Adenomyosis (or uterine adenomyosis) is a common uterine condition of ectopic endometrial tissue in the myometrium, sometimes considered a spectrum of endometriosis. Although most commonly asymptomatic, it may present with menorrhagia and dysmenorrhea.
Pelvic imaging (i.e. ultrasound, MRI) may show characteristic findings, commonly including focal or diffuse myometrial bulkiness, which may be asymmetrical, and heterogeneous myometrium.
On this page:
Epidemiology
Classically, adenomyosis most commonly affects multiparous women of reproductive age. However, this is based on the results of studies with pathologic examinations of hysterectomy specimens, therefore biased towards patients who had surgery. Similarly, this may be the reason adenomyosis is seen with higher frequency in women with a history of uterine surgical procedures (e.g. Cesarean section, dilatation and curettage). Patients with high estrogen exposure (e.g. short menstrual cycles, early menarche) have an increased risk of adenomyosis.
The reported incidence ranges widely from 5-70% (mean 20-30%), depending on the histological definition or the imaging modality used 12. Adenomyosis is relatively rare in postmenopausal women but a higher incidence of adenomyosis has been reported in women treated with tamoxifen for breast cancer 12.
Associations
co-existent endometriosis has been reported in 20% of cases 1
leiomyomas: may be present in almost 50% of cases involving adenomyosis of the uterus 14
-
other reported associations include
Clinical presentation
Most patients with adenomyosis are asymptomatic. Symptoms related to adenomyosis include dysmenorrhea, menorrhagia, dyspareunia, chronic pelvic pain, and menometrorrhagia 11. The ectopic endometrial glands within the myometrium do not respond to cyclic ovarian hormones, unlike those of endometriosis. Pelvic tenderness on examination is associated with diffuse enlargement of the uterus.
Pathology
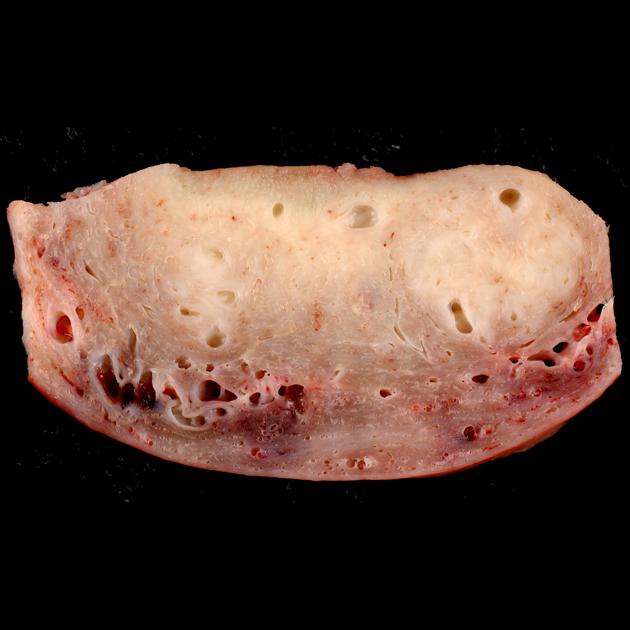
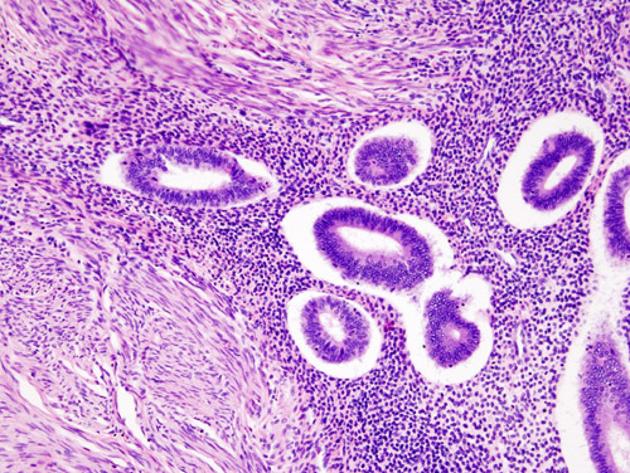
Adenomyosis is histologically-defined as the presence of ectopic endometrial glandular and stromal tissue within the myometrium. The exact cause of adenomyosis is unknown, but it is thought that endometrial glands directly invade the myometrium resulting in spiral vessel angiogenesis, and adjacent smooth muscle hyperplasia and hypertrophy. It has been postulated that this dysfunctional hypertrophied muscular tissue surrounding the ectopic endometrial glands prevents uterine contractions from tamponading bleeding myometrial arterioles; hence, these patients frequently present with dysfunctional uterine bleeding or menorrhagia.
