Mediastinal lymphoma is common, either as part of disseminated disease or less commonly as the site of primary involvement.
On this page:
Epidemiology
Lymphomas are responsible for approximately 15% of all primary mediastinal masses, and 45% of anterior mediastinal masses in children 1.
Only 10% of lymphomas that involve the mediastinum are primary (i.e. mediastinal involvement not part of systemic disease) and the majority are Hodgkin lymphomas (~60%) 5.
Clinical presentation
The mediastinum is commonly involved in systemic lymphomas. Approximately 60% of all Hodgkin lymphoma and 20% of non-Hodgkin lymphoma involves the mediastinum at presentation. Less frequently, the disease is isolated to the mediastinum (3% Hodgkin lymphoma, <10% non-Hodgkin lymphoma) 1. As such, patients are often asymptomatic from the mediastinal component but present with systemic manifestations of lymphoma, most commonly constitutional symptoms 5.
Symptoms directly attributable to the mediastinal component include 4,5:
retrosternal chest pain
dyspnea
cough
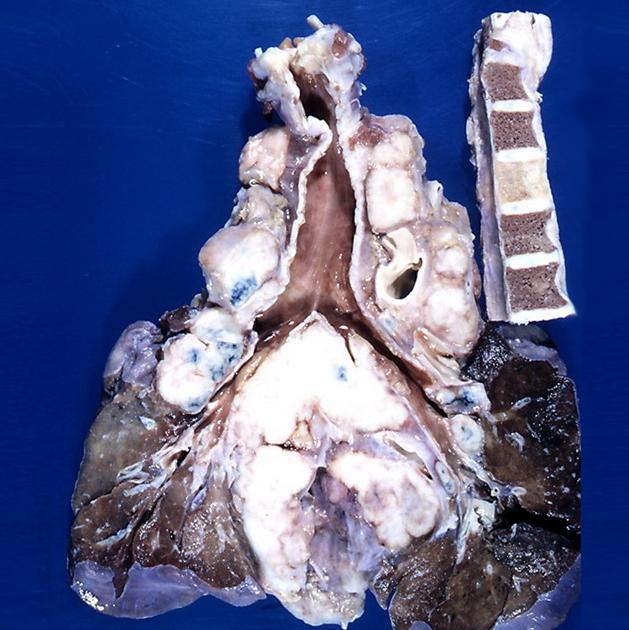
Pathology
Mediastinal lymphomas usually arise from either the thymus or lymph nodes, thus accounting for their predilection for the anterior and middle mediastinum 1. The anterior mediastinal and paratracheal nodes are the most frequently involved regions while isolated hilar node enlargement is uncommon without accompanying mediastinal node enlargement. Posterior mediastinal involvement is also infrequent.
Classification
The World Health Organization classification of neoplastic diseases of the lymphoid tissues includes lymphomas and leukaemias, and is according to the cell of origin, with the main division being:
B-cell neoplasms
T-cell and natural killer cell neoplasms
Primary mediastinal lymphomas are most frequently of three histologic varieties 5:
nodular sclerosing Hodgkin lymphoma
lymphoblastic lymphoma
Radiographic features
The majority of patients have anterior mediastinal and paratracheal involvement. Isolated hilar nodal involvement is uncommon 6.
