Ureteropelvic junction (UPJ) obstruction or pelviureteric junction (PUJ) obstruction partially obstructs the passage of urine from the renal pelvis to the ureter. It is the most frequent cause of hydronephrosis in the foetus and can also present in adulthood.
On this page:
Epidemiology
UPJ obstruction on antenatal ultrasound affects about 1:500 foetuses. It is more common in males and is usually unilateral (90%) being more frequent on the left 12.
Associations
-
in congenital cases, some renal tract abnormalities are recognized
in ~40% of cases, an aberrant, accessory, or early-branching lower pole segment vessel is found and observed to compress the ureter, causing mechanical obstruction
Clinical presentation
Many cases are asymptomatic and identified incidentally when the renal tract is imaged for other reasons. When symptomatic, symptoms include recurrent urinary tract infections, stone formation and even a palpable flank mass. They are also at high risk of renal injury even by minor trauma.
Classically intermittent pain after drinking large volumes of fluid with a diuretic effect is described, due to the reduced outflow from the renal pelvis into the ureter 8.
Pathology
Pelviureteric junction obstruction is most commonly unilateral but is reported to be bilateral in ~30% (range 10-49%) of cases 10. There is a recognized predilection towards the left side (~67% of cases).
During embryogenesis, the pelviureteric junction forms usually around the fifth week and the initial tubular lumen of the ureteric bud become recanalized by ~10-12 weeks. The pelviureteric junction area is the last to recanalize. Inadequate canalization is thought to be the main embryological explanation of a pelviureteric junction obstruction. Extrinsic obstructions secondary to bands, kinks, and aberrant vessels also are commonly encountered.
Interestingly, research has failed to identify any anatomically-discrete pelviureteric junction although physiologically there is evidence of a sphincter-like action in this region 11.
Etiology
-
congenital (neonatal)
-
idiopathic and often unknown; proposed causes include
abnormal muscle arrangement at the pelviureteric junction
anomalous collagen collar at pelviureteric junction
ischemic insult to pelviureteric junction region
urothelial ureteral fold
-
extrinsic ureter compression or encasement
crossing vessel (at pelviureteric junction)
-
-
adult
preceding renal pelvic trauma
obstructing calculus immediately distal to pelviureteric junction
previous pyelitis with scarring
intrinsic malignancy, e.g. upper tract urothelial carcinoma
-
extrinsic ureter compression or encasement
fibrosis
crossing vessel (at pelviureteric junction)
malignancy
Radiographic features
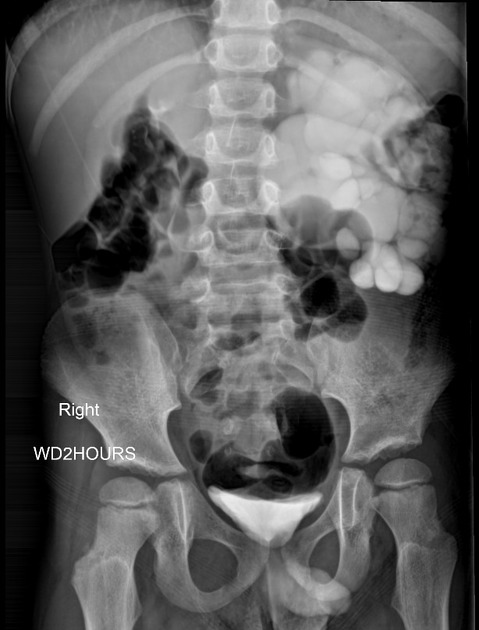
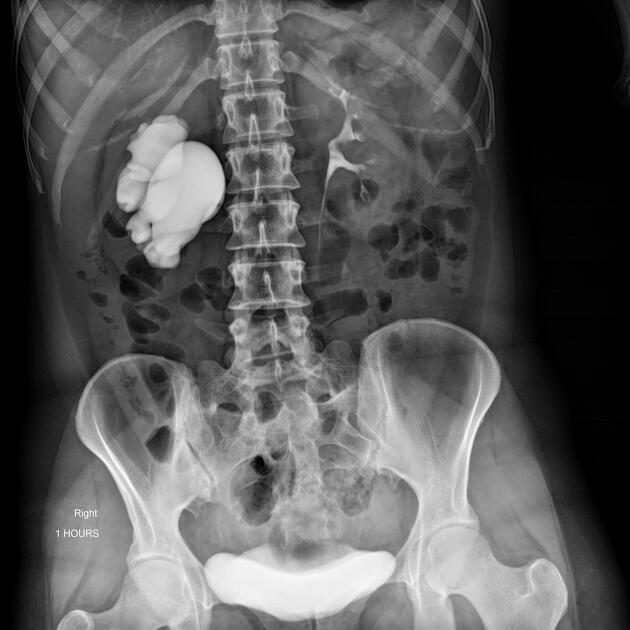
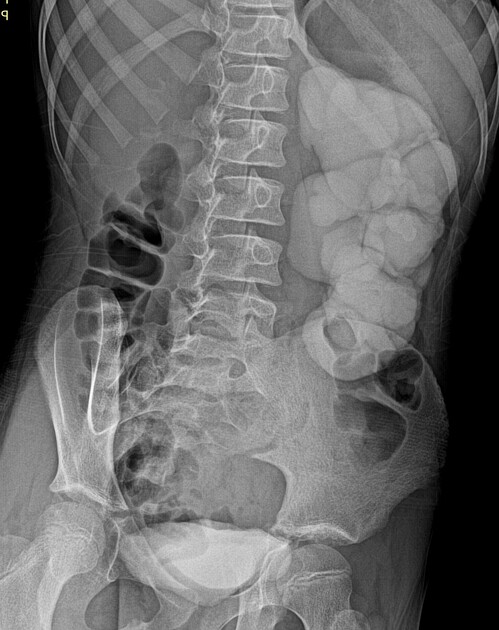
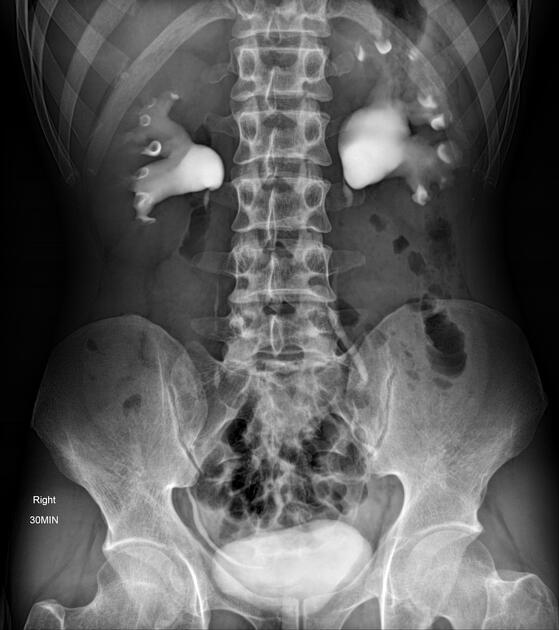
Dilated renal pelvis is described as "ballooned renal pelvis" with collapsed proximal ureter.