Other hypotheses include invagination of the endometrium through the basalis alongside the intramyometrial lymphatics and embryologically displaced pluripotent mullerian remnants.
Radiographic features
Imaging features are variable and in many instances very subtle.
Three (some say four) forms can be distinguished:
diffuse adenomyosis: most common
focal adenomyosis and adenomyoma: sometimes considered distinct (see below)
cystic adenomyosis and adenomyotic cyst: rare
Adenomyosis is usually relatively generalized, affecting large portions of the uterus (typically the posterior wall), but sparing the cervix. Despite often marked enlargement of the uterus, the overall contour is usually preserved 5.
In some cases, adenomyosis may be localized, forming a mass. In such cases, the term adenomyoma may be used, although there appears to be some disagreement about whether the terms focal adenomyosis and adenomyoma refer to exactly the same entity (please refer to the article on adenomyoma for further discussion).
A rare variant is cystic adenomyosis which is believed to be the result of repeated focal hemorrhages resulting in cystic spaces filled with altered blood products 5.
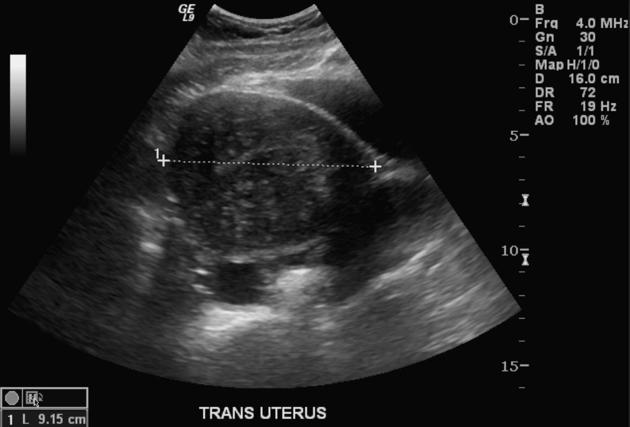
Ultrasound
Although pelvic ultrasound is the primary imaging modality employed to investigate menorrhagia and dysmenorrhea, the sonographic features are variable and the sensitivity is operator and technique dependent. For example, the sensitivity and specificity of transabdominal ultrasound were 32-63% and 95-97%, respectively 7. Yet transvaginal ultrasound is reported to be as sensitive (89%) and specific (89%) as MRI.
In 2021 a consensus on revised definitions of the uterine morphological features of adenomyosis was published 21.
It may be useful to categorize ultrasound findings into three groups that mirror the histological findings 15-17:
-
"adeno": ectopic endometrial glands
subendometrial echogenic linear striations and/or nodules (specific sign), extending from the endometrium and into the inner myometrium
hyperechoic islands 19
irregular endometrial–myometrial junction 19
tiny (1-5 mm) anechoic myometrial and subendometrial cysts (specific sign): reflecting glands filled with fluid
cystic striations
-
"myosis": muscular hyperplasia +/- hypertrophy, which may be hypoechoic
-
focal or diffuse myometrial bulkiness, which may be asymmetric 5
typically of the fundal region and posterior wall
focal lesions have relatively indistinct borders, compared to leiomyomas
asymmetrical myometrial thickening
thickening of the transition zone can sometimes be visualized as a hypoechoic halo surrounding the endometrial layer of ≥12 mm thickness (less specific)
-
-
vascularity: flow on color Doppler
generally increased
increased number of tortuous vessels penetrating the myometrium
areas of increased vascularity reciprocate the distribution of lesions
A "Venetian blind" or "rain shower" appearance (linear striations, parallel shadowing) may be seen as a combination of the aforementioned features: heterogeneous 1,2,20, coarsened echotexture of the myometrium, and acoustic shadowing where endometrial tissues cause a hyperplastic reaction. The combination of this heterogeneity and the subendometrial echogenic nodular and linear striations is not dissimilar to the appearance of chronic liver parenchymal disease - hence, “cirrhosis of the uterus.”
