Intracranial germinomas, also known as dysgerminomas or extra-gonadal seminomas, are a type of germ cell tumor and are predominantly seen in pediatric populations. They tend to occur in the midline, either at the pineal region (majority) or along the floor of the third ventricle/suprasellar region.
On this page:
Epidemiology
Germinomas are tumors of young patients with a peak incidence of 10-12 years of age (90% of patients being younger than 20 at the time of diagnosis). They account for 3-5% of pediatric intracranial tumors but only 0.4-1% of intracranial tumors in adults 10.
They are the most common tumor of the pineal region accounting for approximately 50% of all tumors, and the majority (73-86%) 10 of intracranial germ cell tumor.
Gender ratios are interestingly different depending on location. In the pineal region there is a marked male preponderance with a male to female ratio of 5-22:1 whereas in the suprasellar region, they are slightly more frequent in females with a male to female ratio of 1:1.3. Overall, due to the pineal region being most common, germinomas are seen more frequently in males.
Clinical presentation
Presentation depends on location, with compression of the tectal plate leading to obstructive hydrocephalus and Parinaud syndrome, whereas involvement of the pituitary infundibulum leads to diabetes insipidus (most common), hypopituitarism (common), optic chiasm compression or signs of intracranial hypertension 11. When the thalami and basal ganglia are involved, the presentation is often delayed with a larger tumor at diagnosis.
Pathology
Germinomas derive from germ-cells and typically arise in the midline, relating to the third ventricle 11:
pineal gland: 80-90%, known as a pineal germinoma in this location
suprasellar mass: 15-40%, termed a suprasellar germinoma in this location
-
paraventricular parts of the basal ganglia and thalamus: 5-10%
more frequently seen in Asian populations
both pineal and suprasellar region: 6-13%, termed bifocal germinoma 11
Radiographic features
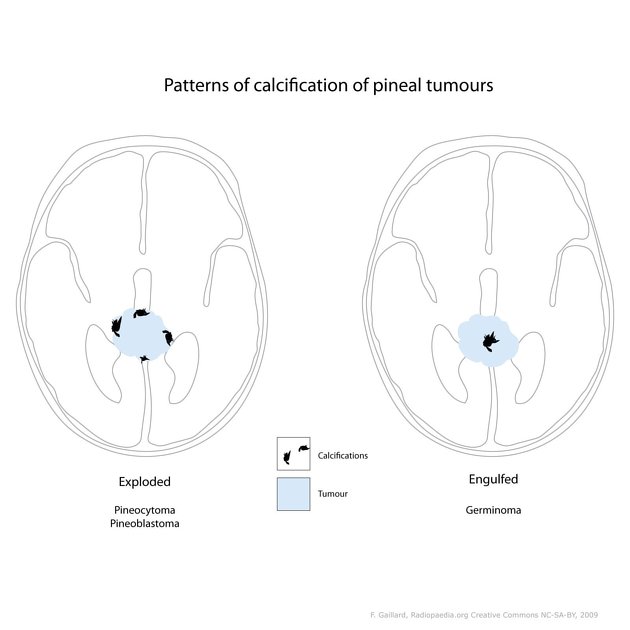
Germinomas are soft tissue density, enhancing masses. When present in the pineal region they appear to "engulf" the normal pineal tissue and can have associated central calcification, in contrast to pineocytomas, and pineoblastomas which are described as "exploding" the foci of calcification. Cystic components are commonly found in up to 45% of cases.
CT
On CT, the high cellularity of these tumors results in hyperdensity compared to adjacent brain. Usually, the mass enhances brightly.
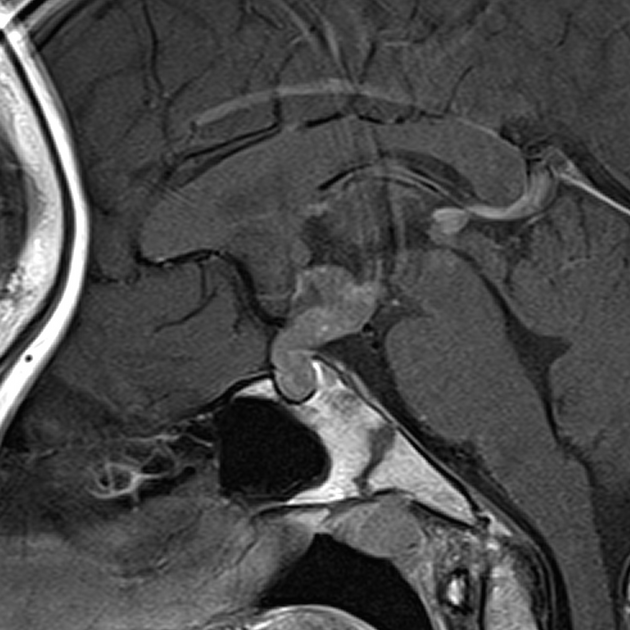
When in the floor of the third ventricle it is typically seen filling and expanding the infundibular recess and supraoptic recess. Imaging may, however, be normal initially and if the diagnosis is suspected clinically (e.g. idiopathic hypothalamic diabetes insipidus) then a close follow-up is required to identify potentially very subtle abnormal pituitary stalk enhancement and thickening.