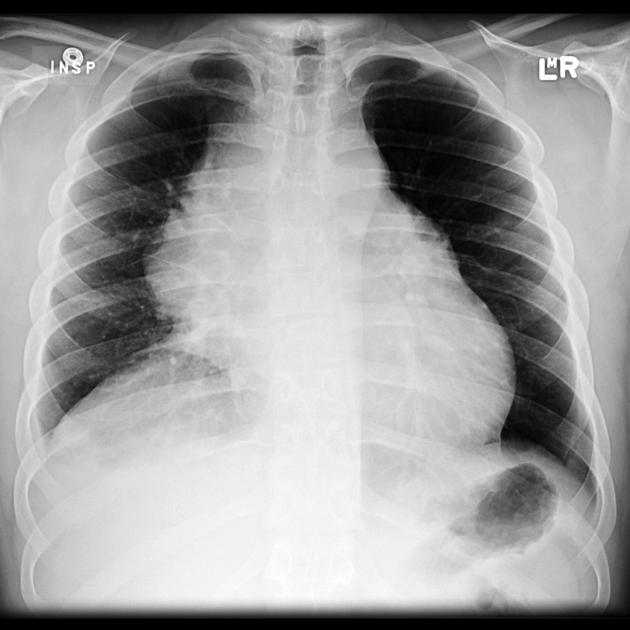
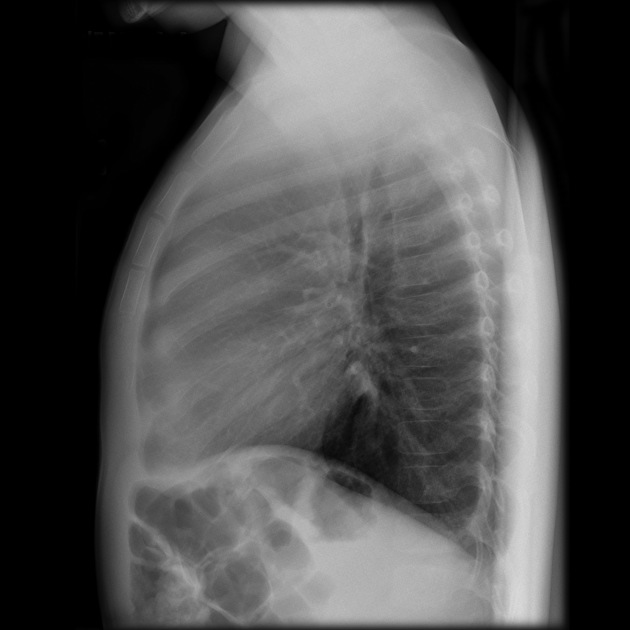
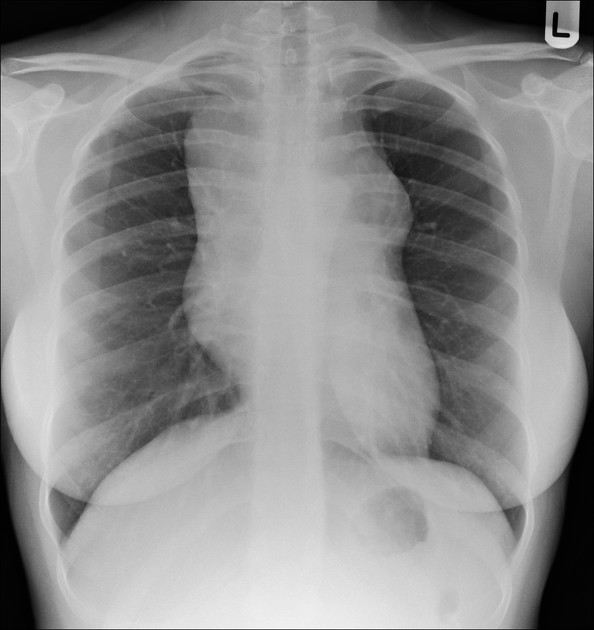
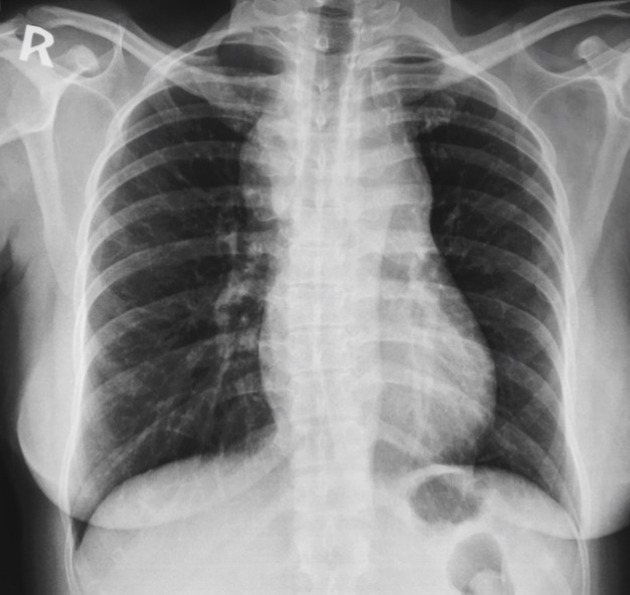
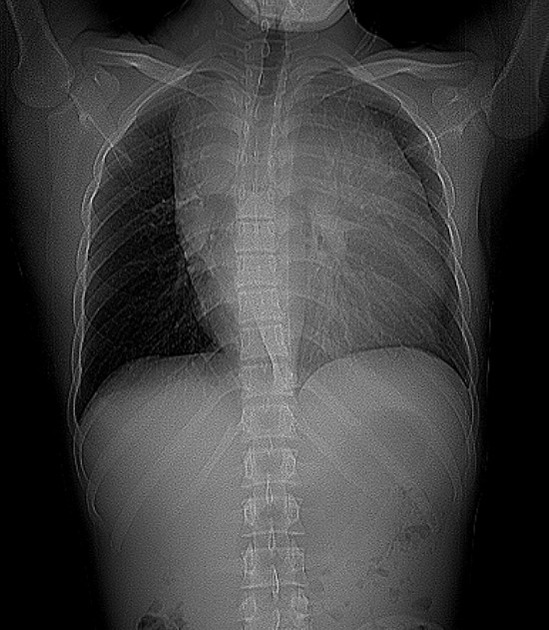
