Pelvic congestion syndrome, also known as pelvic venous insufficiency 9, is a condition that results from retrograde flow through incompetent valves in ovarian veins, resulting in pelvic varices and pelvic pain. It is a commonly missed and potentially treatable cause of chronic abdominopelvic pain.
On this page:
Terminology
The term pelvic varices is also used in the setting of dilated pelvic veins on imaging with or without the presence of pelvic pain ref.
Epidemiology
Pelvic congestion syndrome tends to be more common in multiparous, premenopausal women who typically present with chronic pelvic pain for more than 6 months 1. The overall population prevalence is up to ~35% (range 3-39%) in patients where the presenting complaint is chronic pelvic pain 12,15.
Clinical presentation
Patients have chronic (>6 months) non-cyclical symptoms, including pelvic pain, perineal "heaviness", urinary urgency, and post-coital pain 15. In certain cases, there may be thigh, leg, buttock or vulvar varices 15. It is often considered a diagnosis of exclusion.
Pathology
Pelvic congestion syndrome is considered the female homologue to testicular varicocele. It may be caused by:
venous obstruction: such as retroaortic left renal vein
compression of the left renal vein by SMA also known as the nutcracker phenomenon
incompetent valves in ovarian vein
Associations
multifollicular or polycystic ovarian morphology 5
Radiographic features
Non-invasive imaging is primarily used for excluding other pelvic pathology with catheter venography considered the modality of choice for the diagnosis of pelvic congestion syndrome 15. The reported sensitivity of ultrasound is variable between 20% and 100% 15,16, and MRI between 60% and 100% 15,16.
Ultrasound
criteria for the diagnosis of pelvic varices include a venous diameter ≥4 mm and a venous flow velocity ≤3 cm/s as well as a connection with arcuate vessels in the myometrium 14
vein >5 mm traversing the uterine body (sensitivity ~90%) 16
may show multiple dilated veins in the adnexa with reversed venous flow on color Doppler 16, especially after Valsalva maneuver
the venous calibers may increase in real-time during Valsalva
prominent myometrial veins may also be present 1-8
can associated with polycystic ovaries, larger uterus and thickened endometrial lining 9
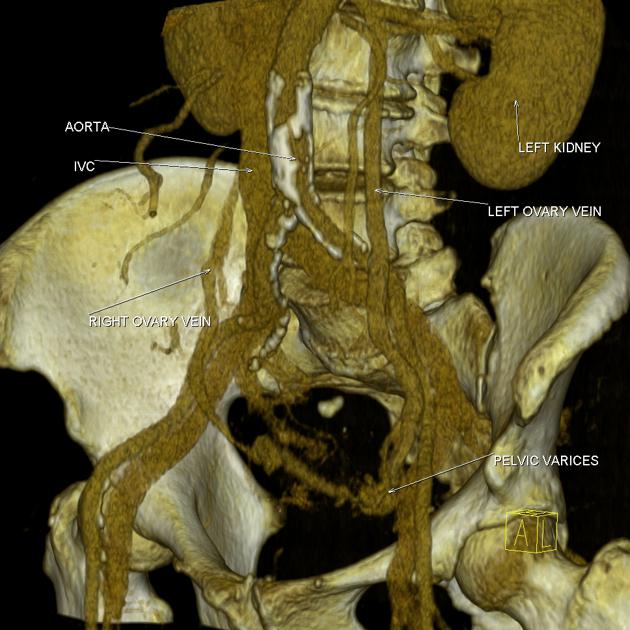
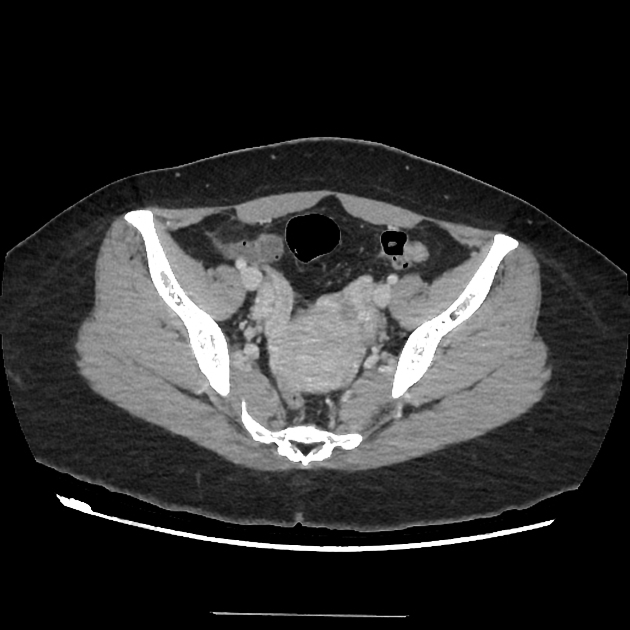
CT
Contrast-enhanced CT typically shows dilated pelvic and ovarian veins. The supine position during scanning may underestimate the size of venous dilatation.
MRI
MR venography
May show dilated veins. Time of flight (TOF) imaging can be performed where contrast is not required.
Signal characteristics
T1: seen as flow voids which represent engorged arcuate vessels
T2: mostly high signal but can vary depending on velocities from low signal to iso signal
GE: high signal
Angiography (DSA)
Catheter pelvic venography is the modality of choice for the diagnosis of pelvic congestion syndrome 15.
Treatment and prognosis
Treatment options include coil embolization of the gonadal vein: ovarian vein embolization. Surgical (e.g. laparoscopic) ligation of the ovarian vein may also be an option in selected cases. The presence of multiple collaterals between iliac and ovarian venous plexuses may cause a recurrence of symptoms.
History and etymology
Pelvic congestion syndrome was first described in 1857 by Louis Alfred Richet (1816-1891), a French anatomist and surgeon 11.















 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.