Small cell lung cancer (SCLC), also known as oat cell lung cancer, is a subtype separated from non-small-cell lung cancer (NSCLC) as it has a unique presentation, imaging appearances, treatment, and prognosis. Small cell lung cancers are neuroendocrine tumors of the lung that rapidly grow, are highly malignant, widely metastasize, and, despite showing an initial response to chemotherapy and radiotherapy, have a poor prognosis and are usually unresectable.
On this page:
Epidemiology
Small cell lung cancers represent 15-20% of lung cancers 1 and are strongly associated with cigarette smoking.
Clinical presentation
Clinical presentation can significantly vary and patients can present in the following ways ref:
constitutional, e.g. fever, weight loss, malaise
primary tumor, e.g. cough, hemoptysis, dyspnea
local invasion, e.g. dysphagia (esophageal compression), hoarseness (recurrent laryngeal nerve palsy), stridor (airway compression), SVC obstruction, rib erosion
metastatic spread (affecting ~70% of patients at presentation), e.g. bone pain (bone metastases), focal neurological deficit (CNS involvement), right upper quadrant pain (liver metastases)
Pathology
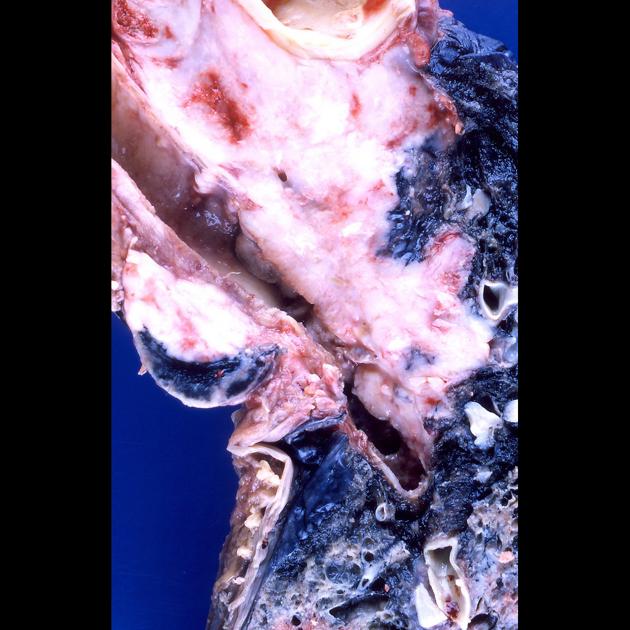
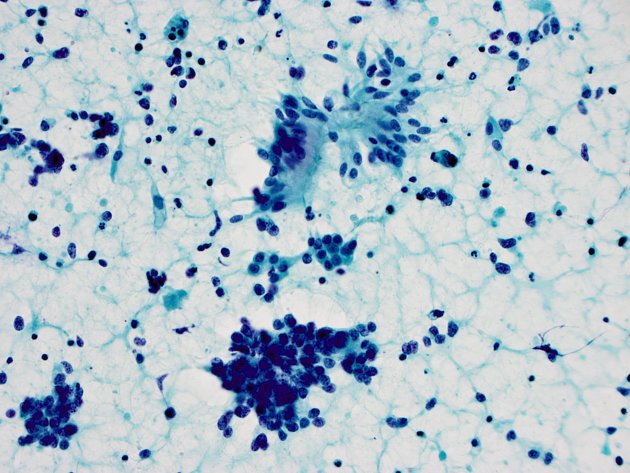
Small cell lung cancer is considered a neuroendocrine tumor of the lung. It arises from the bronchial mucosa. Local invasion occurs in the submucosa with subsequent invasion of peribronchial connective tissue. Cells are small, oval, with scant cytoplasm and a high mitotic count.
It is the most common lung cancer subtype to produce necrosis, superior vena cava (SVC) infiltration/SVC obstruction, and paraneoplastic syndromes (see bronchogenic carcinoma).
Location
Approximately 90-95% of small cell lung cancers occur centrally, usually arising adjacent to a lobar or main bronchus 3.