When an adenomyoma is present, appearances may closely mimic those of a uterine fibroid, which may also co-exist.
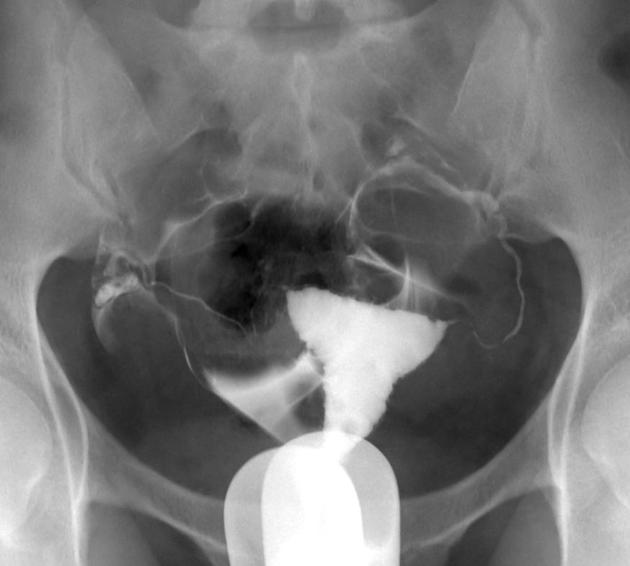
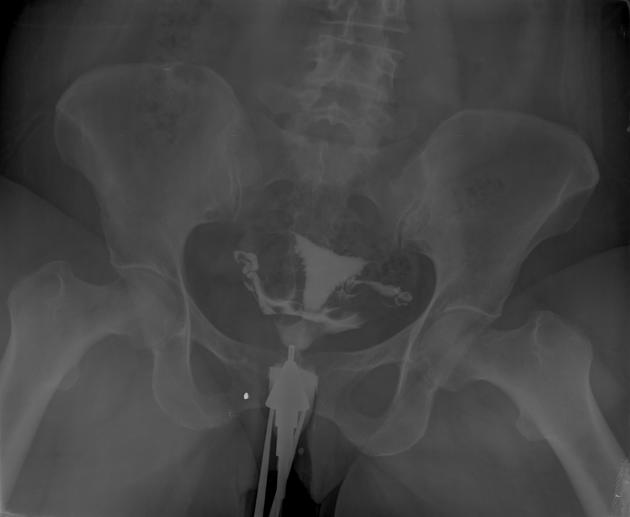
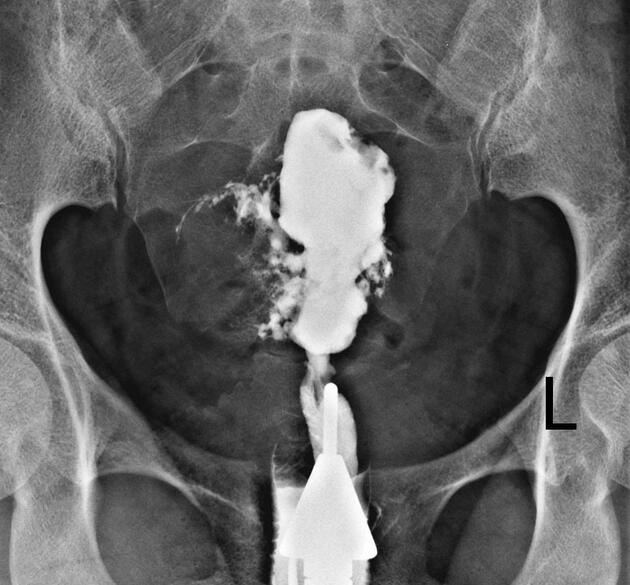
Hysterosalpingogram (HSG)
May show diverticula extending into the myometrium 3.