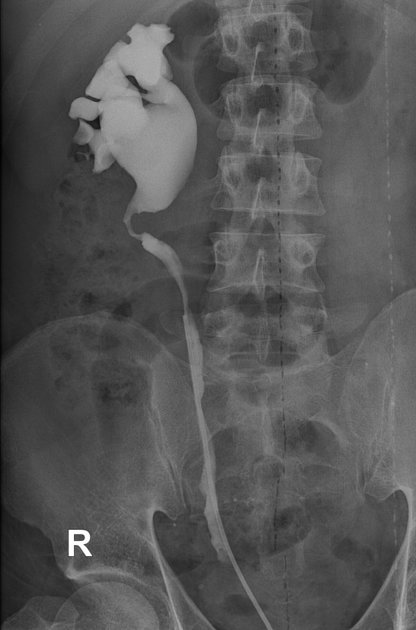
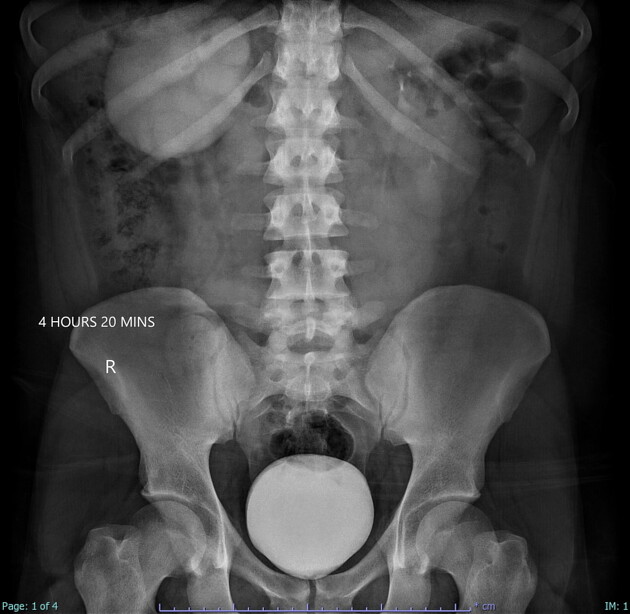
Fluoroscopy/IVU
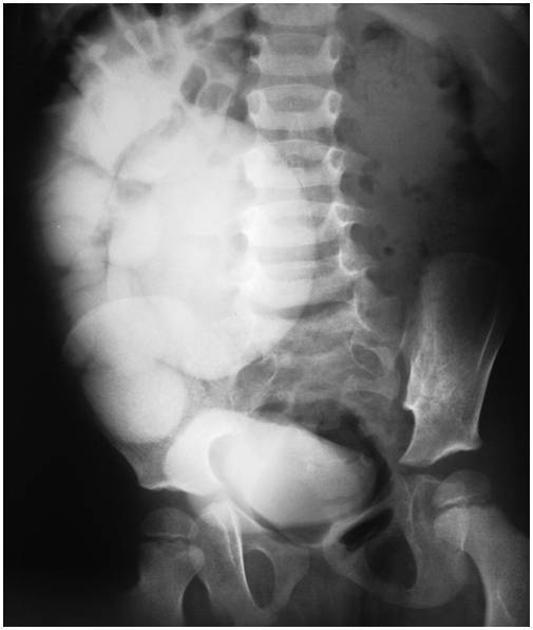
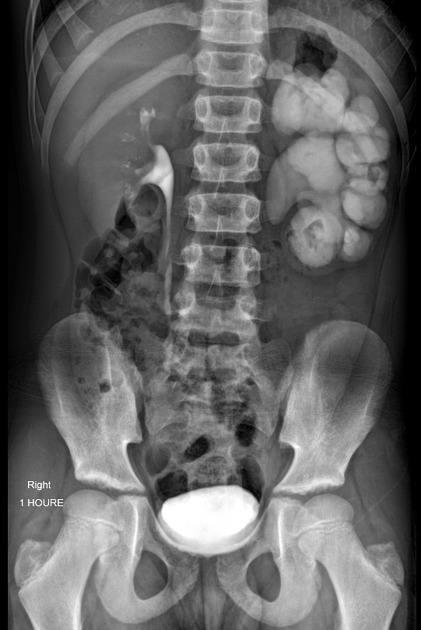
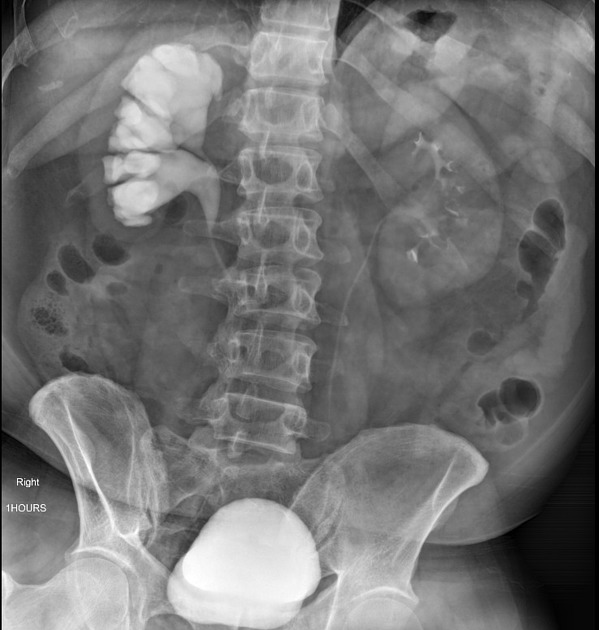
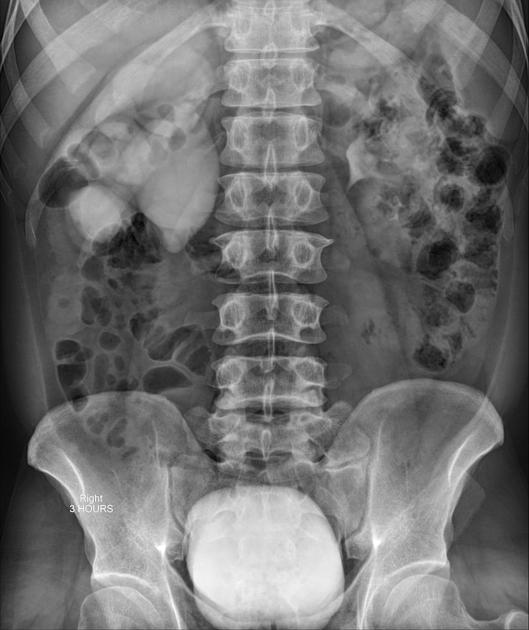
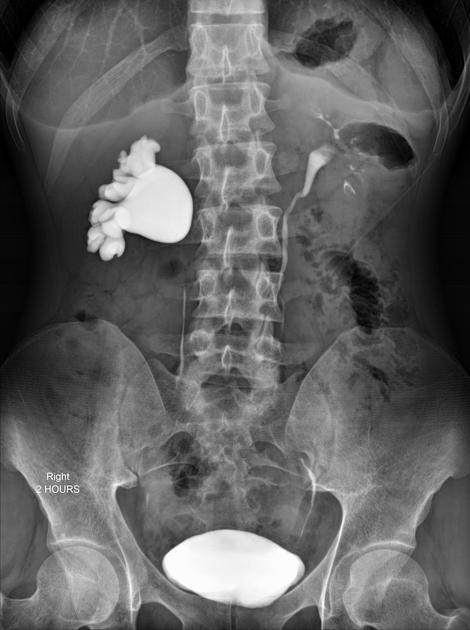
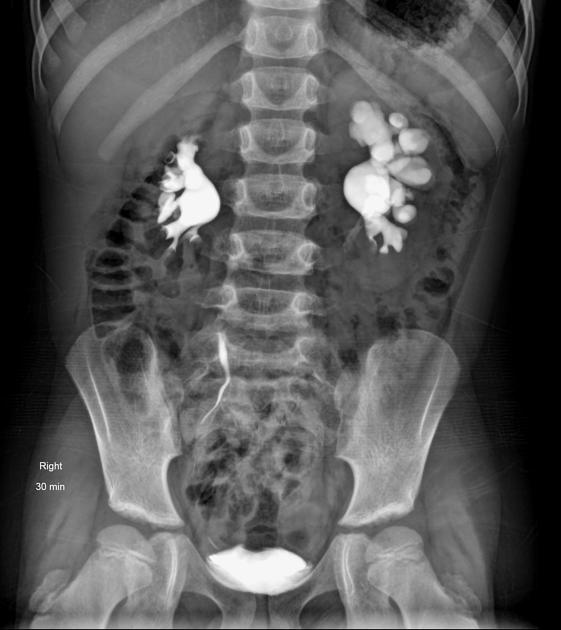
Traditionally intravenous urography/pyelography (IVU/IVP) has been performed for assessing for pelviureteric junction obstruction. The administration of furosemide may be used to assist in confirming the diagnosis, in particular, to exclude a dilated non-obstructed upper collecting system (so-called 'baggy pelvis').