Serology
lactate dehydrogenase (LDH): not a specific marker but poor overall survival has been suggested in patients with small cell lung cancer having elevated LDH levels 6
Radiographic features
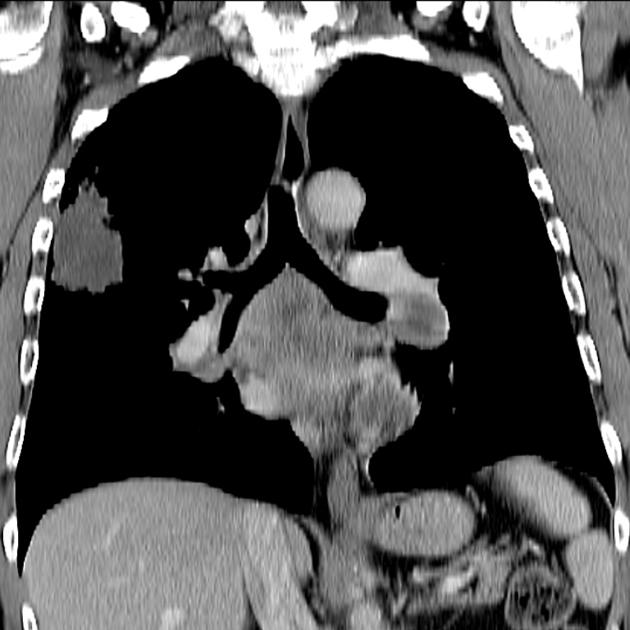
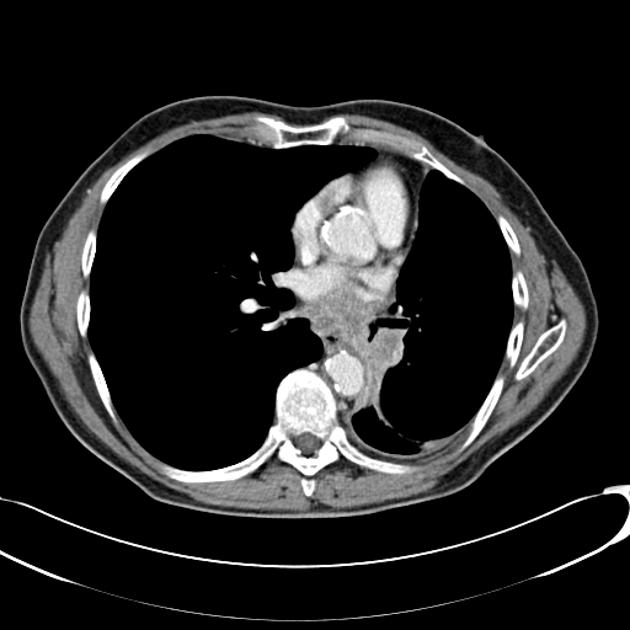
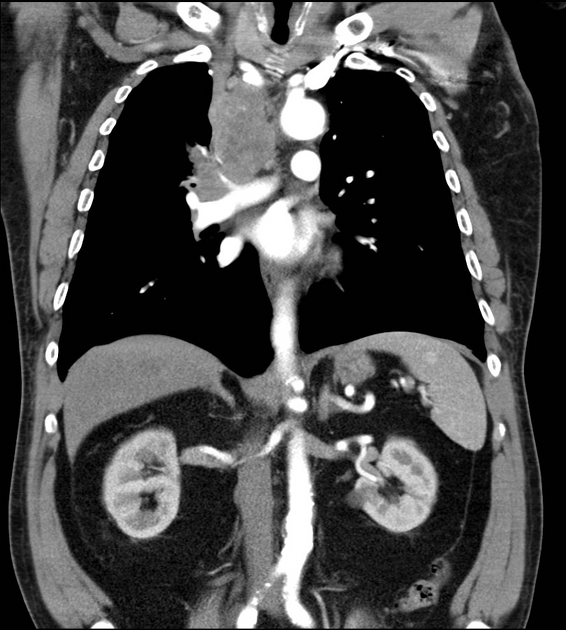
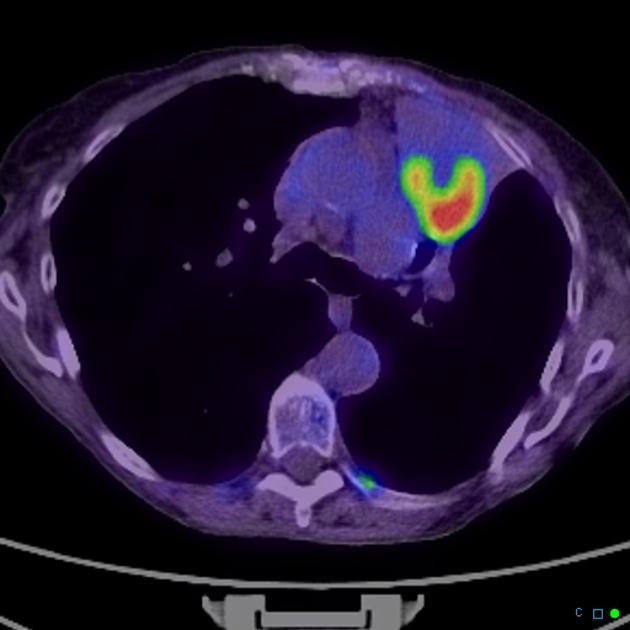