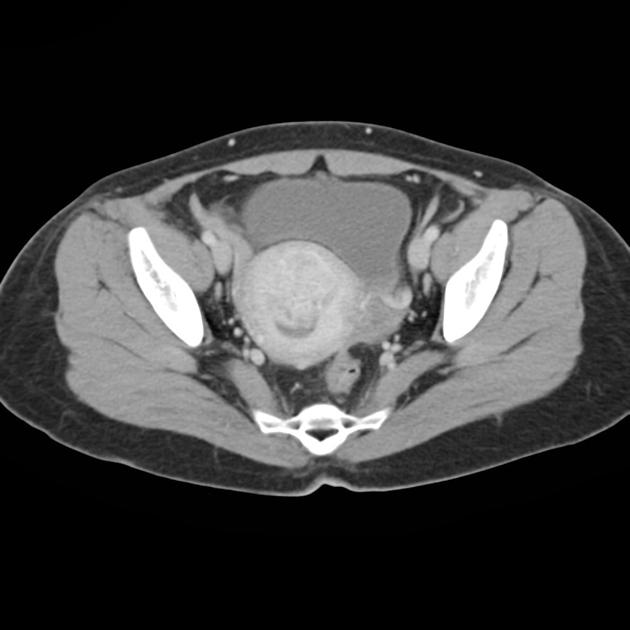
CT
CT is insensitive for adenomyosis but may demonstrate resulting uterine enlargement.
Distinguishing adenomyosis and uterine fibroids on CT is challenging, although the presence of calcifications strongly favors the latter 5.
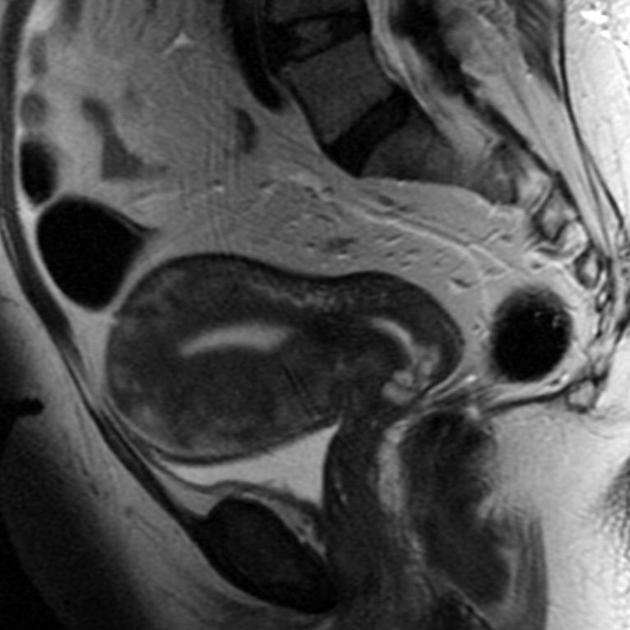
