Hemorrhagic cholecystitis refers to an inflammatory process of the gallbladder, complicated by hemorrhage into the lumen.
On this page:
Epidemiology
Risk factors
bleeding diatheses
anticoagulants
trauma
Clinical presentation
The presenting features may mimic non-hemorrhagic acute cholecystitis, with right upper quadrant pain being a dominant feature. If the blood is passed through the biliary tree into the gut, hematemesis or passage of melena may also occur, or blood oozing from the ampulla of Vater, known as hemobilia, may be seen at endoscopy 1. Blockage of the bile ducts by blood clots may cause biliary obstruction, with secondary painful jaundice and pain mimicking the passage of gallstones. There may be a reduction in the red blood cell count.
Pathology
When a complication of acute cholecystitis, the inflammatory process causes mucosal necrosis with subsequent bleeding from small vessels in the wall. Cystic artery pseudoaneurysms may also be caused by acute cholecystitis, with rupture leading to hemobilia. However, in many reported cases of hemorrhagic cholecystitis, there is no clear underlying cause.
Radiographic features
Ultrasound is the preferred diagnostic modality in the initial investigation of right upper quadrant pain. If the presentation is with gut bleeding, a CT may be performed following endoscopy to seek a source of bleeding.
Ultrasound
The gallbladder is distended with mixed echogenicity non-shadowing material filling the lumen. There may be layering or a swirling appearance depending on how recent the onset was. Signs of acute cholecystitis, namely wall thickening and free pericholecystic fluid may also be present. Stones may be obscured by the luminal blood.
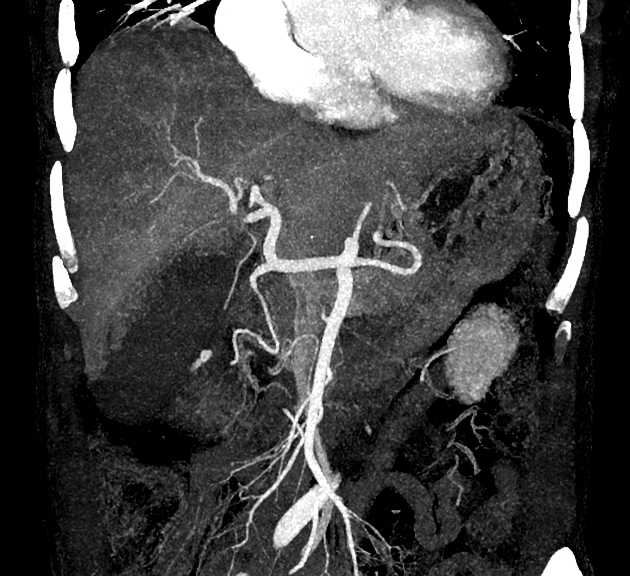
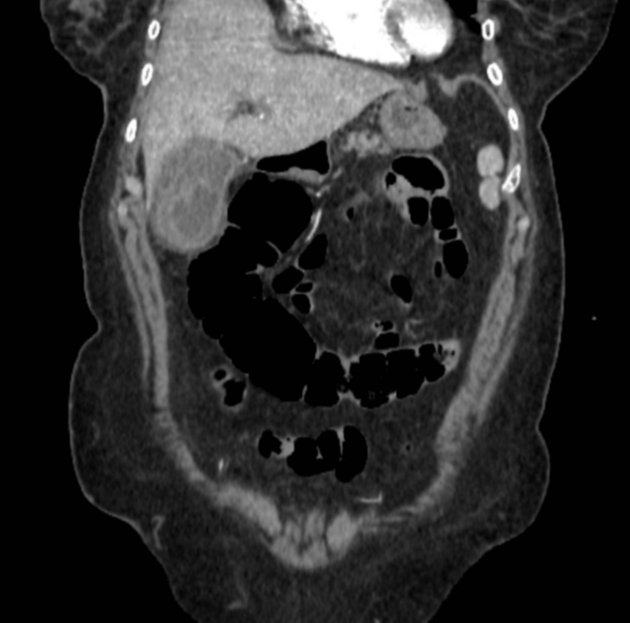
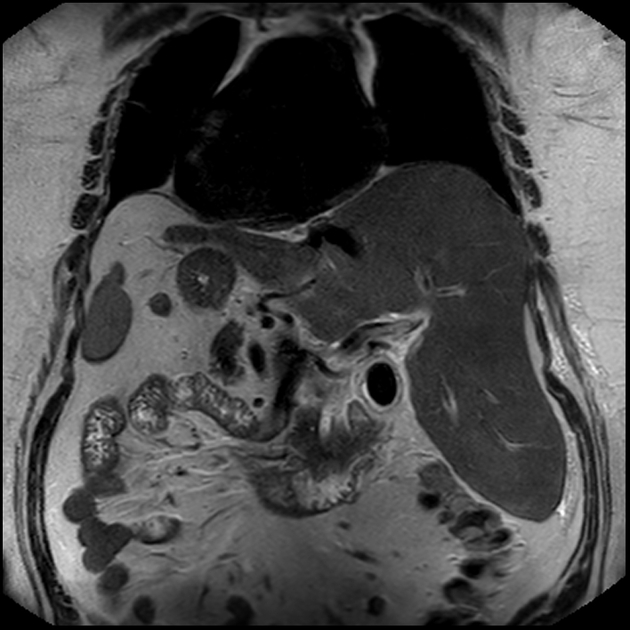
CT
In addition to signs of acute cholecystitis such as wall thickening and free pericholecystic fluid, high-density material is seen within the lumen. Layering or swirling may be seen, depending on the time lapsed between the onset and imaging 3. There may be free fluid elsewhere in the abdomen and pelvis, either simple free fluid or of high density, indicating a possible perforation of the gallbladder.
Treatment and prognosis
In the event of ongoing bleeding, emergent treatment by surgery or embolization of a cystic artery pseudoaneurysm should be considered. A more conservative approach may also be followed with an elective cholecystectomy as an option following recovery from the acute episode.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.