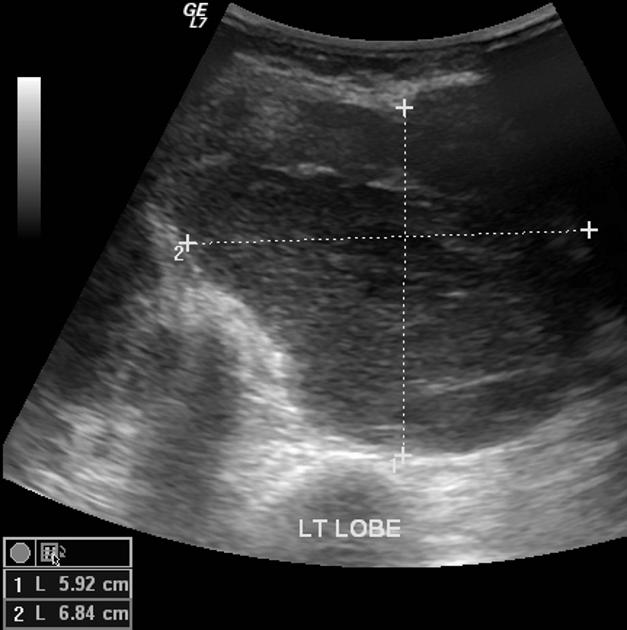
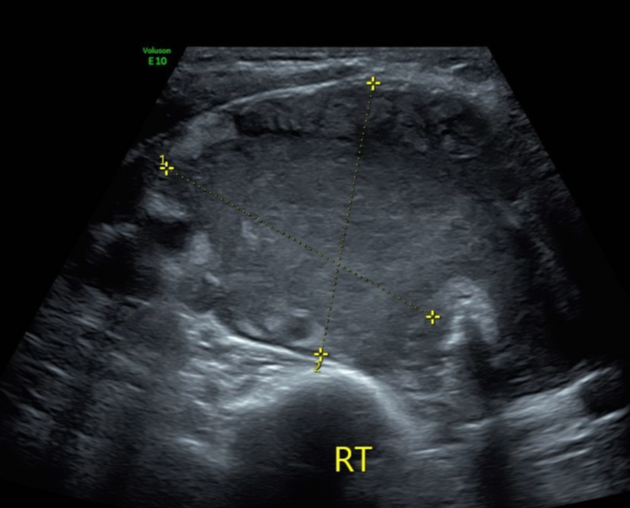
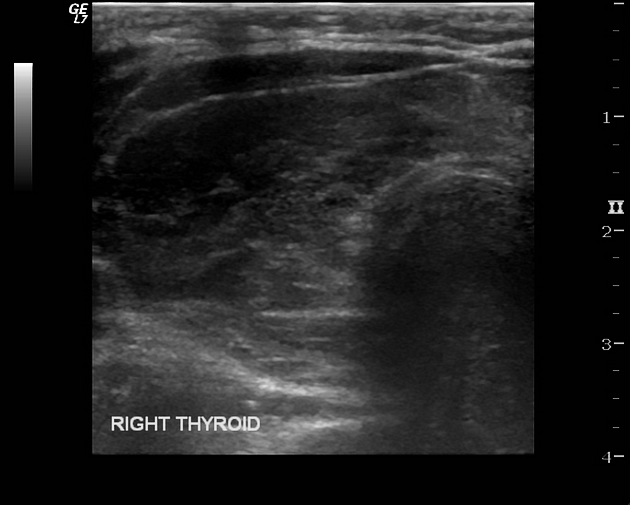
Ultrasound
Three patterns have been described: nodular (hypoechoic mass), diffuse (mixed echotexture), or mixed 1,3. Calcifications are uncommon 4.
