Cystic hepatic metastases are included in the differential for new cystic liver lesions. The internal cystic component may represent necrosis as the tumor outgrows its hepatic blood supply, or it may represent a mucinous component, similar to the primary tumor.
The liver and lungs are the most common sites of metastatic disease, and cystic hepatic metastases may arise from any number of primary tumors, but classically hepatic metastases arise from organs that have the opportunity of seeding the liver with metastases via the portal vein, including the gastrointestinal tract (stomach, small bowel, colon) and the pancreas.
On this page:
Radiographic features
The appearance of the metastases will vary depending on the primary. Multiplicity is a classic feature of hepatic metastases.
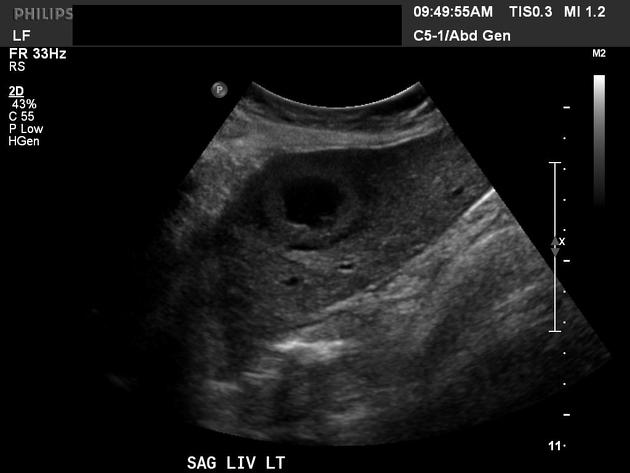
Ultrasound
Target lesions and hyperechoic lesions are more common appearances for hepatic metastases than cystic lesions:
- centrally hypoechoic
- may have thick septations
- may show a hypoechoic halo, corresponding with proliferating metastatic cells or compressed hepatic parenchyma
- may demonstrate increased vascularity on color Doppler imaging
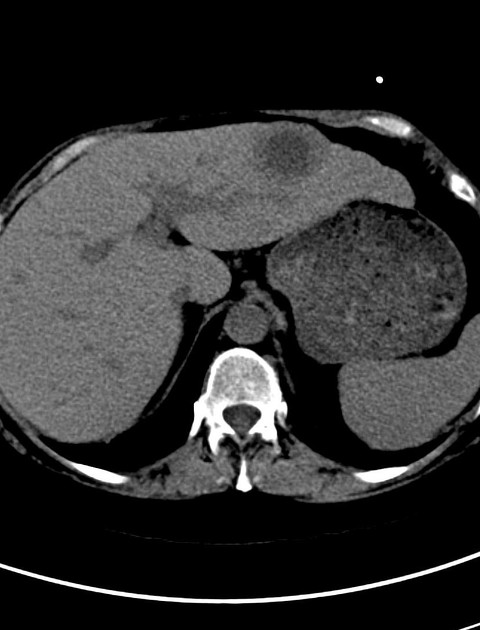
CT
- lesion is centrally hypoattenuating relative to liver, unless complicated by internal hemorrhage
- irregularly thickened and enhancing wall
MRI
- irregularly thickened wall
-
T2:
- mild-moderate T2 hyperintensity
- metastases from mucinous tumors may approach the T2 signal intensity of hemangioma (although the enhancement is different)
-
T1 + C (extracellular):
- early rim enhancement with washout is characteristic, reflecting peripheral angiogenesis
- cystic metastases may be predominantly hypovascular
- T1 + C (Eovist): no retention of contrast on the delayed sequence
Differential diagnosis
Cystic hepatic metastases are part of the differential of cystic liver lesions. There is an overlap in imaging appearance with hepatic abscess. Classically, hepatic metastases are favored if there are multiple lesions (~98% of cases).
A cystic hepatic metastasis may arise from any source, but consideration of primary lesions should include:
- colon cancer
- ovarian cystadenocarcinoma
- squamous cell lung cancer
- sarcomas
- melanoma
- gastrointestinal stromal tumor (GIST)
- pancreatic mucinous cystadenocarcinoma
- pancreatic neuroendocrine tumor: a metastasis with a fluid-fluid level on MRI is characteristic of a neuroendocrine tumor metastasis 4
- a large metastasis from any origin that has outgrown its blood supply
Cystic hepatic metastases are usually easily differentiated from hepatic cysts, since cystic metastases are usually much less well-marginated.
Practical points
If considering placing a percutaneous drain into an equivocal hepatic abscess, biopsy is mandatory since placing a drain in a cystic hepatic metastasis is contraindicated.



 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.