Chondromyxoid fibromas (CMF) are extremely rare, benign cartilaginous neoplasms that account for <1% of all bone tumors 1.
CMF accounts for one of the 'C's in the popular mnemonic for lucent bone lesions FEGNOMASHIC.
On this page:
Epidemiology
As with all rare lesions, reported epidemiology varies:
-
age:
most commonly diagnosed before 30 years of age (~75%), mostly during second and third decades 1,12-15
full reported range from 3 to 70 years of age
-
gender:
conflicting data 2,12,18
some series show slight male predilection 15
Clinical presentation
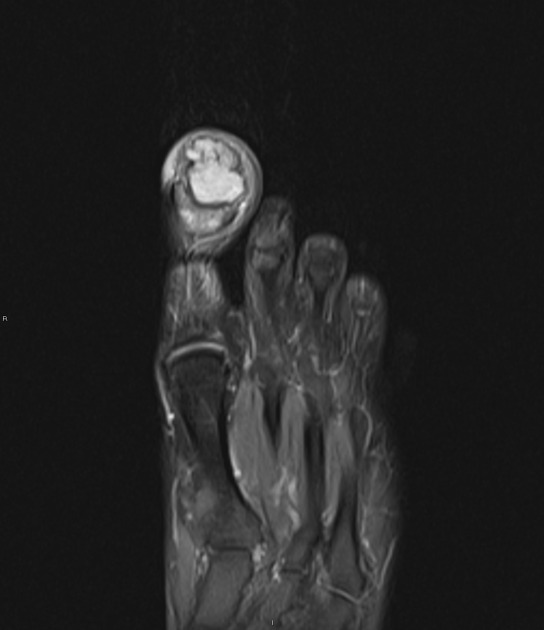
Typically patients present with progressive pain, often long-standing and/or bony swelling and restricted range of movement in the affected limb 3,12. The latter is most often the case in bones with little overlying soft tissues (e.g. short tubular bones of the hands and feet).
Pathology
Microscopic examination, the tumor comprises of a variable combination of chondroid, myxoid, and fibrous tissue components organized in a pseudolobulated architecture 20. Additionally, occasional osteoclast-like giant multinucleated cells are encountered particularly at the periphery. Most cells are morphologically bland, and mitotic figures are rare or absent 13.
Macroscopic appearance
On gross examination, they are typically seen as solid glistening tan-grey intraosseous masses.
Location
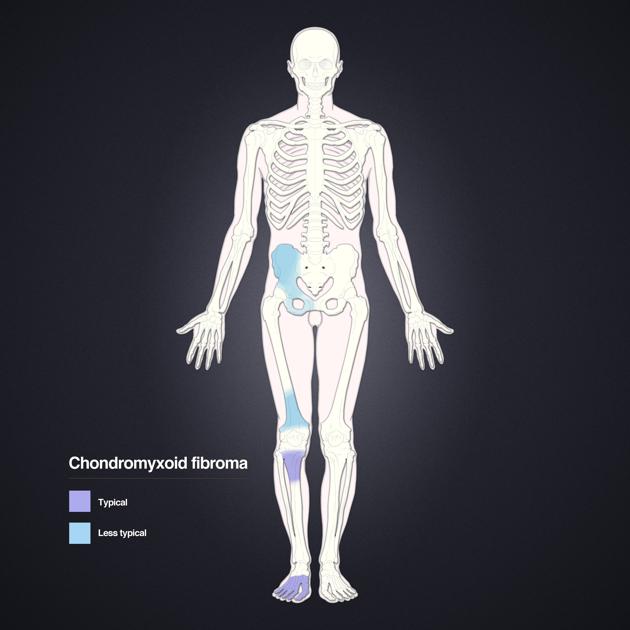
Most chondromyxoid fibromas are located in the metaphyseal region of long bones (60%) and may extend to the epiphyseal line and even rarely abut the articular surface 3,12. They are almost never exclusively epiphyseal 3.
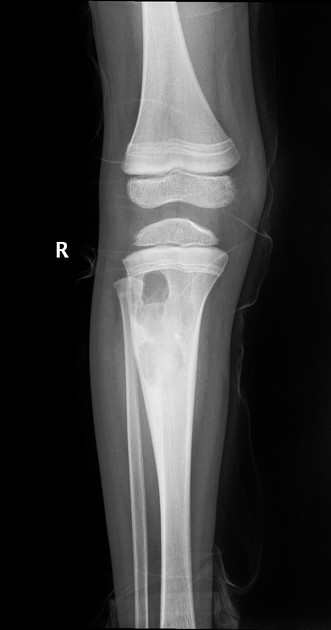
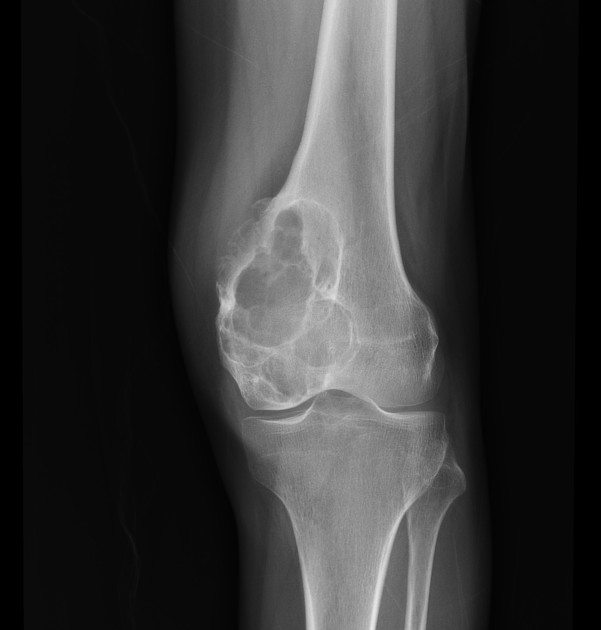
The classical site is the upper one-third of the tibia, which accounts for 25% of all cases, with the small tubular bones of the foot, the distal femur, and pelvis/sacrum being other relatively common locations 12.