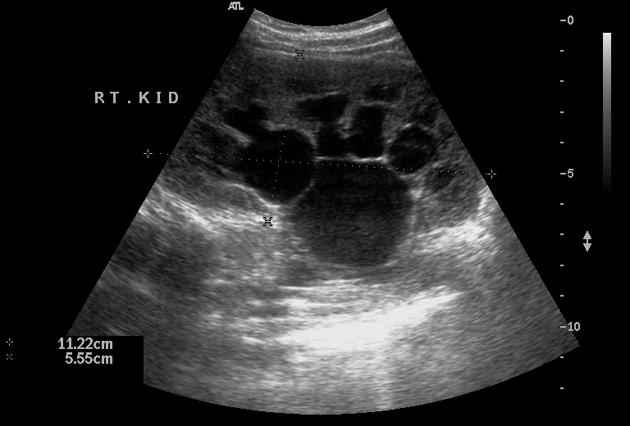
Ultrasound
will often show a dilated renal pelvis with a collapsed proximal ureter
Doppler sonography: the obstructed kidneys may show higher resistive indices
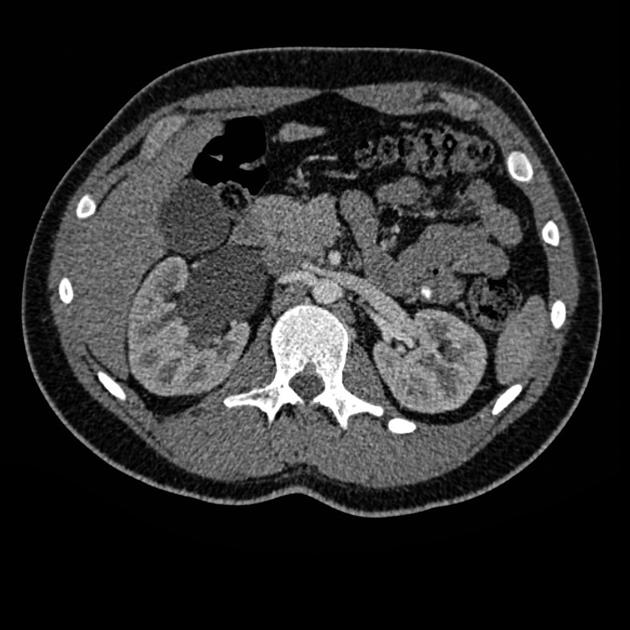
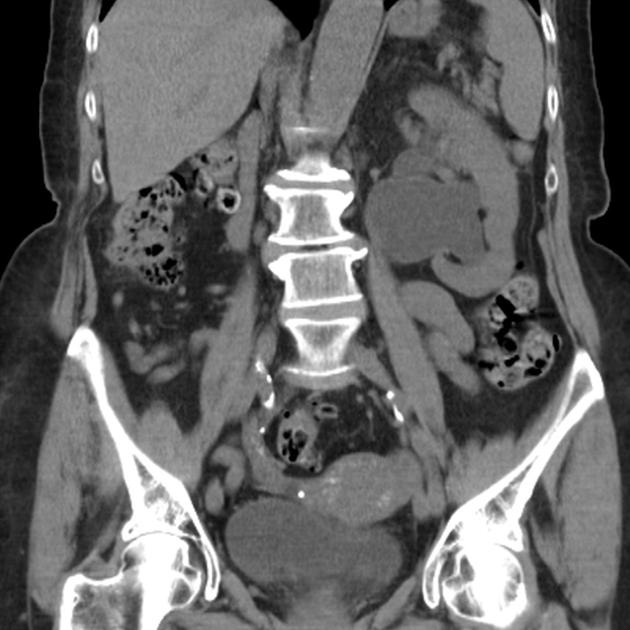
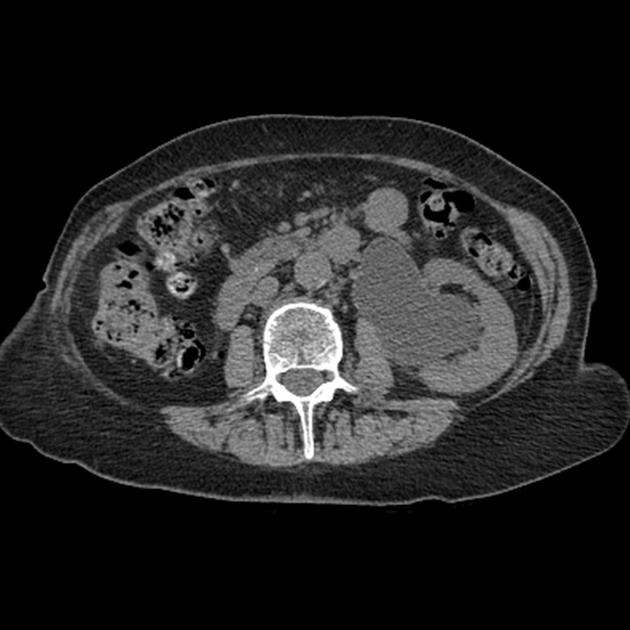
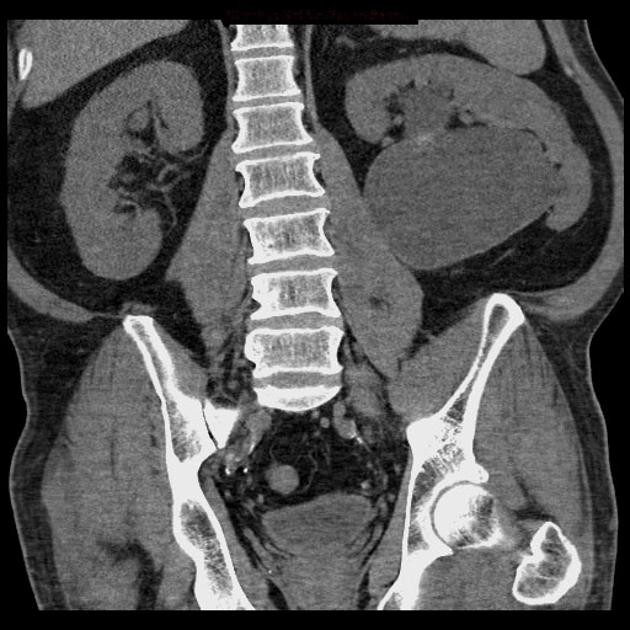
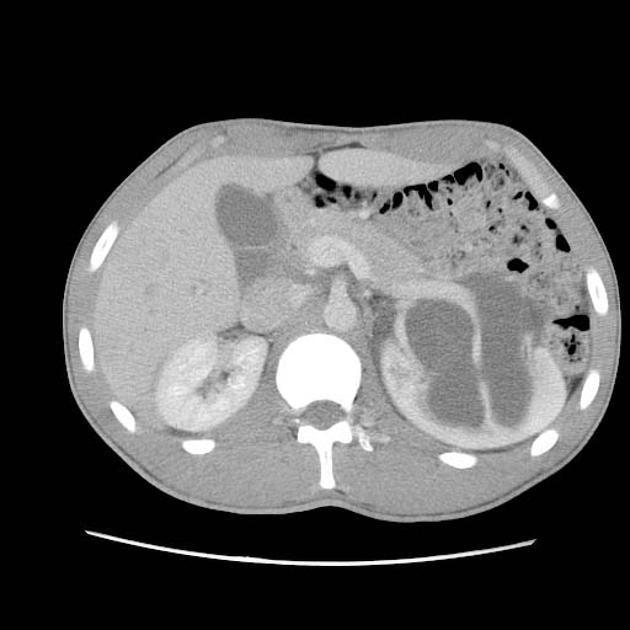
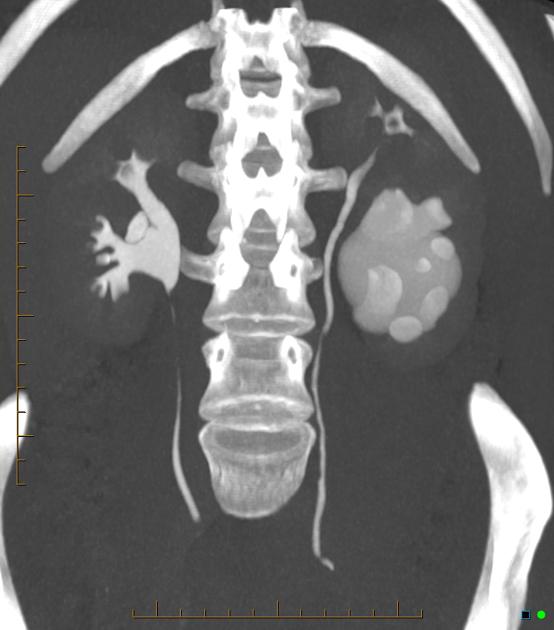
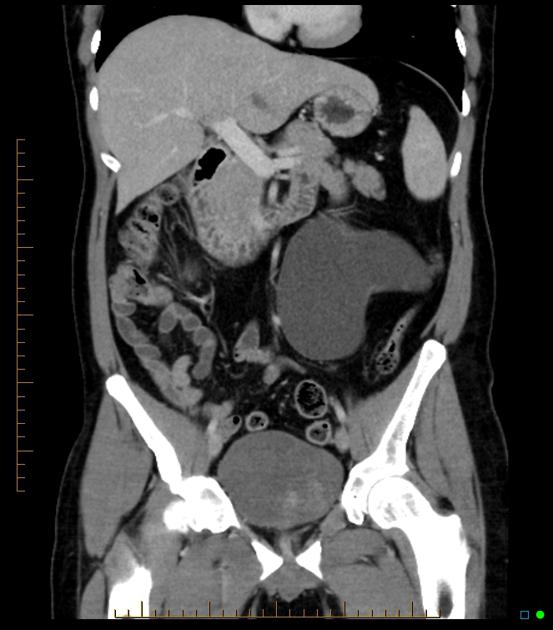
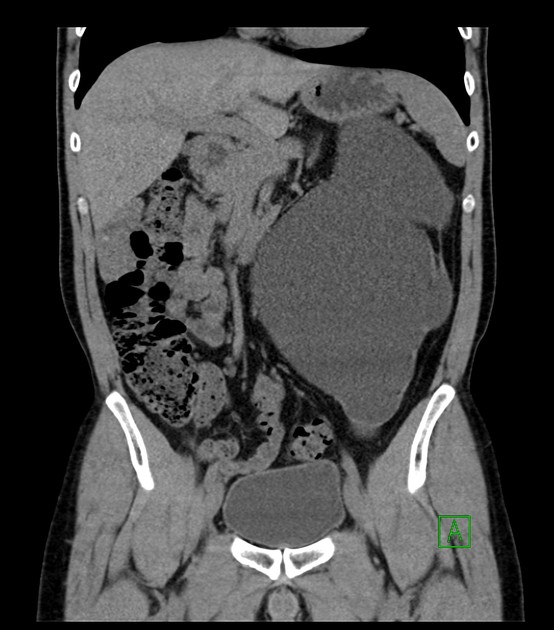
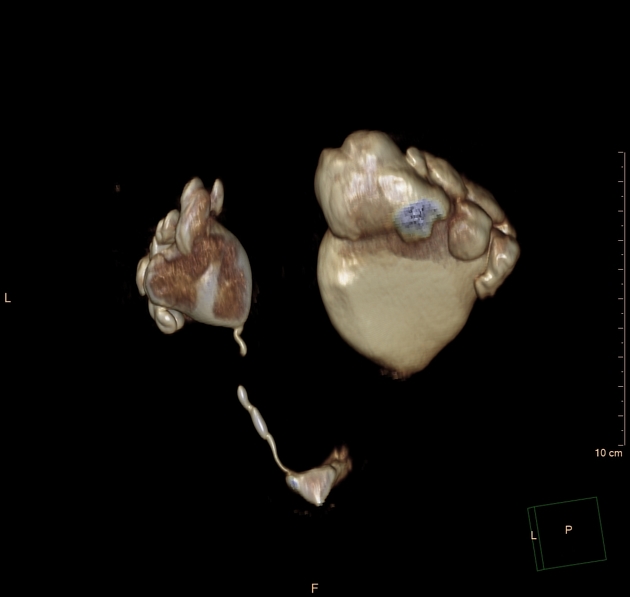
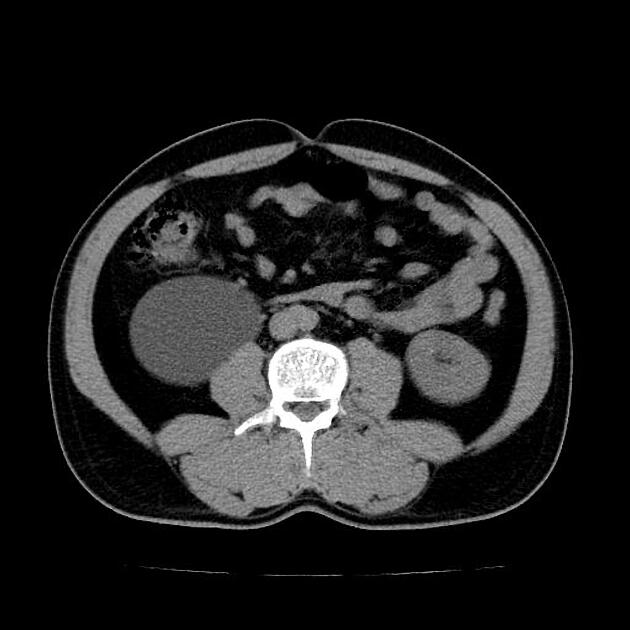