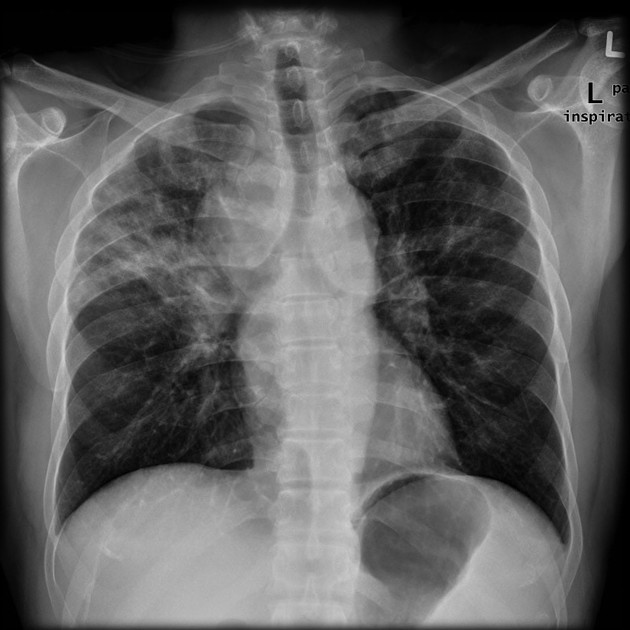
Plain radiograph
A soft tissue mass may be clearly visible, or more frequently the mediastinum is widened, and the retrosternal airspace is obscured.