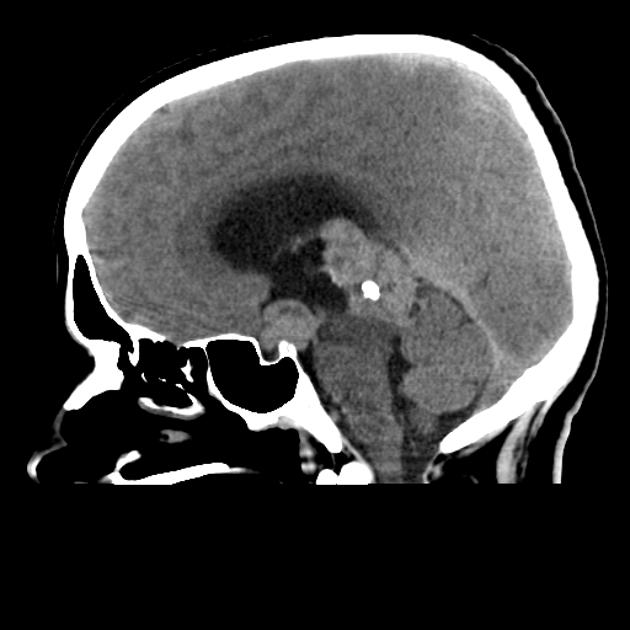
In the pediatric population presence of calcification in the pineal region is a useful marker of an underlying tumor, as no calcification of the pineal is seen in children below the age of 6.5 and only ~10% of children between 11 and 14 years of age.
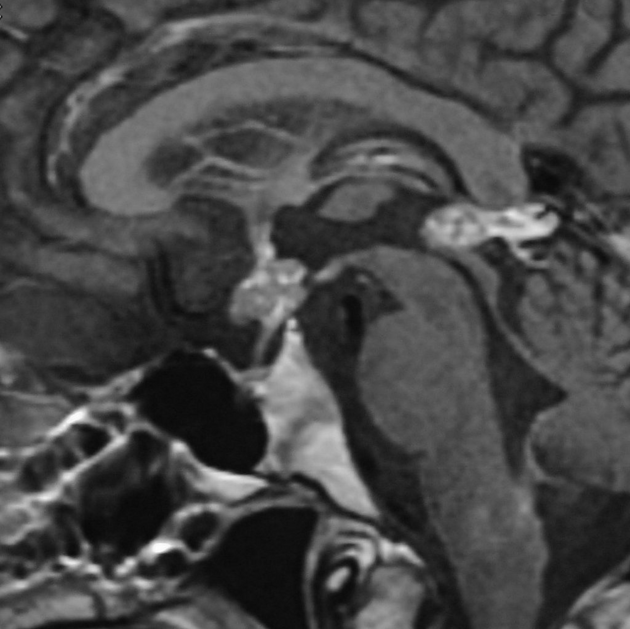
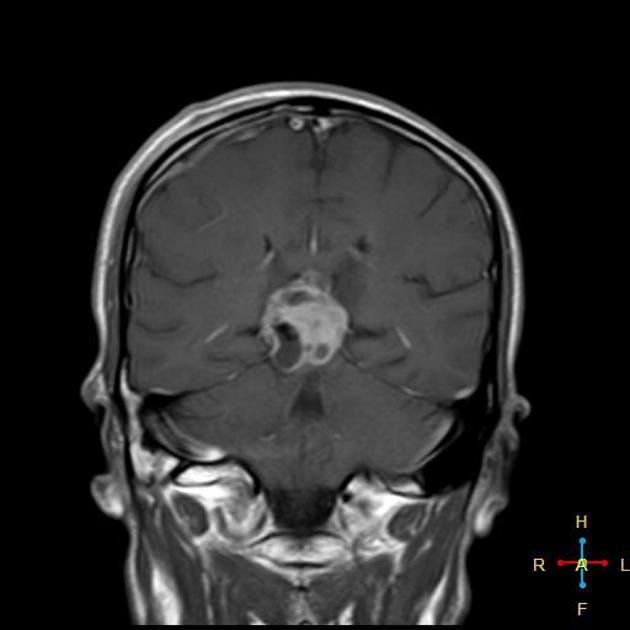
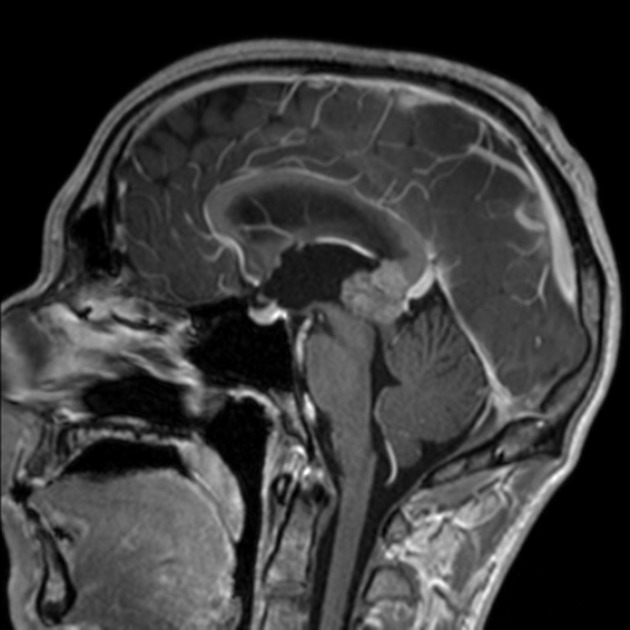
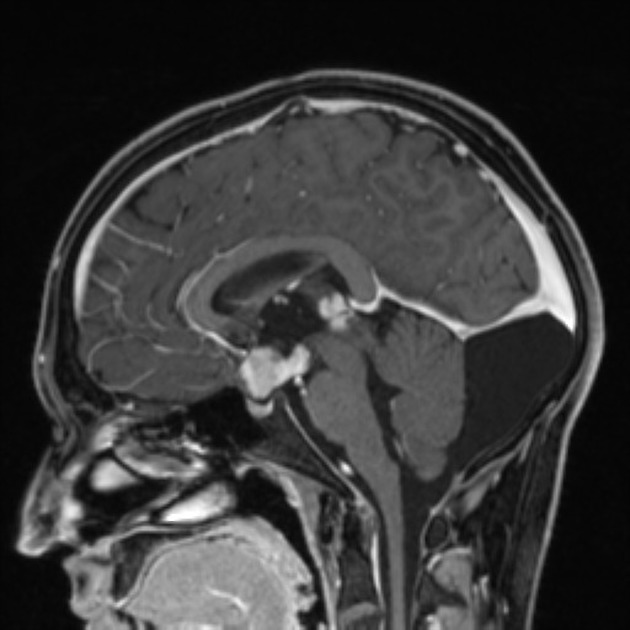
MRI
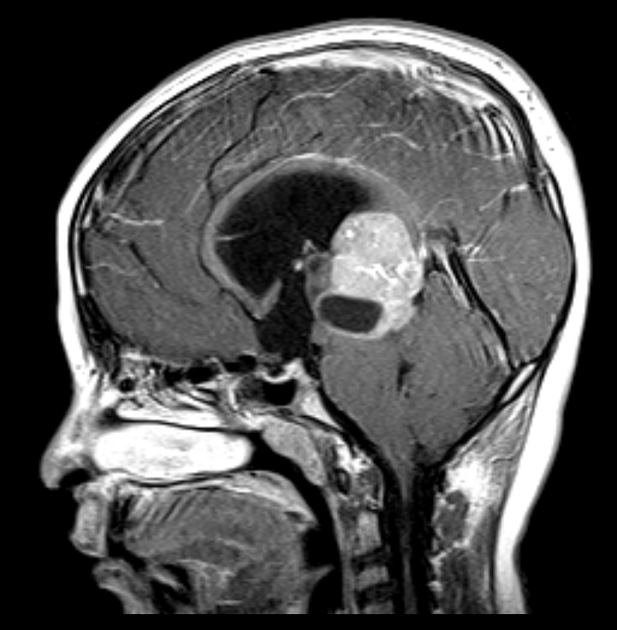
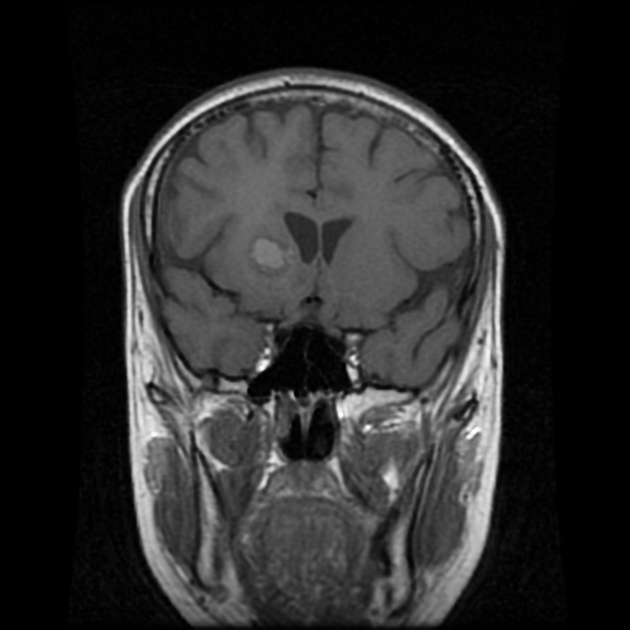
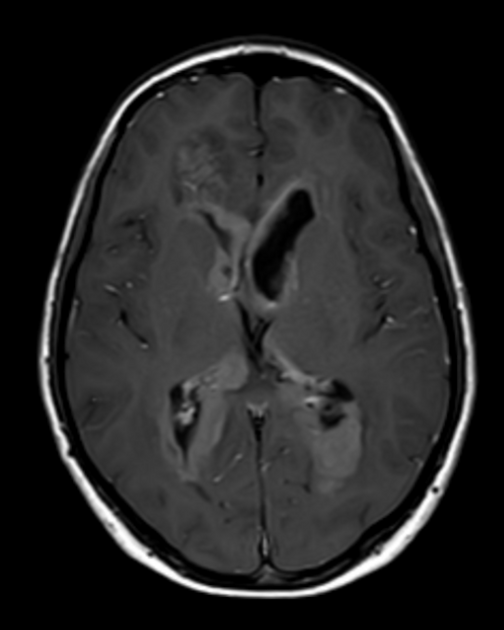