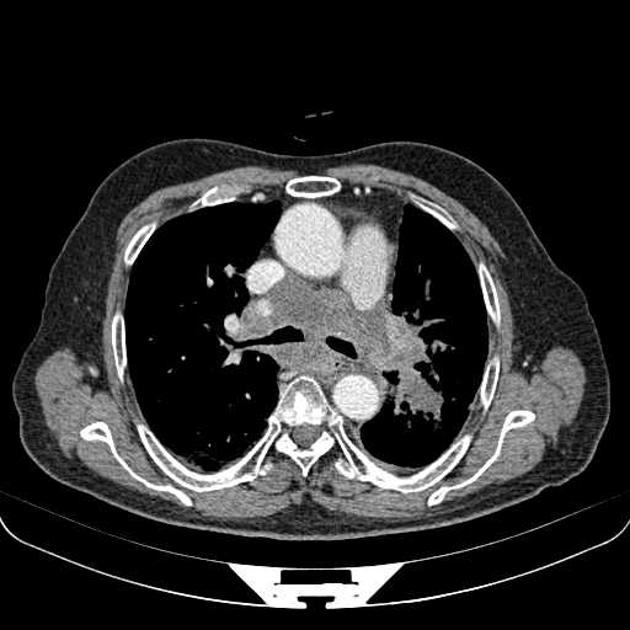
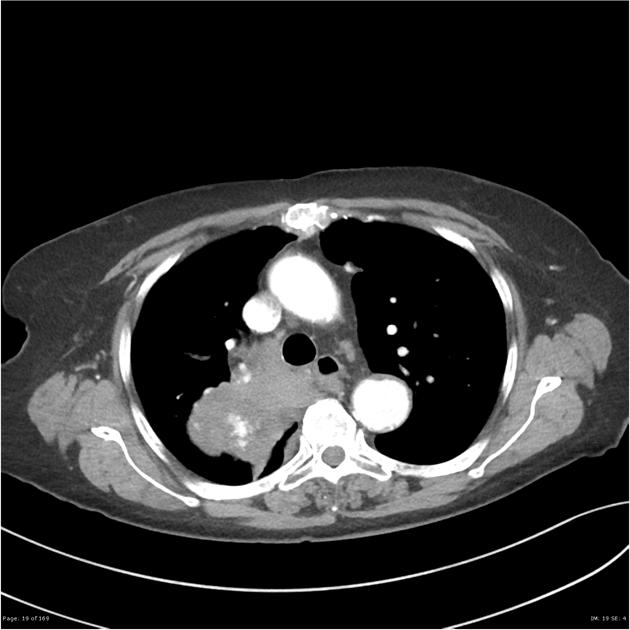
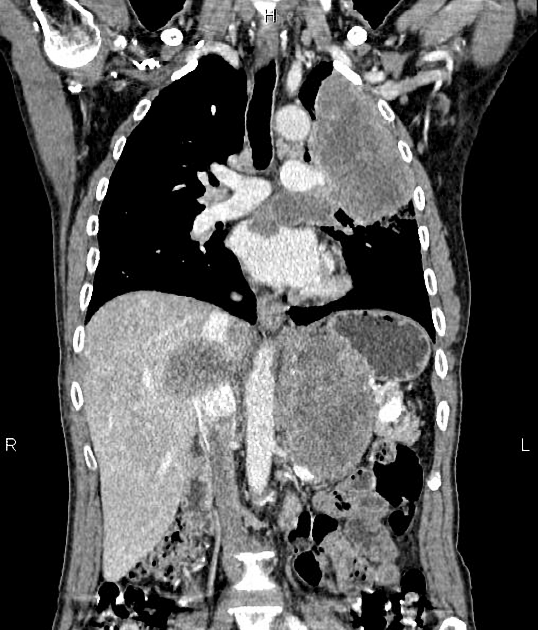
As previously mentioned, small cell tumors are located centrally in the vast majority of cases. They arise from the mainstem or the lobar bronchi and thus appear as hilar or perihilar masses 2, and frequently have mediastinal lymph node involvement at presentation.
