Primary biliary cholangitis (PBC) is a chronic progressive cholestatic liver disease that is the cause of 1-2% of deaths from cirrhosis and constitutes the third most common indication for liver transplantation in adults.
On this page:
Terminology
The name of this disease was changed from primary biliary cirrhosis to primary biliary cholangitis in 2014; however, it was also decided to keep the abbreviation as PBC 11.
Epidemiology
The typical patient is a middle-aged woman presenting with symptoms of fatigue and pruritus and laboratory test evidence of cholestasis.
Associations
other autoimmune diseases: e.g. Sjögren syndrome (~75%), autoimmune thyroiditis (~25%), scleroderma (~10%) 5,12
cholelithiasis: ~40% 8
-
interstitial lung disease: ~15% 6
-
hepatocellular carcinoma: develops in ~5% 7
additional risk in older patients, males, history of diabetes mellitus or past hepatitis B virus infection 7
Kayser-Fleischer rings: may be seen (without Wilson disease) 13
ulcerative colitis: rare 15,16
Clinical presentation
Clinical features include 12:
pruritus (often the first symptom)
skin hyperpigmentation, especially of arms and trunk
-
xanthomas and xanthelasma due to hypercholesterolemia
interestingly hypercholesterolemia does not confer an increased risk of death from atherosclerosis
fatigue
right upper quadrant abdominal discomfort
Pathology
Primary biliary cholangitis is characterized by the destruction of small intrahepatic bile ducts, portal inflammation, and progressive scarring. The cause of primary biliary cholangitis is unknown, but it is probably due to an inherited abnormality of immunoregulation.
Markers
serum anti-mitochondrial antibody (AMA) tests are highly sensitive and specific for primary biliary cholangitis (85-100%10)
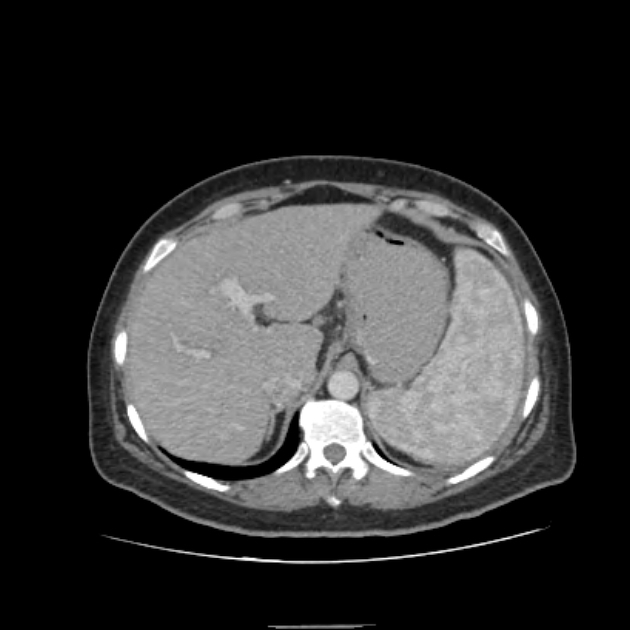
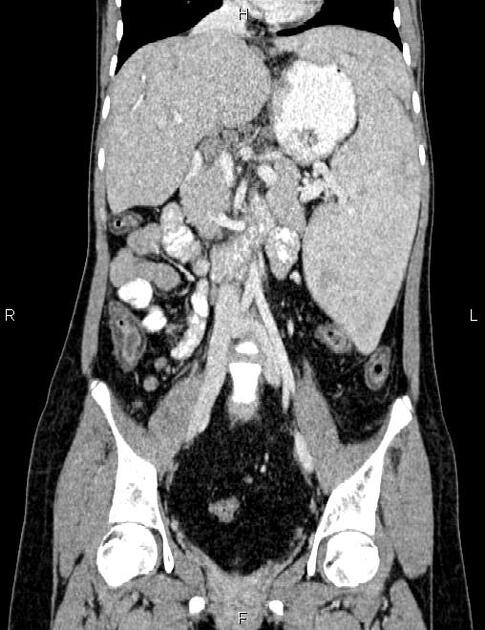
Radiographic features
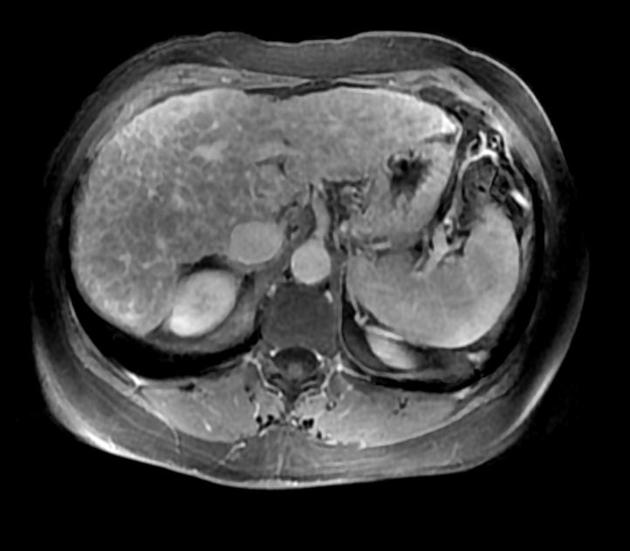
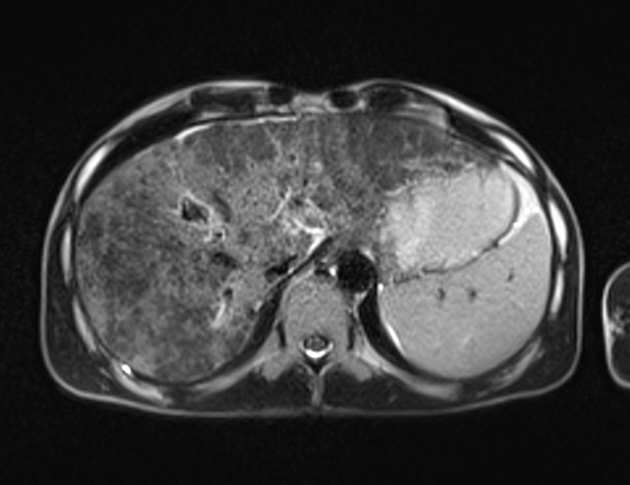
MRI
T2: if parenchymal lace-like fibrosis and periportal halo sign are seen together the sensitivity for primary biliary cholangitis can approach 70% 2
Other features detectable on MRI include:
periportal hyperintensity (cuffing)
segmental hypertrophy, notably of the caudate lobe
hepatic surface irregularity due to regenerative nodules
regional lymphadenopathy: tends to dominate in the gastrohepatic ligament and porta hepatis 4
Treatment and prognosis
Ursodeoxycholic acid is the mainstay for medical management 12. In cases of primary biliary cholangitis that advance despite pharmacotherapy, liver transplantation clearly improves the survival and quality of life.
Primary biliary cholangitis can recur after transplantation but with a frequency much lower than that for hepatitis and other diseases.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.