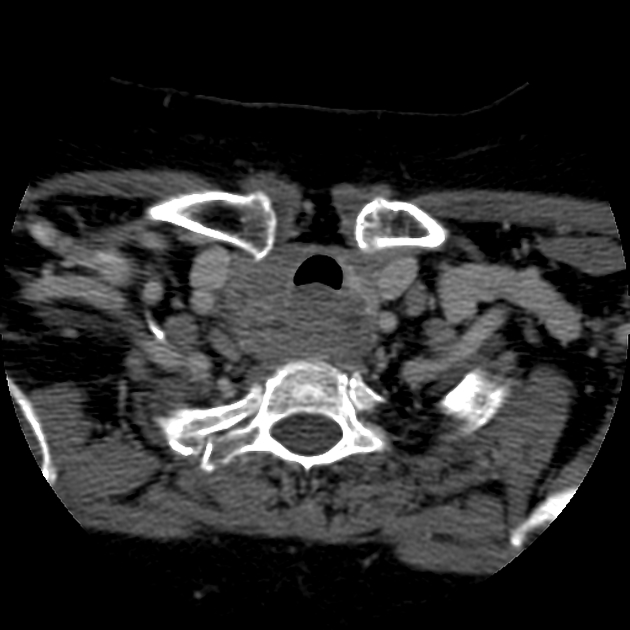
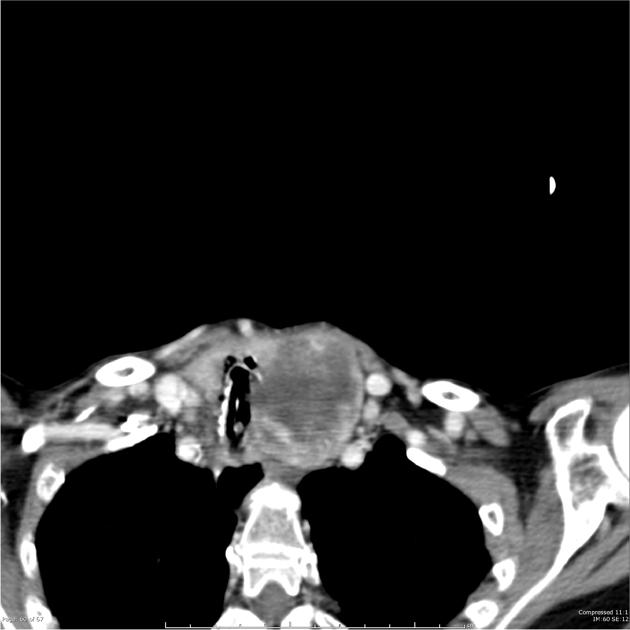
CT
- goiter, which is hypodense to adjacent muscle
- heterogeneous enhancement but still less than adjacent muscle 3
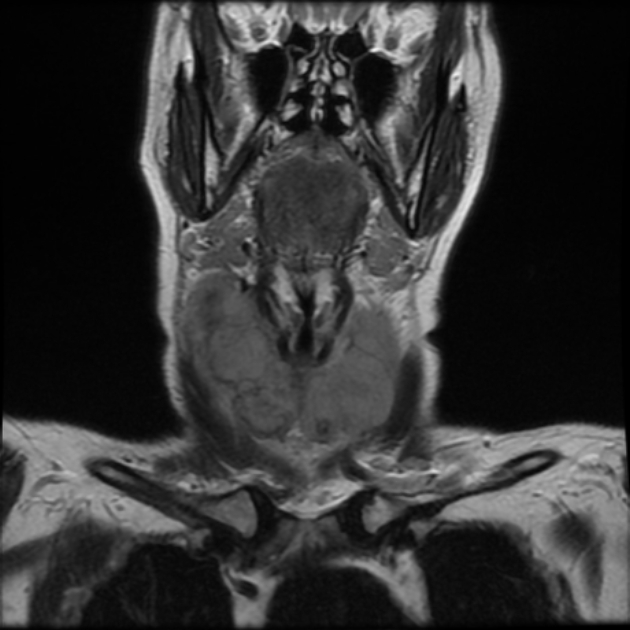
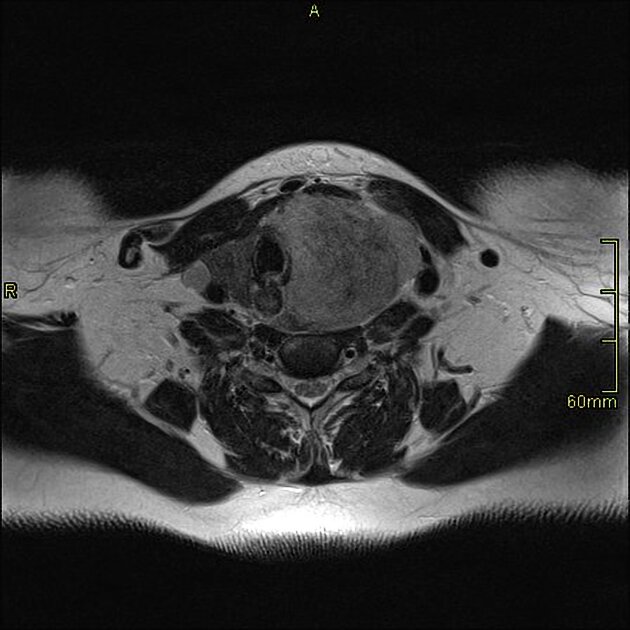
MRI
- T1/T2: iso- to hyperintense
- pseudocapsule may be present 3
Treatment and prognosis
Prognosis is generally considered "excellent" for disease limited to the thyroid. Combination chemotherapy and radiation therapy is generally used with surgical excision less common 1,2,4.
Differential diagnosis
Other causes of goiter should be considered, in particular Hashimoto thyroiditis and other primary thyroid malignancies.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.