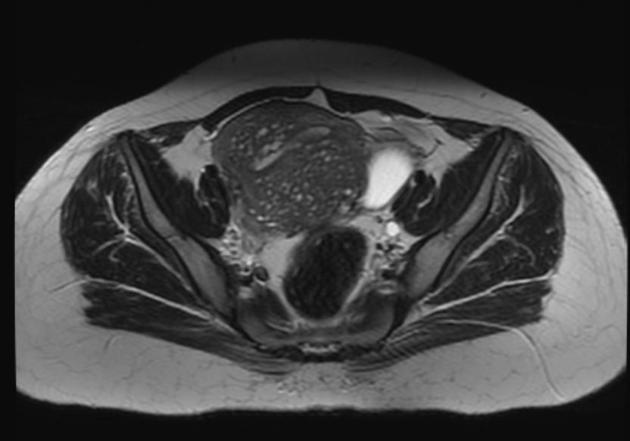
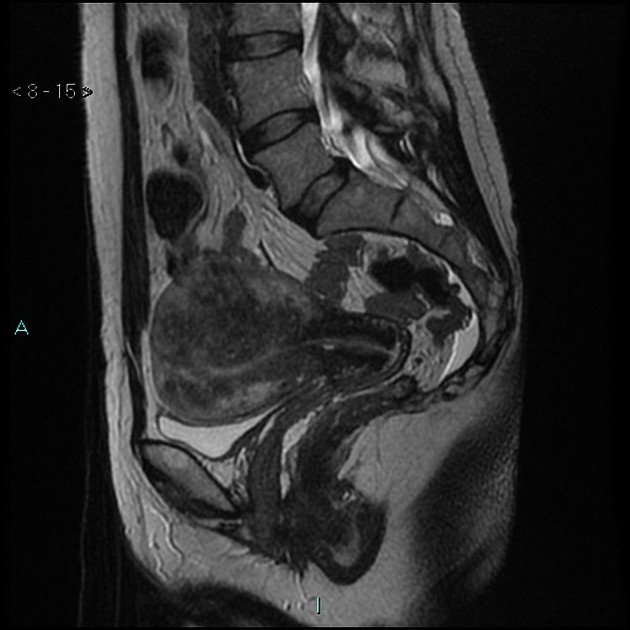
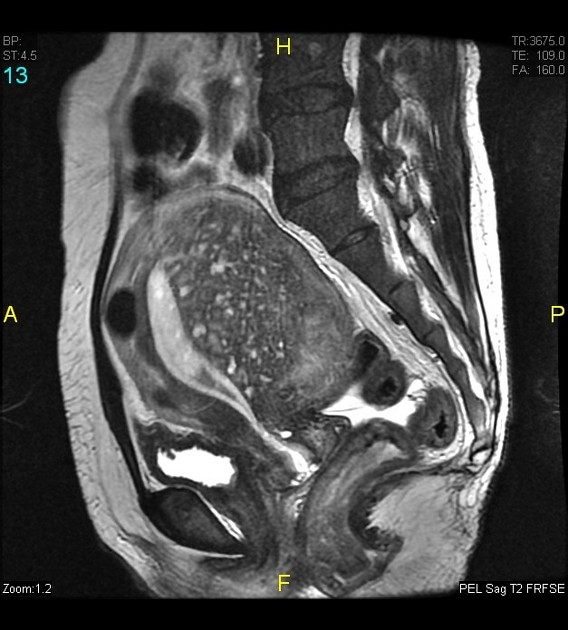
MRI
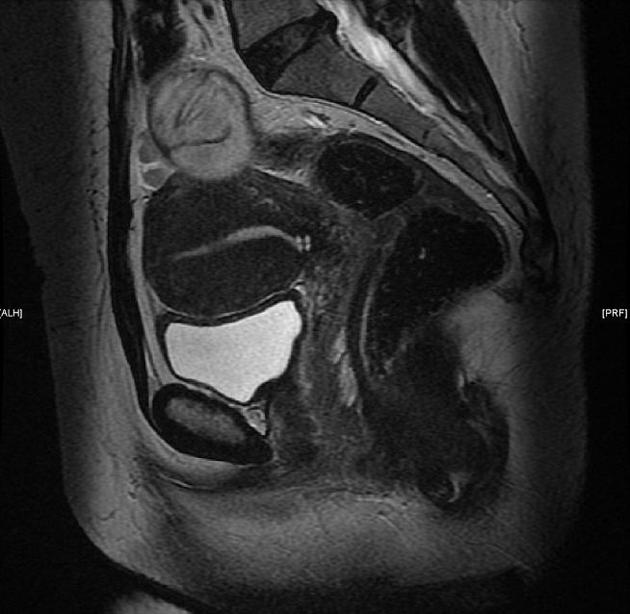
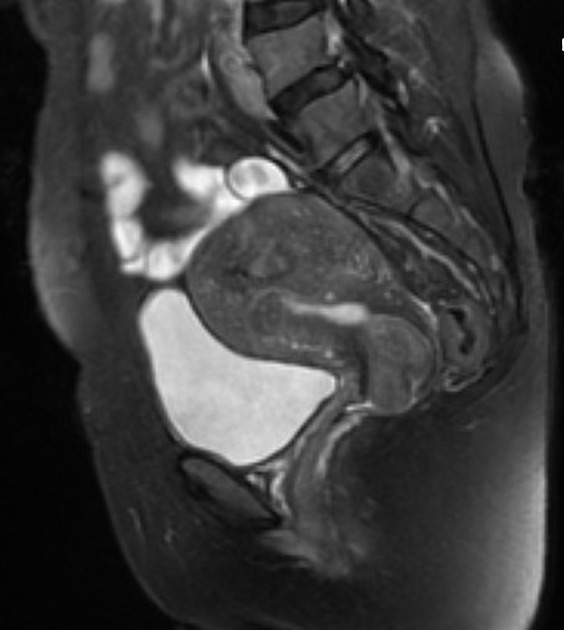
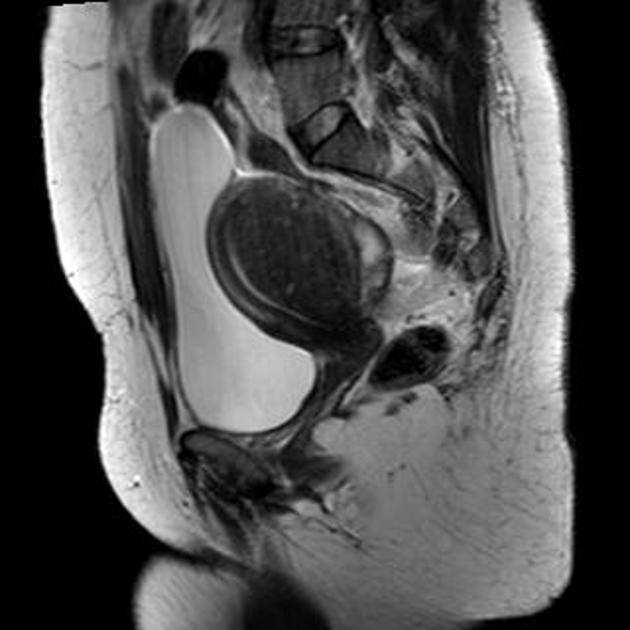
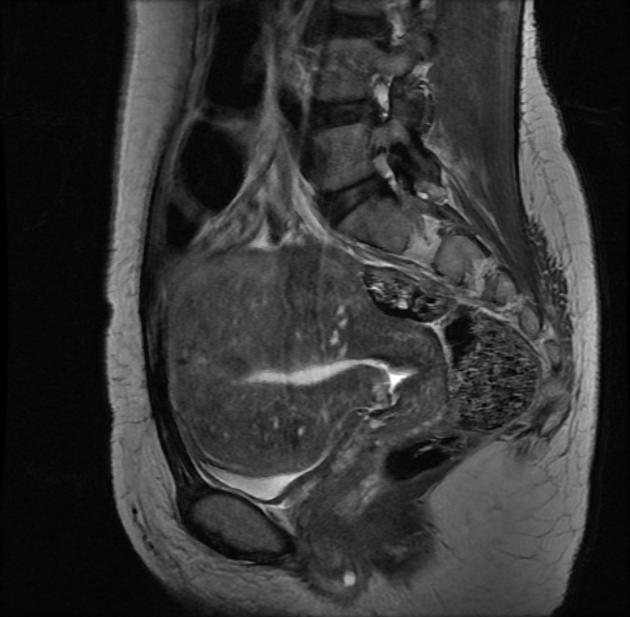