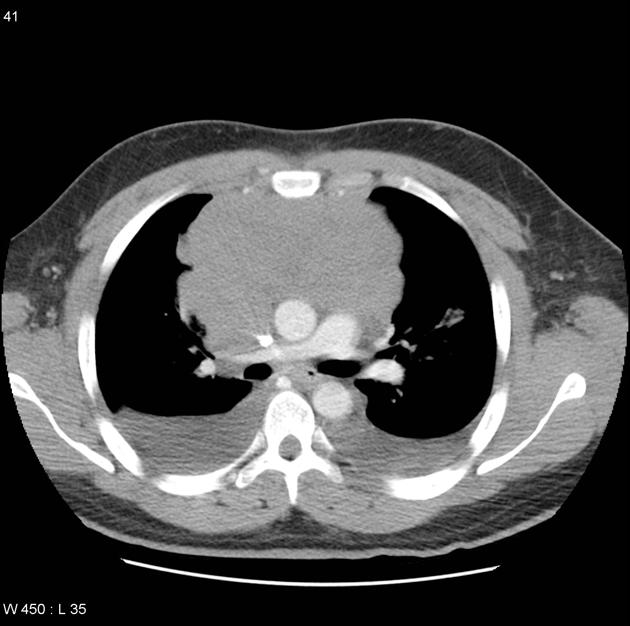
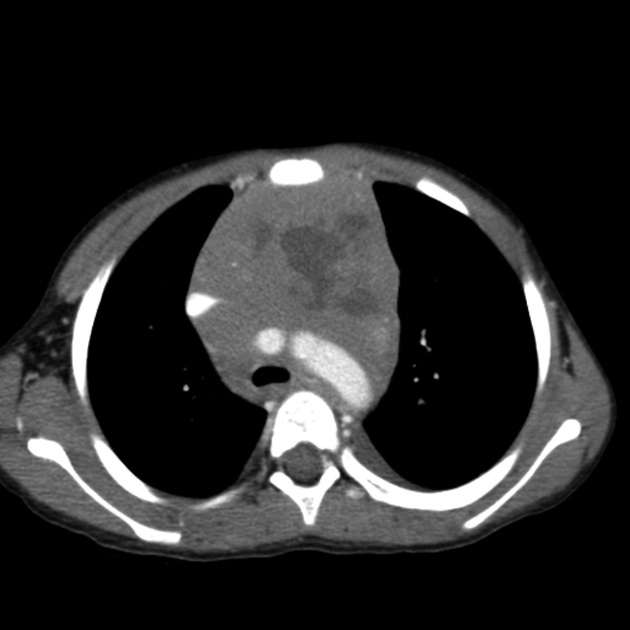
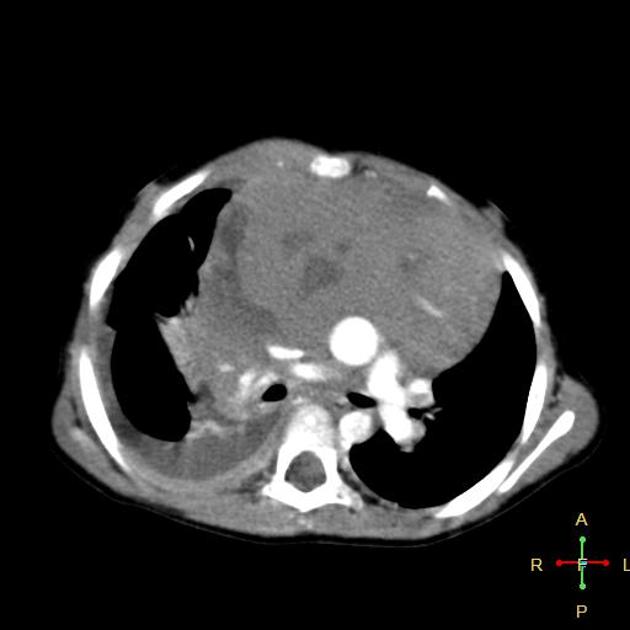
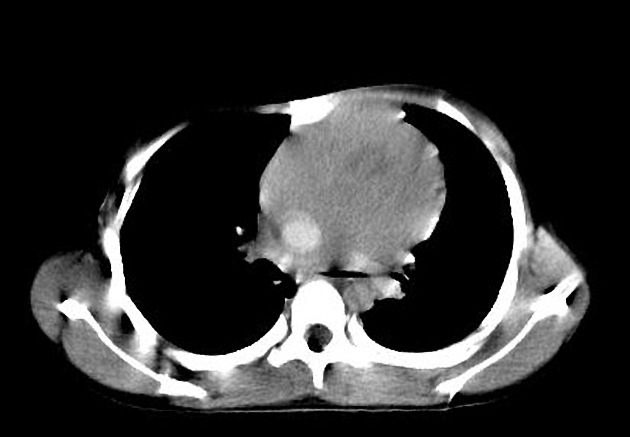
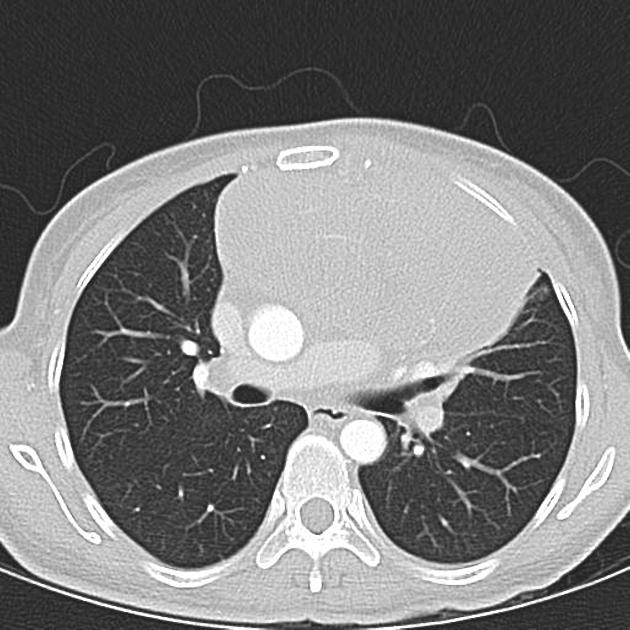
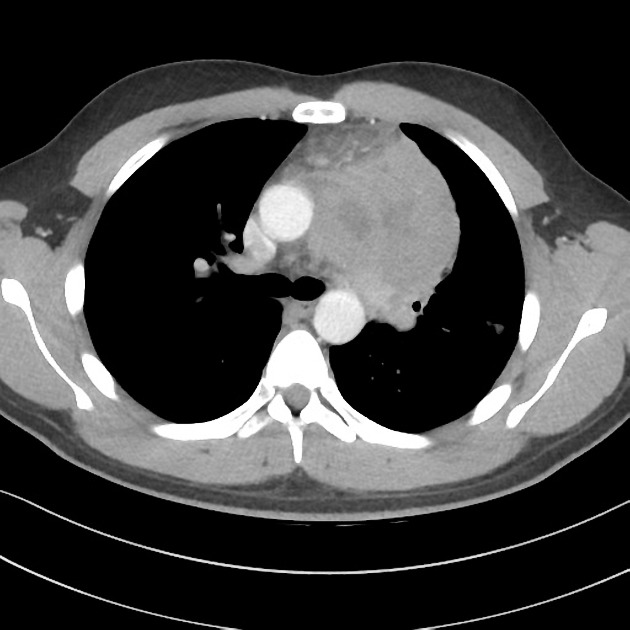