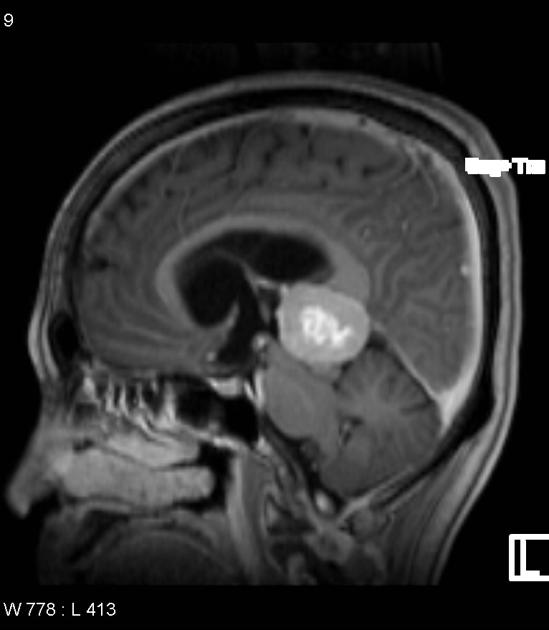
MRI demonstrates a soft tissue mass, typically ovoid or lobulated in contour, engulfing the calcified pineal gland with the following signal characteristics 12:
T1: isointense or slightly hyperintense to adjacent brain
-
T2
isointense or slightly hyperintense to adjacent brain
may have areas of cyst formation
may have areas of hemorrhage (low signal)
have a predilection for invading adjacent brain (edema)
central calcification appears low signal (engulfed pineal gland)
T1 C+ (Gd): vivid and homogeneous
Treatment and prognosis
The mainstay of treatment is with radiotherapy which offers ~85% (range 79-90%) long-term cure rate 10. Leptomeningeal seeding or spillage during surgery are thought to be poor prognostic factors. Imaging of the entire neuraxis is therefore recommended before irradiation.
Overall the prognosis is good, with over 90% 5-year survival with chemotherapy and radiotherapy.
Differential diagnosis
The differential can depend on location:
for lesions in the pineal region: refer to the pineal mass article
for lesions in the suprasellar region: refer to the suprasellar mass article





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.