Plain radiograph
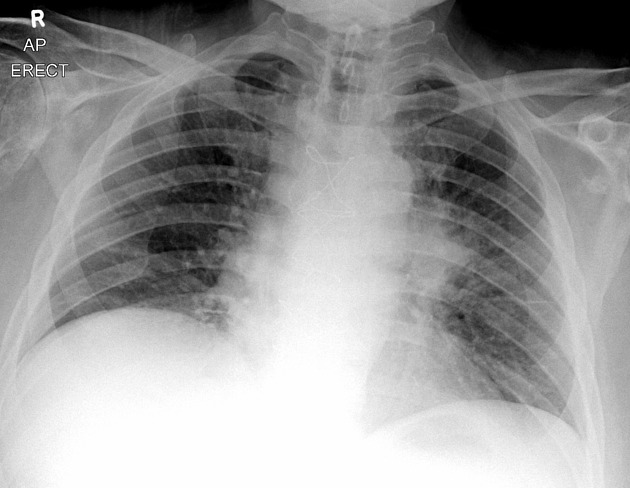
Appearances on chest x-rays are non-specific. They may be seen as a hilar/perihilar mass usually with mediastinal widening due to lymph node enlargement 2. Mediastinal involvement is often the most striking feature and the primary mass may be inapparent.