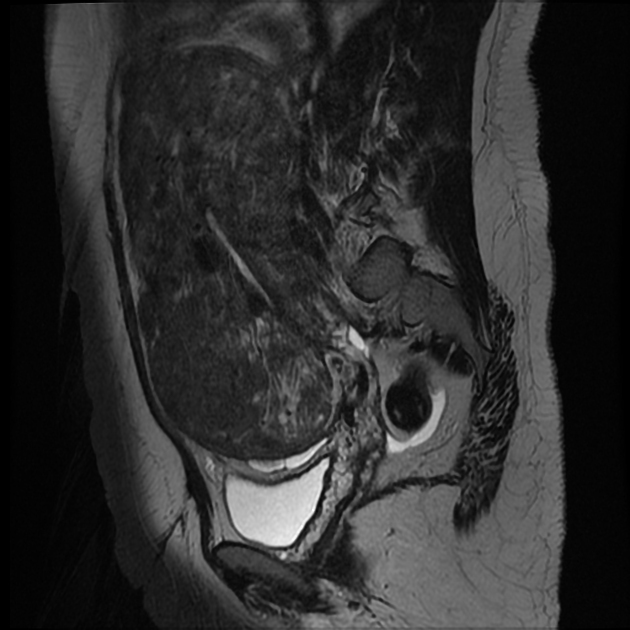
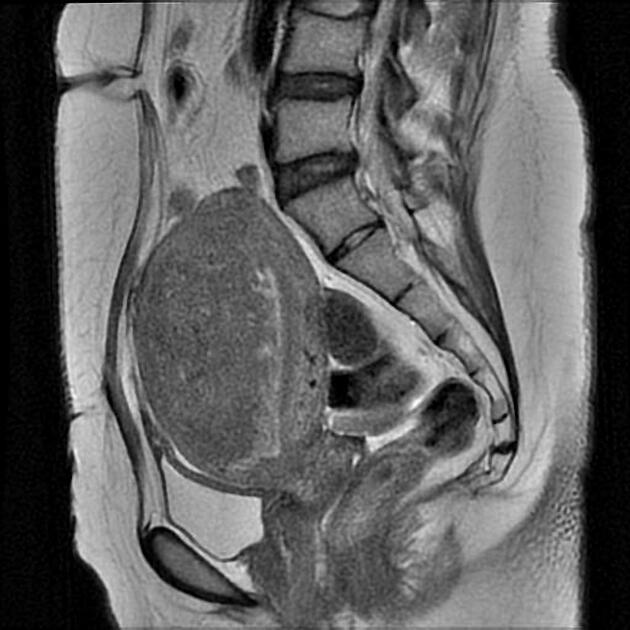
Pelvic MRI is the modality of choice to diagnose and characterize adenomyosis. Small field-of-view T2-weighted images (sagittal and axial) are most useful. MRI has a sensitivity of 78-88% and specificity of 67-93% 7.