Rare cases involving the calvarium/skull base 25-27, and mandible 28, as well as the sternum 29 have been reported.
Radiographic features
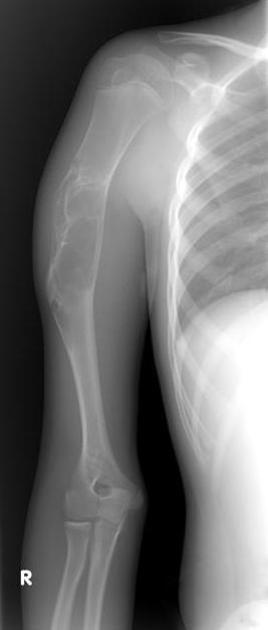
Plain radiograph
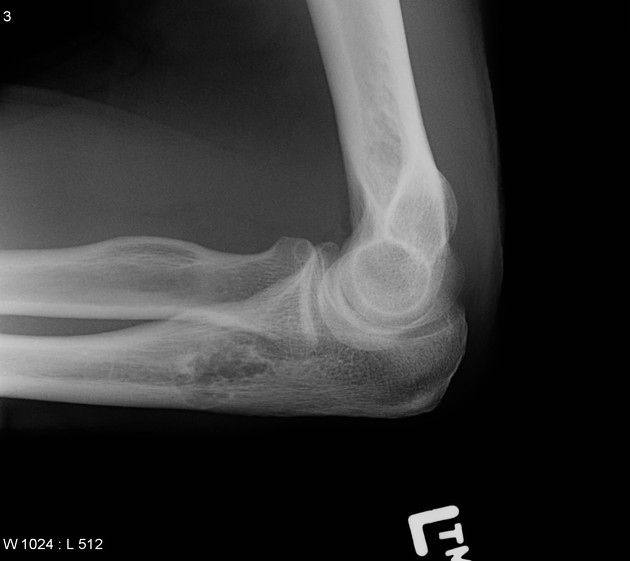
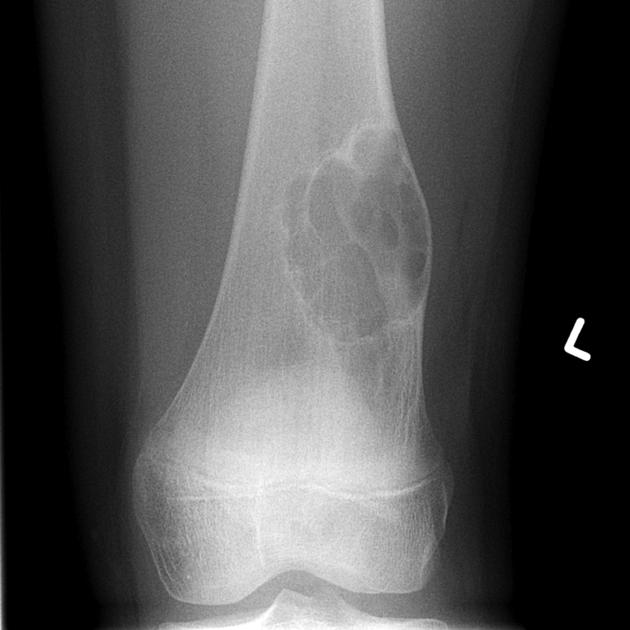
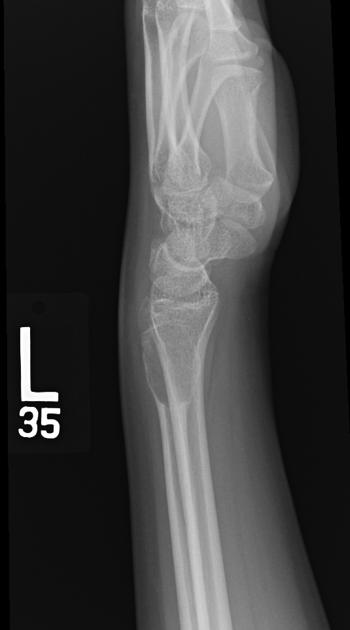
lobulated or oval eccentric lytic lesion
well defined sclerotic margin: ~85%
often expansile, with long axis parallel to long axis of long bone
no periosteal reaction (unless a complicating fracture present)
geographic bone destruction: almost 100%
presence of septations (pseudotrabeculation): ~60% 2
internal matrix calcification - uncommon by imaging (2-15%) 1,23
perilesional sclerosis 24
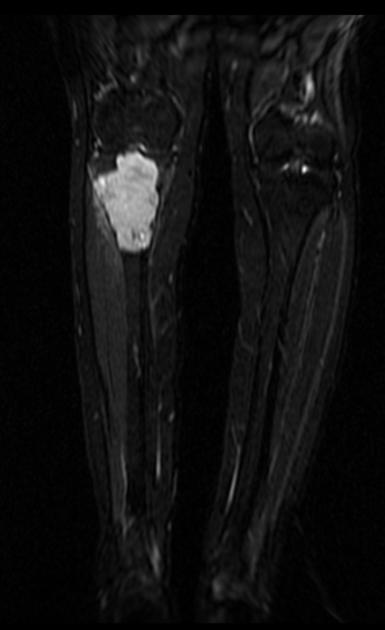
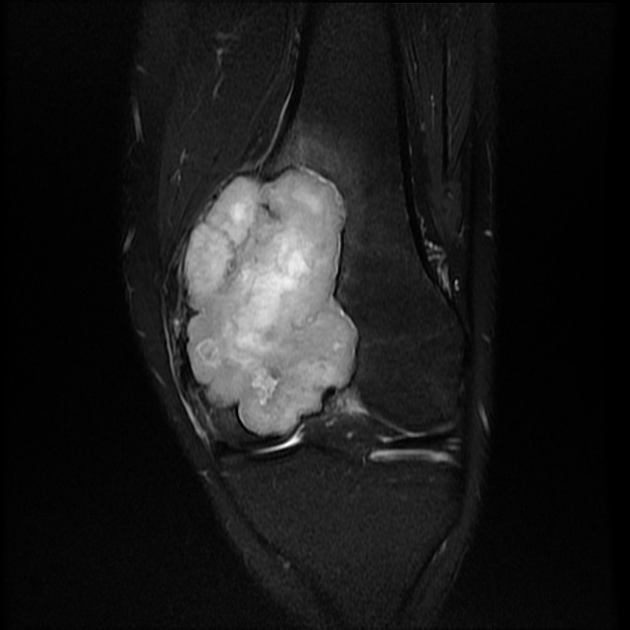
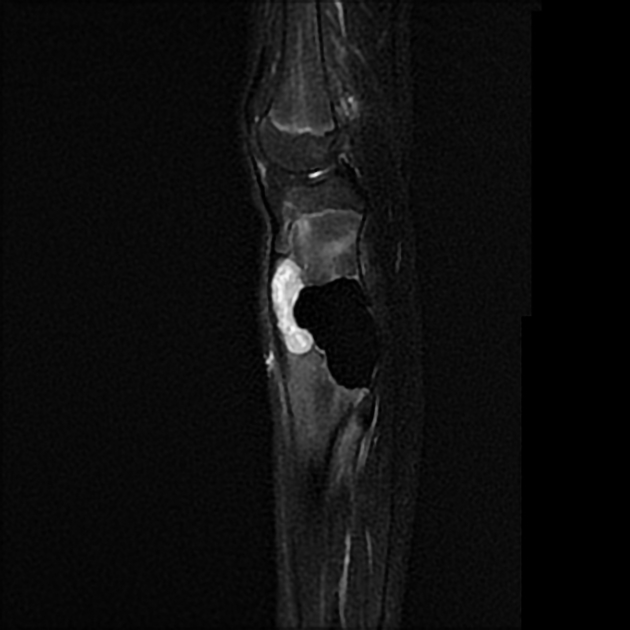
MRI
MR features are often not particularly specific. Signal characteristics include:
T1: low signal
-
T1 C+ (Gd)
majority (~70%) show peripheral nodular enhancement
~30% diffuse contrast enhancement and this can be either homogeneous or heterogeneous 19
T2: intermediate to high signal 24
areas of low signal, both in peripheral rim and centrally, may correspond to perilesional sclerosis and minimal internal mineralization, respectively
Nuclear medicine
On bone scans, the scintigraphic "doughnut sign" has been described in this tumor type 11. However, this is non-specific and can be seen in many other bone lesions.
Treatment and prognosis
They are benign lesions and malignant degeneration is rare. There is a high rate of reported recurrence (up to 80%) with curettage alone, with a lower rate (~20%) with bone grafting. As such if an en-bloc resection is possible this is advisable 14.
History and etymology
It is thought to have been initially described by H L Jaffe and L Lichtenstein in 1948 7.
Differential diagnosis
General imaging differential considerations include:
giant cell tumor of bone (GCT): well-defined, non-sclerotic margin in most cases
non-ossifying fibroma: younger age group
chondroblastoma: younger age group




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.