Tracheal stenosis
Citation, DOI, disclosures and article data
At the time the article was created The Radswiki had no recorded disclosures.
View The Radswiki's current disclosuresAt the time the article was last revised Tariq Walizai had no financial relationships to ineligible companies to disclose.
View Tariq Walizai's current disclosures- Stenosis of the trachea
- Stenosis of trachea
Tracheal stenosis is usually acquired following intubation or tracheostomy. It can also arise as part of the spectrum of tracheobronchial stenosis.
Pathology
Inflammation and pressure necrosis of the tracheal mucosa most commonly occur at either the tracheostomy stoma or at the level of the tube balloon. Acute post-intubation stenosis results from mucosal edema or granulation tissue.
Post-intubation stenosis can extend for several centimeters and typically involves trachea above the level of the thoracic inlet.
Post-tracheostomy stenosis typically begins 1 to 1.5 cm distal to the inferior margin of the tracheostomy stoma and involves 1.5 to 2.5 cm of tracheal wall.
In patients with chronic stricture, tracheomalacia may result from weakness of tracheal cartilage and can be a cause of dyspnea.
Radiographic features
Plain radiograph
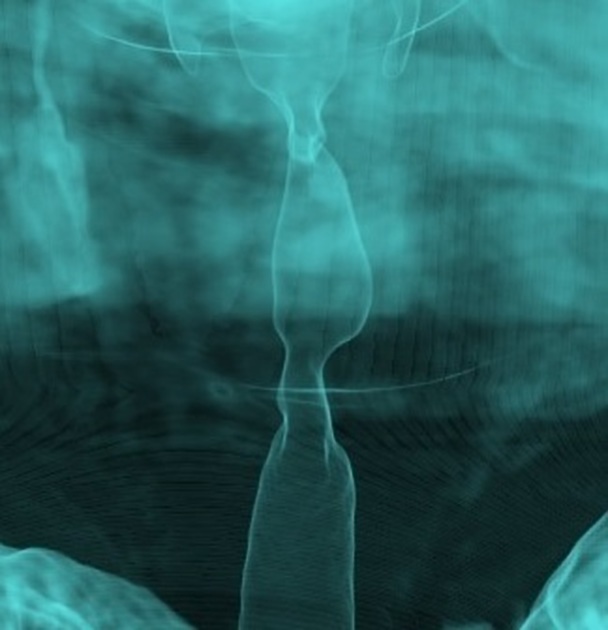
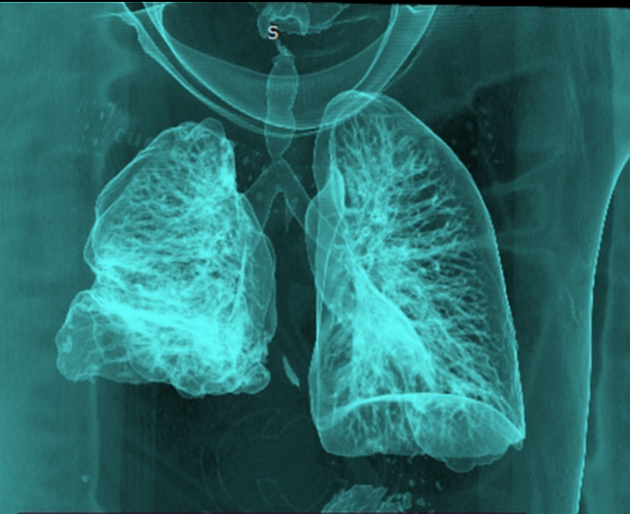
Narrowing of tracheal air shadow.