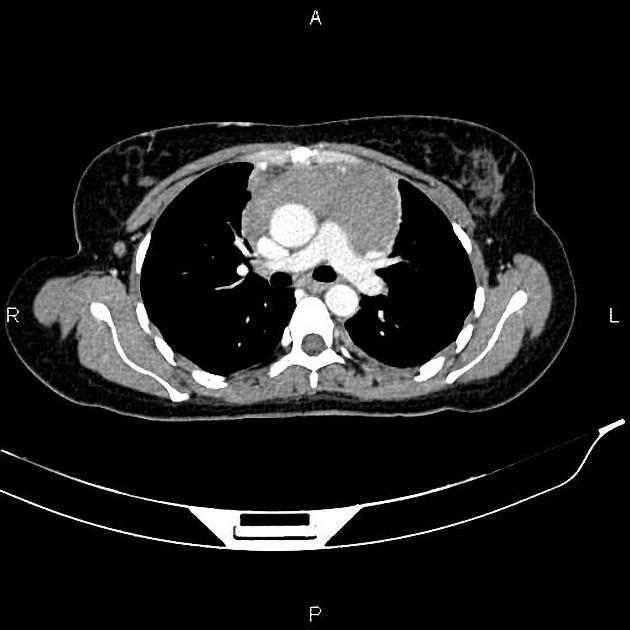
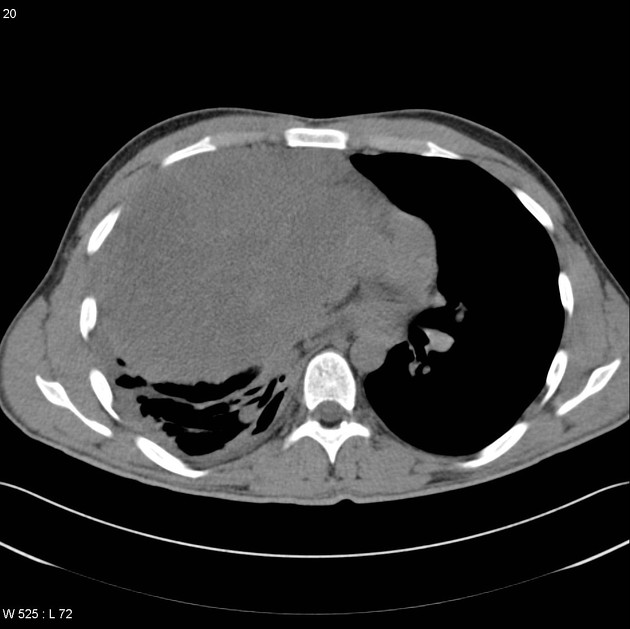
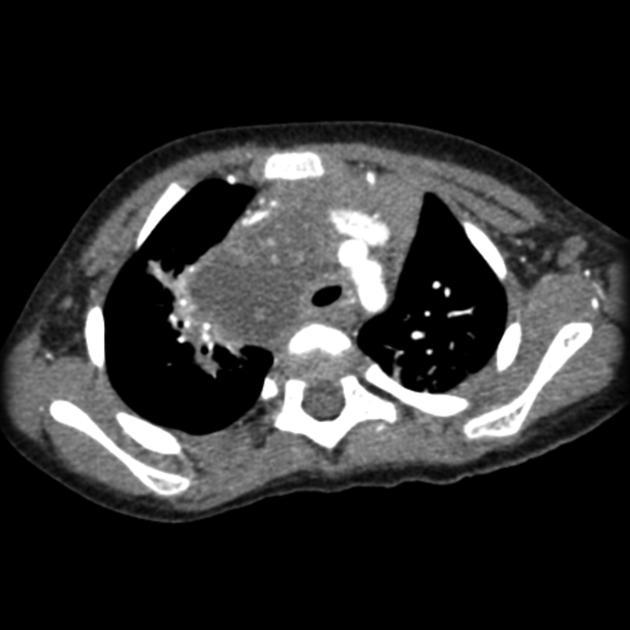
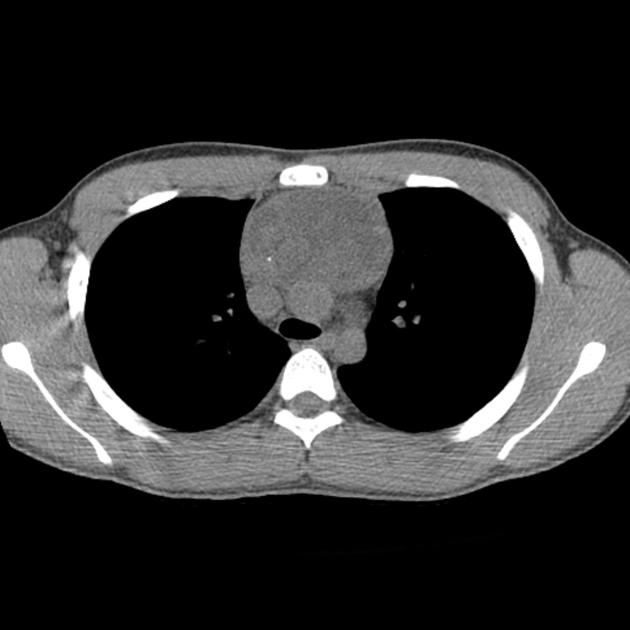
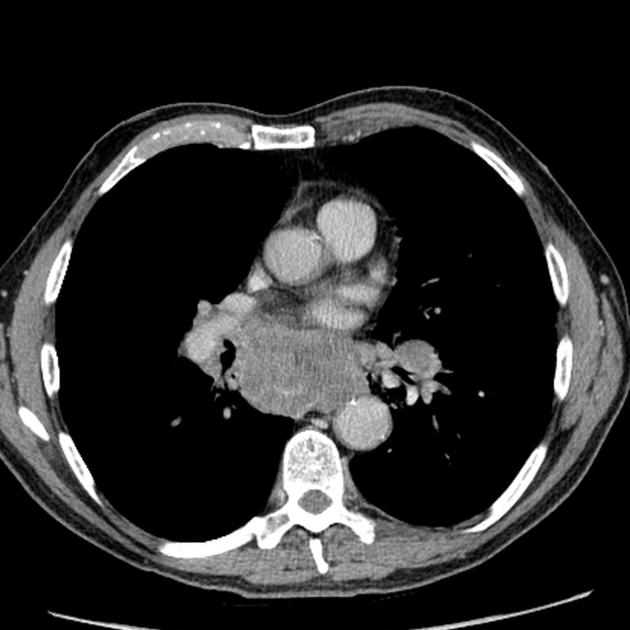
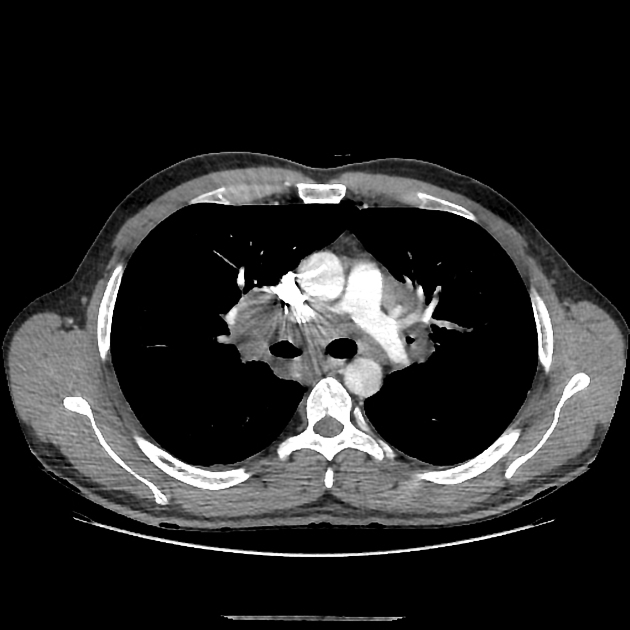
CT
CT demonstrates a soft tissue attenuating mass, with smooth or lobulated margins which conform to surrounding structures. Cystic low-density areas are common. Other features include 6:
parenchymal invasion: uncommon
-
seen in 50% of cases
usually unilateral
usually exudates
pleural deposits may be present
chest wall invasion
Calcification is usually seen following therapy and can have varying morphology, including irregular, diffuse or even eggshell 6.