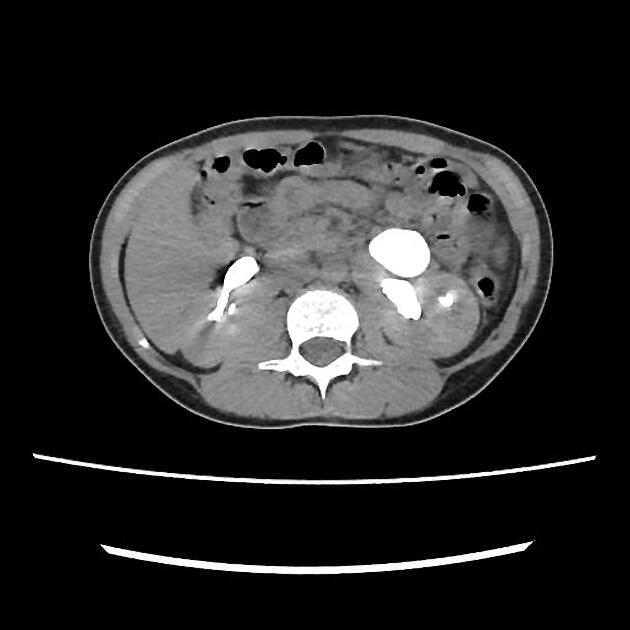
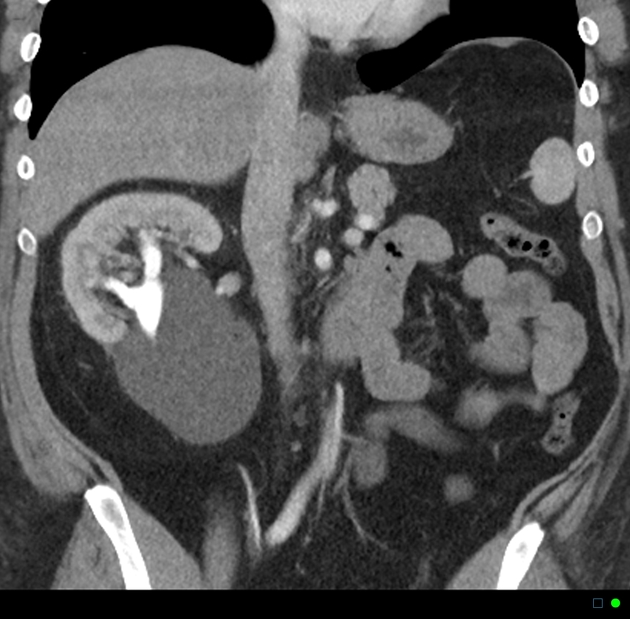
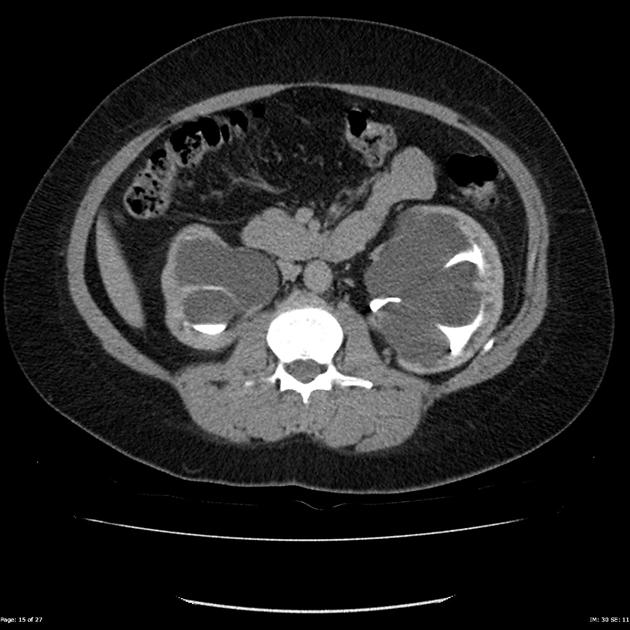
CT
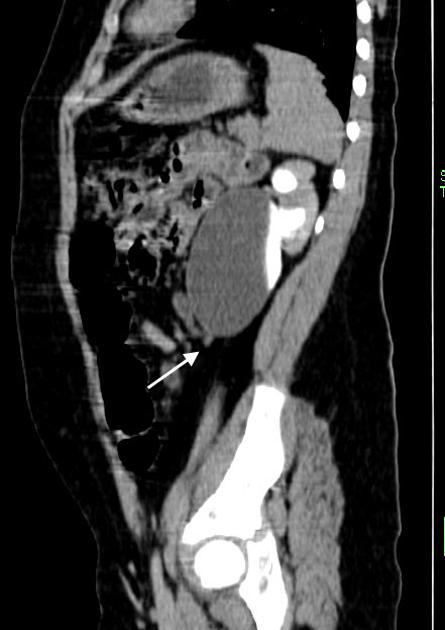
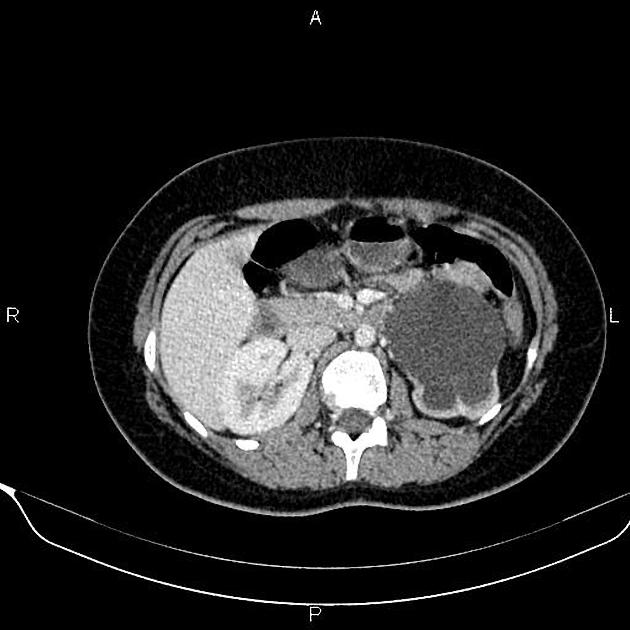
May show evidence of hydronephrosis +/- caliectasis with collapsed ureters. Useful for assessing crossing vessels at the pelviureteric junction, especially when surgical intervention is planned 5,7.
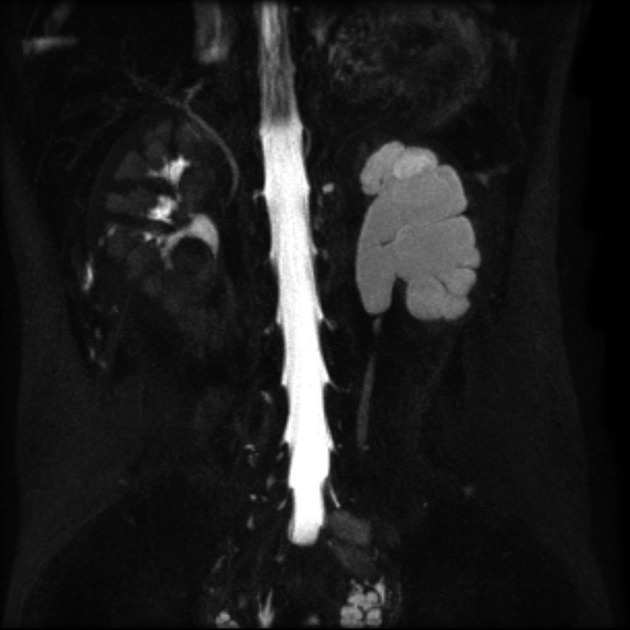
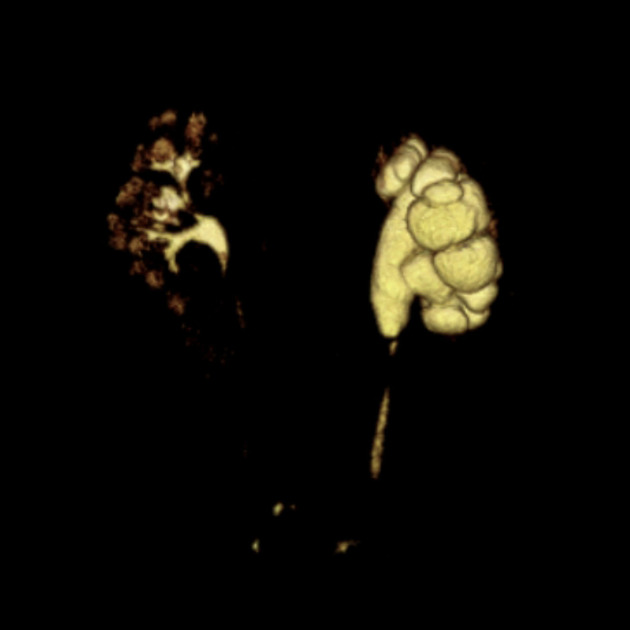
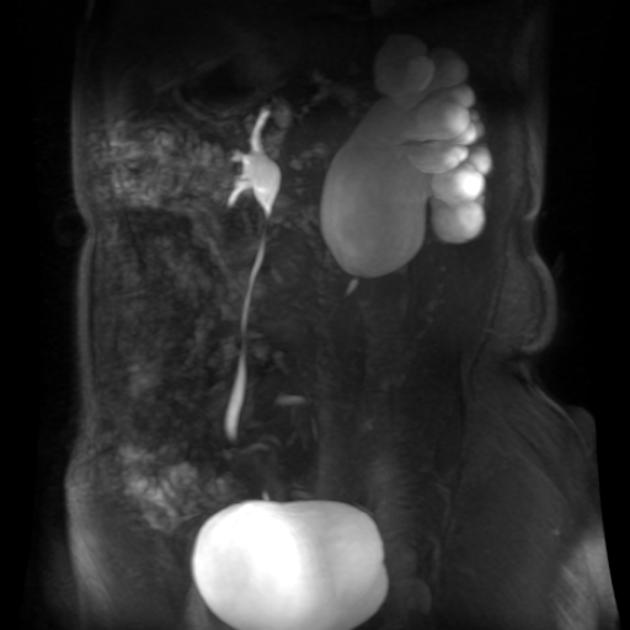
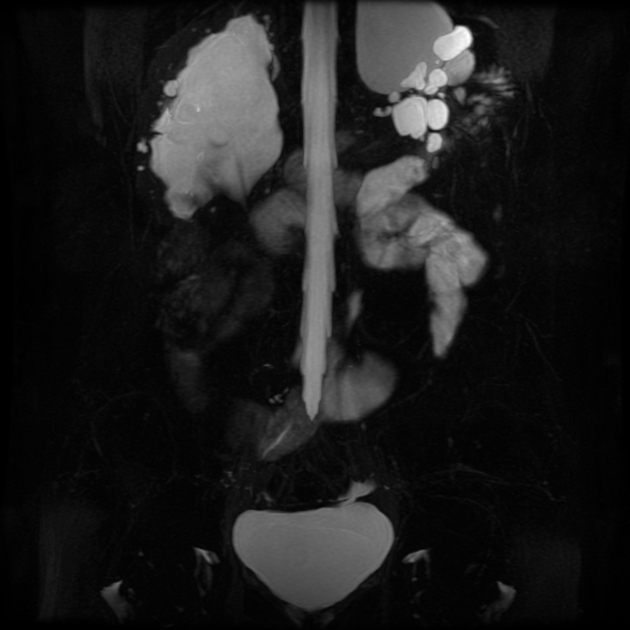
MRI
unilateral or bilateral pelviureteric junction (PUJ) obstruction