CT
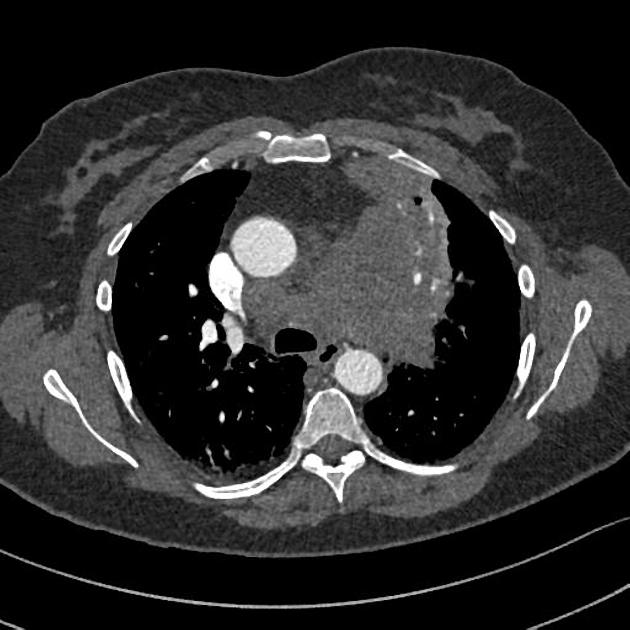
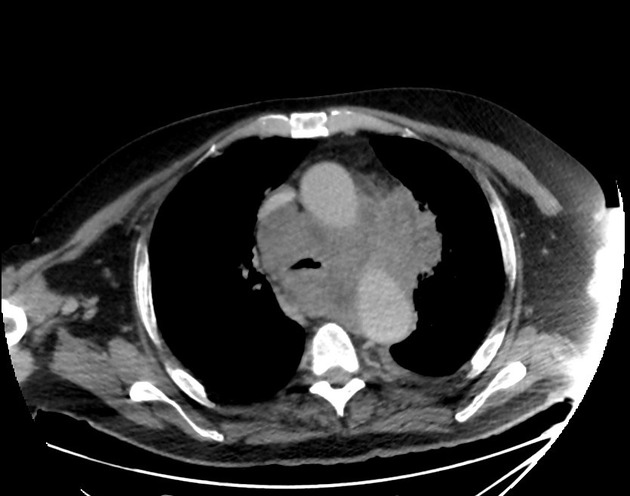
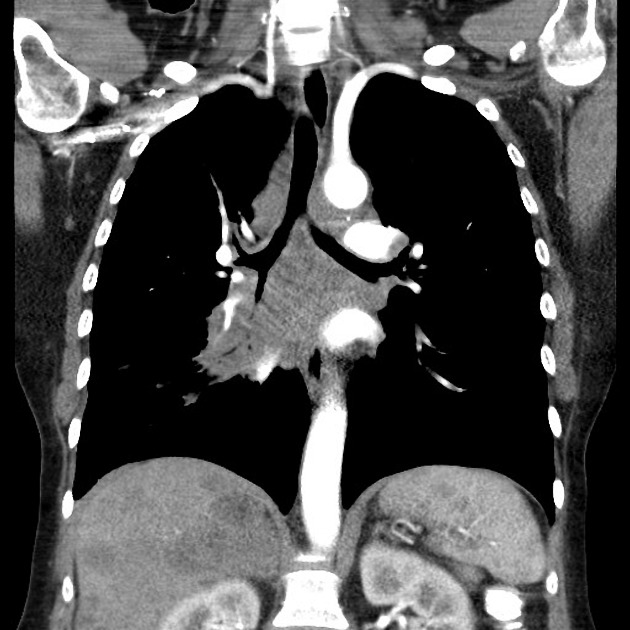
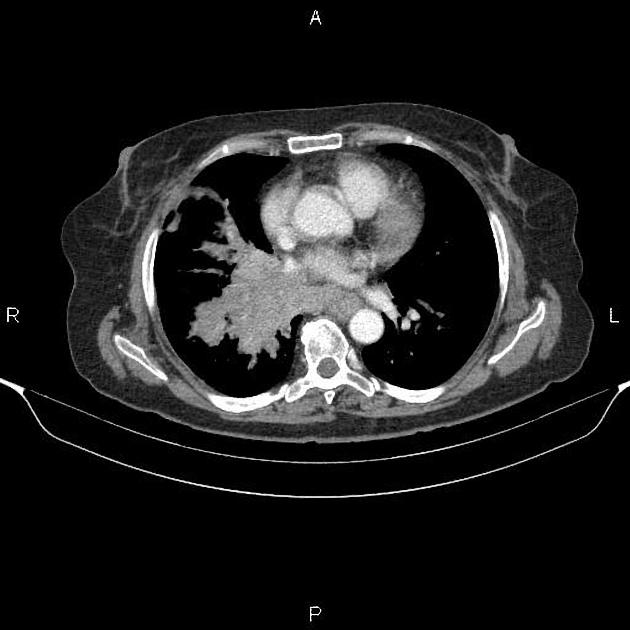
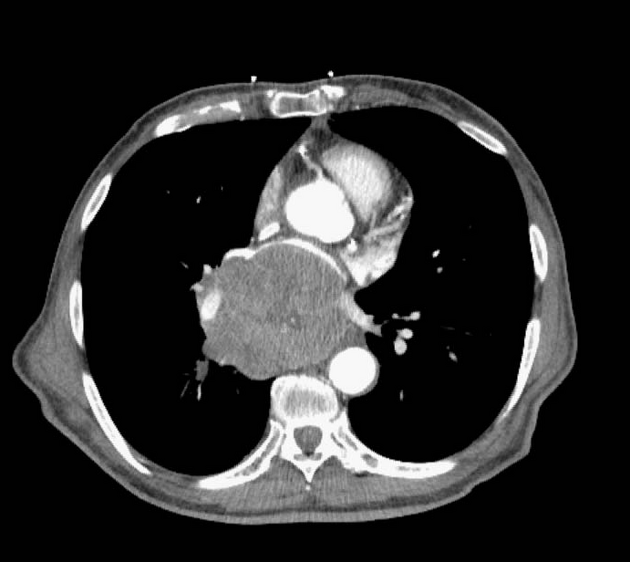
On CT, mediastinal involvement may appear similar to lymphoma, with numerous enlarged nodes. Direct infiltration of adjacent structures is common. Small cell carcinoma of the lung is the most common cause of SVC obstruction, due to both compression/thrombosis and/or direct infiltration 2.
Small cell lung cancers are usually characterized as a mass lesion, where necrosis and hemorrhage are both common. Only rarely do they present as a solitary pulmonary nodule.
For tumor staging, please refer to the article on IASLC (International Association for the Study of Lung Cancer) 8th edition lung cancer staging system (since 2013, small cell lung cancer is staged in the same way as non-small cell lung cancer).
Treatment and prognosis