Following treatment nodal masses usually reduce in size, however in some instances, the size of the mass remains the same or even increases (in cases of thymic hyperplasia) 2. As such CT is not ideal for assessing for treatment response when a decrease in size is not present.
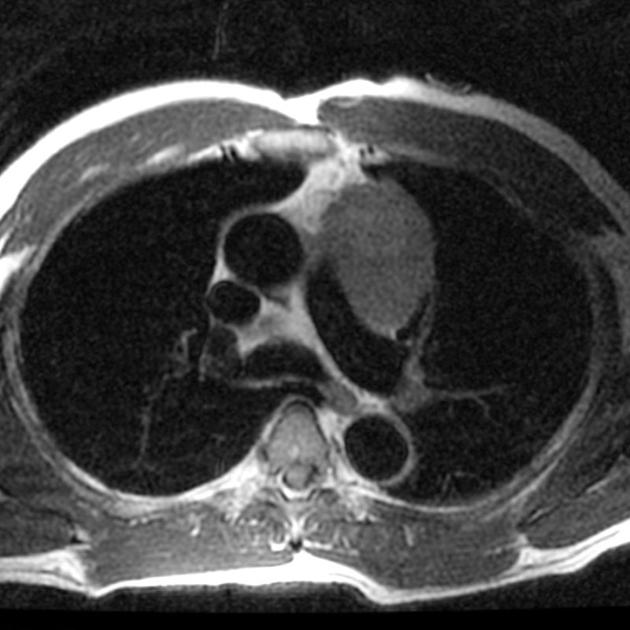
MRI
The appearance of lymphomas on MRI varies with treatment and the type of lymphoma 2.
T1: hypo/isointense to muscle
-
T2
variable, typically hyperintense
after treatment: hypointense
-
T1 C+ (Gd)
avid enhancement
-
after treatment:
decreased enhancement (persistent enhancement suggests residual tumor) 2
may be more heterogeneous due to necrosis and fibrosis
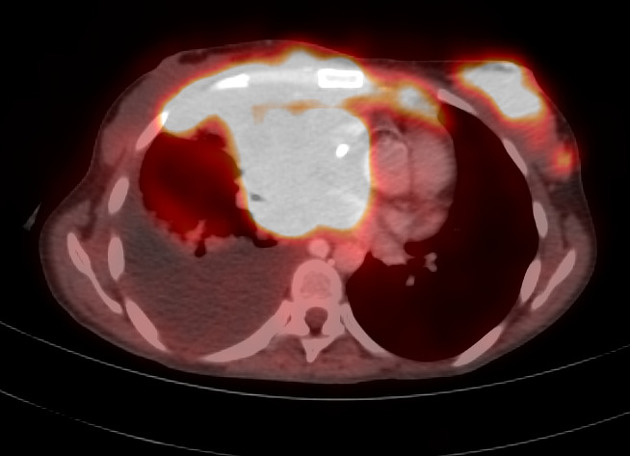
Nuclear medicine
Gallium and FDG-PET
Both gallium-67 scintigraphy and FDG-PET are better able to assess for tumor viability following treatment than CT, as residual mass does not necessarily represent residual viable neoplastic tissue 2.
Unfortunately, up to 20% of cases are gallium negative at diagnosis 2.
Treatment and prognosis
Specific treatment depends on the type of lymphoma and the stage, but broadly requires chemotherapy and or radiotherapy 5.
Similarly, the prognosis is very variable. Stage I and II Hodgkin lymphoma have the best prognosis with a greater than 90% cure rate 5.
Complications
Complications include:
-
vascular compression 4
compression of the aorta
compression of the pulmonary arteries
Differential diagnosis
On chest radiography, the differential is that of mediastinal lymph node enlargement and of an anterior mediastinal mass.
On CT the differential diagnosis includes:
infection: especially tuberculosis





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.