CT
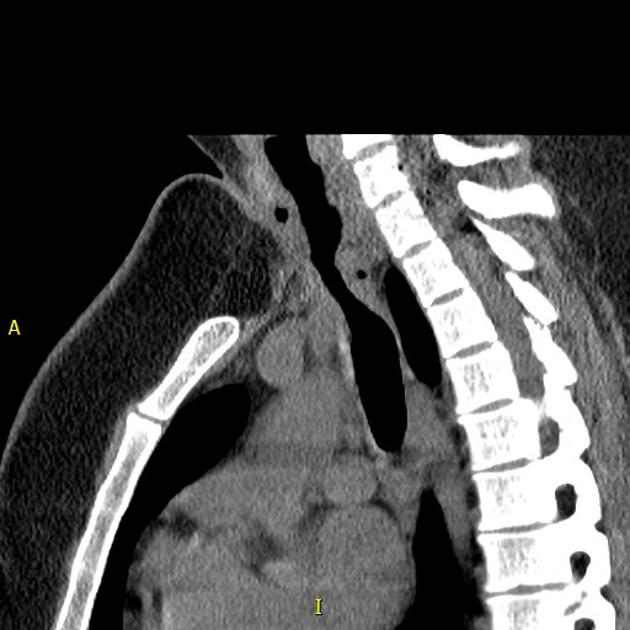
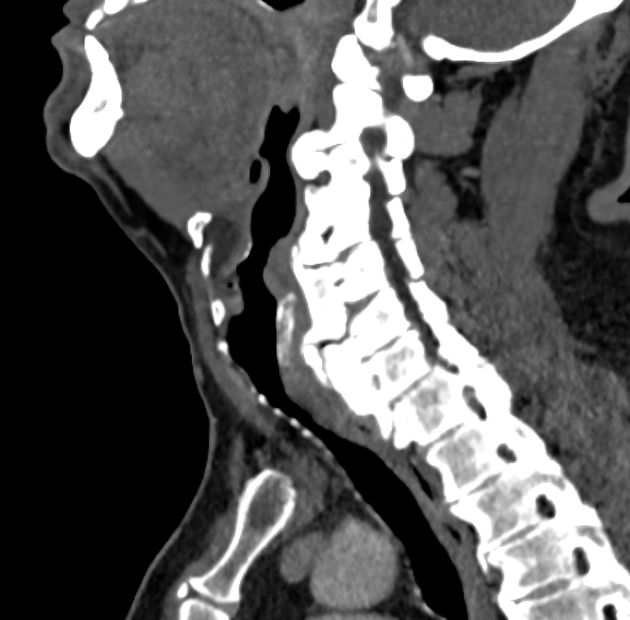
Eccentric or concentric soft tissue thickening internal to normal-appearing tracheal cartilage may be visible. The outer tracheal wall has a normal appearance without evidence of deformity or narrowing. Expiratory CT shows little change in tracheal diameter.
References
- 1. Webb EM, Elicker BM, Webb WR. Using CT to diagnose nonneoplastic tracheal abnormalities: appearance of the tracheal wall. AJR Am J Roentgenol. 2000;174 (5): 1315-21. AJR Am J Roentgenol (full text) - Pubmed citation
- 2. Puchalski J, Musani AI. Tracheobronchial stenosis: causes and advances in management. (2013) Clinics in chest medicine. 34 (3): 557-67. doi:10.1016/j.ccm.2013.05.002 - Pubmed
- 3. Hewitt RJ, Butler CR, Maughan EF, Elliott MJ. Congenital tracheobronchial stenosis. (2016) Seminars in pediatric surgery. 25 (3): 144-9. doi:10.1053/j.sempedsurg.2016.02.007 - Pubmed
- 4. Andy Adam, Adrian K. Dixon, Jonathan H. Gillard. Grainger & Allison's Diagnostic Radiology. (2020) ISBN: 9780702075247 - Google Books
Incoming Links
- Obstetric curriculum
- Innominate artery compression syndrome
- Tracheal web
- Diffuse tracheal narrowing
- Relapsing polychondritis
- Tracheobronchial amyloidosis
- Funnel trachea
- Bilateral hypertranslucent hemithoraces
- Rhinoscleroma
- Subglottic stenosis
- Tracheobronchial injury
- Aberrant left pulmonary artery
- Endobronchial tuberculosis
- Tracheobronchopathia osteochondroplastica
- Tracheobronchial stenosis
- Inflammatory bowel disease (thoracic manifestations)
- Trachea
- Bronchial stenosis
- Severe tracheal narrowing due to multinodular goitre following FNA
- Tracheal web
- Incomplete double aortic arch
- Tracheal stenosis
- Malignant tracheal compression treated with tracheobronchial stent
- Diffuse idiopathic skeletal hyperostosis (DISH) with tracheal stenosis
- Tracheal stenosis - post-intubation
- Tracheal stenosis - postintubation
- Innominate artery compression syndrome
- Bronchial atresia and subglottic stenosis
- Tracheal compression between goitre and oesophagus
- Tracheal stenosis with subsequent stenting
Related articles: Chest
- imaging techniques
-
chest radiograph
- radiography
-
approach
- ABCDE
- ABCDEFGHI
- congenital heart disease
- medical devices in the thorax
- common lines and tubes
- nasogastric tubes
- endotracheal tubes
- central venous catheters
- esophageal temperature probe
- tracheostomy tube
- pleural catheters
- cardiac conduction devices
- prosthetic heart valve
- review areas
-
airspace opacification
- differential diagnoses of airspace opacification
- lobar consolidation
-
atelectasis
- mechanism-based
- morphology-based
- lobar lung collapse
- chest x-ray in the exam setting
- cardiomediastinal contour
- chest radiograph zones
- tracheal air column
- fissures
- normal chest x-ray appearance of the diaphragm
- nipple shadow
-
lines and stripes
- anterior junction line
- posterior junction line
- right paratracheal stripe
- left paratracheal stripe
- posterior tracheal stripe/tracheo-esophageal stripe
- posterior wall of bronchus intermedius
- right paraspinal line
- left paraspinal line
- aortic-pulmonary stripe
- aortopulmonary window
- azygo-esophageal recess
- spaces
- signs