Most cases will present in advanced stages, be inoperable, and with a dismal prognosis. Only about 5% of patients present at an early stage (Ia, Ib, or IIa), with a potentially curable disease. These patients are usually managed with aggressive chemoradiation therapy and, a few, with lobectomy associated with mediastinal lymph node dissection 4,5.
Surgical excision is commonly not recommended beyond these early stages, as studies have shown that any nodal involvement (N1–3 disease) will not benefit from excisional treatment 4,5.
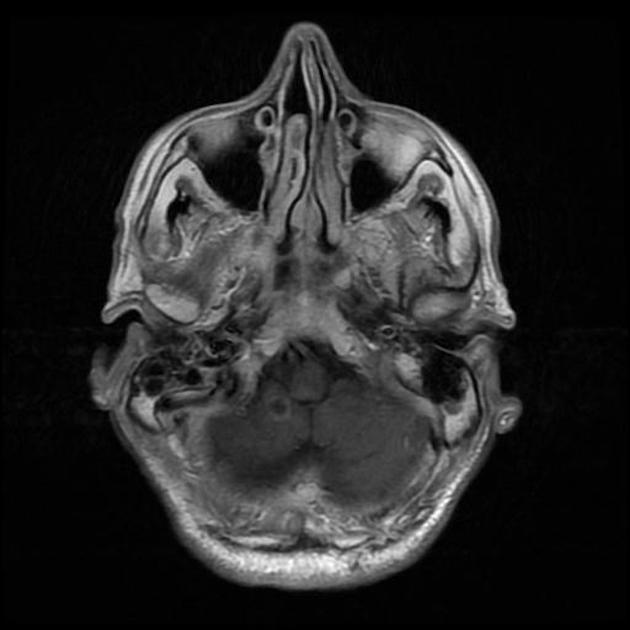
Brain metastases are found in up to a quarter of patients at presentation 4 and are known as a common site of disease recurrence after an initial treatment response. Prophylactic cerebral irradiation (PCI) can be offered for those with adequate systemic control and without central nervous system metastases 4.
Advanced disease (stage IV) is managed only with chemotherapy, primarily for palliation and symptom control.
Differential diagnosis
Imaging differential considerations include:








 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.