upstream hydronephrosis
associated congenital renal abnormalities (MCDK / duplication anomalies/ ectopia etc)
possible source of extrinsic ureteric compression
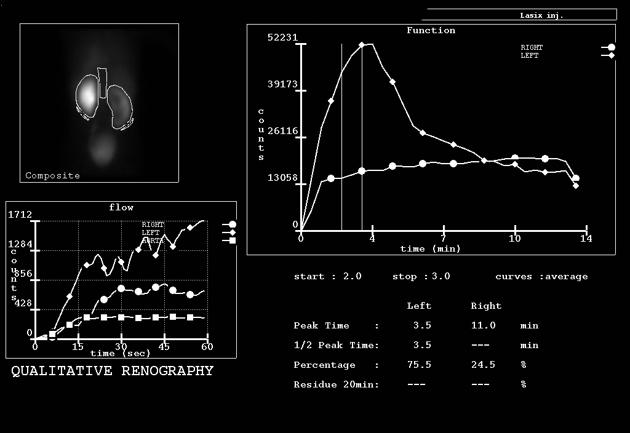
Renal scintigraphy
Renal scintigraphy can quantitate the degree of obstruction:
Tc-99m-MAG3: Agent of choice due to a high extraction rate, which may be necessary for an obstructed system. Diuretic (furosemide) renogram is performed to evaluate between obstructive vs nonobstructive hydronephrosis. The non-obstructive hydronephrosis will demonstrate excretion (downward slope on renogram) after administration of diuretic from the collecting system. Whereas mechanical obstructive hydronephrosis will show no downward slope on renogram, with retained tracer in the collecting system.
Tc-99m-DTPA: Not the agent of choice because of predominantly glomerular filtration of Tc-99m-DTPA. Glomerular function declines earlier and more rapidly than does tubular function in obstructive uropathy. Tc-99m-DTPA may be used if the kidney is known to have good function.
Treatment and prognosis
Treatment depends on the underlying cause. In a majority of congenital cases, the condition is benign, and usually, no intervention is required. However, when there is a definitive structural obstruction (commonly adult cases), surgical intervention with pyeloplasty or stenting may be necessary.
Differential diagnosis
General imaging differential considerations include:
-
central renal pelvis tends to be relatively collapsed
-
calyces are not prominently distended
-
when multiple can be indistinguishable on US or unenhanced CT
IVP or CT with delayed post-contrast phase (CT urography) confirms normal pelvicalyceal system in between the cysts












 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.