- air bronchogram
- big rib sign
- Chang sign
- Chen sign
- coin lesion
- continuous diaphragm sign
- dense hilum sign
- double contour sign
- egg-on-a-string sign
- extrapleural sign
- finger in glove sign
- flat waist sign
- Fleischner sign
- ginkgo leaf sign
- Golden S sign
- Hampton hump
- haystack sign
- hilum convergence sign
- hilum overlay sign
- Hoffman-Rigler sign
- holly leaf sign
- incomplete border sign
- juxtaphrenic peak sign
- Kirklin sign
- medial stripe sign
- melting ice cube sign
- more black sign
- Naclerio V sign
- Palla sign
- pericardial fat tag sign
- Shmoo sign
- silhouette sign
- snowman sign
- spinnaker sign
- steeple sign
- straight left heart border sign
- third mogul sign
- tram-track sign
- walking man sign
- water bottle sign
- wave sign
- Westermark sign
- HRCT
-
chest radiograph
- airways
- bronchitis
- small airways disease
-
bronchiectasis
- broncho-arterial ratio
- related conditions
- differentials by distribution
- narrowing
-
tracheal stenosis
- diffuse tracheal narrowing (differential)
-
bronchial stenosis
- diffuse airway narrowing (differential)
-
tracheal stenosis
- diverticula
- pulmonary edema
-
interstitial lung disease (ILD)
- Anti-Jo-1 antibody-positive interstitial lung disease
- drug-induced interstitial lung disease
-
hypersensitivity pneumonitis
- acute hypersensitivity pneumonitis
- subacute hypersensitivity pneumonitis
- chronic hypersensitivity pneumonitis
- etiology
- bird fancier's lung: pigeon fancier's lung
- farmer's lung
- cheese workers' lung
- bagassosis
- mushroom worker’s lung
- malt worker’s lung
- maple bark disease
- hot tub lung
- wine maker’s lung
- woodsman’s disease
- thatched roof lung
- tobacco grower’s lung
- potato riddler’s lung
- summer-type pneumonitis
- dry rot lung
- machine operator’s lung
- humidifier lung
- shower curtain disease
- furrier’s lung
- miller’s lung
- lycoperdonosis
- saxophone lung
-
idiopathic interstitial pneumonia (mnemonic)
- acute interstitial pneumonia (AIP)
- cryptogenic organizing pneumonia (COP)
- desquamative interstitial pneumonia (DIP)
- non-specific interstitial pneumonia (NSIP)
- idiopathic pleuroparenchymal fibroelastosis
- lymphoid interstitial pneumonia (LIP)
- respiratory bronchiolitis–associated interstitial lung disease (RB-ILD)
- usual interstitial pneumonia / idiopathic pulmonary fibrosis (UIP/IPF)
-
pneumoconioses
- fibrotic
- non-fibrotic
-
lung cancer
-
non-small-cell lung cancer
-
adenocarcinoma
- pre-invasive tumors
- minimally invasive tumors
- invasive tumors
- variants of invasive carcinoma
- described imaging features
- adenosquamous carcinoma
- large cell carcinoma
- primary sarcomatoid carcinoma of the lung
- squamous cell carcinoma
- salivary gland-type tumors
-
adenocarcinoma
- pulmonary neuroendocrine tumors
- preinvasive lesions
-
lung cancer invasion patterns
- tumor spread through air spaces (STAS)
- presence of non-lepidic patterns such as acinar, papillary, solid, or micropapillary
- myofibroblastic stroma associated with invasive tumor cells
- pleural invasion
- vascular invasion
- tumors by location
- benign neoplasms
- pulmonary metastases
- lung cancer screening
- lung cancer staging
-
non-small-cell lung cancer





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.