The most easily recognized feature is a thickening of the junctional zone ≥12 mm, either diffusely or focally (normal junctional zone thickness is up to ~5 mm) 5.
-
T1
foci of high T1 signal are often seen, indicating menstrual hemorrhage into the ectopic endometrial tissues 7
-
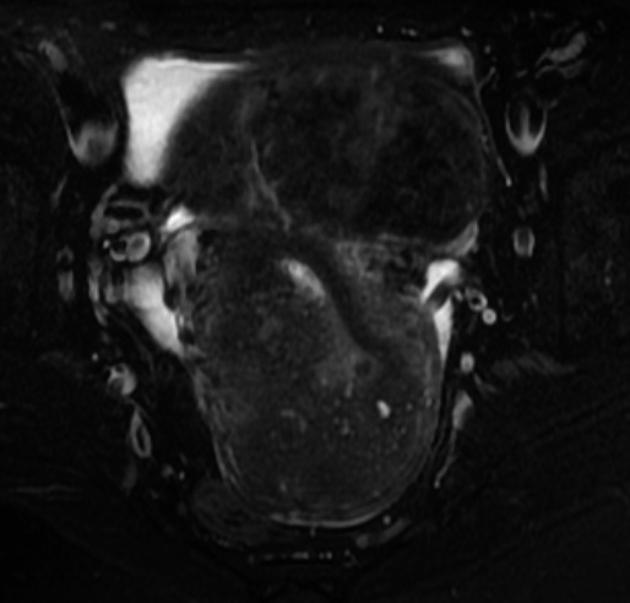
T2
typically a region of adenomyosis appears as an ill-defined ovoid/diffuse region of thickening, often with small high T2 signal regions representing small areas of cystic change
the region may also have a striated appearance 5
-
T1 C+ (Gd)
contrast-enhanced MRI evaluation is usually not required for evaluation of adenomyosis, however, if performed, shows enhancement of the ectopic endometrial glands
Treatment and prognosis
Treatment depends on the severity of symptoms and the need to preserve fertility. In some instances, suppression of normal cyclical hormone-induced proliferation of endometrial tissue (e.g. GnRH agonist) is sufficient.
In women with severe symptoms not relieved medically, and in whom fertility is no longer desirable, a hysterectomy may be performed.
History and etymology
It was first described by Rokitansky in 1860 as “cystosarcoma adenoides uterinum”, and later defined by Von Recklinghausen in 1896 11. The modern definition of adenomyosis was thought to have been provided in 1972 by Bird et al 13.
Differential diagnosis
The differential depends on the macroscopic distribution of endometrial tissue.
For diffuse disease consider:
normal uterus
myometrial contraction: transient finding
-
malignancy
For focal disease (adenomyoma) consider:
-
uterine fibroid (leiomyoma)
better defined than adenomyoma
may have pseudocapsule of compressed adjacent myometrial tissue 5
on color Doppler: tend to displace vessels, demonstrating circumferential peripheral flow
-
uterine contractions
transient in nature
-
vascular malformations
does not disrupt the endometrial-myometrial interface
on color Doppler: demonstrates turbulent high-velocity flow
-
malignancy
Whether focal or diffuse, another potential differential is treatment of breast cancer with tamoxifen which can lead to poorly-defined endometrial hyperplasia and endometrial polyps that can mimic adenomyosis 4 (see: tamoxifen-associated endometrial changes).









 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.